Abstract
Objective:
Infants in neonatal intensive care units (NICUs) are vulnerable to a variety of infections, and occupancy in the unit may correlate with risk of infection.
Study Design:
A retrospective cohort of infants admitted to the NICUs between 1997 and 2014. Survival analysis was used to model the relative hazard of sepsis infection in relation to two measures of occupancy: 1) the average census and 2) proportion of infants <32 weeks gestation in the unit.
Result:
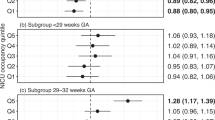
There were 446 (2.3%) lab-confirmed cases of bacterial or fungal sepsis, which steadily declined over time. For each additional percentage of infants <32 weeks gestation, there was an increased hazard of 2% (hazard ratio 1.02, 95% confidence interval: 1.00, 1.03) over their NICU hospitalization. Census was not associated with risk for infection.
Conclusion:
During times of a greater proportion of infants <32 weeks gestation in the NICU, enhanced infection-control interventions may be beneficial to further reduce the incidence of infections.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Shane AL, Stoll BJ . Recent developments and current issues in the epidemiology, diagnosis, and management of bacterial and fungal neonatal sepsis. Am J Perinatol 2013; 30 (2): 131–141.
Cohen-Wolkowiez M, Moran C, Benjamin DK, Cotten CM, Clark RH, Benjamin DK Jr et al. Early and late onset sepsis in late preterm infants. Pediatr Infect Dis J 2009; 28 (12): 1052–1056.
Hilde Verstraete E, De Coen K, Vogelaers D, Blot S . Risk factors for health care-associated sepsis in critically ill neonates stratified by birth weight. Pediatr Infect Dis J 2015; 34 (11): 1180–1186.
Helder OK, Brug J, van Goudoever JB, Looman CW, Reiss IK, Kornelisse RF . Sequential hand hygiene promotion contributes to a reduced nosocomial bloodstream infection rate among very low-birth weight infants: an interrupted time series over a 10-year period. Am J Infect Control 2014; 42 (7): 718–722.
Shepherd EG, Kelly TJ, Vinsel JA, Cunningham DJ, Keels E, Beauseau W et al. Significant reduction of central-line associated bloodstream infections in a network of diverse neonatal nurseries. J Pediatr 2015; 167 (1): 41–6.e1-3.
Bentlin MR, Rugolo LM, Ferrari LS, Brazilian Neonatal Research Network (Rede Brasileira de Pesquisas Neonatais). Practices related to late-onset sepsis in very low-birth weight preterm infants. J Pediatr (Rio J) 2015; 91 (2): 168–174.
Julian S, Burnham CA, Sellenriek P, Shannon WD, Hamvas A, Tarr PI et al. Impact of neonatal intensive care bed configuration on rates of late-onset bacterial sepsis and methicillin-resistant Staphylococcus aureus colonization. Infect Control Hosp Epidemiol 2015; 25: 1–10.
Kaier K, Meyer E, Dettenkofer M, Frank U . Epidemiology meets econometrics: using time-series analysis to observe the impact of bed occupancy rates on the spread of multidrug-resistant bacteria. J Hosp Infect 2010; 76 (2): 108–113.
Sherenian M, Profit J, Schmidt B, Suh S, Xiao R, Zupancic JA et al. Nurse-to-patient ratios and neonatal outcomes: a brief systematic review. Neonatology 2013; 104 (3): 179–183.
van den Hoogen A, Gerards LJ, Verboon-Maciolek MA, Fleer A, Krediet TG . Long-term trends in the epidemiology of neonatal sepsis and antibiotic susceptibility of causative agents. Neonatology 2010; 97 (1): 22–28.
Benjamin DK Jr, Stoll BJ, Gantz MG, Walsh MC, Sánchez PJ, Das A et al. Neonatal candidiasis: epidemiology, risk factors, and clinical judgment. Pediatrics 2010; 126 (4): e865–e873.
Kleinbaum D, Klein M . Survival Analysis. Springer Science+Business Media: New York, NY, USA, 2012.
Rothman KJ, Greenland S, Lash TL (eds). Modern Epidemiology. Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2008.
Hornik CP, Fort P, Clark RH, Watt K, Benjamin DK Jr, Smith PB et al. Early and late onset sepsis in very-low-birth-weight infants from a large group of neonatal intensive care units. Early Hum Dev 2012; 88 (Suppl 2): S69–S74.
Mahieu LM, De Muynck AO, Ieven MM, De Dooy JJ, Goossens HJ, Van Reempts PJ . Risk factors for central vascular catheter-associated bloodstream infections among patients in a neonatal intensive care unit. J Hosp Infect 2001; 48 (2): 108–116.
Schulman J, Stricof R, Stevens TP, Horgan M, Gase K, Holzman IR et al. Statewide NICU central-line-associated bloodstream infection rates decline after bundles and checklists. Pediatrics 2011; 127 (3): 436–444.
Austin N, Cleminson J, Darlow BA, McGuire W . Prophylactic oral/topical non-absorbed antifungal agents to prevent invasive fungal infection in very low birth weight infants. Cochrane Database Syst Rev 2015; 10: CD003478.
Mukerji A, Narciso J, Moore C, McGeer A, Kelly E, Shah V . An observational study of the hand hygiene initiative: a comparison of preintervention and postintervention outcomes. BMJ Open 2013; 3 (5): 1–7.
Pessoa-Silva CL, Hugonnet S, Pfister R, Touveneau S, Dharan S, Posfay-Barbe K et al. Reduction of health care associated infection risk in neonates by successful hand hygiene promotion. Pediatrics 2007; 120 (2): e382–e390.
Won SP, Chou HC, Hsieh WS, Chen CY, Huang SM, Tsou KI et al. Handwashing program for the prevention of nosocomial infections in a neonatal intensive care unit. Infect Control Hosp Epidemiol 2004; 25 (9): 742–746.
Kaufman DA, Blackman A, Conaway MR, Sinkin RA . Nonsterile glove use in addition to hand hygiene to prevent late-onset infection in preterm infants: randomized clinical trial. JAMA Pediatr 2014; 168 (10): 909–916.
Testoni D, Hayashi M, Cohen-Wolkowiez M, Benjamin DK Jr, Lopes RD, Clark RH et al. Late-onset bloodstream infections in hospitalized term infants. Pediatr Infect Dis J 2014; 33 (9): 920–923.
Popoola VO, Budd A, Wittig SM, Ross T, Aucott SW, Perl TM et al. Methicillin-resistant Staphylococcus aureus transmission and infections in a neonatal intensive care unit despite active surveillance cultures and decolonization: challenges for infection prevention. Infect Control Hosp Epidemiol 2014; 35 (4): 412–418.
Boehmer TK, Bamberg WM, Ghosh TS, Cronquist A, Fornof ME, Cichon MK et al. Health care-associated outbreak of Salmonella Tennessee in a neonatal intensive care unit. Am J Infect Control 2009; 37 (1): 49–55.
Cimiotti JP, Haas J, Saiman L, Larson EL . Impact of staffing on bloodstream infections in the neonatal intensive care unit. Arch Pediatr Adolesc Med 2006; 160 (8): 832–836.
Parry GJ, Tucker JS, Tarnow-Mordi WO, UK Neonatal Staffing Study Group. Relationship between probable nosocomial bacteraemia and organisational and structural factors in UK neonatal intensive care units. Qual Saf Health Care 2005; 14 (4): 264–269.
Gagliardi L, Corchia C, Bellù R, Coscia A, Zangrandi A, Zanini R . What we talk about when we talk about NICUs: infants' acuity and nurse staffing. J Matern Fetal Neonatal Med 2015; 19: 1–20.
Petrova A, Mehta R, Anwar M, Hiatt M, Hegyi T . Impact of race and ethnicity on the outcome of preterm infants below 32 weeks gestation. J Perinatol 2003; 23 (5): 404–408.
Perencevich EN, McGregor JC, Shardell M, Furuno JP, Harris AD, Morris JG Jr et al. Summer peaks in the incidences of Gram-negative bacterial infection among hospitalized patients. Infect Control Hosp Epidemiol 2008; 29 (12): 1124–1131.
Al-Hasan MN, Lahr BD, Eckel-Passow JE, Baddour LM . Seasonal variation in Escherichia coli bloodstream infection: a population-based study. Clin Microbiol Infect 2009; 15 (10): 947–950.
McDonald LC, Banerjee SN, Jarvis WR . Seasonal variation of Acinetobacter infections: 1987-1996. Nosocomial Infections Surveillance System. Clin Infect Dis 1999; 29 (5): 1133–1137.
Anderson DJ, Richet H, Chen LF, Spelman DW, Hung YJ, Huang AT et al. Seasonal variation in Klebsiella pneumoniae bloodstream infection on 4 continents. J Infect Dis 2008; 197 (5): 752–756.
Acknowledgements
We thank Gina Moore, Christiana Care Health System, for her assistance with data abstraction and interpretation and Josh Kessler for his assistance in data collection. This work was supported by INBRE grant NIH-NIGMS (p20 BM103446).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Goldstein, N., Eppes, S., Ingraham, B. et al. Characteristics of late-onset sepsis in the NICU: does occupancy impact risk of infection?. J Perinatol 36, 753–757 (2016). https://doi.org/10.1038/jp.2016.71
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.71
This article is cited by
-
Fungi in the indoor air of critical hospital areas: a review
Aerobiologia (2021)