Abstract
Somatic G17V RHOA mutations were found in 50–70% of angioimmunoblastic T-cell lymphoma (AITL). The mutant RHOA lacks GTP binding capacity, suggesting defects in the classical RHOA signaling. Here, we discovered the novel function of the G17V RHOA: VAV1 was identified as a G17V RHOA-specific binding partner via high-throughput screening. We found that binding of G17V RHOA to VAV1 augmented its adaptor function through phosphorylation of 174Tyr, resulting in acceleration of T-cell receptor (TCR) signaling. Enrichment of cytokine and chemokine-related pathways was also evident by the expression of G17V RHOA. We further identified VAV1 mutations and a new translocation, VAV1–STAP2, in seven of the 85 RHOA mutation-negative samples (8.2%), whereas none of the 41 RHOA mutation-positive samples exhibited VAV1 mutations. Augmentation of 174Tyr phosphorylation was also demonstrated in VAV1–STAP2. Dasatinib, a multikinase inhibitor, efficiently blocked the accelerated VAV1 phosphorylation and the associating TCR signaling by both G17V RHOA and VAV1–STAP2 expression. Phospho-VAV1 staining was demonstrated in the clinical specimens harboring G17V RHOA and VAV1 mutations at a higher frequency than those without. Our findings indicate that the G17V RHOA–VAV1 axis may provide a new therapeutic target in AITL.
Similar content being viewed by others
Introduction
Angioimmunoblastic T-cell lymphoma (AITL) is a subtype of peripheral T-cell lymphoma.1 AITL patients display generalized lymphadenopathy and immune system-mediated manifestations including high fever, skin rash, polyarthritis, hemolytic anemia and hypergammaglobulinemia.2 We and others previously conducted gene mutational profiling of AITL samples and observed RHOA mutations converting glycine to valine at amino acid 17 (the G17V RHOA mutation) in up to 70% of AITL.3, 4, 5 Genes encoding the epigenetic regulators TET2, DNMT3A and IDH2 are also frequently mutated in AITL.3, 4, 6, 7, 8, 9, 10
RHOA is a small GTPase that cycles between guanosine diphosphate (GDP)-bound inactive and guanosine-triphosphate (GTP)-bound active forms. Guanine nucleotide exchange factors (GEFs) activate RHOA by replacing GDP with GTP. Physiologically, RHOA mediates migration and polarity of T cells.11, 12 RHOA also functions in thymocyte development13, 14 and activation of pre-T-cell receptor (pre-TCR) signaling in thymocytes.13, 15 Glycine at RHOA residue 17 is located at a critical position for GTP binding. G17V RHOA protein is considered to be a loss-of-function mutant, as G17V RHOA does not bind Rhotekin, a molecule with high affinity for the GTP-bound form.3, 4, 5 Nonetheless, the impact of G17V RHOA expression on AITL remains unclear.
The VAV1 protein mediates a signaling cascade triggered by the TCR engagement partly through GEF activity,16 whereas GEF-independent VAV1 functions are also reported.17, 18 In the latter, VAV1 functions as an adaptor in a protein complex that promotes phosphorylation of phospholipase C-γ1 (PLCγ1).18, 19
PLCγ1 phosphorylation induces its own enzymatic activity to upregulate the second messengers diacylglycerol and inositol 1,4,5-triphosphate, in turn promoting calcium–calmodulin signaling and enhancing nuclear factor of activated T cells (NFAT) transcription.20 VAV1 also functions in extracellular signal-regulated kinase, c-Jun N-terminal kinase and nuclear factor-κB pathways,21 and its activation is tightly regulated by multilayered autoinhibition by interaction of its Dbl-homology (DH) domain with both acidic (167–178)22 and C-terminal Src homology 2 (SH2)/SH3 domains. TCR engagement initially triggers the phosphorylation of Tyr142 and Tyr160 of VAV1 protein, destabilizing modulatory contacts and facilitating recruitment of the Src kinases LCK and FYN by providing a docking site for their SH2 domains. Thereafter, VAV1 Tyr174 is phosphorylated,23 relieving core inhibitory interactions with the acidic and DH domains, resulting in the activation of downstream effectors. Conversion of Tyr174 to either Phe17 or Asp24 or physiologic phosphorylation of the wild-type Tyr174 residue reportedly activates VAV1 signaling. In addition, deletion of the VAV1 C terminus enhances its signaling.25
Here we used mass spectrometry and immunoprecipitation to show that the G17V RHOA protein specifically binds to VAV1 protein. Upon TCR stimulation, VAV1 binding to G17V RHOA accelerated VAV1 phosphorylation and the eventual downstream signaling cascade.
Materials and methods
Patients and samples
Samples were obtained from patients with approval of local ethics committees in all participating institutes. Informed consent was obtained from all living subjects.
Cells
Jurkat cells inducibly expressing the wild-type (WT) and G17V RHOA mutant complementary DNA (cDNA) and mock-transduced cells have been previously described.3 We newly established VAV1–STAP2-expressing Jurkat cells with a method similar to the previous one.3 SU9T01 cells inducibly expressing WT or G17V RHOA cDNA and mock-transduced cells were also established previously.
Jurkat cells and SU9T01 cells were cultured at 37 °C in RPMI-1640 Medium (Sigma-Aldrich, St Louis, MO, USA) supplemented with 10% fetal calf serum and 1% penicillin streptomycin. The 293T cells were cultured at 37 °C in Dulbecco’s modified Eagle’s medium (Sigma-Aldrich) supplemented with 10% fetal calf serum and 1% penicillin streptomycin.
Other experimental methods
DNA extractions, targeted sequencing of RHOA, VAV1, PLCg1, CD28, FYN and LCK genes, antibodies, inhibitors, mRNA sequencing, plasmids, in vitro TCR stimulation, immunoprecipitation, mass spectrometry, NFAT reporter assay, interleukin-2 (IL-2) expression assay and immunohistochemistry are described in Supplementary Information.
Results
Identification of G17V RHOA-specific binding proteins in Jurkat cells
To identify specific binding partners of G17V RHOA, we performed immunoprecipitation analysis in Jurkat cells overexpressing Flag-tagged WT RHOA (JurkatWTRHOA) or the G17V RHOA mutant (JurkatG17V). Specifically, we used ANTI-FLAG Magnetic beads in either line, with or without TCR stimulation (Supplementary Figure 1). By targeted pull-down followed by mass spectrometry, we identified G17V RHOA-specific binding proteins: 44 proteins were identified specifically using G17V bait, both with and without TCR stimulation, 36 specifically without stimulation and 71 specifically with stimulation (Supplementary Table 1, rows 54–56). The corresponding database search results for the 44-protein subset showed the highest Mascot scores to be attributable to VAV family proteins, namely VAV1 and VAV3 (Supplementary Table 2, rows 77 and 78). Here, Mascot protein score is a surrogate for protein abundance. Notably, PLCγ1, an essential component of the TCR pathway, was detected among the G17V RHOA-specific binding proteins only with TCR stimulation (Supplementary Table 2, row 105).
Both tumor-associated G17V3, 4, 5 and engineered G17A RHOA mutants26 lose nucleotide binding capacity, and both have been shown to tightly bind various GEFs. Notably, in COS7 cells the G17A RHOA mutant interacts with active VAV1 mutants that lack the inhibitory N-terminal regions (Δ1–186) or C-terminal SH3 domains (Δ835–845).25 Here, we performed western blot and immunoprecipitation analysis using JurkatWTRHOA and JurkatG17V to validate mass spectrometry results reported above (Supplementary Figure 2). VAV1 was specifically coprecipitated with the G17V RHOA mutant but not with wild-type RHOA in the presence or absence of TCR stimulation, but binding efficiency was markedly augmented by TCR stimulation (Supplementary Figure 2). The result was consistent with the elevated Mascot score by mass spectrometry (Supplementary Table 2, row 78). In contrast, in similar assays we did not observe VAV3 binding to the G17V RHOA mutant (data not shown).
Various deletion mutants lacking the functional domains of VAV1 to determine the binding site for the G17V RHOA were made (Supplementary Figure 7a). A deletion mutant lacking the DH domain did not bind to the G17V RHOA, whereas other mutants as well as wild-type VAV1 did (Supplementary Figure 7b). These observations suggest that the DH domain is essential for binding to the G17V RHOA.
Interaction with G17V RHOA activates VAV1, enhancing its adaptor function
As described, VAV1 phosphorylation at Tyr174 is critical for its activation following TCR stimulation. Remarkably, we detected VAV1 Tyr174 phosphorylation in JurkatG17V cells, even in an unstimulated state, although at low levels, whereas Tyr174 phosphorylation was not seen in unstimulated JurkatWTRHOA or mock-transduced cells (Figure 1 and Supplementary Figure 3). TCR stimulation enhanced VAV1 phosphorylation in both JurkatWTRHOA and mock cells, but that effect was more pronounced in JurkatG17V cells (Figure 1 and Supplementary Figure 3). VAV1 mediates PLCγ1 phosphorylation through facilitating assembly of a PLCγ1–SLP76–LAT complex.19 As anticipated, PLCγ1 phosphorylation was more striking in JurkatG17V than in mock-transduced or JurkatWTRHOA cells upon TCR stimulation (Figure 1 and Supplementary Figure 3). SLP76, an adaptor molecule, and phosphorylated PLCγ1 as well as total and phosphorylated VAV1 were also co-immunoprecipitated with G17V but not with wild-type RHOA (Figure 2). These observations suggest that G17V RHOA–VAV1 interaction enhanced the adaptor function of VAV1 to facilitate formation of a TCR signaling complex.
VAV1 activation by G17V RHOA in Jurkat cells. Jurkatmock, JurkatWTRHOA and JurkatG17V cells were stimulated for 5 or 30 min with or without anti-CD3 antibody, followed by anti-mouse IgG antibody. Immunoblots of lysates were performed with antibodies to VAV1, phospho VAV1 (Tyr174), PLCγ1 and phospho PLCγ1. β-Actin served as loading control. p-PLCγ1, phospho PLCγ1; p-VAV1, phospho VAV1.
Binding of SLP 76 and phosphorylated PLCγ1 as well as VAV1 and phospho VAV1 to G17V RHOA in Jurkat cells. Jurkatmock, JurkatWTRHOA and JurkatG17V cells were stimulated for 5 min with or without anti-CD3 antibody, followed by anti-mouse IgG antibody. Protein was immunoprecipitated from lysates using anti-Flag antibody and then immunoblotted with antibodies to Flag (RHOA), VAV1, phospho VAV1 (Tyr174), PLCγ1, phospho PLCγ1, and SLP76. β-Actin served as loading control. Asterisk (*) indicates G17V RHOA mutant. p-PLCγ1, phospho PLCγ1; p-VAV1, phospho VAV1.
Src kinases reportedly mediate TCR signaling-dependent VAV1 phosphorylation. PP2, a pan-Src inhibitor, dose-dependently inhibited VAV1 phosphorylation (Figure 3a). In addition, some Src kinases including LCK and FYN are known targets of dasatinib, a drug used to treat BCR-ABL-positive leukemias. Thus, we asked whether dasatinib would inhibit VAV1 phosphorylation. As expected, dasatinib dose-dependently inhibited VAV1 phosphorylation, almost completely at 10 nM, in both JurkatG7V and JurkatWT cells (Figure 3b). PLCγ1 phosphorylation was also inhibited by PP2 and more efficiently by dasatinib (Figures 3a and b).
Effect of Src inhibitors on VAV1 activation by G17V RHOA following TCR stimulation. Jurkatmock, JurkatWTRHOA and JurkatG17V cells were stimulated with or without anti-CD3 antibody, followed by anti-mouse IgG antibody after (a) PP2 or (b) dasatinib treatment at indicated concentrations. Lysates were fractionated and immunoblotted with antibodies to VAV1, phospho VAV1 (Tyr174), PLCγ1 and phospho PLCγ1. β-Actin served as loading control. p-PLCγ1, phospho PLCγ1; p-VAV1, phospho VAV1.
We also observed enhanced phosphorylation of VAV1 and PLCγ1 following induction of G17V RHOA expression in SU9T01 cells, an adult T-cell leukemia/lymphoma (ATLL) line, whereas induction of WT RHOA had no effect (Supplementary Figure 4). Furthermore, transient transduction of 293T cells with VAV1 cDNA plus either WT or G17V RHOA revealed greater VAV1 phosphorylation in the presence of G17V RHOA (Supplementary Figure 5). VAV1 and G17V RHOA also co-immunoprecipitated in 293T cells (Supplementary Figure 6). These data overall suggest that VAV1 activation in the presence of the G17V RHOA mutant occurs in a variety of cell types.
Activating VAV1 mutations occur in human AITL and PTCL-NOS
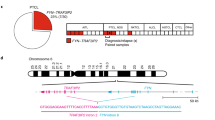
VAV1 translocations and missense/deletion mutations have been identified in T-cell lymphomas.27, 28, 29 Here, RNA sequencing of 9 peripheral T-cell lymphoma (PTCL) samples (6 AITL and 3 PTCL-not otherwise specified (NOS)) identified a VAV1–STAP2 fusion gene in an AITL sample lacking the RHOA mutation (PTCL35, Figures 4a–c and Supplementary Tables 3 and 4). Targeted deep sequencing of VAV1 in 126 PTCL samples (69 AITL and 57 PTCL-NOS) identified two in-frame deletion mutations in an acidic region (c.C518_529del, p. 173_177del in PTCL47; c.C494_520del, p.165_174del in PTCL56) and two in-flame deletion mutations in C-terminal site of an SH2 domain (c.2333_2352del, p.778_786del29 in PTCL181; c.2303_2329del, p.768_777del in PTCL213) in four AITL samples and two missense mutations in the zinc-finger domain and the SH3-SH2-SH3 module, respectively (c.G1668C, p.Glu556Asp in PTCL204; c.C1844T, p.Pro615Leu in PTCL67), in one PTCL-NOS and one AITL sample (Figures 4b and c and Supplementary Table 5). In total, seven VAV1 alterations including mutations of varying types and a fusion were found in 85 RHOA mutation-negative samples (8.2%), whereas none of the 41 RHOA mutation-positive PTCL samples exhibited VAV1 mutations (Figure 4d). In addition, we examined mutations in PLCG1, CD28, FYN and LCK for 49 samples. Six PLCG1 mutations, two CD28 mutations and one FYN mutation were detected, whereas LCK mutations were not (Supplementary Figure 8). Although the sample number was too small to elicit proper conclusion, both RHOA and VAV1 mutations were not exclusive with these mutations.
Identification of VAV1 mutations in human AITL and PTCL-NOS. (a) Schematic diagram of VAV1–STAP2 fusion genes. (b) Structure of VAV1 mutations and VAV1 functional domains. (c) Confirmation of VAV1 mutations by Sanger sequencing. Arrows indicate where mutations occur. (d) Mutation profile of RHOA and VAV1 mutations. Three slushed samples had RHOA mutations other than typical c.G50T mutations. In PTCL 216, c.50_51GA>TC mutations resulted in p.Gly17Val alternation; in PTCL 223, c.50G>A mutation resulted in p.Gly17Glu alternation; and in PTCL 198, c.49_50GG>TT mutations resulted in p.Gly17Leu alternation. *, tatgeted sequencing for VAV1 was not performed.
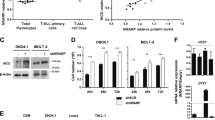
Analysis of Jurkat cells inducibly overexpressing VAV1–STAP2 (JurkatVAV1–STAP2) showed robust phosphorylation of VAV1–STAP2 at Tyr174, even in TCR-unstimulated conditions (Figure 5a and Supplementary Figure 9). VAV1 phosphorylation was faintly detected in cells overexpressing WT VAV1 (JurkatWTVAV1) but not in mock-transduced (Jurkatmock) cells when the TCR was unstimulated (Figure 5a and Supplementary Figure 9). TCR stimulation enhanced phosphorylation of both VAV1–STAP2 and WT VAV1, but VAV1–STAP2 was more highly phosphorylated than WT VAV1 (Figure 5a and Supplementary Figure 9). Unlike G17V RHOA expression, VAV1–STAP2 expression enhanced PLCγ1 phosphorylation, even without TCR stimulation (Figure 5a). These observations suggest that VAV1–STAP2 may autonomously activate TCR signaling without antigen stimulation. PLCγ1 phosphorylation was more striking in JurkatVAV1–STAP2 than in mock-transduced or JurkatWTVAV1 cells upon TCR stimulation. Phosphorylation of VAV1–STAP2 and WT VAV1 was dose-dependently inhibited by either PP2 or dasatinib treatment (Figures 5b and c).
Effect of Src inhibitors on VAV1–STAP2 activation. (a–c) Jurkatmock, JurkatWTVAV1 and JurkatVAV1–STAP2 cells were stimulated with or without anti-CD3 antibody followed by anti-mouse IgG antibody. Cells were treated with (b) PP2 or (c) dasatinib at indicated concentrations. Lysates were fractionated and immunoblotted with antibodies to VAV1, phospho VAV1, and PLCγ1. β-Actin served as loading control. p-PLCγ1, phospho PLCγ1; p-VAV1, phospho VAV1.
Enhanced NFAT activity upon TCR stimulation by G17V RHOA and VAV1 mutants
NFAT transcription factors are essential for T-cell activation and differentiation, and TCR stimulation activates NFATs through Ca2+ mobilization.30 VAV1 mediates Ca2+ mobilization mainly through PLCγ1 activation.19
To identify potential function of G17V RHOA in NFAT activity, we transiently transfected Jurkat cells with a reporter vector containing an NFAT response element plus WT or G17V RHOA cDNAs in the presence or absence of TCR stimulation. Expression of G17V RHOA augmented NFAT activity upon TCR stimulation, whereas that of the WT construct did not (Figure 6a). Dasatinib dose-dependently inhibited NFAT activity in Jurkat cells transduced with either WT or G17V RHOA (Figure 6b).
Effect of G17V RHOA on NFAT activity or IL-2 expression in Jurkat cells. (a, b) Jurkat cells were transiently transfected with a reporter containing an NFAT response element (NFAT-RE) together with WT or G17V RHOA mutant cDNAs in the presence of absence of Dynabeads Human T-activator CD3/CD28. (a) NFAT activity in indicated samples. (b) Effect of dasatinib on NFAT activity. The mean±s.d. from triplicate samples is shown. (c, d) Jurkatmock, JurkatWTRHOA and JurkatG17V cells were stimulated in the presence or absence of Dynabeads Human T-activator CD3/CD28. (c) IL-2 gene expression based on real-time PCR. (d) Effect of dasatinib treatment on IL-2 expression in JurkatG17V cells. Cells were harvested at 3 h. The mean±s.d. from triplicate samples is shown.
We also assessed NFAT activity in Jurkat cells transiently transduced with the NFAT response element reporter plus WT VAV1 or VAV1–STAP2, VAV1 p.173_177del, p.165_174del and p.Pro615Leu mutant cDNAs with or without TCR stimulation. In unstimulated conditions, the VAV1–STAP2 construct promoted induced NFAT activity in Jurkat cells as the previously reported fusions, VAV1–MYO1F and VAV1–S100A729 did, whereas the other mutants and WT VAV1 did not (Supplementary Figures 10a and 11). Under TCR stimulation, NFAT activity was enhanced by transduction of WT VAV1 relative to mock control cells, whereas all VAV1 mutants had a greater enhancement effect than did WT VAV1 (Supplementary Figure 10a). Dasatinib treatment abrogated NFAT activity in Jurkat cells transduced with either WT or mutant VAV1 (Supplementary Figure 10b).
G17V RHOA and VAV1–STAP2 enhances IL-2 mRNA expression
IL-2 is a pivotal NFAT target gene.30 We observed increased IL-2 mRNA expression following TCR stimulation of Jurkatmock, peaking at 3 h and decreasing to slightly above basal levels by 6 h (Figure 6c). Such TCR stimulation-dependent IL-2 expression was markedly enhanced by G17V RHOA, whereas WT RHOA rather repressed TCR stimulation-dependent IL-2 mRNA expression (Figure 6c). Dasatinib almost completely suppressed IL-2 mRNA induction by TCR stimulation in JurkatG17V cells at doses that suppressed VAV1 phosphorylation (Figure 6d).
We also examined IL-2 expression in JurkatVAV1–STAP2, JurkatWTVAV1 and Jurkatmock cells in the presence or absence of TCR stimulation. IL-2 expression under TCR stimulation was higher in JurkatVAV1–STAP2 than in JurkatWTVAV1 or Jurkat mock control cells (Supplementary Figure 12a). IL-2 induction by TCR stimulation in JurkatVAV1–STAP2 was dose-dependently inhibited by dasatinib treatment (Supplementary Figure 12b).
Enrichment of cytokine- or chemokine-related signaling by G17V RHOA expression
We next performed mRNA sequencing analysis to examine effects of G17V RHOA on gene expression using RNA prepared from Jurkat cells inducibly expressing WT RHOA or G17V RHOA, or mock transduced, after CD3 and CD28 stimulation. Gene Set Enrichment Analysis demonstrated that cytokine–cytokine receptor interactions, chemokine signaling and TCR signaling pathways were significantly enriched at a false discovery rate q-value of <0.25 for cells expressing WT RHOA or for mock-transduced cells (Figure 7, Supplementary Figure 13 and Supplementary Table 6).
Transcriptome analysis of JurkatG17V and JurkatWTRHOA cells. Gene set enrichment analysis (GSEA) for Jurkat cells inducibly overexpressing WT or G17V RHOA or mock-transfected cells (n=2 each). Representative differentially enriched pathways include (a) cytokine–cytokine receptor interactions, (b) chemokine signaling or (c) TCR signaling and refer to KEGG gene sets (C2) shown.
AITL samples harboring RHOA or VAV1 mutations show enhanced VAV1 Tyr174 phosphorylation
To determine whether VAV1 activation occurs in AITL tumor cells, we stained 26 human lymphoma samples using an antibody to VAV1 phosphorylated at Tyr174 (p-VAV1). In 12 AITL samples, all 8 samples with RHOA or VAV1 mutations were p-VAV1-positive, whereas 4 samples that did not exhibit mutations in either gene were unstained (P<0.05) (Supplementary Table 7). Nine samples from patients with hematologic malignancies other than PTCL were negative for anti-p-VAV1 antibody. To determine the identities of anti-p-VAV1 antibody-positive cells, we performed double fluorescence staining in 11 PTCL samples exhibiting RHOA or VAV1 mutations. The p-VAV1-positive cells costained with antibody to programmed cell death 1 (PDCD1), a marker of AITL tumor cells in 9 of 11 PTCL samples with RHOA or VAV1 mutations (Figure 8 and Supplementary Table 7).
Immunostaining of phosphorylated VAV1 in human AITL samples. Immunofluorescence staining of an AITL sample to detect phosphorylated VAV1. Phosphorylated VAV1 (Tyr174, green) or PDCD1 (red) plus diamidino-2-phenylindole (DAPI) counterstaining. The yellow arrows indicate costained cells in p-VAV1 and PDCD1. Original magnification: × 600 for all panels.
Discussion
In AITL, the G17V RHOA mutation is among the most frequent gene alterations, whereas VAV1 mutations are seen at much lower frequencies. All of these alterations if examined activate VAV1 protein through promoting tyrosine phosphorylation and enhance TCR signaling. The G17V RHOA and VAV1 mutations were mutually exclusive in our cohort, though VAV1 fusions were examined only in a part of samples.
Nonetheless, the physiologic functions of RHOA are presumably abrogated in the G17V mutant, as the protein cannot be converted to the active GTP-bound form. VAV1 mediates TCR signaling as both a GEF to activate small GTPases and as an adaptor to facilitate formation or function of the TCR signaling complex. The results reported here strongly indicate that G17V RHOA modulates VAV1 function as an adaptor (Supplementary Figure 14).
VAV1 mutations seen in AITL also enhance TCR signaling. Recent studies demonstrated that genes encoding members participating in TCR signaling are frequently mutated in AITL and related T-cell lymphomas.28 Among genes encoding TCR signaling molecules, PLCG1 (14.1%),28 CD28 (9.4–11.3%),28, 31, 32 VAV1 (4.7%),28, 29 and FYN (2.9-3.5%)4, 28 are most frequently mutated. ITK,27, 33 VAV1(refs. 27, 29) and CD28(ref. 34) loci are also involved in recurrent chromosomal translocations. This evidence combined with our functional analysis of G17V RHOA suggest that enhanced TCR signaling induces development of T-cell neoplasms, comparable to the idea that enhanced BCR signaling due to mutations is a critical factor in development of B-cell neoplasms.35, 36
In terms of gene expression, AITL tumor cells exhibit profiles comparable to follicular helper T cells,2 and the transcription factors NFAT1 and NFAT2 are essential for follicular helper T-cell development.37 Activation of NFAT by G17V RHOA may promote AITL tumor cell phenotypes. In addition, deregulated expression of ICOS, a signaling factor critical for follicular helper T-cell differentiation,38 reportedly results in development of AITL-like disease in Roquinsan heterozygous mice.39
Several reports show that cyclosporine A, which blocks TCR signaling by inhibiting calcineurin,40 is effective to treat some AITL patients.41, 42 Dasatinib, which inhibits the tyrosine kinase ABL in BCR-ABL-positive chronic myelogenous leukemia and acute lymphoblastic leukemia,43 also inhibits other cytoplasmic and receptor tyrosine kinases.44 We found that aberrant VAV1 activation and subsequent signaling by G17V RHOA and VAV1 mutations are efficiently inhibited by dasatinib treatment. It is now important to conduct clinical studies to evaluate effects of dasatinib in AITL patients. G17V RHOA and VAV1 mutations were seen in AITL samples positive for phospho-VAV1 at a statistically higher frequency. Thus, detection of phospho-VAV1 by immunostaining may serve as a surrogate biomarker for dasatinib sensitivity.
Recent genetic studies identified RHOA mutations in lymphoid malignancies other than AITL, such as Burkitt’s lymphoma45 and ATLL,46 as well as in diffuse-type gastric carcinoma, a nonhematologic malignancy.47 These findings suggest that structural alteration of RHOA by mutation is a common mechanism underlying development of some malignancies. Mutational hot spots, however, differ among diseases: p.Arg5Gln and p.Tyr42Cys are most frequent in Burkitt’s lymphoma45 and gastric carcinomas,47 whereas p.Cys16Arg is most frequent in ATLL.46 Some RHOA mutants upregulate classical RHOA signaling whereas others downregulate it, even in a single disease.46, 48 These outcomes are complex but possibly understandable if these RHOA mutants mediate oncogenesis through mechanisms other than modification of classical RHOA signaling as is shown here in AITL. VAV1 mutations are found in T-cell malignancies other than AITL, such as ATLL,49 PTCL-NOS27 and anaplastic large cell lymphoma,27 as well as in nonhematologic cancers such as those of stomach,47 pancreas50 and melanoma.50 Thus, RHOA and VAV1 mutations are frequent events in several cancers, although downstream mechanisms of these mutations in malignancies other than AITL remain to be elucidated.
In summary, our results demonstrate that the G17V RHOA–VAV1 axis is activated in AITL. This finding contributes to our understanding of AITL mechanisms and to efforts to develop targeted therapies.
References
Swerdlow SH, Campo E, Pileri SA, Harris NL, Stein H, Siebert R et al. The 2016 revision of the World Health Organization classification of lymphoid neoplasms. Blood 2016; 127: 2375–2390.
de Leval L, Gisselbrecht C, Gaulard P . Advances in the understanding and management of angioimmunoblastic T-cell lymphoma. Br J Haematol 2010; 148: 673–689.
Sakata-Yanagimoto M, Enami T, Yoshida K, Shiraishi Y, Ishii R, Miyake Y et al. Somatic RHOA mutation in angioimmunoblastic T cell lymphoma. Nat Genet 2014; 46: 171–175.
Palomero T . Recurrent mutations in epigenetic regulators, RHOA and FYN kinase in peripheral T cell lymphomas. Nat Genet 2014; 46: 166–170.
Yoo HY, Sung MK, Lee SH, Kim S, Lee H, Park S et al. A recurrent inactivating mutation in RHOA GTPase in angioimmunoblastic T cell lymphoma. Nat Genet 2014; 46: 371–375.
Moran-Crusio K, Reavie L, Shih A, Abdel-Wahab O, Ndiaye-Lobry D, Lobry C et al. Tet2 loss leads to increased hematopoietic stem cell self-renewal and myeloid transformation. Cancer Cell 2011; 20: 11–24.
Couronne L, Bastard C, Bernard OA . TET2 and DNMT3A mutations in human T-cell lymphoma. N Engl J Med 2012; 366: 95–96.
Lemonnier F, Couronne L, Parrens M, Jais JP, Travert M, Lamant L et al. Recurrent TET2 mutations in peripheral T-cell lymphomas correlate with TFH-like features and adverse clinical parameters. Blood 2012; 120: 1466–1469.
Cairns RA, Iqbal J, Lemonnier F, Kucuk C, de Leval L, Jais JP et al. IDH2 mutations are frequent in angioimmunoblastic T-cell lymphoma. Blood 2012; 119: 1901–1903.
Sakata-Yanagimoto M . Multistep tumorigenesis in peripheral T cell lymphoma. Int J Hematol 2015; 102: 523–527.
Rougerie P, Delon J . Rho GTPases: masters of T lymphocyte migration and activation. Immunol Lett 2012; 142: 1–13.
Cantrell DA . GTPases and T cell activation. Immunol Rev 2003; 192: 122–130.
Corre I, Gomez M, Vielkind S, Cantrell DA . Analysis of thymocyte development reveals that the GTPase RhoA is a positive regulator of T cell receptor responses in vivo. J Exp Med 2001; 194: 903–914.
Zhang S, Konstantinidis DG, Yang JQ, Mizukawa B, Kalim K, Lang RA et al. Gene targeting RhoA reveals its essential role in coordinating mitochondrial function and thymocyte development. J Immunol 2014; 193: 5973–5982.
Henning SW, Cantrell DA . p56lck signals for regulating thymocyte development can be distinguished by their dependency on Rho function. J Exp Med 1998; 188: 931–939.
Saveliev A, Vanes L, Ksionda O, Rapley J, Smerdon SJ, Rittinger K et al. Function of the nucleotide exchange activity of vav1 in T cell development and activation. Sci Signal 2009; 2: ra83.
Kuhne MR, Ku G, Weiss A . A guanine nucleotide exchange factor-independent function of Vav1 in transcriptional activation. J Biol Chem 2000; 275: 2185–2190.
Tybulewicz VL . Vav-family proteins in T-cell signalling. Curr Opin Immunol 2005; 17: 267–274.
Reynolds LF, Smyth LA, Norton T, Freshney N, Downward J, Kioussis D et al. Vav1 transduces T cell receptor signals to the activation of phospholipase C-gamma1 via phosphoinositide 3-kinase-dependent and -independent pathways. J Exp Med 2002; 195: 1103–1114.
Wu J, Katzav S, Weiss A . A functional T-cell receptor signaling pathway is required for p95vav activity. Mol Cell Biol 1995; 15: 4337–4346.
Katzav S . Vav1: a hematopoietic signal transduction molecule involved in human malignancies. Int J Biochem Cell Biol 2009; 41: 1245–1248.
Aghazadeh B, Lowry WE, Huang XY, Rosen MK . Structural basis for relief of autoinhibition of the Dbl homology domain of proto-oncogene Vav by tyrosine phosphorylation. Cell 2000; 102: 625–633.
Amarasinghe GK, Rosen MK . Acidic region tyrosines provide access points for allosteric activation of the autoinhibited Vav1 Dbl homology domain. Biochemistry 2005; 44: 15257–15268.
Yu B, Martins IR, Li P, Amarasinghe GK, Umetani J, Fernandez-Zapico ME et al. Structural and energetic mechanisms of cooperative autoinhibition and activation of Vav1. Cell 2010; 140: 246–256.
Barreira M, Fabbiano S, Couceiro JR, Torreira E, Martinez-Torrecuadrada JL, Montoya G et al. The C-terminal SH3 domain contributes to the intramolecular inhibition of Vav family proteins. Sci Signal 2014; 7: ra35.
Arthur WT, Ellerbroek SM, Der CJ, Burridge K, Wennerberg K . XPLN, a guanine nucleotide exchange factor for RhoA and RhoB, but not RhoC. J Biol Chem 2002; 277: 42964–42972.
Boddicker RL, Razidlo GL, Dasari S, Zeng Y, Hu G, Knudson RA et al. Integrated mate-pair and RNA sequencing identifies novel, targetable gene fusions in peripheral T-cell lymphoma. Blood 2016; 128: 1234–1245.
Vallois D, Dobay MP, Morin RD, Lemonnier F, Missiaglia E, Juilland M et al. Activating mutations in genes related to TCR signaling in angioimmunoblastic and other follicular helper T-cell-derived lymphomas. Blood 2016; 128: 1490–1502.
Abate F, da Silva-Almeida AC, Zairis S, Robles-Valero J, Couronne L, Khiabanian H et al. Activating mutations and translocations in the guanine exchange factor VAV1 in peripheral T-cell lymphomas. Proc Natl Acad Sci USA 2017; 114: 764–769.
Muller MR, Rao A . NFAT, immunity and cancer: a transcription factor comes of age. Nat Rev Immunol 2010; 10: 645–656.
Esensten JH, Helou YA, Chopra G, Weiss A, Bluestone JA . CD28 costimulation: from mechanism to therapy. Immunity 2016; 44: 973–988.
Lee SH, Kim JS, Kim J, Kim SJ, Kim WS, Lee S et al. A highly recurrent novel missense mutation in CD28 among angioimmunoblastic T-cell lymphoma patients. Haematologica 2015; 100: e505–e507.
Streubel B, Vinatzer U, Willheim M, Raderer M, Chott A . Novel t(5;9)(q33;q22) fuses ITK to SYK in unspecified peripheral T-cell lymphoma. Leukemia 2006; 20: 313–318.
Yoo HY, Kim P, Kim WS, Lee SH, Kim S, Kang SY et al. Frequent CTLA4-CD28 gene fusion in diverse types of T-cell lymphoma. Haematologica 2016; 101: 757–763.
Young RM, Shaffer AL 3rd, Phelan JD, Staudt LM . B-cell receptor signaling in diffuse large B-cell lymphoma. Semin Hematol 2015; 52: 77–85.
Wilcox RA . A three-signal model of T-cell lymphoma pathogenesis. Am J Hematol 2016; 91: 113–122.
Martinez GJ, Hu JK, Pereira RM, Crampton JS, Togher S, Bild N et al. Cutting edge: NFAT transcription factors promote the generation of follicular helper T cells in response to acute viral infection. J Immunol 2016; 196: 2015–2019.
Yu D, Tan AH, Hu X, Athanasopoulos V, Simpson N, Silva DG et al. Roquin represses autoimmunity by limiting inducible T-cell co-stimulator messenger RNA. Nature 2007; 450: 299–303.
Ellyard JI, Chia T, Rodriguez-Pinilla SM, Martin JL, Hu X, Navarro-Gonzalez M et al. Heterozygosity for Roquinsan leads to angioimmunoblastic T-cell lymphoma-like tumors in mice. Blood 2012; 120: 812–821.
Kapturczak MH, Meier-Kriesche HU, Kaplan B . Pharmacology of calcineurin antagonists. Transplant Proc 2004; 36 (2 Suppl): 25S–32S.
Advani R, Horwitz S, Zelenetz A, Horning SJ . Angioimmunoblastic T cell lymphoma: treatment experience with cyclosporine. Leuk Lymphoma 2007; 48: 521–525.
Chen XG, Huang H, Tian Y, Guo CC, Liang CY, Gong YL et al. Cyclosporine, prednisone, and high-dose immunoglobulin treatment of angioimmunoblastic T-cell lymphoma refractory to prior CHOP or CHOP-like regimen. Chin J Cancer 2011; 30: 731–738.
Talpaz M, Shah NP, Kantarjian H, Donato N, Nicoll J, Paquette R et al. Dasatinib in imatinib-resistant Philadelphia chromosome-positive leukemias. N Engl J Med 2006; 354: 2531–2541.
Montero JC, Seoane S, Ocana A, Pandiella A . Inhibition of SRC family kinases and receptor tyrosine kinases by dasatinib: possible combinations in solid tumors. Clin Cancer Res 2011; 17: 5546–5552.
Rohde M, Richter J, Schlesner M, Betts MJ, Claviez A, Bonn BR et al. Recurrent RHOA mutations in pediatric Burkitt lymphoma treated according to the NHL-BFM protocols. Genes Chromosomes Cancer 2014; 53: 911–916.
Nagata Y, Kontani K, Enami T, Kataoka K, Ishii R, Totoki Y et al. Variegated RHOA mutations in adult T-cell leukemia/lymphoma. Blood 2015; 127: 596–604.
Kakiuchi M, Nishizawa T, Ueda H, Gotoh K, Tanaka A, Hayashi A et al. Recurrent gain-of-function mutations of RHOA in diffuse-type gastric carcinoma. Nat Genet 2014; 46: 583–587.
Ishikawa S . Opposite RHOA functions within the ATLL category. Blood 2016; 127: 524–525.
Kataoka K, Nagata Y, Kitanaka A, Shiraishi Y, Shimamura T, Yasunaga J et al. Integrated molecular analysis of adult T cell leukemia/lymphoma. Nat Genet 2015; 47: 1304–1315.
Katzav S . Vav1: A Dr. Jekyll and Mr. Hyde protein—good for the hematopoietic system, bad for cancer. Oncotarget 2015; 6: 28731–28742.
Acknowledgements
We thank N Obara, Y Yokoyama, N Kurita and Y Hasegawa for contributing to sample collection and banking. We also thank Y Sakashita and T Takahashi for technical assistance. We are grateful to Teressa Palomero for providing us with VAV1 fusion cDNAs and Naomichi Arima for SU9T01 cells. This work was supported by Grants-in-Aid for Scientific Research (KAKENHI) from the Ministry of Education, Culture, Sports, Science and Technology of Japan (25112703, 15H01504 and 16H02660 to SC and JP16K15497 to MS-Y) and the Project for Cancer Research and Therapeutic Evolution (P-CREATE) from the Japan Agency for Medical Research and Development, AMED, to SC. Mass spectrometry was supported by NIH SIG 1S10OD016328 to P Gershon. This study was partly supported by TaNeDS program (Daiichi Sankyo).
Author contributions
M F, MS-Y and SC wrote the manuscript; MF, MS-Y, SN, DK, M K, ST, K F and TE contributed to functional analysis; P Gershon performed mass spectrometry; MM, KY and SO performed mRNA sequencing; MF, HM and KO performed immunostaining; KM, NN, KT, KI, K Fujimoto, TT and P Gaulard contributed to sample collection and vital discussion.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
SC received research funding from Bristol-Meyer Squibb that markets dasatinib.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Fujisawa, M., Sakata-Yanagimoto, M., Nishizawa, S. et al. Activation of RHOA–VAV1 signaling in angioimmunoblastic T-cell lymphoma. Leukemia 32, 694–702 (2018). https://doi.org/10.1038/leu.2017.273
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2017.273
This article is cited by
-
Novel clinical risk stratification and treatment strategies in relapsed/refractory peripheral T-cell lymphoma
Journal of Hematology & Oncology (2024)
-
Tumor heterogeneity and immune-evasive T follicular cell lymphoma phenotypes at single-cell resolution
Leukemia (2023)
-
Mature T-cell and NK-cell lymphomas: updates on molecular genetic features
International Journal of Hematology (2023)
-
Updates in the Classification of T-cell Lymphomas and Lymphoproliferative Disorders
Current Hematologic Malignancy Reports (2023)
-
Advances in the pathogenesis and therapeutic strategies of angioimmunoblastic T-cell lymphoma
Clinical and Experimental Medicine (2023)