Abstract
Objective:
To examine outcomes of neonates based on the mode and intensity of resuscitation received in the delivery room (DR).
Study Design:
A retrospective study of 439 infants with birth weight ⩽1500 g receiving DR resuscitation at two hospital centers in Philadelphia, Pennsylvania.
Results:
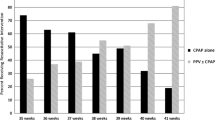
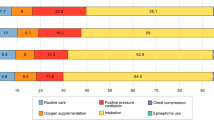
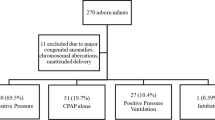
Of 439 infants, 22 (5%) received routine care, 188 (43%) received noninvasive positive pressure ventilation (PPV) and 229 (52%) received endotracheal tube (ETT) intubation in the DR. Adjusted odds for respiratory distress syndrome was associated with lower rates in infants requiring lower intensity of DR resuscitation (P<0.001). Noninvasive PPV vs ETT was associated with decreased odds of developing intraventricular hemorrhage and retinopathy of prematurity (P<0.05). Routine vs noninvasive PPV or ETT had decreased odds of developing bronchopulmonary dysplasia (P<0.05).
Conclusion:
Decreased intensity of DR resuscitation was associated with a decreased risk of specific morbidities.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Kattwinkel J, Perlman JM, Aziz K, Colby C, Fairchild K, Gallagher J et al. Neonatal resuscitation: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122: S909–S919.
American Academy of Pediatrics and American Heart Association. Resuscitation of Babies Born Preterm. NRP Neonatal Resuscitation Textbook, 6th edn. American Academy of Pediatrics: Elk Grove Village, IL, USA, 2011, pp 267–282.
Bhandari V . Postnatal inflammation in the pathogenesis of bronchopulmonary dysplasia. Birth Defects Res A 2014; 100: 189–201.
O’Donnell CP, Schmolzer GM . Resuscitation of preterm infants—delivery room interventions and their effect on outcomes. Clin Perinatol 2012; 34 (4): 857–869.
SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Finer NN SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Carlo WA SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Walsh MC SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Rich W SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Gantz MG SUPPORT Study of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Laptook AR et al. Early CPAP versus surfactant in extremely preterm neonates. N Engl J Med 2010; 362: 1970–1979.
Jobe AH, Bancalari E . Bronchopulmonary dysplasia. Am J Respir Crit Care Med 2001; 163: 1723–1729.
Burstein J, Papile LA, Burstein R . Intraventricular hemorrhage and hydrocephalus in premature newborns: a prospective study with CT. Am J Roentgenol 1979; 132: 631–635.
An International Classification for Retinopathy of Prematurity. The Committee for the Classification of Retinopathy of Prematurity. Arch Ophthalmol 1984; 102: 1130–1134.
Volpe JJ. Hypoxic ischemic encephalopathy: neuropathology and pathogenesis. In: Neurology of the Newborn, 3rd edn. WB Saunders: Philadelphia, PA, USA, 1987, pp 291–299..
Bell MJ . Neonatal necrotizing enterocolitis therapeutic decisions based on clinical staging. Ann Surg 1978; 187: 1–7.
R Core Team R: A Language and Environment for Statistical Computing. R Foundation for Statistical Computing: Vienna, Austria; URL https://www.R-project.org/ 2015.
Wyckoff MH, Salhab WA, Heyne RJ, Kendrick DE, Stoll BJ, Laptook AR National Institute of Child Health and Human Development Neonatal Research Network. Outcome of extremely low birth weight infants who received delivery room cardiopulmonary resuscitation. J Pediatr 2012; 160: 239–244.
Soraisham AS, Lodha AK, Singhal N, Aziz K, Yang J, Lee SK et al. Neonatal outcomes following extensive cardiopulmonary resuscitation in the delivery room for infants born at less than 33 weeks gestational age. Resuscitation 2014; 85: 238–243.
DeMauro SB, Roberts RS, Davis RS, Davis P, Alvaro R, Bairam A et al. Impact of delivery room resuscitation on outcomes up to 18 months in very low birth weight infants. J Pediatr 2011; 159: 546–550.
Handley SC, Sun Y, Wyckoff MH, Lee HC . Outcomes of extremely preterm infants after delivery room cardio pulmonary resuscitation in a population-based cohort. J Perinatol 2015; 35: 379–383.
Shah PS . Extensive cardiopulmonary resuscitation for VLBW and ELBW infants: a systematic review and meta-analyses. J Perinatol 2009; 29: 655–661.
Jiang S, Lyu Y, Ye XY, Monterrosa L, Shah PS, Lee SK . Intensity of delivery room resuscitation and neonatal outcomes in infants born at 33 to 36 weeks’ gestation. J Perinatol 2016; 36: 100–105.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Bashir, A., Bird, B., Wu, L. et al. Neonatal outcomes based on mode and intensity of delivery room resuscitation. J Perinatol 37, 1103–1107 (2017). https://doi.org/10.1038/jp.2017.102
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.102
This article is cited by
-
Electrocardiogram for heart rate evaluation during preterm resuscitation at birth: a randomized trial
Pediatric Research (2022)