Abstract
Atypical hemolytic uremic syndrome (aHUS) is a severe renal disorder that is associated with mutations in genes encoding proteins of the alternative complement pathway. Previously, we identified pathogenic variations in genes encoding complement regulators (CFH, CFI and MCP) in our aHUS cohort. In this study, we screened for mutations in the alternative pathway regulator CFHR5 in 65 aHUS patients by means of PCR on genomic DNA and sequence analysis. Potential pathogenicity of genetic alterations was determined by published data on CFHR5 variants, evolutionary conservation and in silico mutation prediction programs. Detection of serum CFHR5 was performed by western blot analysis and enzyme-linked immunosorbent assay. A potentially pathogenic sequence variation was found in CFHR5 in three patients (4.6%). All variations were located in short consensus repeats that might be involved in binding to C3b, heparin or C-reactive protein. The identified CFHR5 mutations require functional studies to determine their relevance to aHUS, but they might be candidates for an altered genetic profile predisposing to the disease.
Similar content being viewed by others
Introduction
Thrombotic microangiopathies are a spectrum of syndromes associated with thrombocytopenia and multiple organ failure, of which thrombotic thrombocytopenic purpura and the hemolytic uremic syndrome (HUS) are the most common. HUS is characterized by hemolytic anemia, thrombocytopenia and acute renal failure, and is preceded by an infection with Shiga-like producing Escherichia coli (STEC) in 90–95% of the cases.1, 2 Atypical HUS or aHUS, which is not associated with STEC infection, is thought to be caused by dysregulation of the alternative complement pathway in 50–60% of the cases. Loss-of-function mutations have been identified in the regulators factor H (CFH), factor I (CFI), membrane cofactor protein (CD46, also known as MCP) and thrombomodulin, whereas in the complement activation proteins C3 (C3) and factor B (CFB), gain-of-function mutations were found.3, 4, 5, 6, 7, 8, 9 Recently, the presence of auto-antibodies against CFH (αFH) (particularly common in the presence of polymorphic homozygous deletion of CFHR1 and CFHR3 (ΔCFHR1–3)) has been associated with aHUS.10 Genetic variations are of prognostic value for the outcome of renal transplantation and kidney donation.11
CFHR5 is a member of the CFH protein family that consists of six structurally and immunologically related proteins, of which CFHR5 was discovered most recently. The 65 kDa protein contains nine short consensus repeats (SCRs); SCR1 and 2 show homology with the first two SCRs of CFHR1 and CFHR2, SCR3-7 share significant homology with SCR10–14 of CFH, and SCR8–10 are comparable to SCR19 and 20 of CFH.12 The protein is strongly associated with glomerular complement deposits, suggesting a role in complement regulation. It has already been shown that SCRs 5–7 can bind to heparin and C-reactive protein (CRP).13 Furthermore, an inhibition of the C3 convertase activity in the fluid phase, a cofactor activity for CFI-dependent cleavage of C3b to iC3b, and binding to C3b in a dose-dependent and saturable manner was demonstrated, although these characteristics have not been linked to specific SCRs.12, 14 According to Monteferrante et al,15 genetic aberrations in CFHR5 might have a secondary role in the pathogenesis of aHUS.
Genetic aberrations in CFHR5 have already been associated with other glomerular diseases. In dense deposit disease or MPGNII three single-nucleotide polymorphisms (SNPs) have been identified with significantly different allele frequencies in patients;16 in CFHR5 nephropathy a duplication in the gene has been associated with the disease.17 Furthermore, a synonymous SNP might have a protective role in the development of age-related macular degeneration, an eye disease associated with complement dysregulation.18
Previously, a cohort of Dutch and Belgian aHUS patients was screened for mutations in CFH, CFI, CD46 and CFB, and for the presence of αFH. In 31.9% of the patients, complement deficiencies were found.6 More than 4.5% of the patients carried an alteration in more than one gene. For >68% of the cohort, no cause of the disease could be identified yet. In the present study, the gene encoding CFHR5 was screened for genetic aberrations in 65 aHUS patients and CFHR5 levels were evaluated for two of the sequence variations.
Materials and methods
Study population
The research population consisted of 65 aHUS patients, referred to the Paediatric Nephrology Centre of the Radboud University Medical Centre. The patients were of Dutch or Belgian origin with a Caucasian background. In 16 aHUS patients the familial form was identified; the remaining patients are thought to have sporadic aHUS. Permission to study DNA material was given by all patients or their parents.
Genetic analysis of gene encoding CFHR5
Genomic DNA was amplified for CFHR5 (NCBI RefSeq NM_030787.2) by means of PCR; primer data are shown in Table 1. The primers are specific for CFHR5. The amplimers, including the individual exons and the splice donor and acceptor sites, were subjected to double-stranded DNA sequence analysis on an ABI 3130 xl GeneticAnalyzer (Applied Biosystems, Carlsbad, CA, USA). Sequence analysis was performed using Sequencher 4.8 software. Note that the nucleotide and amino-acid numbering begins with the start site ATG and, therefore, includes the signal peptide. Detected genetic aberrations were confirmed on a second PCR product. Genomic DNA from more than 145 healthy, ethnically matched control individuals was used to confirm sequence variations that might be potentially pathogenic. Data from the 1000 Genomes Project (http://www.1000genomes.org), in which almost all known variants with a population frequency of at least 1% are listed, and data from the Exome Variant Server (NHLBI Exome Sequencing Project (ESP), Seattle, WA, USA; http://evs.gs.washington.edu/EVS/, March 2012 accessed), in which results of whole exome sequencing of almost 5400 individuals are provided, was checked for the presence of identified sequence variations as well.
Internal duplication or depletions of the first three exons of CFHR5 and the presence of ΔCFHR1/3 was assessed in mutated patients by multiplex ligation-dependent probe amplification (P236 A1 ARMD mix 1; MRC-Holland, Amsterdam, The Netherlands). Copy number variation was not interrogated in other patients.
In silico evaluation of pathogenicity
Potential pathogenicity of genetic alterations was checked in literature, evolutionary conservation, in silico prediction programs SIFT (Sorting Intolerant From Tolerant; http://sift.jcvi.org/), PolyPhen-2 (Polymorphism Phenotyping v2; http://genetics.bwh.harvard.edu/pph2/) and Align GVGD (http://agvgd.iarc.fr/index.php), and in splice site prediction software (Human Splicing Finder: http://www.umd.be/HSF/). In SIFT, a change resulting in a value below 0.05 was considered to be not tolerated and this change might therefore affect protein function. A high classification in Align GVGD (ordered from C0 to C65) indicates an aberration that is likely to interfere with protein function. For evolutionary conservation, the UCSC Genome Browser (http://genome.ucsc.edu) was used.
Statistical analysis
Differences between allele frequencies of SNPs found in patients and in the European population (Database of Single Nucleotide Polymorphisms (dbSNP); http://www.ncbi.nlm.nih.gov/SNP/) were analyzed by calculating 95% confidence intervals. Differences were considered statistically significant if the 95% confidence interval did not include zero.
Detection of CFHR5 in serum
CFHR5 was detected in serum of HUS patients, who were not in the acute phase of the disease, and in pooled normal human serum by means of western blotting analysis and by enzyme-linked immunosorbent assay (ELISA) using a polyclonal rabbit anti-human CFHR5 antibody12 (a kind gift from J McRae, Immunology Research Centre, Melbourne, Australia) and a horseradish peroxidase (HRP)-conjungated polyclonal swine anti-rabbit IgG antibody (Dako Denmark A/S, Glostrup, Denmark). This antibody also detects other members of the CFH protein family. Serum of 18 healthy control individuals was used to determine a control range in the ELISA; 2 other controls were used in the western blot.
Determination of sC5b-9 values
The soluble C5b-9 (sC5b-9) complex, also known as the fluid phase terminal complement complex (TCC) or membrane attack complex, is increased in patients with complement activation. SC5b-9 was determined by means of ELISA in serum or plasma samples of HUS patients, who were not in the acute phase of the disease, using a human TCC ELISA kit (Hycult Biotech, Uden, The Netherlands; catalog number HK328).
Results
Molecular genetic studies in the human gene encoding CFHR5
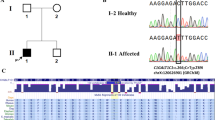
The total open-reading frame of the CFHR5 gene was analyzed in 65 aHUS patients. Four heterozygous sequence variations were found in six patients (Table 2). None of the changes were found in any of the controls. The p.Lys144Asn variation, previously described as a non-disease-causing variant in a HUS family,15 is present once in the 1000 Genomes Project, and in 10 out of 5378 individuals (0.2%) of the Exome Variant Server; no RefSNP (rs) number has been assigned to this variation. Evolutionary conservation was moderate to high in all cases. Conservation within SCRs of CFHR5 was seen for p.Trp436Cys (Figure 1). According to SIFT and Align GVGD, protein function will be affected by all sequence variations. PolyPhen-2 predicted three of the four changes to be probably or possibly damaging; only p.Lys144Asn was predicted to be benign, probably because it is not located in a functional domain of the protein, but between SCR 2 and 3. Therefore, this aberration is considered as a previously unknown SNP. Previously, a genetic aberration was found in CFH in two patients; in one of these patients αFH were also identified (Table 2). Clinically relevant data of the patients are shown in Table 3. No duplications or depletions of the first three exons of CFHR5 have been identified (data not shown).
Locations of the described CFHR5 aberrations in the SCR structure of the CFHR5 protein. The sequences are aligned according to their conserved amino acids.12 Amino-acid coordinates are shown within brackets. The mutated amino acids are in italic and are circled.
Single-nucleotide polymorphisms
Three known SNPs (rs9427662, associated with dense deposit disease;16 rs3748557; and rs35662416, associated with age-related macular degeneration18), were identified in the coding region of CFHR5, but allele frequencies did not differ statistically from the European population (data not shown). Other SNPs associated with dense deposit disease or age-related macular degeneration were not identified. One unknown change was identified in the 3′ splice site of exon 3 (c.254–5C>T), but did not result in a change at splice site level. This aberration was therefore considered as a not previously described polymorphism.
Detection of CFHR5 and sC5b-9 in serum
Serum was only available for three patients (P73, P74 and P75). CFHR5 detection by means of western blot and ELISA could therefore be performed for only two different variations: p.Leu105Arg and p.Lys144Asn. The results of the western blot and ELISA are shown in Figure 2. In the western blot it seems that the CFHR5 level in P75 may be higher than normal human serum; the ELISA confirms this result.
Detection of CFHR5 in serum samples of mutated patients. (a) Western blot of serum samples of three patients, two controls and pooled human serum with polyclonal anti-CFHR5 antibody for detection of CFHR5. Molecular mass marker proteins are indicated on the left. (b) CFHR5 antigen levels measured by ELISA, expressed as percentage in respect to the mean concentration in the control group of 18 healthy individuals (P73: 124.8%, P74: 118.5%, P75: 189.7%, pooled human serum: 116.7%). The range within the controls is shown (64–152%).
In the same three patients, sC5b-9 levels were determined to analyze complement activation. EDTA plasma samples were available for P73 and P74; for P75, only a serum sample was available. Results are shown in Table 2: P75 (p.Leu105Arg) shows increased sC5b-9 levels.
Discussion
Mutational screening of the gene encoding CFHR5 was performed in 65 aHUS patients. Four heterozygous genetic aberrations were identified in six patients (9.2%); one of these sequence variations (p.Lys144Asn), identified in three patients, is considered as a previously unknown SNP. Again, combined complement defects were identified among the patients (CFHR5 and CFH: one patient; CFHR5, CFH and αFH: one patient).
The sequence variation p.Trp436Cys is located in SCR7 of the protein. McRae et al.14 demonstrated that the binding sites for heparin and CRP are located within SCR5-7, although the exact binding sites are not identified yet. Complement regulation at sites of tissue damage is important to prevent complement-mediated damage of host cells. Binding to the polyanion heparin on host cell membranes is probably important in positioning of CFHR5 on host cells and thereby regulate complement activity at the site of tissue damage. In this aberration, the nonpolar amino acid tryptophan is changed into a polar cysteine, which could influence heparin binding. Furthermore, introduction of a cysteine at codon 436 might result in new disulfide bonds and therefore in different protein folding.
The remaining variations are located in SCR2 and SCR3, which are 37% homologous to SCR6 and SCR7 of CFH that show binding capacity to C3b and heparin as well.19 A recombinant CFHR5 protein fragment containing SCR1-4, however, did not show CRP and heparin binding, whereas a SCR3-7 fragment did show binding capacity. Therefore, the involvement of SCR3 and 4 in heparin and CRP binding cannot be ruled out, but alone they are not sufficient enough. Binding to C3b has not been localized to specific SCRs of CFHR5 yet, but as C3b binding sites are present in SCR6 and 7 of CFH, they might be present in SCR2 and 3 of CFHR5 as well.
The variations might all result in decreased complement regulation. Ongoing activity of the alternative complement pathway will lead to an increased formation of membrane attack complex and to increased attraction of leukocytes to the site of endothelial damage, resulting in local thrombosis and inflammation in the glomerular vessels, and eventually to thrombotic microangiopathy and HUS.
The p.Lys144Asn aberration has been described before in two affected sisters and their healthy mother in an aHUS family.15 Another affected family member did not possess this aberration, and therefore it did not seem to be the primary cause of HUS in that specific family, but it was not found in 80 screened control individuals. We identified this sequence variation in three aHUS patients, but not in any of the 146 control individuals, whereas it is present once in the 1000 Genomes Project and in 0.2% of the individuals in the Exome Variant Server. We do agree that p.Lys144Asn does not seem to be the primary cause of the disease, as P73 and P74 also carry a pathogenic aberration in CFH (p.Arg1206Cys)6 and the variation did not appear to influence protein levels in serum. The three remaining aberrations could still be the primary cause of aHUS in our patients: they were not found in our controls, all prediction programs predict them to be damaging to protein function, and no other genetic variations were identified in these patients yet (Table 2). The p.Leu105Arg variation showed a slight increase in CFHR5 protein levels. The reasons for this are not clear. We do see that sC5b-9 levels are altered in the serum of P75, which indicates a increased complement activation. It is known that sC5b-9 levels are higher in serum than in plasma, but even in serum of control individuals, levels were not higher than 3.5 AU per ml (data not shown). Although no other genetic aberration has been identified in this patient, we cannot conclude that the p.Leu105Arg variation is indeed the cause of this increase. The exact functions of CFHR5 are still not known and no functional tests are available to investigate this, yet.20
It has been shown that CFHR5 has a high affinity for heparin on host cell surfaces, even higher than CFH.14 On the other hand, its cofactor and convertase inhibitory activity is lower than CFH, which suggests a specific complement regulation at the site of glomerular endothelial cell surfaces instead of in the fluid phase. This is emphasized by the association with glomerular immune deposits. The question remains why a dysregulation of the complement system at the cell surface due to variations in CFHR5 can result in both CFHR5 nephropathy, a C3 glomerulonephritis, and aHUS, a thrombotic microangiopathy. One explanation might be the different locations of the genetic aberrations; in CFHR5 nephropathy, a duplication of SCR1 and SCR2 is seen, whereas in aHUS, variations are also identified in SCR3-9. Anyhow, as the exact biological role of CFHR5 in complement regulation is still not fully understood, a precise answer cannot be given.
The outcome of plasmapheresis and renal transplantation is correlated with the type of complement mutation.11 Patients with aberrations in complement proteins produced in the liver, such as CFH and CFI, have a worse outcome after renal transplantation than patients with a mutation in the membrane-bound MCP. This could be the case in patients with a change in CFHR5 as well, as this soluble protein is produced in the liver, although we do see that one of our transplanted patients (P74), with both a mutation in CFH and a SNP in CFHR5, still had good graft function after 1 year. Three other patients had a recurrence of the disease in the graft within 1 year after transplantation. Eculizumab, a monoclonal anti-C5 antibody that has positive effects in the treatment of aHUS patients,21 might also be a treatment option for aHUS patients with CFHR5 aberrations.
The prevalence of potentially pathogenic sequence variations in CFHR5 in our cohort (4.6%) are higher than in two other screened aHUS cohorts. Monteferrante et al.15 identified four different genetic alterations in 17.7% (8/45) of their cohort, but three of these variations were found in 1.3% of the controls as well. In an American cohort, a novel mutation was identified in CFHR5 in 2/144 (1.4%) aHUS patients.22 The differences between these cohorts and ours might be explained by regional differences.
In our research population of 65 aHUS patients, the genes encoding CFH, CFI, CD46, CFB and CFHR5 have been screened. In 38.5% (25/65) of the patients, at least one (sequence variation was identified in one of the complement genes. Five of these patients (7.7%) carried bigenic aberrations. aHUS is now considered to be driven by a combination of genetic susceptibility factors (mutations and associated polymorphisms) and an environmental trigger.23, 24 In the remaining patients, no genetic aberrations have been found yet, and therefore, further research on genes involved in the complement system and the coagulation cascade is needed to increase the knowledge about the pathogenesis of aHUS. Understanding how sequence variations influence aHUS susceptibility will require detailed functional analysis so that rare sequence variations are not mistaken as disease-associated changes. As the exact biological role of CFHR5 in HUS and other renal diseases is not known yet,20 the investigation of the significance of identified sequence variants to disease pathogenesis still has to be established.
References
Boyce, T. G., Swerdlow, D. L., Griffin, P. M. Escherichia coli O157:H7 and the hemolytic-uremic syndrome. N. Engl. J. Med. 333, 364–368 (1995).
Kaplan, B. S., Meyers, K. E., Schulman, S. L. The pathogenesis and treatment of hemolytic uremic syndrome. J. Am. Soc. Nephrol. 9, 1126–1133 (1998).
Noris, M., Brioschi, S., Caprioli, J., Todeschini, M., Bresin, E., Porrati, F. et al. Familial haemolytic uraemic syndrome and an MCP mutation. Lancet 362, 1542–1547 (2003).
Caprioli, J., Noris, M., Brioschi, S., Pianetti, G., Castelletti, F., Bettinaglio, P. et al. Genetics of HUS: the impact of MCP, CFH, and IF mutations on clinical presentation, response to treatment, and outcome. Blood 108, 1267–1279 (2006).
Fremeaux-Bacchi, V., Dragon-Durey, M. A., Blouin, J., Vigneau, C., Kuypers, D., Boudailliez, B. et al. Complement factor I: a susceptibility gene for atypical haemolytic uraemic syndrome. J. Med. Genet. 41, e84 (2004).
Westra, D., Volokhina, E., van der Heijden, E., Vos, A., Huigen, M., Jansen, J. et al. Genetic disorders in complement (regulating) genes in patients with atypical haemolytic uraemic syndrome (aHUS). Nephrol. Dial Transplant. 25, 2195–2202 (2010).
Goicoechea de, J. E., Harris, C. L., Esparza-Gordillo, J., Carreras, L., Arranz, E. A., Garrido, C.A et al. Gain-of-function mutations in complement factor B are associated with atypical hemolytic uremic syndrome. Proc. Natl Acad. Sci. USA 104, 240–245 (2007).
Fremeaux-Bacchi, V., Miller, E. C., Liszewski, M. K., Strain, L., Blouin, J., Brown, A. L. et al. Mutations in complement C3 predispose to development of atypical hemolytic uremic syndrome. Blood 112, 4948–4952 (2008).
Delvaeye, M., Noris, M., De, V.A., Esmon, C.T., Esmon, N.L., Ferrell, G. et al. Thrombomodulin mutations in atypical hemolytic-uremic syndrome. N. Engl. J. Med. 361, 345–357 (2009).
Jozsi, M., Licht, C., Strobel, S., Zipfel, S. L., Richter, H., Heinen, S. et al. Factor H autoantibodies in atypical hemolytic uremic syndrome correlate with CFHR1/CFHR3 deficiency. Blood 111, 1512–1514 (2008).
Noris, M., Remuzzi, G. Atypical hemolytic-uremic syndrome. N. Engl. J. Med. 361, 1676–1687 (2009).
McRae, J. L., Cowan, P. J., Power, D. A., Mitchelhill, K. I., Kemp, B. E., Morgan, B. P. et al. Human factor H-related protein 5 (FHR-5). A new complement-associated protein. J. Biol. Chem. 276, 6747–6754 (2001).
Murphy, B., Georgiou, T., Machet, D., Hill, P., McRae, J. Factor H-related protein-5: a novel component of human glomerular immune deposits. Am. J. Kidney. Dis. 39, 24–27 (2002).
McRae, J. L., Duthy, T. G., Griggs, K. M., Ormsby, R. J., Cowan, P. J., Cromer, B. A. et al. Human factor H-related protein 5 has cofactor activity, inhibits C3 convertase activity, binds heparin and C-reactive protein, and associates with lipoprotein. J. Immunol 174, 6250–6256 (2005).
Monteferrante, G., Brioschi, S., Caprioli, J., Pianetti, G., Bettinaglio, P., Bresin, E. et al. Genetic analysis of the complement factor H related 5 gene in haemolytic uraemic syndrome. Mol. Immunol. 44, 1704–1708 (2007).
Abrera-Abeleda, M. A., Nishimura, C., Smith, J. L., Sethi, S., McRae, J. L., Murphy, B. F. et al. Variations in the complement regulatory genes factor H (CFH) and factor H related 5 (CFHR5) are associated with membranoproliferative glomerulonephritis type II (dense deposit disease). J. Med. Genet. 43, 582–589 (2006).
Gale, D. P., de Jorge, E. G., Cook, H. T., Martinez-Barricarte, R., Hadjisavvas, A., McLean, A. G. et al. Identification of a mutation in complement factor H-related protein 5 in patients of Cypriot origin with glomerulonephritis. Lancet 376, 794–801 (2010).
Narendra, U., Pauer, G. J., Hagstrom, S. A. Genetic analysis of complement factor H related 5, CFHR5, in patients with age-related macular degeneration. Mol. Vis. 15, 731–736 (2009).
Skerka, C., Zipfel, P. F. Complement factor H related proteins in immune diseases. Vaccine 26 (Suppl 8), I9–14 (2008).
Gale, D. P., Pickering, M. C. Regulating complement in the kidney: insights from CFHR5 nephropathy. Dis. Model Mech. 4, 721–726 (2011).
Nurnberger, J., Philipp, T., Witzke, O., Opazo, S.A., Vester, U., Baba, H.A. et al. Eculizumab for atypical hemolytic-uremic syndrome. N. Engl. J. Med. 360, 542–544 (2009).
Maga, T. K., Nishimura, C. J., Weaver, A. E., Frees, K. L., Smith, R. J. Mutations in alternative pathway complement proteins in American patients with atypical hemolytic uremic syndrome. Hum. Mutat. 31, E1445–E1460 (2010).
Caprioli, J., Castelletti, F., Bucchioni, S., Bettinaglio, P., Bresin, E., Pianetti, G. et al. Complement factor H mutations and gene polymorphisms in haemolytic uraemic syndrome: the C-257T, the A2089G and the G2881T polymorphisms are strongly associated with the disease. Hum. Mol. Genet. 12, 3385–3395 (2003).
Esparza-Gordillo, J., Goicoechea de, J. E., Buil, A., Carreras, B. L., Lopez-Trascasa, M., Sanchez-Corral, P. et al. Predisposition to atypical hemolytic uremic syndrome involves the concurrence of different susceptibility alleles in the regulators of complement activation gene cluster in 1q32. Hum. Mol. Genet. 14, 703–712 (2005).
Acknowledgements
We would like to thank patients, their parents and their physicians for their participation in this study, in particular Dr van Son (Groningen, The Netherlands). We also thank Mitali Patel (CCIR, London, United Kingdom) for helping with the MLPA. This work was partially supported by the Dutch Kidney Foundation (C09.2313, KBSO 07.0004, and KBSO 09.0008) and the Wellcome Trust (WT082291MA).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Westra, D., Vernon, K., Volokhina, E. et al. Atypical hemolytic uremic syndrome and genetic aberrations in the complement factor H-related 5 gene. J Hum Genet 57, 459–464 (2012). https://doi.org/10.1038/jhg.2012.57
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2012.57
Keywords
This article is cited by
-
Mutations in the alternative complement pathway in multiple myeloma patients with carfilzomib-induced thrombotic microangiopathy
Blood Cancer Journal (2023)
-
Complement dysregulation associated with a genetic variant in factor H-related protein 5 in atypical hemolytic uremic syndrome
Pediatric Nephrology (2023)
-
Whole exome sequencing identifies monogenic forms of nephritis in a previously unsolved cohort of children with steroid-resistant nephrotic syndrome and hematuria
Pediatric Nephrology (2022)
-
Thrombotic microangiopathy in a patient with eosinophilic granulomatosis with polyangiitis: case-based review
Rheumatology International (2019)
-
Role of complement in the pathogenesis of thrombotic microangiopathies
memo - Magazine of European Medical Oncology (2018)