Abstract
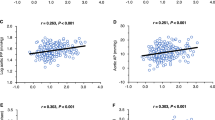
Salt-sensitivity is associated with a more severe target organ injury and higher mortality, even in normotensive subjects. As endothelial dysfunction is predictive for future cardiovascular events, we evaluated whether normotensive salt-sensitive (NSS) subjects have more pronounced endothelial dysfunction compared with normotensive salt-resistant (NSR) subjects. Normotensive subjects (n=99, aged 25–50 years) were selected from a rural community in northern China. Salt sensitivity was assigned if mean BP increased by ⩾10% from a 1-week high salt (18 g/day, NaCl) to low-salt diet (3 g/day, NaCl). Endothelial function was assessed by testing the flow-mediated dilatation (FMD) of the brachial artery using high-resolution ultrasound, as well as nitrogen oxide (NOx) levels, in plasma and urine at baseline. Blood pressure at baseline was similar between NSS and NSR subjects, but diverged during salt intervention. Furthermore, FMD was significantly lower in 17 NSS subjects (10.2±2.5 vs 14.5±1.6%, P=0.037) compared with NSR subjects. In addition, average plasma NOx levels were lower in NSS subjects than NSR subjects (61.2±3.23 μM vs 82.5±1.61 μM, P=0.034). Moreover, Both FMD and plasma NOx levels were negatively correlated with the degree of salt sensitivity (r=−0.435 and r=−0.459, respectively, P<0.01). However, there was no difference in urine NOx between the two groups. Our study indicates that endothelial dysfunction could contribute to the long-term higher levels of target organ injury and higher mortality observed in NSS subjects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Muntzel M, Drüeke T . A comprehensive review of the salt and blood pressure relationship. Am J Hypertens 1992; 5: 1S–42S.
Weinberger MH . Salt sensitivity of blood pressure in humans. Hypertension 1996; 27: 481–490.
Weinberger MH, Fineberg NS, Fineberg SD et al. Salt sensitivity, pulse pressure, and death in normal and hypertensive humans. Hypertension 2001; 37: 429–432.
Atsushi M, Takashi U . Sodium sensitivity and cardiovascular events in patients with essential hypertension[J]. Lancet 1997; 350: 1734–1737.
Vanhoutte PM . Endothelium and control of vascular funcion. State of the Art lecture. Hypertension 1989; 13: 658–667.
Luscher TF . Imbalance of endothelium-derived relaxing and contracting factors. A new concept in hypertension? Am J Hypertens 1990; 3: 317–330.
Facchini F, DoNascimento C, Reaven GM, Yip JW, Ni Ping X, Humphreys M . Blood pressure, sodium intake, insulin resistance and urinary nitrate excretion. Hypertension 1999; 33: 1008–1012.
Fujiwara N, Osanai T, Kamada T, Katoh T, Takahashi K, Okumura K . Study on the relationship between plasma nitrite and nitrate level and salt sensitivity in human hypertension. Circulation 2000; 101: 856–861.
Miyoshi A, Suzuki H, Fujiwara M, Masai M, Iwasaki T . Impairment of endothelial function in salt-sensitive hypertension in humans. Am J Hypertens 1997; 10: 1083–1090.
Celermajer DS, Sorensen KE, Gooch VM, Spiegelhalter DJ, Miller OI, Sullivan ID, Lloyd JK, Deanfield JE . Non-invasive detection of endothelial dysfunction in children and adults at risk of atherosclerosis. Lancet 1992; 340: 1111–1115.
Marguerite ME, Mary BE, Mary JM, Elisa YC, Monique CS, Steven MP et al. Antioxidant vitamins C and E improve endothelial function in children with hyperlipidemia: Endothelial Assessment of Risk from Lipids in Youth (EARLY) Trial. Circulation 2003; 108: 1059–1063.
Mullen MJ, Kharbanda RK, Cross J, Donald AE, Taylor M, Vallance P et al. Heterogenous nature of flow-mediated dilatation in human conduit arteries in vivo: relevance to endothelial dysfunction in hypercholesterolemia. Circ Res 2001; 88: 145–151.
Soga J, Nishioka K, Nakamura S, Umemura T, Jitsuiki D, Hidaka T et al. Measurement of flow-mediated vasodilation of the brachial artery: a comparison of measurements in the seated and supine positions. Circ J 2007; 71: 736–740.
Gokce N, Keaney Jr JF, Hunter LM, Watkins MT, Menzoian JO, Vita JA . Risk stratification for postoperative cardiovascular events via noninvasive assessment of endothelial function: a prospective study. Circulation 2002; 105: 1567–1572.
Dickinson KM, Keogh JB, Clifton PM . Effects of a low-salt diet on flow-mediated dilatation in humans. Am J Clin Nutr. 2009; 89 (2): 485–490.
Bragulat E, de la Sierra A, Antonio MT, Coca A . Endothelial Dysfunction in Salt-Sensitive Essential Hypertension. Hypertension 2001; 37: 444–448.
Fang Y, Mu JJ, He LC, Wang SC, Liu ZQ . Salt loading on plasma asymmetrical dimethylarginine and the protective role of potassium supplement in normotensive salt-sensitive asians. Hypertension. 2006; 48 (4): 724–729.
Mu JJ, Liu ZQ, Liu FQ, Xu XL, Liang YM, Zhu DJ . Family-based randomized trial to detect effects on blood pressure of a salt substitute containing potassium and calcium in hypertensive adolescents. Am J Hyperten, 2009; 22 (9): 943–947.
Raitakari OT, Celermajer DS . Flow-mediated dilatation. Br J Clin Pharmacol 2000; 50 (5): 397–404.
Forte P, Copland M, Smith LM, Milne E, Sutherland J, Benjamin N . Basal nitric oxide synthesis in essential hypertension. Lancet 1997; 349: 837–842.
Fujiwara N, Osanai T, Kamada T, Katoh T, Takahashi K, Okumura K . Study on the relationship between plasma nitrite and nitrate level and salt sensitivity in human hypertension. Circulation 2000; 101: 856–861.
Facchini F, Do Nascimento C, Reaven GM, Yip JW, Ni Ping X, Humphreys M . Blood pressure, sodium intake, insulin resistance and urinary nitrate excretion. Hypertension 1999; 33: 1008–1012.
Tousoulis D, Antoniades C, Stefanadis C . Evaluating endothelial function in humans: a guide to invasive and non-invasive techniques. Heart 2005; 91: 553–558.
Miyoshi A, Suzuki H, Fujiwara M . Impairment of endothelial function in salt-sensitive hypertension in humans. Am J Hypertens 1997; 10: 1083–1090.
Higashi Y, Sasaki S, Nakagawa K, Kimura M, Noma K, Sasaki S et al. Sodium chloride loading does not alter endothelium-dependent vasodilation of forearm vasculature in either salt-sensitive or salt-resistant patients with essential hypertension. Hypertens Res 2001; 27: 6 24(6):711-6.
Muiesan ML, Salvetti M, Paini A, Monteduro C, Galbassini G, Poisa P et al. Prognostic role of flow-mediated dilatation of the brachial artery in hypertensive patients. J Hypertens 2008; 26 (8): 1612–1618.
Avolio A, Grassi G . Flow-mediated dilatation as a biomarker for cardiovascular risk in hypertension. J Hypertens 2008; 26 (8): 1546–1547.
Xu JZ, Zhang Y, Wu SN, Niu WQ, Zhu DL, Gao PJ . Impaired endothelial function in hypertensive patients with target organ damage. J Hum Hypertens 2009; 23 (11): 751–757.
Luft FC, Rankin LI, Bloch R, Weyman AE, Willis LR, Murray RH et al. Cardiovascular and humoral responses to extremes of sodium intake in normal black and white men. Circulation 1979; 60: 697–706.
Wilson DK, Sica DA, Miller SB . Effects of potassium on blood pressure in salt-sensitive and salt-resistant black adolescents. Hypertension 1999; 34: 181–186.
Acknowledgements
This study was supported with grants from Natural Science Foundation of China (NO: 81070218 and 30671160).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Liu, FQ., Mu, JJ., Liu, ZQ. et al. Endothelial dysfunction in normotensive salt-sensitive subjects. J Hum Hypertens 26, 247–252 (2012). https://doi.org/10.1038/jhh.2011.13
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2011.13