Abstract
Imatinib mesylate (IM) trough concentration varies among IM-treated chronic myeloid leukemia (CML) patients. Although IM pharmacokinetics is influenced by several enzymes and transporters, little is known about the role of pharmacogenetic variation in IM metabolism. In this study, associations between IM trough concentration, clinical response and 11 single-nucleotide polymorphisms in genes involved in IM pharmacokinetics (ABCB1, ABCC2, ABCG2 CYP3A5, SLC22A1 and SLCO1B3) were investigated among 67 Japanese chronic phase CML patients. IM trough concentration was significantly higher in patients with a major molecular response than in those without one (P=0.010). No significant correlations between IM trough concentration and age, weight, body mass index or biochemical data were observed. However, the dose-adjusted IM trough concentration was significantly higher in patients with ABCG2 421A than in those with 421C/C (P=0.015). By multivariate regression analysis, only ABCG2 421A was independently predictive of a higher dose-adjusted IM trough concentration (P=0.015). Moreover, previous studies have shown that the ABCG2 421C>A (p.Q141K) variant is prevalent among Japanese and Han Chinese individuals and less common among Africans and Caucasians. Together, these data indicate that plasma IM concentration monitoring and prospective ABCG2 421C>A genotyping may improve the efficacy of IM therapy, particularly among Asian CML patients.
Similar content being viewed by others
Introduction
Imatinib mesylate (IM) is a potent and selective inhibitor of BCR–ABL tyrosine kinase activity, and is approved for the treatment of Philadelphia chromosome-positive chronic myeloid leukemia (CML).1, 2 Despite the outstanding results obtained with IM for the treatment of CML, cases of treatment failure or of suboptimal response are sometimes seen. A number of factors likely underlie IM resistance, including (i) biological factors, such as the baseline presence or later emergence of bcr–abl and/or other mutations; (ii) clinical features, such as the disease status of the patient or the Sokal risk score at baseline; and (iii) constitutional pharmacogenetic variation affecting IM metabolism and/or transport.3
Recently, two studies suggested that plasma IM trough concentration variability influences clinical response among CML patients.4, 5 In addition, Picard et al. reported that the threshold for IM trough concentration should be set above 1002 ng ml–1, as this level was significantly associated with a major molecular response (MMR).5 Although several important clinical trials indicated that 400 mg of IM should be the standard daily dose for chronic phase CML patients,1, 2 in clinical practice, lower doses of IM are administered to ∼40% of Japanese patients.6, 7 This is largely because of the fact that for some Japanese patients, lower IM doses have sufficient trough concentration for therapeutic CML treatment.7 Although this interindividual variability in IM pharmacokinetics is observed among Japanese CML patients, little is known about potential pharmacogenetic variation influencing IM metabolism and drug transport efficacy.
The cytochrome-P450 (CYP) system is involved in the oxidative metabolism of IM and the major pathway is catalyzed by CYP3A4/5.2, 8, 9 Although few common CYP3A4 polymorphisms have been identified with in vivo effect on enzyme activity, CYP3A5 expression is strongly correlated with a single-nucleotide polymorphism (SNP) within intron 3 (6986A>G; CYP3A5*3).10 This allele is prevalent among Japanese individuals,11 suggesting that germline CYP3A5 SNPs may influence IM trough concentration and drug efficacy in this population.
IM is transported by P-glycoprotein (MDR1), organic cation transporter 1 (OCT1) and breast cancer resistance protein (BCRP).12, 13, 14, 15 P-Glycoprotein, which is encoded by the ABCB1 gene, is a membrane efflux transporter normally expressed in the small intestine, in biliary canalicular front of hepatocytes and in renal proximal tubules.16 Previous studies have investigated whether SNPs in ABCB1, including 1236T>C, 2677G>T/A and 3435T>C, affect IM pharmacokinetics; however, the role of ABCB1 genetic variation in IM trough concentration is still unclear.17, 18 OCT1, which is encoded by SLC22A1, is primarily expressed on hepatocytes, suggesting that it has a role in substrate uptake into the liver.19, 20, 21 Although IM is a substrate of OCT1,15, 22, 23 no association between IM and SLC22A1 286C>T or 1498G>A, variants not common in the Japanese population, was previously observed.24, 25 In addition, in vitro studies have shown that organic anion-transporting polypeptide 1B3 (OATP1B3), which is encoded by SLCO1B3, contributes to IM uptake into hepatocytes.24 However, to date, the influence of SLCO1B3 SNPs on the pharmacokinetics of IM has not been reported.
IM is excreted into bile predominantly by BCRP, which is encoded by ABCG2, and less so by multidrug-resistance protein 2 (MRP2), which is encoded by ABCC2, and MDR1.12, 13, 14 BCRP also belongs to the ABC efflux transporter superfamily26 and is widely expressed in the small intestine, liver and placenta, influencing the absorption and disposition of a variety of substrates.27, 28 It is noteworthy that Petain et al. reported that IM clearance in patients carrying the ABCG2 421C/A genotype was significantly lower than in those with the 421C/C genotype.29
To investigate the role of pharmacogenetic variation in IM metabolism and efficacy, SNPs within important IM exposure genes (ABCB1 (MDR1), ABCC2 (MRP2), ABCG2 (BCRP), CYP3A5, SLC22A1 (OCT1) and SLCO1B3 (OATP1B3)) were analyzed in IM-treated CML patients. In addition, IM trough concentration was determined in all patients to assess the association between IM pharmacokinetics and efficacy.
Materials and methods
Patients
A total of 67 chronic phase CML patients (37 male and 30 female) from 15 major hospitals in Akita Prefecture, Japan, all of whom were being treated with IM, were enrolled in this study. The study protocol was approved by the Ethics Committee of Akita University School of Medicine and all patients gave written informed consent. Among them, 34 (51%) were treated with 400 mg of IM daily, 17 (25%) with 300 mg, 14 (21%) with less than 300 mg and two (3%) with more than 400 mg. Although the standard daily dose of IM for chronic-phase CML is 400 mg, dose reduction or dose escalation was required for some patients because of adverse events or IM resistance, respectively. Patient characteristics are listed in Table 1. No patients had any serious renal or hepatic dysfunction.
Clinical parameters including response to therapy
A complete cytogenetic response (CCyR) was defined as no Philadelphia-positive metaphases in 20 or more examined cells. In some cases, fluorescent in situ hybridization analysis of the bcr–abl fusion gene in peripheral blood neutrophils was also performed.30 A MMR was defined as a threefold log reduction in bcr–abl transcripts measured using real-time reverse transcriptase-mediated quantitative-PCR. The samples used for IM response evaluation were obtained from patients on the same day as samples used for measurement of plasma trough levels. In patients without a CCyR, mutation analysis of the bcr–abl fusion transcript was performed using the Invader assay,31 which detects 25 mutations, including M244V, L248VR, G250E, Q252H, Q252R, Y253F, Y253H, E255K, E255V, E279K, F311L, T315A, T315I, F317L, M351T, F359IV, V379I, L387M, H396P, H396R, S417Y, E459K and F486S.
Measurement of plasma IM concentration
Blood samples were collected by venipuncture 24 h (± 2 h) after oral administration of IM. Plasma was then isolated by centrifugation at 1900 × g for 15 min and stored at −40 °C until further analysis. IM trough concentration was determined by high-performance liquid chromatography equipped with a mass spectrometric detector from Toray Research Center, Inc. (Nihonbashi, Tokyo, Japan),32, 33 which is the only Novartis Global authorized platform in Japan.
Genotyping
DNA was extracted from peripheral blood samples using the QIAamp Blood Mini Kit (Qiagen, Tokyo, Japan) and stored at −80 °C until analyzed. CYP3A5*3 (6986A>G (rs776746)) and SLC22A1 (156T>C (rs1867351), 480G>C (rs683369), 1022C>T (rs2282143) and 1222A>G (rs628031)) genotyping was performed by PCR–RFLP, as previously described by Fukuen et al.34 and Itoda et al.,25 respectively. Similarly, ABCC2 (−24C>T (rs717620)) and ABCB1 (1236T>C (rs1128503), 2677G>T/A (rs2032582) and 3435T>C (rs1045642)) were genotyped as described by Naesens et al.,35 Wu et al.,36 Tanaka et al.37 and Cascorbi et al.,38 respectively. ABCG2 421C>A (rs2231142) was genotyped as described by Kobayashi et al.,39 and SLCO1B3 (334T>G (rs4149117)) as described by Tsujimoto et al.40 All genotype frequencies were tested for Hardy–Weinberg equilibrium.
Statistical analyses
Statistical analyses were carried out using SPSS statistical software (SPSS Japan, Tokyo, Japan, version 17.0). Differences in IM trough concentration between subgroups were evaluated using the Student’s t-test. Clinical parameters were compared using one-way analysis of variance with the post hoc Tukey multiple comparison procedure. The χ2-test or Fisher's exact test was used to compare MMR and specific genotypes. Pearson’s product moment correlation was applied to assess the relation between dose-adjusted IM trough concentrations and clinical variables (age, weight, body mass index and biochemical data). Stepwise forward selection multiple regression analysis for dose-adjusted IM trough concentrations and stepwise forward selection multiple logistic analysis for MMR were performed to determine the effect of the variables examined in the univariate analysis. Positive and negative predictive values for selected genotypes and MMR were determined by standard calculations. Only variables for which the correlation coefficient (r) was >0.2 in the Pearson product moment correlation coefficient test or for which the P-value was <0.1 in the univariate analysis were included in the multivariate analysis. Clinical variables (age and genotypes) were considered for possible inclusion in the multivariate analysis. P-values of <0.05 were considered significant.
Results
Patient characteristics and response to imatinib therapy
A total of 67 Japanese CML patients participated in the study. Among them, five patients without a CCyR were excluded from correlating IM trough concentration with clinical response because of the identification of ABL kinase domain mutations (G250E, G250E, E279K, T315I and F317L, respectively). Of the remaining 62 patients, 51 (82%) showed a CCyR and 34 (55%) showed an MMR.
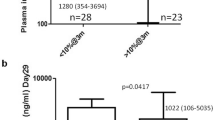
Clinical characteristics of the 62 patients with (all doses, n=34; 400 mg, n=21) or without (all doses, n=28; 400 mg, n=10) an MMR are summarized in Table 2. Notably, IM trough concentration was significantly higher in patients with an MMR than in those who did not achieve an MMR (P=0.010; Figure 1). Furthermore, when restricting the analysis to the 31 patients treated with 400 mg of IM daily, the median IM trough concentration was again significantly higher in patients with an MMR (P=0.017). No association between plasma IM trough concentrations and CCyR was observed (data not shown).
Box plots of steady-state IM trough concentrations at all doses in patients with and without an MMR. Boxes span data between two quartiles (interquartile range), with medians represented by bold horizontal lines. The ends of the whiskers (vertical lines) represent the smallest and largest values that are not outliers. Outliers (circles) are values between 1.5 and 3 interquartile ranges from the end of a box. The median IM trough concentrations were 779 ng ml–1 (range 353–1950 ng ml–1) and 701.5 ng ml–1 (111–1210 ng ml–1) among patients with and without an MMR, respectively.
Genotype and response to imatinib therapy
The genotypes of all patients and their molecular responses to IM therapy are summarized in Table 3. For the 62 patients without an ABL kinase domain mutation, the percentage with an MMR was significantly higher among those with the SLC22A1 1222G/G genotype than in those carrying the A allele (P=0.013). Moreover, logistic regression models revealed that patients with SLC22A1 1222G/G had a greater likelihood of achieving an MMR, with an odds ratio of 3.71 (95% confidence interval (CI): 1.288–10.685, P=0.015). The positive and negative predictive values of SLC22A1 1222A>G for MMR in CML were 70.6 and 60.7%, respectively. However, among the 31 patients treated with 400 mg of IM daily, there was no significant SLC22A1 1222A>G genotype-dependent difference in the percentage of patients who achieved an MMR.
Genotype and imatinib trough concentration
The five patients with an ABL kinase domain mutation were included in this analysis, as these mutations presumably would not affect IM exposure. For all patients, the mean IM trough concentration was 904.8±795.2 ng ml–1. No significant correlations between age, weight, body mass index or biochemical data and IM trough concentration were observed (Table 1).
The dose-adjusted plasma IM trough concentrations for each ABCB1, ABCC2, ABCG2, CYP3A5, SLC22A1 and SLCO1B3 genotype were determined and are listed in Table 4. There were no significant differences in dose-adjusted IM trough concentrations among the ABCB1, ABCC2, CYP3A5, SLC22A1 or SLCO1B3 genotype. However, the dose-adjusted IM trough concentration was significantly higher in the 25 patients with ABCG2 421C/A or 421A/A than in the 42 patients with 421C/C (P=0.015). The mean dose-adjusted IM trough concentration in the ABCG2 421C/A+A/A and 421C/C genotypes was 3.18 and 2.34 ng ml–1 mg–1, respectively. Moreover, by multivariate regression analysis, only ABCG2 421A was independently predictive of a higher dose-adjusted IM trough concentration (P=0.015). The identified prediction formula was as follows: dose-adjusted IM trough concentration (C0/dose) =−0.845 (standard error 0.339) × G +3.183 (standard error 0.207), where G=1 for the ABCG2 421C/C genotype and 0 for other genotypes.
Discussion
In this study, a significant correlation was identified between steady-state IM trough concentration and MMR, but not CCyR; however, it is possible that the number of patients without a CCyR in our study (11 patients, 18%) was too small for statistical significance to be reached. Moreover, in patients with an MMR, the median trough concentration (1020 ng ml–1) was greater than the 1002 ng ml–1 threshold reportedly required for efficacy,5 further supporting the observed statistical association between plasma IM levels and clinical response. In addition, our study identified a significant correlation between ABCG2 421C>A (p.Q141K) and IM trough concentration, suggesting an important role for the BCRP efflux transporter in IM metabolism.
In addition, the SLC22A1 1222A>G polymorphism appears to be an independent factor associated with clinical response to IM. Although SLC22A1 1222A>G was associated with achieving an MMR in our study among patients treated with less than 400 mg of IM (P=0.048), a larger patient cohort is needed to confirm this finding. The level of SLC22A1 (OCT1) likely correlates with intracellular IM concentration, as primary CML cells with high levels of OCT1 previously had greater uptake than those exhibiting a more modest OCT1 expression.22, 23 This may be why, in our patients treated with lower doses of IM, clinical response was dependent on SLC22A1 (OCT1), whereas in patients with plasma IM levels above the 1002 ng ml–1 threshold, IM exposure seemed to be more dependent on ABCG2 (BCRP).
The dose-adjusted IM trough concentration was significantly higher in CML patients with ABCG2 (BCRP) 421A than in those with the 421C/C genotype, indicating that interindividual variation in plasma IM concentration may reflect the activity of the BCRP efflux transporter. IM is predominantly excreted through the biliary-fecal route41 and BCRP is highly expressed in the small intestine and bile canaliculi of the liver.42, 43 The presence of BCRP in the small intestine suggests that it contributes to the regulation of substrate uptake from the gastrointestinal tract through back-transport of substrates reentering the gut lumen. Given the fact PA317 cells transfected with ABCG2 421A have reduced BCRP expression compared with wild type,44 the plasma IM concentration for patients carrying the ABCG2 421C/C genotype is therefore thought to be lower than in those carrying the 421A allele.
Orally administered IM has an absolute bioavailability of 98% in patients with CML,2 and the intracellular uptake of IM is reportedly associated with the organic anion transporting polypeptide SLCO1A2 (OATP1A2).24 In the human intestine, OATP1A2 is expressed on the apical brush-border membrane of human enterocytes,45 which suggests that net absorption of IM may reflect a situation in which there is greater uptake by SLCO1A2 (OATP1A2) than efflux by ABCG2 (BCRP). In this study, SLCO1A2 genotyping was not performed because SNPs that affect OATP1A2 transport activity are not typically found in the Asian population.46 Consequently, the disposition of IM may be altered by ABCG2 421C>A, such that polymorphism-dependent differences in IM trough concentration reflect a difference in hepatic IM biliary excretion rather than a difference in intestinal IM absorption.
Although SLC22A1 (OCT1) has a major role in determining the clinical efficacy of IM in CML cells,22, 23 its role relating to IM exposure in hepatocytes is likely to be minor. For example, patients with the SLC22A1 (OCT1) 480G variant tended to have slightly higher IM trough concentrations, but multivariate analysis showed that only ABCG2 421A was significantly associated with a higher dose-adjusted IM trough concentration. Notably, when our multivariate regression prediction formula for the dose-adjusted IM trough concentration (C0/dose =−0.845 × G+3.183, where G=1 for ABCG2 421C/C and 0 for other genotypes) was applied to the reported 1002 ng ml–1 plasma threshold by Picard et al.,5 the predicted IM dose for patients with ABCG2 421C/C is 400 mg, and that for patients with 421C/A or 421A/A is 300 mg. This is particularly pertinent, given the fact that the Japanese and Han Chinese populations have markedly higher ABCG2 421C>A allele frequencies (30.7 and 28.9%, respectively) than do Caucasian (11.7%) and African-American populations (2.3%).47, 48, 49 Our group is currently pursuing a prospective clinical study to validate this prediction formula.
Both ABCB1 (MDR1) and ABCG2 (BCRP) display high affinity for IM and can confer IM resistance in vitro by extruding IM from hematopoietic cells.50, 51 Moreover, both transporters show elevated expression in CML stem cells,52, 53 and several known SNPs modify their activity.18, 54 For example, Dulucq et al. reported that ABCB1 polymorphisms were associated with MMR in CML.55 More recently, Kim et al. described three SNPs in ABCG2, CYP3A5 and SLC22A1 that were significantly associated with treatment outcomes following IM therapy.56 Although they did not investigate the relationship between the tested SNPs and plasma IM concentration, the authors noted that interindividual variation in hepatic IM uptake and clearance could lead to changes in systemic IM concentration.
Our results should be interpreted within the context of the study limitations, which primarily involve the sample size of the study. As noted, only variables with univariate P-values below 0.1 were included in the multivariate analysis. With respect to MMR and imatinib trough concentration, the only variables that reached the significance threshold were the SLC22A1 1222A>G and ABCG2 421C>A genotype, respectively. For the ABCG2 421C>A two-sample t-test power calculation, a sample size of 16 subjects per genotype group was necessary to obtain a detection power of 90% (α=0.05 and β=0.1), satisfying statistical sample size. However, for the SLC22A1 1222A>G two-sample comparison of proportions power calculation, when 37.0 and 68.6% of patients with the SLC22A1 1222 A/A+G/A and G/G genotype, respectively, arrived at an MMR, a sample size of 51 subjects for one genotype was necessary to obtain a detection power of 90%. In addition, multivariate modeling covariates cannot be specified with this sample size, suggesting that a confirmatory study using a larger patient cohort may be warranted.
Similar to bcr–abl mutation analyses, IM plasma monitoring may be useful in clinical practice when the expected response is not achieved during IM therapy. However, the clinical feasibility of this approach requires further consideration. For example, similar to previous studies on IM plasma level quantitation,4, 5 our study used high-performance liquid chromatography equipped with a mass spectrometric detector. This method is not always available in standard hospital laboratories and the running costs are more expensive than those for high-performance liquid chromatography with an ultraviolet detector. As such, a validated high-performance liquid chromatography-ultraviolet assay may be a more practical platform for measuring IM plasma concentration in actual clinical practice.
In conclusion, ABCG2 421C>A may influence the interindividual variation in plasma IM concentration observed among Japanese CML patients. Although a prospective study with a larger patient population is necessary to validate these findings, plasma IM concentration monitoring and clinical ABCG2 421C>A genotyping may improve IM therapy for CML, particularly in Asian populations.
References
Druker, B. J., Talpaz, M., Resta, D. J., Peng, B., Buchdunger, E., Ford, J. M. et al. Efficacy and safety of a specific inhibitor of the BCR-ABL tyrosine kinase in chronic myeloid leukemia. N. Engl. J. Med. 344, 1031–1037 (2001).
Peng, B., Lloyd, P. & Schran, H. Clinical pharmacokinetics of imatinib. Clin. Pharmacokinet. 44, 879–894 (2005).
Cortes, J. E., Egorin, M. J., Guilhot, F., Molimard, M. & Mahon, F. X. Pharmacokinetic / pharmacodynamic correlation and blood-level testing in imatinib therapy for chronic myeloid leukemia. Leukemia. 23, 1537–1544 (2009).
Larson, R. A., Druker, B. J., Guilhot, F., O’Brien, S. G., Riviere, G. J., Krahnke, T. et al. Imatinib pharmacokinetics and its correlation with response and safety in chronic-phase chronic myeloid leukemia: a subanalysis of the IRIS study. Blood. 111, 4022–4028 (2008).
Picard, S., Titier, K., Etienne, G., Teilhet, E., Ducint, D., Bernard, M. A. et al. Trough imatinib plasma levels are associated with both cytogenetic and molecular responses to standard-dose imatinib in chronic myeloid leukemia. Blood. 109, 3496–3499 (2007).
Kanda, Y., Okamoto, S., Tauchi, T., Kizaki, M., Inokuchi, K., Yabe, M. et al. Multicenter prospective trial evaluating the tolerability of imatinib for Japanese patients with chronic myelogenous leukemia in the chronic phase: does body weight matter? Am. J. Hematol. 83, 835–839 (2008).
Sakai, M., Miyazaki, Y., Matsuo, E., Moriuchi, Y., Hata, T., Fukushima, T. et al. Long-term efficacy of imatinib in a practical setting is correlated with imatinib trough concentration that is influenced by body size: a report by the Nagasaki CML Study Group. Int. J. Hematol. 89, 319–325 (2009).
Lin, Y. S., Dowling, A. L., Quigley, S. D., Farin, F. M., Zhang, J., Lamba, J. et al. Co-regulation of CYP3A4 and CYP3A5 and contribution to hepatic and intestinal midazolam metabolism. Mol. Pharmacol. 62, 162–172 (2002).
Williams, J. A., Ring, B. J., Cantrell, V. E., Jones, D. R., Eckstein, J., Ruterbories, K. et al. Comparative metabolic capabilities of CYP3A4, CYP3A5, and CYP3A7. Drug. Metab. Dispos. 30, 883–891 (2002).
Hustert, E., Haberl, M., Burk, O., Wolbold, R., He, Y. Q., Klein, K. et al. The genetic determinants of the CYP3A5 polymorphism. Pharmacogenetics. 11, 773–779 (2001).
Saeki, M., Saito, Y., Nakamura, T., Murayama, N., Kim, S. R., Ozawa, S. et al. Single nucleotide polymorphisms and haplotype frequencies of CYP3A5 in a Japanese population. Hum. Mutat. 21, 653 (2003).
Burger, H., van Tol, H., Boersma, A. W., Brok, M., Wiemer, E. A., Stoter, G. et al. Imatinib mesylate (STI571) is a substrate for the breast cancer resistance protein (BCRP)/ABCG2 drug pump. Blood. 104, 2940–2942 (2004).
Burger, H. & Nooter, K. Pharmacokinetic resistance to imatinib mesylate: role of the ABC drug pumps ABCG2 (BCRP) and ABCB1 (MDR1) in the oral bioavailability of imatinib. Cell Cycle. 3, 1502–1505 (2004).
Burger, H., van Tol, H., Brok, M., Wiemer, E. A., de Bruijn, E. A., Guetens, G. et al. Chronic imatinib mesylate exposure leads to reduced intracellular drug accumulation by induction of the ABCG2 (BCRP) and ABCB1 (MDR1) drug transport pumps. Cancer Biol. Ther. 4, 747–752 (2005).
Choi, M. K. & Song, I. S. Organic cation transporters and their pharmacokinetic and pharmacodynamic consequences. Drug. Metab. Pharmacokinet. 23, 243–253 (2008).
Thiebaut, F., Tsuruo, T., Hamada, H., Gottesman, M. M., Pastan, I. & Willingham, M. C. Cellular localization of the multidrug-resistance gene product P-glycoprotein in normal human tissues. Proc. Natl. Acad. Sci. USA 84, 7735–7738 (1987).
Gurney, H., Wong, M., Balleine, R. L., Rivory, L. P., McLachlan, A. J., Hoskins, J. M. et al. Imatinib disposition and ABCB1 (MDR1, P-glycoprotein) genotype. Clin. Pharmacol. Ther. 82, 33–40 (2007).
Gardner, E. R., Burger, H., van Schaik, R. H., van Oosterom, A. T., de Bruijn, E. A., Guetens, G. et al. Association of enzyme and transporter genotypes with the pharmacokinetics of imatinib. Clin. Pharmacol. Ther. 80, 192–201 (2006).
Zhang, L., Schaner, M. E. & Giacomini, K. M. Functional characterization of an organic cation transporter (hOCT1) in a transiently transfected human cell Line (HeLa). J. Pharmacol. Exp. Ther. 286, 354–361 (1998).
Zhang, L., Brett, C. M. & Giacomini, K. M. Role of organic cation transporters in drug absorption and elimination. Annu. Rev. Pharmacol. Toxicol. 38, 431–460 (1998).
Zhang, L., Dresser, M. J., Gray, A. T., Yost, S. C., Terashita, S. & Giacomini, K. M. Cloning and Functional Expression of a Human Liver Organic Cation Transporter. Mol. Pharmacol. 51, 913–921 (1997).
White, D. L., Saunders, V. A., Dang, P., Engler, J., Zannettino, A. C., Cambareri, A. C. et al. OCT-1-mediated influx is a key determinant of the intracellular uptake of imatinib but not nilotinib (AMN107): reduced OCT-1 activity is the cause of low in vitro sensitivity to imatinib. Blood 108, 697–704 (2006).
Wang, L., Giannoudis, A., Lane, S., Williamson, P., Pirmohamed, M. & Clark, R. E. Expression of the uptake drug transporter hOCT1 is an important clinical determinant of the response to imatinib in chronic myeloid leukemia. Clin. Pharmacol. Ther. 83, 258–264 (2008).
Hu, S., Franke, R. M., Filipski, K. K., Hu, C., Orwick, S. J., de Bruijn, E. A. et al. Interaction of imatinib with human organic ion carriers. Clin. Cancer Res. 14, 3141–3148 (2008).
Itoda, M., Saito, Y., Maekawa, K., Hichiya, H., Komamura, K., Kamakura, S. et al. Seven novel single nucleotide polymorphisms in the human SLC22A1 gene encoding organic cation transporter 1 (OCT1). Drug. Metab. Pharmacokinet. 19, 308–312 (2004).
Zamber, C. P., Lamba, J. K., Yasuda, K., Farnum, J., Thummel, K., Schuetz, J. D. et al. Natural allelic variants of breast cancer resistance protein (BCRP) and their relationship to BCRP expression in human intestine. Pharmacogenetics 13, 19–28 (2003).
Hirano, M., Maeda, K., Matsushima, S., Nozaki, Y., Kusuhara, H. & Sugiyama, Y. Involvement of BCRP (ABCG2) in the biliary excretion of pitavastatin. Mol. Pharmacol. 68, 800–807 (2005).
Zhang, W., Yu, B. N., He, Y. J., Fan, L., Li, Q., Liu, Z. Q. et al. Role of BCRP 421C>A polymorphism on rosuvastatin pharmacokinetics in healthy Chinese males. Clin. Chim. Acta. 373, 99–103 (2006).
Petain, A., Kattygnarath, D., Azard, J., Chatelut, E., Delbaldo, C., Geoerger, B. et al. Innovative Therapies with Children with Cancer European consortium. Population pharmacokinetics and pharmacogenetics of imatinib in children and adults. Clin. Cancer Res. 14, 7102–7109 (2008).
Takahashi, N., Miura, I., Kobayashi, Y., Kume, M., Yoshioka, T., Otane, W. et al. Fluorescence in situ hybridization monitoring of BCR-ABL-positive neutrophils in chronic-phase chronic myeloid leukemia patients during the primary stage of imatinib mesylate therapy. Int. J. Hematol. 81, 235–241 (2005).
Yamamoto, M., Kakihana, K., Ohashi, K., Yamaguchi, T., Tadokoro, K., Akiyama, H. et al. Serial monitoring of T315I BCR-ABL mutation by Invader assay combined with RT-PCR. Int. J. Hematol. 89, 482–488 (2009).
Bakhtiar, R., Lohne, J., Ramos, L., Khemani, L., Hayes, M. & Tse, F. High-throughput quantification of the anti-leukemia drug STI571 (Gleevec) and its main metabolite (CGP 74588) in human plasma using liquid chromatography-tandem mass spectrometry. J. Chromatogr. B. Analyt. Technol. Biomed. Life Sci. 768, 325–340 (2002).
Parise, R. A., Ramanathan, R. K., Hayes, M. J. & Egorin, M. J. Liquid chromatographic-mass spectrometric assay for quantitation of imatinib and its main metabolite (CGP 74588) in plasma. J. Chromatogr. B. Analyt. Technol. Biomed. Life Sci. 791, 39–44 (2003).
Fukuen, S., Fukuda, T., Maune, H., Ikenaga, Y., Yamamoto, I., Inaba, T. et al. Novel detection assay by PCR-RFLP and frequency of the CYP3A5 SNPs, CYP3A5*3 and *6, in a Japanese population. Pharmacogenetics 12, 331–334 (2002).
Naesens, M., Kuypers, D. R., Verbeke, K. & Vanrenterghem, Y. Multidrug resistance protein 2 genetic polymorphisms influence mycophenolic acid exposure in renal allograft recipients. Transplantation 82, 1074–1084 (2006).
Wu, L., Xu, X., Shen, J., Xie, H., Yu, S., Liang, T. et al. MDR1 gene polymorphisms and risk of recurrence in patients with hepatocellular carcinoma after liver transplantation. J. Surg. Oncol. 96, 62–68 (2007).
Tanaka, H., Imamura, N., Oguma, N., Shintani, T., Tanaka, K., Hyodo, H. et al. Acute myelogenous leukemia with PIG-A gene mutation evolved from aplastic anemia-paroxysmal nocturnal hemoglobinuria syndrome. Int. J. Hematol. 73, 206–212 (2001).
Cascorbi, I., Gerloff, T., Johne, A., Meisel, C., Hoffmeyer, S., Schwab, M. et al. Frequency of single nucleotide polymorphisms in the P-glycoprotein drug transporter MDR1 gene in white subjects. Clin. Pharmacol. Ther. 69, 169–174 (2001).
Kobayashi, D., Ieiri, I., Hirota, T., Takane, H., Maegawa, S., Kigawa, J. et al. Functional assessment of ABCG2 (BCRP) gene polymorphisms to protein expression in human placenta. Drug. Metab. Dispos. 33, 94–101 (2005).
Tsujimoto, M., Hirata, S., Dan, Y., Ohtani, H. & Sawada, Y. Polymorphisms and linkage disequilibrium of the OATP8 (OATP1B3) gene in Japanese subjects. Drug. Metab. Pharmacokinet. 21, 165–169 (2006).
Gschwind, H. P., Pfaar, U., Waldmeier, F., Zollinger, M., Sayer, C., Zbinden, P. et al. Metabolism and disposition of imatinib mesylate in healthy volunteers. Drug. Metab. Dispos. 33, 1503–1512 (2005).
Maliepaard, M., Scheffer, G. L., Faneyte, I. F., van Gastelen, M. A., Pijnenborg, A. C., Schinkel, A. H. et al. Subcellular localization and distribution of the breast cancer resistance protein transporter in normal human tissues. Cancer Res. 61, 3458–3464 (2001).
Lepper, E. R., Nooter, K., Verweij, J., Acharya, M. R., Figg, W. D. & Sparreboom, A. Mechanisms of resistance to anticancer drugs: the role of the polymorphic ABC transporters ABCB1 and ABCG2. Pharmacogenomics 6, 115–138 (2005).
Imai, Y., Nakane, M., Kage, K., Tsukahara, S., Ishikawa, E., Tsuruo, T. et al. C421A polymorphism in the human breast cancer resistance protein gene is associated with low expression of Q141K protein and low-level drug resistance. Mol. Cancer Ther. 1, 611–616 (2002).
Glaeser, H., Bailey, D. G., Dresser, G. K., Gregor, J. C., Schwarz, U. I., McGrath, J. S. et al. Intestinal drug transporter expression and the impact of grapefruit juice in humans. Clin. Pharmacol. Ther. 81, 362–370 (2007).
Lee, W., Glaeser, H., Smith, L. H., Roberts, R. L., Moeckel, G. W., Gervasini, G. et al. Polymorphisms in human organic anion-transporting polypeptide 1A2 (OATP1A2): implications for altered drug disposition and central nervous system drug entry. J. Biol. Chem. 280, 9610–9617 (2005).
Itoda, M., Saito, Y., Shirao, K., Minami, H., Ohtsu, A., Yoshida, T. et al. Eight novel single nucleotide polymorphisms in ABCG2/BCRP in Japanese cancer patients administered irinotacan. Drug. Metab. Pharmacokinet. 18, 212–217 (2003).
Kobayashi, D., Ieiri, I., Hirota, T., Takane, H., Maegawa, S., Kigawa, J. et al. Functional assessment of ABCG2 (BCRP) gene polymorphisms to protein expression in human placenta. Drug. Metab. Dispos. 33, 94–101 (2005).
de Jong, F. A., Marsh, S., Mathijssen, R. H., King, C., Verweij, J., Sparreboom, A. et al. ABCG2 pharmacogenetics: ethnic differences in allele frequency and assessment of influence on irinotecan disposition. Clin. Cancer Res. 10, 5889–5894 (2004).
Mahon, F. X., Belloc, F., Lagarde, V., Chollet, C., Moreau-Gaudry, F., Reiffers, J. et al. MDR1 gene overexpression confers resistance to imatinib mesylate in leukemia cell line models. Blood 101, 2368–2373 (2003).
Nakanishi, T., Shiozawa, K., Hassel, B. A. & Ross, D. D. Complex interaction of BCRP/ABCG2 and imatinib in BCR-ABL-expressing cells: BCRP-mediated resistance to imatinib is attenuated by imatinib-induced reduction of BCRP expression. Blood 108, 678–684 (2006).
Jordanides, N. E., Jorgensen, H. G., Holyoake, T. L. & Mountford, J. C. Functional ABCG2 is overexpressed on primary CML CD34+ cells and is inhibited by imatinib mesylate. Blood 108, 1370–1373 (2006).
Jiang, X., Zhao, Y., Smith, C., Gasparetto, M., Turhan, A., Eaves, A. et al. Chronic myeloid leukemia stem cells possess multiple unique features of resistance to BCR-ABL targeted therapies. Leukemia. 21, 926–935 (2007).
Morisaki, K., Robey, R. W., Ozvegy-Laczka, C., Honjo, Y., Polgar, O., Steadman, K. et al. Single nucleotide polymorphisms modify the transporter activity of ABCG2. Cancer Chemother. Pharmacol. 56, 161–172 (2005).
Dulucq, S., Bouchet, S., Turcq, B., Lippert, E., Etienne, G., Reiffers, J. et al. Multidrug resistance gene (MDR1) polymorphisms are associated with major molecular responses to standard-dose imatinib in chronic myeloid leukemia. Blood 112, 2024–2027 (2008).
Kim, D. H., Sriharsha, L., Xu, W., Kamel-Reid, S., Liu, X., Siminovitch, K. et al. Clinical relevance of a pharmacogenetic approach using multiple candidate genes to predict response and resistance to imatinib therapy in chronic myeloid leukemia. Clin. Cancer Res. 15, 4750–4758 (2009).
Acknowledgements
We thank the Akita CML Study Group for its participation in this study; a complete membership appears in the ‘Appendix.’ We also thank Etsuko Kobayashi and Hiromi Kataho for technical assistance.
Author contributions: NT conceived and designed the research, analyzed results, arrived at the figures and wrote the paper; MM and SAS designed the research, analyzed results, arrived at the figures and wrote the paper; HK, YK, HT, NF, HS, TY and MH conducted experiments and discussed results; KS directed the study. The authors declare no competing financial interests.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Appendix
Appendix
The Akita CML Study Group: Hitoshi Ogasawara, Yoshiaki Hatano, Atsushi Kitabayashi, Yoshinari Kawabata, Jun Kuroki, Tamio Nishinari, Yutaka Nakayama, Hidetaka Niitsu, Yoshikazu Ichikawa, Ryutaro Inaba, Arata Watanabe, Kaoru Takahashi, Koki Saito, Masaaki Kume, Yoshinobu Saito, Atsushi Oshima, Akihiko Chubachi, Takashi Nimura, Mutsuhito Motegi, Naoto Takahashi, Kenichi Sawada.
Rights and permissions
About this article
Cite this article
Takahashi, N., Miura, M., Scott, S. et al. Influence of CYP3A5 and drug transporter polymorphisms on imatinib trough concentration and clinical response among patients with chronic phase chronic myeloid leukemia. J Hum Genet 55, 731–737 (2010). https://doi.org/10.1038/jhg.2010.98
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2010.98
Keywords
This article is cited by
-
Effects of CYP3A4/5 and ABC transporter polymorphisms on osimertinib plasma concentrations in Japanese patients with non-small cell lung cancer
Investigational New Drugs (2022)
-
Influences of ABC transporter and CYP3A4/5 genetic polymorphisms on the pharmacokinetics of lenvatinib in Chinese healthy subjects
European Journal of Clinical Pharmacology (2020)
-
Comprehensive analyses of safety and efficacy toward individualizing imatinib dosage in patients with chronic myeloid leukemia
International Journal of Hematology (2020)
-
Influence of CYP3A4/5 and ABC transporter polymorphisms on lenvatinib plasma trough concentrations in Japanese patients with thyroid cancer
Scientific Reports (2019)
-
Impact of CYP3A4*22 on Pazopanib Pharmacokinetics in Cancer Patients
Clinical Pharmacokinetics (2019)