Abstract
Objective:
To describe the hemodynamic changes that occur with sodium bicarbonate (NaHCO3) administration in premature neonates.
Study Design:
This retrospective study included premature neonates 23 to 31+6 weeks of gestational age who underwent continuous cardiac and cerebral monitoring as participants in prospective trials at our institution, and who received NaHCO3 infused over 30 min in the first 24 h of life. Blood pressure (BP), heart rate, cardiac output (CO), SpO2 and cerebral oximetry (StO2) were captured every 2 s. A baseline was established for all continuous data and averaged over the 10 min before NaHCO3 administration. Baseline was compared with measurements over 10 min epochs until 80 min after administration. Arterial blood gases before and within 1 h of administration were also compared. Significance was set at P<0.05.
Results:
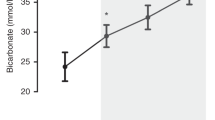
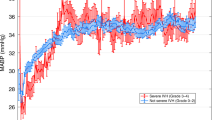
A total of 36 subjects received NaHCO3 (1.3±0.3 mEq kg−1) in the first 24 h (14±8.5 h) of life. NaHCO3 administration increased pH (7.23 vs 7.28, P<0.01) and decreased base deficit (−8.9 vs −6.8, P<0.01) and PaCO2 (45 vs 43 mm Hg, P<0.05). There was a transient but significant (P<0.05) decrease in systemic BP coinciding with an increase in cerebral oxygenation without an increase in oxygen extraction. CO did not change.
Conclusion:
Early postnatal NaHCO3 administration does not acutely improve CO but does cause transient fluctuations in cerebral and cardiovascular hemodynamics in extremely premature infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Stevens CP, Raz S, Sander CJ . Peripartum hypoxic risk and cognitive outcome: a study of term and preterm birth children at early school age. Neuropsychology 1999; 13: 598–608.
Orchard CH, Kentish JC . Effects of changes of pH on the contractile function of cardiac muscle. Am J Physiol 1990; 258: C967–C981.
Goldstein RF, Thompson RJ, Ochler JM, Brazy JE . Influence of acidosis, hypoxemia and hypotension on neurodevelopmental outcome in very low birthweight infants. Pediatrics 1995; 95: 238–243.
Lokesh L, Kumar P, Murki S, Narang A . A randomized controlled trial of sodium bicarbonate in neonatal resuscitation—effect on immediate outcome. Resuscitation 2004; 60: 219–223.
Corbet AJ, Adams JM, Kenny JD, Kennedy J, Rudolph AJ . Controlled trial of bicarbonate therapy in high-risk premature newborn infants. J Pediatr 1977; 91: 771–776.
Berg CS, Barnette AR, Myers BJ, Shimony MK, Barton AW, Inder TE . Sodium bicarbonate administration and outcome in preterm infants. J Pediatr 2010; 157: 684–687.
Aschner JL, Poland RL . Sodium bicarbonate: basically useless therapy. Pediatrics 2008; 122: 831–835.
Mintzer JP, Parvez B, Alpan G, La Gamma EF . Effects of sodium bicarbonate correction of metabolic acidosis on regional tissue oxygenation in very low birth weight neonates. J Perinatol 2015; 35: 601–606.
Fanconi S, Burger R, Ghelfi D, Uehlinger J, Arbenz U . Hemodynamic effects of sodium bicarbonate in critically ill neonates. Intensive Care Med 1993; 19: 65–69.
Lou HC, Lassen NA, Friis-Hansen B . Decreased cerebral blood flow after administration of sodium bicarbonate in the distressed newborn infant. Acta Neurol Scand 1978; 57: 239–247.
van Alfen-van der Velden AA, Hopman JC, Klaessens JH, Feuth T, Sengers RC, Liem KD . Effects of rapid versus slow infusion of sodium bicarbonate on cerebral hemodynamics and oxygenation in preterm infants. Biol Neonate 2006; 90: 122–127.
Katheria AC, Sauberan JB, Akotia D, Rich W, Durham J, Finer NN . A pilot randomized controlled trial of early versus routine caffeine in extremely premature infants. Am J Perinatol 2015; 32: 879–886.
Katheria AC, Truong G, Cousins L, Oshiro B, Finer NN . Umbilical cord milking versus delayed cord clamping in preterm infants. Pediatrics 2015; 136: 61–69.
Katheria A, Poeltler D, Durham J, Steen J, Rich W, Arnell K et al. Neonatal resuscitation with an intact cord: a randomized controlled trial. J Pediatr 2016; 178: 75–80e3.
The Neuprem Trial: neuromonitoring of preterm newborn brain during birth resuscitation. Available athttps://clinicaltrials.gov/ct2/show/NCT02605733.
Mintzer JP, Parvez B, Chelala M, Alpan G, LaGamma EF . Quiescent variability of cerebral, renal, and splanchnic regional tissue oxygenation in very low birth weight neonates. J Neonatal Perinatal Med 2014; 7: 199–206.
Fujioka T, Takami T, Ishii H, Kondo A, Sunohara D, Kawashima H . Difference in cerebral and peripheral hemodynamics among term and preterm infants during the first three days of life. Neonatology 2014; 106: 181–187.
Cooper DJ, Walley KR, Wiggs BR, Russell JA . Bicarbonate does not improve hemodynamics in critically ill patients who have lactic acidosis. Ann Intern Med 1990; 112: 492–498.
Mathieu D, Neviere R, Billard V, Fleyfel M, Wattel F . Effects of bicarbonate therapy on hemodynamics and tissue oxygenation in patients with lactic acidosis: a prospective, controlled clinical study. Crit Care Med 1991; 19: 1352–1356.
Gephart SM, Spitzer AR, Effken JA, Dodd E, Halpern M, McGrath JM . Discrimination of GutCheckNEC: a clinical risk index for necrotizing enterocolitis. J Perinatol 2014; 34: 468–475.
Thome UH, Genzel-Boroviczeny O, Bohnhorst B, Schmid M, Fuchs H, Rohde O et al. Permissive hypercapnia in extremely low birthweight infants (PHELBI):a randomized controlled multicenter trial. Lancet Respir Med 2015; 3: 534–543.
Huseman D, Metze B, Walch E, Bührer C . Laboratory markers of perinatal acidosis are poor predictors of neurodevelopmental impairment in very low birth weight infants. Early Hum Dev 2011; 87: 677–681.
Diviney M, Pinnamaneni R, Murphy JF, Lynch B, Rushe H, Madigan C et al. Neurodevelopmental outcome at seven years in term, acidotic newborns. Ir Med J 2015; 108: 106–109.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Katheria, A., Brown, M., Hassan, K. et al. Hemodynamic effects of sodium bicarbonate administration. J Perinatol 37, 518–520 (2017). https://doi.org/10.1038/jp.2016.258
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.258
This article is cited by
-
The effects of sodium bicarbonate infusion on cerebrovascular function in newborn pigs
Pediatric Research (2022)
-
Use of intravenous sodium bicarbonate in neonatal intensive care units in Italy: a nationwide survey
Italian Journal of Pediatrics (2021)
-
Versorgung und Reanimation des Neugeborenen nach der Geburt
Notfall + Rettungsmedizin (2021)