Abstract
Increase in hepatic arterial flow in response to reduced portal flow (hepatic arterial buffer response) has been demonstrated experimentally and surgically. We provide pathologic evidence for hepatic arterial buffer response in non-cirrhotic patients with extrahepatic portal vein thrombosis and elucidate the histopathologic spectrum of non-cirrhotic portal vein thrombosis. Liver biopsies and resections from non-cirrhotic patients with extra-hepatic portal vein thrombosis were retrieved. Morphologic features, extent of CD34 staining, outer diameters, luminal diameters and wall thickness of hepatic arteries cut in cross-section and outer diameters of cross-sectioned paired bile ducts were compared with age- and gender-matched controls. There were 12 male and 9 female patients. Measurements of 280 and 193 arteries from patients and controls, respectively, demonstrated statistically significant (P<0.05) arterial dilatation (increase in percentage of arterial lumen to outer diameter) and arterial wall thinning in resection specimens of non-cirrhotic patients with extra-hepatic portal vein thrombosis. Subtle and/or focal dilatation of central veins, portal veins and sinusoids; focal trabecular thinning/thickening and mild ductular reaction were common findings in both the patient and control groups. Diffuse and obvious changes, and portal vein absence or attenuation were seen only in the patient group. Capillarization of sinusoids was not seen on CD34 stain. Two patients showed significant ductular reaction, one of who developed biliary strictures on follow-up. Hepatic arterial dilatation and wall thinning in non-cirrhotic patients with portal vein thrombosis provide pathologic evidence of hepatic arterial buffer response in the human liver. Obvious and diffuse sinusoidal dilatation and absence or attenuation of portal veins are highly suggestive of extrahepatic portal vein thrombosis in non-cirrhotic patients with portal hypertension. Periportal shunt vessels, hypervascular portal tracts, muscularized portal veins, large thick-walled or dilated arteries aid diagnosis but are rare findings. Normal or near-normal biopsies do not rule out portal vein thrombosis.
Similar content being viewed by others
Introduction
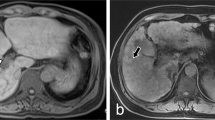
The portal vein is responsible for approximately 70% of blood supply to the liver. Decrease in portal flow leads to compensatory increase in hepatic arterial flow, which is termed hepatic arterial buffer response.1 This response has been demonstrated as an immediate reaction to portal flow reduction in experimental animals as well as in patients undergoing surgery that involves clamping of the portal vein.2, 3, 4, 5, 6 Dilatation of the left hepatic artery and arterial hyperperfusion were demonstrated in a young woman with thrombosis of the left anterior portal vein using high-resolution 3D gadolinium-enhanced magnetic resonance angiography.7 Pathologic evidence of hepatic arterial buffer response, however, has never been demonstrated, probably because microscopic study of vascular diseases is not easy in the human liver as compensatory responses of the dual blood supply blunt pathological effects, which moreover, are neither uniform throughout the liver nor amenable to immunohistochemical study. Furthermore, patients with portal vein thrombosis rarely undergo biopsies or surgical resections, albeit biopsies would not be ideal for study of processes that are patchy in nature. In this study, we tested the hypothesis that induction of hepatic arterial buffer response results in structural modifications of hepatic arteries over time in non-cirrhotic patients with extrahepatic portal vein thrombosis. By comparing arterial measurements with age- and gender-matched controls, this study presents the first ever pathologic validation of hepatic arterial buffer response in the non-cirrhotic human liver.
In addition to hepatic arterial buffer response, portal vein thrombosis leads to the formation of a mass of collaterals, termed a cavernoma, around the obliterated segment of the vein. Although both mechanisms aim to restore blood flow to the liver, normal physiological levels are not achieved. Chronic decrease in blood flow because of portal vein thrombosis may be expected to have effects on the hepatic parenchyma but there is sparse documentation of the histological findings of extrahepatic portal vein thrombosis in the non-cirrhotic liver. The few published pathologic studies have discussed cases of non-cirrhotic extrahepatic portal vein thrombosis in the context of a diverse mix of entities that give rise to non-cirrhotic portal hypertension. Sinusoidal and central vein dilatation are frequently described but are not specific enough to be readily applicable, especially because no study has compared these cases with gender- and age-matched controls. Other described features such as portal hypervascularity or presence of periportal shunt vessels, although seemingly more specific, lack precise definitions. Furthermore, no study addresses morphologic changes in the hepatic arteries in patients with portal vein thrombosis and no cirrhosis. By systematically comparing pathologic features with age- and gender-matched controls, our study aims to elucidate the spectrum of parenchymal and arterial changes associated with non-cirrhotic portal vein thrombosis.
Materials and methods
Following approval of the study protocol by the Institutional Review Board of Indiana University, clinical and pathology databases of Indiana University Health were queried to identify patients with portal vein thrombosis and no cirrhosis who had pathology material available for study. Patients with concomitant liver diseases and portal vein obstruction by tumor were excluded. We also excluded a hepatectomy specimen with advanced chronic biliary disease in a patient with extrahepatic portal vein thrombosis (possible portal biliopathy) to avoid the effects of confounding factors on the hepatic parenchyma and hepatic arteries. Liver biopsies from age- and gender-matched individuals reported as being normal or showing only minimal nonspecific histological changes served as controls for biopsy specimens. Blocks representing non-tumor liver from tumor resection specimens of age- and gender-matched controls served as controls for resection specimens. More than one control was used for patients who had multiple biopsies at different ages to match each age point. Relevant clinical information was obtained from the electronic medical records.
Archived 3–4-μ-thick slides of liver biopsies and resection specimens stained with hematoxylin and eosin, Masson trichrome and silver stain for reticulin fibers were available for study. All tissue had been fixed in formalin and processed in paraffin. The slides were reviewed by two pathologists (RS and NR) who were blinded to the clinical diagnosis. Sinusoidal dilatation, central vein dilatation, trabecular thinning and trabecular thickening were graded as subtle or obvious and focal or diffuse. Hematoxylin eosin and silver-stained slides were used to evaluate trabecular thinning and thickening. Portal vein dilatation, muscularization of the portal veins, portal vein absence and/or attenuation, periportal shunt vessels (dilated thin-walled veins outside but attached to portal tracts), portal hypervascularity, portal fibrosis, perivenular fibrosis and nodularity were recorded as being present or absent. Ductular reaction was graded as none, minimal/mild, moderate or severe. Additional changes related to the bile ducts were noted. Presence or absence of unpaired arterioles in the lobules was recorded. Any other notable finding was also recorded. Multiple specimens from the same patient were additionally reviewed to elucidate any identifiable pattern of progression with time.
Cross-sectional profiles of hepatic arterial branches were identified on trichrome-stained slides. For each hepatic arteriole, the widest cross-sectional diameter, the arterial wall thickness and the diameter of the lumen were measured by a previously published method8 (Figure 1). The outer diameter of the accompanying bile duct, when one was present and cut in cross-section, was measured. Tangential profiles of hepatic arteries and bile ducts were excluded. A Nikon DS Camera Control Unit DS-L1 was utilized to take measurements. The unit was calibrated before each measurement based on the magnification of the objective lens. The percentage of luminal to outer diameter was calculated for each measured hepatic artery. The ratio of the outer diameters of the bile duct to hepatic artery (BD:HA) was calculated in each instance in which cross-sections of a hepatic artery–bile duct pair were present for measurement.
Three-micron-thick sections were stained immunohistochemically with an antibody against CD34 (QBEnd10, prediluted, Dako, Carpinteria, CA, USA) by an automated method. Slides were reviewed to identify structures that were positive for CD34, and for the extent of staining of sinusoidal lining cells. Staining of sinusoidal lining cells in the periportal areas was considered normal. Extension of staining beyond the periportal areas was considered to be evidence of 'capillarisation of sinusoids'.
The two-tailed Student's t-test was used to compare parametric variables and Mann–Whitney U-test was used for nonparametric variables; a P-value of <0.05 was considered to be statistically significant.
Results
Twenty-one patients with extrahepatic portal vein thrombosis and no cirrhosis or other concomitant liver disease were identified between 1998 and 2015. Of the 21 patients, one patient had three-needle biopsies, another had two-needle biopsies and a third patient had three-needle biopsies and a total hepatectomy. Thus, there were 27 specimens available for review including one wedge biopsy, 20-needle biopsies and six total hepatectomies (Figure 2). The control group consisted of liver biopsy or resection specimens from 23 age- and gender-matched individuals.
The 21 patients comprise 12 males and 9 females ranging in age from 30 to 68 years (mean age 48.4 years). One patient had acute portal vein thrombosis because of sepsis by Streptococcus viridians following a dental procedure, whereas the remaining 20 patients had chronic portal vein thrombosis. A cavernoma was documented in 19 of these 20 patients. Almost all patients with chronic portal vein thrombosis had manifestations of portal hypertension in the form of esophageal varices, splenomegaly and ascites. The medical records documented a hypercoagulable state in six patients with one case each of myelodysplastic syndrome, polycythemia vera, JAK2 mutation with history of renal cell carcinoma, and combined protein C and protein S deficiency. The underlying cause of hypercoagulability was not known in the other two patients in whom a hypercoagulable state had been demonstrated. In the remaining patients, the medical records did not document a definite cause for the portal vein thrombosis. One patient had a history of schistosomiasis and two patients had a liver abscess; it is uncertain whether the latter was a cause or consequence of the portal vein thrombosis (Table 1).
In addition to portal vein thrombosis, six patients had superior mesenteric vein thrombosis and an additional patient had splenic vein thrombosis. The patients with mesenteric vein thrombosis included one each with polycythemia vera, myelodysplastic syndrome and JAK2 mutation; a fourth patient had a demonstrable hypercoagulable state of unknown cause whereas the remaining two patients did not have a documented hypercoagulable state. Two of the six patients with portal vein thrombosis and superior mesenteric vein thrombosis underwent multivisceral transplantation that included liver transplantation (Table 1).
Hepatectomy was performed for liver dysfunction including hepatic encephalopathy and portal hypertension as part of isolated liver transplantation in one patient and as part of multivisceral transplantation in five patients. Of the latter, two patients had extensive mesenteric vein, including portal vein, thrombosis (Table 1).
Measurements were obtained for a total of 193 (2–19 per case) and 280 (1–22 per case) hepatic arteries as well as for 105 (2–11 per case) and 150 (1– 17 per case) bile ducts in the control and patient groups, respectively. The BD:HA ratio was 0.8 in each group. Given this ratio in our series and because septal bile ducts are 100 μ or more in diameter, we designated arteries 120 μm or more in diameter as septal arteries and those <120 μm in diameter as terminal arteries. Measurements for septal and terminal arteries in biopsy and resection specimens are shown in Tables 2 and 3. There was a statistically significant difference in the arterial wall thickness and percentage of arterial lumen to outer diameter between the control and patient groups in resection specimens; the wall was thinned out and the lumen dilated in patients with non-cirrhotic portal vein thrombosis as compared with controls. There were no statistically significant differences in the hepatic arteries from biopsy specimens (Table 3).
Two of 27 (7%) patient and 5 of 23 (22%) control specimens showed no pathological changes. Subtle and/or focal dilatation of central veins, portal veins and sinusoids were a common finding in both the patient and control groups; however, these changes were diffuse and obvious only in patients with portal vein thrombosis (Table 4, Figure 3). Similarly, subtle and/or focal trabecular thickening or thinning was a common finding in both groups but these changes were diffuse and obvious only in patients with portal vein thrombosis (Table 2, Figure 4). Portal vein absence or attenuation (Figure 5) was seen in seven specimens from the non-cirrhotic portal vein thrombosis group and in none of the control group. Periportal shunt vessels were present in three specimens from the patient and two from the control group; in each case, the periportal shunt vessel was seen in only one portal tract (Figure 6). Portal hypervascularity was present in only one portal tract in two biopsies from the patient group; this feature was not seen in the control group. Muscularization of the portal veins was seen in four specimens from the patient group and no controls (Figure 7). Abnormally large arteries with thick muscular walls were occasionally noticed in random portal tracts (Figure 8) in some patients. Similarly, dilated arteries with wide lumina and thin walls were visualized in random portal tracts in some patients (Figure 7b). Unpaired arterioles in the lobules were rare, one such arteriole being present in one patient and one control biopsy each. Two biopsies from one patient showed moderate ductular reaction and periductal fibrosis around some bile ducts (Figure 9); this patient developed biliary strictures on follow-up. A second patient showed severe ductular reaction. Ductular reaction was never more than mild in biopsies from the control group. Immunohistochemical stain for CD34 showed positivity in endothelium of portal vein branches, hepatic artery branches, hepatic vein tributaries and sinusoidal lining cells in periportal regions in all specimens from both patient and control groups (Figure 10). In neither group did staining extend beyond the periportal regions as may be expected with 'capillarisation of sinusoids'. All these observations were true for both biopsy and resection specimens. In the resection specimens, where many sections were available for review, sinusoidal dilatation, trabecular thinning, phlebosclerosis/attenuation of portal veins and muscularization of the portal veins were the most common findings. One biopsy specimen showed patchy area of very abnormal architecture with irregular fibrosis. The three cases of multiple specimens from the same patient did not show a specific pattern of evolution. The findings in these patients varied widely between specimens suggesting that changes are not uniform throughout the liver.
Sinusoidal dilatation of varying degrees and extent was seen in many liver biopsies: diffuse and obvious sinusoidal dilatation in a non-cirrhotic patient with portal vein thrombosis (a); severe sinusoidal dilatation in another non-cirrhotic patient with portal vein thrombosis (b) and focal but obvious sinusoidal dilatation in a liver biopsy from the control group (c). Hematoxylin and eosin; 10x (a, c) and 20x (b).
Disproportionately large thick-walled hepatic arterial branches in liver biopsies from two patients with non-cirrhotic portal vein thrombosis. Attenuated portal vein profiles are seen in (a). No portal vein is seen in (b) but the complete portal tract is not represented in the biopsy. Masson trichrome 400x (a) and hematoxylin eosin 200x (b).
Immunohistochemical stain for CD34 shows positivity in endothelium of hepatic artery branches, portal vein branches, hepatic vein tributaries and sinusoidal lining cells in periportal areas in a patient with non-cirrhotic portal vein thrombosis (a) and a control specimen (b). Staining of sinusoidal lining cells beyond the periportal areas, indicative of capillarization of sinsuoids, was not seen in the patient group. 3,3'-diaminobenzidine 200x (a, b).
Discussion
Absorbed nutrients and xenobiotics are carried directly by the portal vein from the intestines to the liver where they are efficiently cleared by the formidable metabolic machinery of hepatocytes. This is greatly aided by a sinusoidal structure that is remarkable for a lining of fenestrated endothelial cells and absence of basement membranes, dual features that allow hepatocytes easy access to metabolic substrates as they pass through the low pressure sinusoidal bed. This sophisticated microarchitecture is complimented by physiologic mechanisms that ensure a steady rate of blood flow in the sinusoidal bed, which is crucial for hepatic clearance of metabolic substrates.9, 10
The portal vein and hepatic artery comprise a dual blood supply, contributing 70 and 30% of blood flow respectively, into the liver. The portal vein is a low pressure low resistance vessel, which cannot regulate its blood flow, portal flow being simply a function of total splanchnic flow. The hepatic artery, on the other hand, is a high pressure high resistance vessel that regulates not only its own flow by a process of autoregulation but also total flow in the liver by responding to changes in portal flow. If portal blood flow is reduced, the hepatic artery dilates and when portal flow is increased, the hepatic artery constricts.2, 11 This response, termed hepatic arterial buffer response is capable of buffering up to 60% of decreased portal flow and ensures that physiologic levels of blood flow are maintained in the sinusoidal bed.1, 11 Hepatic arterial buffer response has been demonstrated by flow measurements and imaging modalities in experimental animals as well as in human subjects with portal vein thrombosis or with clamping of portal vein during abdominal surgery.2, 3, 4, 5, 6, 7 Hepatic arterial buffer response is also functional in fetal circulation12 and the cirrhotic liver.13 There is no portal reciprocity to hepatic arterial buffer response; portal flow2 or resistance14 do not change in response to changes in hepatic arterial flow.
The importance of hepatic arterial buffer response cannot be overstated. Not only does the liver metabolize and clear nutrients and xenobiotics but also endogenous substances including hormones, appropriate circulating levels of which are essential for maintaining overall body homeostasis. Hepatic clearance of hormones depends primarily on physiologically adequate levels of sinusoidal blood flow; changes in the latter alter clearance and therefore plasma hormonal concentrations, which affect whole body homeostasis. Blood flow in the hepatic artery is thus regulated to subserve the overarching objective of preserving whole body homeostasis by maintaining steady physiological levels of sinusoidal flow. The hepatic arterial flow does not respond to local metabolic or oxygen demands of the liver itself.9, 10, 15, 16
Ours is the first study to demonstrate histologic changes in hepatic arteries as pathologic evidence for hepatic arterial buffer response in the non-cirrhotic human liver. Comparison of arterial measurements of 280 arteries in our series of non-cirrhotic portal vein thrombosis patients with 193 arteries in an age- and gender-matched control group demonstrates that there is dilatation of the hepatic arteries as evidenced by a decrease in wall thickness and increase in the percentage of arterial lumen to outer diameter. These changes were seen in resection specimens, but not in biopsy specimens. This may simply be a reflection of relative numbers of arteries amenable to measuring in biopsy and resection specimens as there were more terminal arteries in biopsy specimens and more septal arteries in resection specimens. Alternatively, these findings may indicate that structural alterations in hepatic arteries are established either over a longer term or with severe, advanced or decompensated disease that necessitates transplantation and therefore hepatic resection.
We observed morphologic alterations in the hepatic arteries to complement the statistical data; the changes were often, but not always, associated with portal vein absence or attenuation. The arterial changes were patchy and not uniform throughout the biopsy or resection specimens. Thus, some arteries appeared dilated with luminal widening whereas others showed thick muscular walls with luminal narrowing. This may explain the absence of any statistical difference in the biopsy specimens whereas the statistically significant dilatation in the resection specimens may signify an end-stage result of continuously increased hepatic arterial flow because of long-term or severe disease.
Thrombosis of the extrahepatic portal vein in the absence of cirrhosis is the major cause of portal hypertension and variceal bleeding in children in developing countries17, 18 and the second most common cause of portal hypertension in the world.19 In these cases, the presence of variceal bleeding triggers investigations for presence of cirrhosis and its underlying cause, which may include a liver biopsy. No study has specifically addressed the pathologic findings of portal vein thrombosis in the non-cirrhotic liver although cases have been discussed in larger series of diverse entities that cause non-cirrhotic portal hypertension. These reports describe sinusoidal dilatation, portal vein dilatation, portal hypervascularity, presence of periportal shunt vessels, phlebosclerosis and perisinusoidal fibrosis,20, 21, 22, 23 findings that are not easily applied to routine diagnostic practice because some are subtle and lack precise definitions whereas others are relatively nonspecific. In addition, no study has compared these findings with age- and gender-matched controls and none mentions arterial changes in the non-cirrhotic liver with extrahepatic portal vein thrombosis. To close this knowledge gap, we compared histologic findings in liver tissue of non-cirrhotic patients with portal vein thrombosis with near-normal liver tissue from age- and gender-matched controls. In doing so, we found that subtle dilatation of portal veins, central veins and sinusoids is present in otherwise normal biopsies, particularly when these features are specifically looked for. The same is true for presence of thick or thin hepatic trabecula. However, these changes are diffuse and more obvious in liver biopsies from non-cirrhotic patients with portal vein thrombosis. Absence and/or attenuation of portal veins were only seen in patients with extrahepatic portal vein thrombosis. Several publications demonstrate excellent images of periportal shunt vessels, portal hypervascularity, phlebosclerosis/attenuation of the portal vein, and muscularization (also referred to as arterialization in many publications) of the portal vein, suggesting that these are common and specific findings of extrahepatic portal vein thrombosis.21, 22, 23 We found that these features, although definitively more specific than dilatation of the sinusoids or other vascular structures, were only occasional findings in our study. This may also be true in the studies mentioned in the aforementioned publications but is not explicitly stated. In addition, all these features may be present in the entity called 'hepatoportal sclerosis' or 'obliterative portal venopathy', which is characterized by obliteration of the intrahepatic branches of the portal vein in the presence of a patent extrahepatic portal vein.24, 25 The finding of 'periportal shunt vessels' in two specimens from the control group may reflect tangential cuts of branching portal veins and the associated difficulty of accurately defining a periportal shunt vessel.
Portal biliopathy is a complication of extrahepatic portal vein thrombosis; most patients are asymptomatic and biliary tract abnormalities are found incidentally on imaging studies.26 Two patients in our study cohort had moderate-to-severe degree of ductular reaction, which is probably a reflection of portal biliopathy; one of these patients developed biliary strictures on follow-up. Although portal vein thrombosis is a known cause of nodular regenerative hyperplasia, none of our cases, including the hepatectomy specimens, showed this change. The reason for this is not clear; it may be speculated that there was not enough time for nodular regenerative hyperplasia to develop. We are unable to answer this question because the medical records were less than comprehensive in most cases. This weakness of our series hinders detailed clinical correlation but does not detract from the main goals of the study.
We propose that the presence of diffuse and obvious dilatation of portal veins, central veins and sinusoids in a liver biopsy from a patient with portal hypertension and no cirrhosis should raise suspicion of extrahepatic portal vein thrombosis. In addition, the presence of abnormal arteries, which may be disproportionately large and thick walled or dilated and thin walled, is a special feature of portal vein thrombosis in the non-cirrhotic liver that has never been documented; often, these abnormal arteries are present in portal tracts with attenuated or absent portal veins (Figures 5, 7 and 8; Box 1). The presence of periportal shunt vessels, muscularized portal veins or attenuated/absent portal veins lend support to this diagnosis; all these features are also seen in obliterative portal venopathy, a differential that can be easily sorted out by Doppler sonography of the extrahepatic portal vein. Other causes of sinusoidal dilatation with portal hypertension include right-sided cardiac decompensation, veno-occlusive disease/sinusoidal obstruction syndrome and Budd–Chiari syndrome. In the latter two conditions and some but not all cases of right-sided cardiac decompensation, dilatation of sinusoids is most often accompanied by congestion and even hemorrhagic necrosis around the central veins. In addition, there are clinical signs and symptoms of cardiac disease in right-sided cardiac decompensation and a history of risk factors such as chemotherapy or radiotherapy in cases of veno-occlusive disease/sinusoidal obstruction syndrome. These pathologies are not expected to cause attenuation and/or absence of portal veins although there is no controlled study that specifically addresses this feature in these cases. Sinusoidal dilatation is also seen in systemic inflammatory diseases, and wedge biopsies from abdominal surgeries.27 These cases would not be expected to show attenuation and/or absence of portal veins unless there is associated extrahepatic portal vein thrombosis in the systemic inflammatory conditions. Our series also demonstrates that some cases of portal vein thrombosis do not show any pathologic changes in a liver biopsy; thus a normal or near-normal liver biopsy does not exclude the presence of extrahepatic portal vein thrombosis. These cases either represent an early stage of the disease, compensated disease or sampling variability because of the patchy nature of the findings. Gradual loss of hepatic mass because of chronically decreased blood flow is considered responsible for the ultimate functional decompensation that occurs in non-cirrhotic patients with portal vein thrombosis.28
References
Lautt WW . The 1995 Ciba-Geigy Award Lecture. Intrinsic regulation of hepatic blood flow. Can J Physiol Pharmacol 1996;74:223–233.
Jakab F, Rath Z, Schmal F et al. The interaction between hepatic arterial and portal venous blood flows; simultaneous measurement by transit time ultrasonic volume flowmetry. Hepatogastroenterology 1995;42:18–21.
Rocheleau B, Ethier C, Houle R et al. Hepatic artery buffer response following left portal vein ligation: its role in liver tissue homeostasis. Am J Physiol 1999;277:G1000–G1007.
Payen DM, Fratacci MD, Dupuy P et al. Portal and hepatic arterial blood flow measurements of human transplanted liver by implanted Doppler probes: interest for early complications and nutrition. Surgery 1990;107:417–427.
Henderson JM, Gilmore GT, Mackay GJ et al. Hemodynamics during liver transplantation: the interactions between cardiac output and portal venous and hepatic arterial flows. Hepatology 1992;16:715–718.
Bolognesi M, Sacerdoti D, Bombonato G et al. Change in portal flow after liver transplantation: effect on hepatic arterial resistance indices and role of spleen size. Hepatology 2002;35:601–608.
Gulberg V, Schoenberg SO . Hepatic arterial buffer response: visualization by multiphasic high-resolution 3D magnetic resonance angiography. J Hepatol 2004;40:181.
Fiel MI, Deniz K, Elmali F et al. Increasing hepatic arteriole wall thickness and decreased luminal diameter occur with increasing age in normal livers. J Hepatol 2011;55:582–586.
Lautt WW . Relationship between hepatic blood flow and overall metabolism: the hepatic arterial buffer response. Fed Proc 1983;42:1662–1666.
Lautt WW . The hepatic artery: subservient to hepatic metabolism or guardian of normal hepatic clearance rates of humoral substances. Gen Pharmacol 1977;8:73–78.
Lautt WW, Legare DJ, Ezzat WR . Quantitation of the hepatic arterial buffer response to graded changes in portal blood flow. Gastroenterology 1990;98:1024–1028.
Ebbing C, Rasmussen S, Godfrey KM et al. Hepatic artery hemodynamics suggest operation of a buffer response in the human fetus. Reprod Sci 2008;15:166–178.
Gulberg V, Haag K, Rossle M et al. Hepatic arterial buffer response in patients with advanced cirrhosis. Hepatology 2002;35:630–634.
Legare DJ, Lautt WW . Hepatic venous resistance site in the dog: localization and validation of intrahepatic pressure measurements. Can J Physiol Pharmacol 1987;65:352–359.
Lautt WW . Control of hepatic arterial blood flow: independence from liver metabolic activity. Am J Physiol 1980;239:H559–H564.
Lautt WW . Mechanism and role of intrinsic regulation of hepatic arterial blood flow: hepatic arterial buffer response. Am J Physiol 1985;249:G549–G556.
Poddar U, Thapa BR, Rao KL et al. Etiological spectrum of esophageal varices due to portal hypertension in Indian children: is it different from the West? J Gastroenterol Hepatol 2008;23:1354–1357.
Yachha SK . Portal hypertension in children: an Indian perspective. J Gastroenterol Hepatol 2002;17 (Suppl 3):S228–S231.
Garcia-Pagan JC, Hernandez-Guerra M, Bosch J . Extrahepatic portal vein thrombosis. Semin Liver Dis 2008;28:282–292.
Ibarrola C, Colina F . Clinicopathological features of nine cases of non-cirrhotic portal hypertension: current definitions and criteria are inadequate. Histopathology 2003;42:251–264.
Roskams T, Baptista A, Bianchi L et al. Histopathology of portal hypertension: a practical guideline. Histopathology 2003;42:2–13.
Schouten JN, Verheij J, Seijo S . Idiopathic non-cirrhotic portal hypertension: a review. Orphanet J Rare Dis 2015;10:67.
Verheij J, Schouten JN, Komuta M et al. Histological features in western patients with idiopathic non-cirrhotic portal hypertension. Histopathology 2013;62:1083–1091.
Aggarwal S, Fiel MI, Schiano TD . Obliterative portal venopathy: a clinical and histopathological review. Dig Dis Sci. 2013;58:2767–2776.
Mikkelsen WP, Edmondson HA, Peters RL et al. Extra- and intrahepatic portal hypertension without cirrhosis (hepatoportal sclerosis). Ann Surg 1965;162:602–620.
Khan MR, Tariq J, Raza R et al. Portal hypertensive biliopathy: review of pathophysiology and management. Trop Gastroenterol. 2012;33:173–178.
Kakar S, Kamath PS, Burgart LJ . Sinusoidal dilatation and congestion in liver biopsy: is it always due to venous outflow impairment? Arch Pathol Lab Med 2004;128:901–904.
Harmanci O, Bayraktar Y . Portal hypertension due to portal venous thrombosis: etiology, clinical outcomes. World J Gastroenterol 2007;13:2535–2540.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Rush, N., Sun, H., Nakanishi, Y. et al. Hepatic arterial buffer response: pathologic evidence in non-cirrhotic human liver with extrahepatic portal vein thrombosis. Mod Pathol 29, 489–499 (2016). https://doi.org/10.1038/modpathol.2016.43
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.2016.43
This article is cited by
-
Two cases of benign hepatic nodules caused by sinusoidal dilatation with different hemodynamics
Clinical Journal of Gastroenterology (2020)