Abstract
Toll-like receptors (TLRs) and myeloid differentiation primary response protein 88 (MYD88) gene polymorphisms may be involved in the pathogenesis of Hodgkin's lymphoma (HL) through altered immunoregulatory and inflammatory responses. A candidate–gene association study was conducted to investigate the association between TLR9 −1237T>C, TLR9 2848A>G, MYD88 −938C>A and MYD88 1944C>G gene polymorphisms and the risk for HL. The impact of haplotypes was also examined. The study showed that carriership for −1237C and 2848A was associated with an increased risk for HL (odds ratio (OR)=2.53 (1.36–4.71) and OR=6.20 (1.3–28.8)). The MYD88 polymorphisms produced nonsignificant results. The estimated frequencies of the TLR9/1237C-2848A and MYD88/938C-1944G haplotypes were also significantly different between HL and controls (P<0.01). In addition, a significant difference between HL and controls was observed for the TLR9/1237C-TLR9/2848A-MYD88/938C-MYD88/1944C haplotypes (P<0.01). In conclusion, our study showed that TLR polymorphisms, and TLR9 and MYD88 haplotypes are related to the development of HL.
Similar content being viewed by others
Introduction
Hodgkin's lymphoma (HL) is an uncommon neoplasm with an age-adjusted incidence of 2.5–3.1 per 10E5 in the Western world.1, 2 Involved lymph nodes show an inflammatory cellular background and rare Reed Sternberg (RS) cells, which are the malignant cells of HL. The pathogenesis of HL remains unclear. A transcription factor that has been implicated in the pathogenesis of HL is nuclear factor-κB (NF-κB), a pleiotropic mediator of inflammation. Strong constitutive NF-κB activity is a common feature of HL cell lines3 and is required for the proliferation and survival of RS cells.3 However, the cause of NF-kB triggering is still elusive, but there is evidence that it may be linked to the Epstein Bar Virus (EBV), a herpes virus that has been associated with HL.4, 5, 6, 7, 8, 9 In addition, one of the EBV proteins, the Latent Membrane Protein 1 (LMP1), activates NF-κB, stimulates cell proliferation and prevents apoptosis.10
Family studies have shown that inherited factors may also have a role in the development of HL; individuals related to HL patients have more than a three-fold increased risk of developing HL, as shown by population11, 12, 13, 14, 15 and twin studies.16 Factors that are involved in EBV recognition and NF-kB activation are the Toll-like receptors (TLRs). Specifically, TLR9 recognizes viral CpG islands and, once activated, it signals through myeloid differentiation primary response protein 88 (MYD88) and leads to NF-κB activation.17, 18, 19 Considering the importance of TLRs in NF-κB activation, one could hypothesize that these receptors may have a role in the abundant inflammatory background present in HL. To test this hypothesis, we chose to examine whether genetic variations in TLR9 and MYD88 are associated with the development of HL. Previous studies in HL20 showed an odds ratio (OR) of 0.82 for TLR9-1237C that was of borderline significance, whereas weak associations were also detected for follicular lymphoma and chronic lymphocytic leukemia.
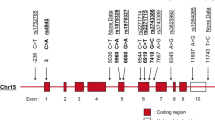
TLR9 is located on chromosome 3p21.3;21 it consists of two exons and two single-nucleotide polymorphisms (SNPs) define the four most common haplotypes in Caucasians.22 These include the −1237T>C (dbSNP rs5743836) and the synonymous 2848A>G (P545P) (dbSNP rs352140) SNP located in exon 2. TLR9 is in close proximity to the MYD88 gene, which is located on chromosome 3p22 and consists of five exons.23 The −938C>A SNP (dbSNP rs4988453) and the 1944C>G (dbSNP rs4988457) SNP define the two most common haplotypes in Caucasians.24 In this analysis, we undertook a gene–candidate association study to investigate whether the above-mentioned polymorphisms contribute to the risk of HL.
Materials and methods
Subjects
A total of 90 formalin-fixed paraffin-embedded tissue sections collected from HL patients were analyzed from the Pathology Laboratories of Hygeia Hospital (Athens, Greece), the Evaggelismos Hospital (Athens, Greece) and from the University Hospital of Larissa (Larissa, Greece). All patients were of Caucasian origin and met the World Health Organization criteria for classic HL. Peripheral blood samples were obtained from 92 healthy subjects from the University Hospital of Larissa (Larissa, Greece), after receiving informed consent. The control subjects were healthy individuals of Caucasian origin, with no known history of HL or any other disorder.
SNP genotyping
Case and control subjects were genotyped for the TLR9 (GenBank Accession No. NM_017442) and MYD88 (GenBank Accession No. NM_002468) SNPs of interest. After consecutive attempts, genotyping was successful for 86 HL cases and for 84 control subjects for the TLR9 −1237T>C SNP, for 90 cases and 90 controls for the TLR9 2848A>G SNP, for 90 cases and 87 controls for the MYD88 −938C>A SNP and for 86 cases and 89 controls for the MYD88 1944C>G SNP. PCR was used to amplify DNA fragments encompassing SNPs of interest in a typical reaction containing the 1 × PCR buffer, ∼30 ng genomic DNA, 1–1.5 mM MgCl2, 0.2 mM dNTPs, 0.2 mM of each primer and 1.25 Units Go Taq Flexi Polymerase (Promega, Southampton, UK). Samples were denatured for 5 min at 96 °C and subjected to 35 cycles of denaturation at 96 °C for 1 min, annealing at 56–64 °C (depending on the primers used) for 1 min and extension at 72 °C for 1 min, followed by an extension step at 72 °C for 5 min.
The TLR9 −1237T>C genotypes were determined by amplification of a 456 bp fragment of the 5′-flanking region of TLR9 using primers 5′-AAG AAG CTG ACA TTC CAG CAG GG-3′ (forward) and 5′-CTA GGT CCC TCC TCT GCT CAG AC-3′ (reverse) at 64 °C annealing, followed by BstNI digestion of the PCR product. Digestion resulted in fragments of 31, 38, 48, 89, 112 and 186 bp in the presence of the T allele, and in fragments of 31, 38, 48, 89, 112 and 138 bp in the presence of the C allele. The TLR9 2848A>G genotypes were identified by amplification of a 371 bp fragment of exon 2 using primers 5′-TGG ATC TGC CAC GGA ACA ACC-3′ (forward) and 5′-CAG CGA CGT ACT GCA GAG CTG-3′ (reverse) at 62 °C annealing, followed by BstUI digestion. Digestion of the PCR product resulted in fragments of 226 and 145 bp in the presence of the G allele, and 371 bp in the presence of the A allele. The MYD88 −938C>A genotypes were determined by PCR amplification of a 503 bp fragment of the 5′-flanking region of MYD88 using primers 5′-GCA GCC AGG ACC GCT TACT GC T-3′ (forward) and 5′-GCA CGT GGC CTT GCC CTT GCC CTT TAG G-3′ (reverse) at 62 °C annealing, followed by BsrI digestion of the PCR product. The expected fragment sizes after digestion were 23, 97, 165 and 218 bp in the presence of the C allele, and 97, 165 and 241 bp in the presence of the A allele. The MYD88 1944C>G genotypes were identified by amplification of a 448 bp fragment of intron 3 using primers 5′-GCC CCA GCG ACA TCC AGT TTG TG-3′ (forward) and 5′-TCT TGC CAG AGC AGG GTT GAG CTT-3′ (reverse) at 56 °C annealing, followed by Cac8I digestion. Digestion of the PCR products resulted in fragments of 92, 135 and 221 bp in the presence of the G allele, and in fragments of 135 and 313 bp in the presence of the C allele. At least 10% of the samples were randomly selected as an internal control for repeated genotyping.
Data analysis
The genotypes were tested for Hardy–Weinberg (HW) equilibrium and the loci were tested for linkage disequilibrium using exact tests according to Weir.25, 26 The haplotype frequencies were estimated and compared using PHASE v2.1 (Seattle, WA, USA) (http://www.stat.washington.edu/stephens/). The disequilibrium and correlation coefficients were estimated according to Weir.26 The genotype distribution, allele contrast and the dominant model (risk allele carriers) of the HL patients was compared with the control group using a log-linear model.27 The comparisons were expressed in terms of OR unadjusted and adjusted for age and sex. A P-value of <0.05 was considered statistically significant.
Results
Demographic characteristics of the study population
A total of 91 cases and 92 controls were analyzed in this study. The mean age (±s.d.) was 42.9±18.5 and 35.5±10.1 years for cases and controls, respectively; there were 44 (50.6%) males and 43 (49.4%) females in the case group, whereas the control group comprised 27 (29.3%) males and 65 (70.7) females. HL samples were of the following histological subtypes: nodular sclerosis (73 cases), mixed cellulary (15 cases) and lymphocyte rich (3 cases). The control subjects were younger and comprised a higher percentage of females than did the cases.
Genotype distributions and study quality
The distributions of the TLR9 −1237T>C, TLR9 2848A>G, MYD88 −938C>A and MYD88 1944C>G genotypes in both cases and controls are shown in Table 1. Significant differences were detected in the distribution of genotypes of the two TLR polymorphisms between cases and controls (P=0.01 for TLR9 −1237T>C and P=0.03 for TLR9 2848A>G). In contrast, there were no differences for the MYD88 polymorphisms (P=0.16 for MYD88 −938C>A and P=0.25 for MYD88 1944C>G). No individuals homozygous for the mutant allele in either cases or controls were present for the MYD88 polymorphisms.
The controls were in HW equilibrium for all investigated polymorphisms, indicating the lack of stratification and/or genotyping error28 (P=0.11 for TLR9 −1237T>C, P=0.37 for TLR9 2848A>G, P=0.99 for MYD88 −938C>A and P=0.60 for MYD88 1944C>G).
Polymorphisms in TLR9 and association with HL
Table 2 shows the association results for the TLR9 polymorphisms. The allele contrast showed that for the −1237C allele there was a two-fold risk for HL relative to the −1237T allele (OR=1.99 (1.18–3.36)). Furthermore, −1237C-carrier individuals were associated with a higher risk of HL unadjusted and adjusted for age and sex (OR=2.53 (1.36–4.71) and OR=2.02 (1.04–3.89), respectively).
With regard to the TLR9 2848A>G polymorphism, the allele contrast produced a marginal association (OR=1.54 (1.00–2.39)). 2848A carriers had an increased risk for HL, as the unadjusted OR was significant (OR=6.20 (1.3–28.8)); however, the adjusted OR was marginally significant (OR=4.66 (1.00–22.9)).
Polymorphisms in the MYD88 gene and association with HL
Table 2 shows that the MYD88 polymorphisms produced nonsignificant results. The allele contrasts −938C vs A and 1944G vs C were not significant (OR=1.77 (0.75–4.16) and OR=1.40 (0.77–2.56)). In addition, 1944G carriers were not associated with increased risk of HL (unadjusted OR=1.47 (0.76–2.84) and adjusted OR=1.38 (0.68–2.78)).
TLR9 and MYD88 haplotype frequency in HL patients and control subjects
Table 3 shows the P-values, and the respective D′ and r2, for testing linkage disequilibrium between pairs of SNPs for HL patients and controls. In the patient population, TLR9 −1237T>C was in linkage disequilibrium with TLR9 2848A>G (P<0.01), MYD88 −938C>A (P=0.04) and MYD88 1944C>G (P=0.05). TLR9 2848A>G was also found in linkage disequilibrium with MYD88 −938C>A (P<0.01) in HL patients. In controls, the two MYD88 polymorphisms were in linkage disequilibrium (P<0.01) (Table 3).
The distribution of the estimated haplotype frequency of the two TLR9 polymorphisms and the two MYD88 polymorphisms for the HL and controls is presented in Table 4. Regarding the TLR9 haplotypes, there was an overall significant difference between the HL and controls (P=0.03). This difference was due to the 1237C-2848A haplotype (or the 1237T-2848G haplotype) (P<0.01). For the MYD88 haplotypes, the overall difference was not significant (P=0.20). However, the estimated frequency of the haplotype 938C-1944G was different in HL and controls; this difference might be due to the linkage disequilibrium with the TLR9 polymorphisms or because of the interaction between the two polymorphisms, given that the individual MYD88 polymorphisms were not significant.
When the estimated haplotypes of the four investigated polymorphisms were considered (Table 5), a significant difference between HL and controls was observed for the 1237T-2848G-938C-1944C and the 1237C-2848A-938C-1944C haplotypes (P<0.01), further indicating the association of 1237T and 2848G alleles (or allele carriers) with HL susceptibility.
Discussion
This study investigated whether certain TLR9 and MYD88 gene polymorphisms were associated with the development of HL. Our results showed that the TLR9 −1237C allele confers a two-fold increased risk of HL and that the TLR9 2848A allele increased HL risk by ∼4.5-fold in the Caucasian population examined. None of the MYD88 SNPs analyzed (MYD88 −938C>A and MYD88 1944C>G) were found to alter the susceptibility to HL. The genotype distributions of the SNPs examined were all in HW in the control group, indicating no population stratification. Haplotype analysis also showed that the distribution of the TLR9 1237C-2848A haplotypes were different between cases and controls.
Others have also examined the role of TLRs and particularly that of TLR9 gene polymorphisms in susceptibility to human diseases associated with altered immune responses and inflammation. Among the other TLR polymorphisms, Nieters et al.20 investigated the contribution of the TLR9 −1486T>C and −1237T>C SNPs to the development of lymphomas, including 115 cases of HL. A 20% decreased risk of all lymphomas was associated with the TLR9 −1237C allele, but this was of borderline significance. In contrast to our study, no contribution of the −1237T>C SNP to HL was found.
Although significant associations were detected in our study, the size was relatively small. However, candidate–gene association studies have the tendency to lack the power to detect a statistically significant association. For example, to achieve a power of >80% to identify a modest genetic effect (OR=1.2) of a polymorphism present in 10% of individuals, a sample size of ⩾10 000 subjects would be required.28 Therefore, the sample sizes required to predict association have to be far beyond what is currently available and no single institution or entity alone will be able to provide a reasonable number of patients. However, a future meta-analysis of multiple studies clearly has a role in offering an analysis with the potential for higher power.28, 29 Future collaborative studies may allow the pooling of data, providing more power to detect significant associations. Furthermore, consortia performing gene–candidate or genome-wide association studies will be able to replicate the validity of the present findings.
This study was based on the hypothesis that genetic variations in TLR9 and MYD88, both of which have crucial roles in immunity and inflammation, could alter the downstream immunological responses after NF-κB activation. Given that increased NF-κB activation is a characteristic of HL cell lines and is required for the proliferation and survival of RS cells,3 TLR expression variability could participate in the pathogenesis of HL. This hypothesis was further supported by the fact that EBV has been repeatedly associated with the development of HL and that, on EBV infection, LMP1 constitutively transmits signals that activate NF-κB.10
So far, the functional role of the TLR9 −1237T>C polymorphism seems controversial. Deletions spanning the −3.2 to −0.7 kb promoter region did not alter the TLR9 promoter activity,30 although the region was shown to be important for the Human Papillomavirus 16-mediated inhibition of TLR9 expression.31 In silico analysis of the TLR9 promoter showed that the −1237T>C change introduces a putative c-Rel/NF-κB transcription factor binding site;32 in vitro gene reporter assays showed that the TLR9 −1237T>C SNP alters the TLR9 promoter activity, with the −1237T allele having a higher promoter activity (P=0.018), suggesting the existence of regulatory elements across the polymorphic site33 and implying that the −1237C allele is associated with lower TLR9 expression levels.
In conclusion, this study showed that a genetic variation in TLR9 may alter the susceptibility to HL. Although the functional significance, if any, of the TLR9 −1237T>C and the TLR9 2848A>G SNPs remains to be elucidated, our results suggest that TLR9 polymorphisms and TLR9 and MYD88 haplotypes may be involved in the pathogenesis of HL.
References
Ries, L. A. G., Harkins, D., Krapcho, M., Mariotto, A., Miller, B. A., Feuer, E. J. et al. SEER Cancer Statistics Review, 1975–2005 (National Cancer Institute, Bethesda, MD, 2006) (http://seer.cancer.gov/statfacts/html/hodg.html).
Cartwright, R. A. & Watkins, G. Epidemiology of Hodgkin's disease: a review. Hematol. Oncol. 22, 11–26 (2004).
Bargou, R. C., Emmerich, F., Krappmann, D., Bommert, K., Mapara, M. Y., Arnold, W. et al. Constitutive nuclear factor-kappaB-RelA activation is required for proliferation and survival of Hodgkin's disease tumor cells. J. Clin. Invest 100, 2961–2969 (1997).
Serraino, D., Franceschi, S., Talamini, R., Barra, S., Negri, E., Carbone, A. et al. Socio-economic indicators, infectious diseases and Hodgkin's disease. Int. J. Cancer 47, 352–357 (1991).
Levine, R., Zhu, K., Gu, Y., Brann, E., Hall, I., Caplan, L. et al. Self-reported infectious mononucleosis and 6 cancers: a population-based, case-control study. Scand J. Infect. Dis. 30, 211–214 (1998).
Hjalgrim, H., Askling, J., Sorensen, P., Madsen, M., Rosdahl, N., Storm, H. H. et al. Risk of Hodgkin's disease and other cancers after infectious mononucleosis. J. Natl Cancer Inst. 92, 1522–1528 (2000).
Alexander, F. E., Daniel, C. P., Armstrong, A. A., Clark, D. A., Onions, D. E., Cartwright, R. A. et al. Gene clustering, Epstein-Barr virus Reed-Sternberg cell status and herpes virus serology in Hodgkin's disease: results of a case-control study. Eur. J. Cancer 31A, 1479–1486 (1995).
Grässer, F. A., Murray, P. G., Kremmer, E., Klein, K., Remberger, K., Feiden, W. et al. Monoclonal antibodies directed against the Epstein-Barr virus-encoded nuclear antigen 1 (EBNA1): immunohistologic detection of EBNA1 in the malignant cells of Hodgkin's disease. Blood 84, 3792–3798 (1994).
Gallagher, A., Armstrong, A. A., MacKenzie, J., Shield, L., Khan, G., Lake, A. et al. Detection of Epstein-Barr virus (EBV) genomes in the serum of patients with EBV-associated Hodgkin's disease. Int. J. Cancer 84, 442–448 (1999).
Hiscott, J., Kwon, H. & Genin, P. Hostile takeovers: viral appropriation of the NF-kappaB pathway. J. Clin. Invest 107, 143–151 (2001).
Goldgar, D. E., Easton, D. F., Cannon-Albright, L. A. & Skolnick, M. H. Systematic population-based assessment of cancer risk in first-degree relatives of cancer probands. J. Natl Cancer Inst. 86, 1600–1608 (1994).
Westergaard, T., Melbye, M., Pedersen, J. B., Frisch, M., Olsen, J. H. & Andersen, P. K. Birth order, sibship size and risk of Hodgkin's disease in children and young adults: a population-based study of 31 million person-years. Int. J. Cancer 72, 977–981 (1997).
Paltiel, O., Schmit, T., Adler, B., Rachmilevitz, E. A., Polliack, A., Cohen, A. et al. The incidence of lymphoma in first-degree relatives of patients with Hodgkin disease and non-Hodgkin lymphoma: results and limitations of a registry-linked study. Cancer 88, 2357–2366 (2000).
Shugart, Y. Y., Hemminki, K., Vaittinen, P., Kingman, A. & Dong, C. A genetic study of Hodgkin's lymphoma: an estimate of heritability and anticipation based on the familial cancer database in Sweden. Hum. Genet. 106, 553–556 (2000).
Goldin, L. R., Pfeiffer, R. M., Gridley, G., Gail, M. H., Li, X., Mellemkjaer, L. et al. Familial aggregation of Hodgkin lymphoma and related tumors. Cancer 100, 1902–1908 (2004).
Mack, T. M., Cozen, W., Shibata, D. K., Weiss, L. M., Nathwani, B. N., Hernandez, A. M. et al. Concordance for Hodgkin's disease in identical twins suggesting genetic susceptibility to the young-adult form of the disease. N. Engl. J. Med. 332, 413–418 (1995).
Parker, L. C., Prince, L. R. & Sabroe, I. Translational mini-review series on Toll-like receptors: networks regulated by Toll-like receptors mediate innate and adaptive immunity. Clin. Exp. Immunol. 147, 199–207 (2007).
Bowie, A. G. & Haga, I. R. The role of Toll-like receptors in the host response to viruses. Mol. Immunol. 42, 859–867 (2005).
Hemmi, H., Takeuchi, O., Kawai, T., Kaisho, T., Sato, S., Sanjo, H. et al. Toll-like receptor recognizes bacterial DNA. Nature 408, 740–745 (2000).
Nieters, A., Beckmann, L., Deeg, E. & Becker, N. Gene polymorphisms in Toll-like receptors, interleukin-10, and interleukin-10 receptor alpha and lymphoma risk. Genes Immun. 7, 615–624 (2006).
Du, X., Poltorak, A., Wei, Y. & Beutler, B. Three novel mammalian toll-like receptors: gene structure, expression, and evolution. Eur. Cytokine Netw. 11, 362–371 (2000).
Lazarus, R., Klimecki, W. T., Raby, B. A., Vercelli, D., Palmer, L. J., Kwiatkowski, D. J. et al. Single-nucleotide polymorphisms in the Toll-like receptor 9 gene (TLR9): frequencies, pairwise linkage disequilibrium, and haplotypes in three U.S. ethnic groups and exploratory case-control disease association studies. Genomics 81, 85–91 (2003).
Bonnert, T. P., Garka, K. E., Parnet, P., Sonoda, G., Testa, J. R. & Sims, J. E. The cloning and characterization of human MyD88: a member of an IL-1 receptor related family. FEBS Lett. 402, 81–84 (1997).
Lazarus, R., Vercelli, D., Palmer, L. J., Klimecki, W. J., Silverman, E. K., Richter, B. et al. Single nucleotide polymorphisms in innate immunity genes: abundant variation and potential role in complex human disease. Immunol. Rev. 190, 9–25 (2002).
Lewis, P. O. & Zaykin, D. Genetic Data Analysis: computer program for the analysis of allelic data release 1.0 (2001).
Weir, B. S. Genetic Data Analysis II (Sinauer Associates, Inc, Sunderland, MA, USA, 1996).
Baker, R. J. GLIM 3.77 Reference Manual (Numerical Algorithms Group Ltd, Oxford, UK, 1987).
Zintzaras, E. & Lau, J. Synthesis of genetic association studies for pertinent gene-disease associations requires appropriate methodological and statistical approaches. J. Clin. Epidemiol. 61, 634–645 (2008).
Zintzaras, E., Kitsios, G. D., Triposkiadis, F., Lau, J. & Raman, G. APOE gene polymorphisms and response to statin therapy. Pharmacogenomics J. 4, 248–257 (2009).
Takeshita, F., Suzuki, K., Sasaki, S., Ishii, N., Klinman, D. M. & Ishii, K. J. Transcriptional regulation of the human TLR9 gene. J. Immunol. 173, 2552–2561 (2004).
Hasan, U. A., Bates, E., Takeshita, F., Biliato, A., Accardi, R., Bouvard, V. et al. TLR9 expression and function is abolished by the cervical cancer-associated human papillomavirus type 16. J. Immunol. 178, 3186–3197 (2007).
Hamann, L., Glaeser, C., Hamprecht, A., Gross, M., Gomma, A. & Schumann, R. R. Toll-like receptor (TLR)-9 promotor polymorphisms and atherosclerosis. Clin. Chim. Acta. 364, 303–307 (2006).
Novak, N., Yu, C. F., Bussmann, C., Maintz, L., Peng, W. M., Hart, J. et al. Putative association of a TLR9 promoter polymorphism with atopic eczema. Allergy 62, 766–772 (2007).
Acknowledgements
This work was supported in part by Grant EP.AN, YB-90 (GSRT, Athens, GR) and by CONSERT (LSHB 005242, EU).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mollaki, V., Georgiadis, T., Tassidou, A. et al. Polymorphisms and haplotypes in TLR9 and MYD88 are associated with the development of Hodgkin's lymphoma: a candidate–gene association study. J Hum Genet 54, 655–659 (2009). https://doi.org/10.1038/jhg.2009.90
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2009.90
Keywords
This article is cited by
-
TLR4 896A/G and TLR9 1174G/A polymorphisms are associated with the risk of infectious mononucleosis
Scientific Reports (2020)
-
Association of Toll-like receptor 3 and Toll-like receptor 9 single-nucleotide polymorphisms with hepatitis C virus persistence among Egyptians
Archives of Virology (2018)
-
Association between toll-like receptors 9 (TLR9) gene polymorphism and risk of pulmonary tuberculosis: meta-analysis
BMC Pulmonary Medicine (2015)
-
Toll-like receptors in the pathogenesis of human B cell malignancies
Journal of Hematology & Oncology (2014)
-
Polymorphisms and haplotypes in MyD88 are associated with the development of sarcoidosis: a candidate-gene association study
Molecular Biology Reports (2013)