Abstract
Mutations in CDH1, which encodes E-cadherin, have been associated with hereditary diffuse gastric cancer (HDGC) in Western populations but have not been shown to play a major role in Asians. Recently, a patient with familial gastric cancer (FGC) was shown to harbor a germline mutation in the TP53 gene, which encodes p53 and has been previously associated with Li-Fraumeni Syndrome (LFS). To determine whether mutations in TP53 are associated with FGC in Asians, we screened the entire coding region of TP53 in probands from 23 Korean FGC families. We identified a nonsense (E287X) TP53 germline mutation in a family whose history is compatible with both HDGC and LFS. Two members of this family (SNU-G2) were afflicted with brain tumors, seven with gastric cancers, two with sarcomas, and one with both gastric cancer and a sarcoma. The E287X TP53 mutation segregated with the cancer phenotype in the family members from whom DNA samples were available. To our knowledge, this is the first report of a large family with both HDGC and LFS. Our results suggest that TP53 mutational screening in FGC families should be interpreted with caution because additional TP53 mutation-carrying HDGC families may also show LFS-related phenotypes.
Similar content being viewed by others
Introduction
Germline mutations in CDH1, which encodes E-cadherin, were first associated with familial gastric cancer (FGC) when germline mutations were found in a large Maori family with hereditary diffuse gastric cancer (HDGC) (Guilford et al. 1998). Since then, several other groups have reported CDH1 germline mutations in HDGC families. Western populations show a large proportion of truncating mutations (25–37%) in this gene (Oliveira et al. 2002) whereas East-Asian countries that show very high rates of gastric cancer were found to have only a few missense germline mutations in CDH1 (Yabuta et al. 2002; Iida et al. 1999; Kim et al. 2000), suggesting that there may be a second causative gene for HDGC. Researchers have sought to identify another genetic event in FGC patients (Lee et al. 2000; Kim et al. 2003); our lab and another Korean group found MET germline mutations in one out of 24 Korean FGC patients (Kim et al. 2003) and one out of 85 gastric cancer patients with unknown family histories (Lee et al. 2000). However, no major genetic cause for FGC has yet been identified in an East-Asian population.
Recently, a TP53 germline missense mutation was found in a European FGC patient without CDH1 germline mutation (Keller et al. 2004). Thus, we investigated whether TP53 germline mutations contribute to development of FGC without CDH1 germline mutations in a Korean population. We screened probands from 23 Korean FGC families for TP53 mutations and identified a single nonsense germline mutation in one large HDGC family. A thorough investigation revealed that the family history of this pedigree was also compatible with Li-Fraumeni syndrome (LFS), which is characterized by a family constellation including a proband younger than 45 years with a sarcoma having a first-degree relative younger than 45 years with any cancer and an additional first-degree or second-degree relative younger than 45 years in the same lineage with any cancer or a sarcoma at any age (Li et al. 1988).
Materials and methods
Patient samples
Twenty-three Korean families affected with FGC were investigated for TP53 germline mutations. These families had previously been screened for CDH1 and MET germline mutations (Yoon et al. 1999; Kim et al. 2003). Criteria for family inclusion were at least two first-degree or second-degree relatives affected with gastric cancer, at least one of which was diagnosed with cancer prior to age 50 (Yoon et al. 1999). Out of 23 probands, 11 represented families suffering from diffuse-type gastric cancer, four represented families suffering from intestinal types, and histological data for the type of the remaining eight families were not available. Blood samples from each proband were collected from Seoul National University Hospital, and affected and unaffected members of family SNU-G2 were sampled following identification of a mutation in this family. Informed consent was obtained from all participants prior to testing. Total genomic DNA was extracted from the blood samples using Ficoll-Paque (Amersham Pharmacia Biotech, Uppsala, Sweden) and the Trizol reagent (Invitrogen, Carlsbad, CA, USA) according to the manufacturers’ instructions.
PCR amplification and sequencing
Fragments covering the entire coding sequence of TP53 were PCR amplified as previously described (Bakkar et al. 2003). PCR reactions were carried out in a volume of 25 ul containing 100 ng genomic DNA, 10 pmol of each primer, 250 μM each dNTP, 0.5 units of Taq polymerase, and the reaction buffer provided by the supplier (QIAGEN, Hilden, Germany). Samples were denatured for 5 min at 94°C in a GeneAmp PCR system 9700 (Applied Biosystems, Inc., Foster City, CA, USA) then amplified by 35 cycles of 94°C for 30 s, 56°C for 30 s, and 72°C for 1 min with a final elongation of 10 min at 72°C. Exons 2–11 of TP53 were bidirectionally sequenced in duplicate reactions using the Taq dideoxy terminator cycle sequencing kit and an ABI 3100 DNA sequencer (Applied Biosystems). Samples showing a mutation in direct sequencing were freshly PCR amplified, ligated into PCR-TOPO vectors (Invitrogen), and subcloned using the TA cloning system (Invitrogen) for sequencing and confirmation of the mutation.
Two patients in family SNU-G2 who had been previously reported to harbor CDH1 germline mutations (Yoon et al. 1999) were rescreened at this gene in an attempt to confirm the mutations by direct sequencing.
Denaturing high-performance liquid chromatography (DHPLC) analysis
Members of family SNU-G2 were screened for the presence of TP53 germline mutations by DHPLC (WAVE, Transgenomic, Omaha, USA). DHPLC analyses were performed as described by Kim et al. (2003). Melting curves were investigated by WAVEMAKER (WAVE) software to set the optimized temperature for each amplicon. Samples showing abnormal DHPLC results were further examined by automatic sequencing.
Immunohistochemistry (IHC)
Among the family members, two patients had undergone surgical resection for liposarcoma and medulloblastoma, respectively, and their paraffin blocks were available. Immunohistochemistry was performed on the two paraffin-embedded tissue sections using the avidin–biotin peroxidase complex (ABC) method. After antigen retrieval using a citrate buffer solution (Antigen Unmasking Solution, Vector Laboratories, Burlingame, CA, USA) for 15 min in an 800-W microwave oven, mouse anti-p53 monoclonal antibody (clone Bp53.11, DAKO, Carpinteria, CA; dilution 1:50) was applied. Negative controls included the use of nonimmune serum or PBS in place of the primary antibody.
Results
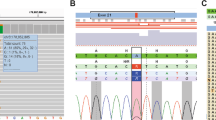
Out of 23 Korean FGC probands tested, we found a nonsense TP53 germline mutation [E287X mutation in exon 8 (codon 287, GAG→TAG)] in the proband for family SNU-G2, which had been diagnosed as an HDGC family according to the criteria suggested by Caldas et al. (1999). As TP53 germline mutations are found in about 70% of LFS patients, we thoroughly investigated the history of family SNU-G2 and found, to our surprise, that this family also showed evidence of the sarcoma and brain tumor incidences characteristic of LFS. The proband of SNU-G2 died of gastric cancer, as did his five older siblings (three male, two female) (Fig. 1). The father of the proband died of a brain tumor, his mother died of gastric cancer, and his eldest brother had both a liposarcoma and gastric cancer. The proband’s five siblings were not available for genetic analysis due to a lack of tissue samples, but we were able to obtain blood samples from 14 of the siblings’ children, two of whom were affected with LFS. One had died of a brain tumor while the other had a metastatic lung leiomyosarcoma of unknown origin. For segregation analysis of the mutation within family SNU-G2, the 14 members of the third generation were all screened for the presence of E287X TP53 germline mutation. We identified eight carriers of the mutation and six noncarriers. Of the eight carriers, two were the individuals affected with LFS whereas the other six individuals showed no symptoms of the disease. None of the noncarriers showed any clinical phenotype related with LFS. Thus, the E287X TP53 germline mutation appeared to be associated with the cancer phenotype in family SNU-G2. Although this family was previously reported as harboring a CDH1 missense mutation, we were unable to confirm this mutation by direct sequencing. Immunohistochemical staining for p53 did not show any p53 nuclear protein accumulation in the tumor cells of the liposarcoma or medulloblastoma samples.
TP53 germline mutation in exon 8 of the proband of family SNU-G2. a Automatic sequencing showing the nucleotide substitution that results in an amino-acid change (E287X). b Pedigree of SNU-G2 with both hereditary diffuse gastric cancer (HDGC) and Li-Fraumeni Syndrome (LFS). Square male, circle female, solid symbols affected with gastric cancer, diagonal symbols deceased, arrow mutation carrier, pro proband, BR brain tumor, ML metastatic leiomyosarcoma, LS liposarcoma. The numbers indicate ages of death (for deceased family members) or age at the time of analysis (for living family members).
Discussion
Recently, a European group found a TP53 germline mutation in one gastric cancer patient (Keller et al. 2004). In search of a genetic mechanism for hereditary gastric cancer in families without CDH1 or MET germline mutations, we screened the entire coding region of TP53 in 23 Korean FGC families. We identified a nonsense germline TP53 mutation in one HDGC family (SNU-G2) that had been previously reported as having a CDH1 germline missense mutation (Yoon et al. 1999). This unexpected result prompted us to carefully rescreen CDH1 in this family (SNU-G2) and another CDH1 mutation-carrying family (SNU-G1001). Repeated experiments with DHPLC and automatic sequencing did not show any CDH1 germline mutations in these two families. We hypothesize that the previous incorrect results might have originated from experimental artifacts generated during the PCR-SSCP or cloning-sequencing steps. Further analysis of family SNU-G2, in which the TP53 mutation seemed to segregate with the cancers, revealed that the phenotypes in this family were compatible with both HDGC and LFS.
LFS is a rare autosomal hereditary cancer syndrome characterized by a combination of tumors, predominantly sarcomas, breast cancers, brain tumors, and adrenocortical carcinomas (Olivier et al. 2003). Other less-common cancers have also been associated with LFS, including leukemia, lung cancers, melanoma, gastric cancers, pancreatic cancer, and prostate cancer (Olivier et al. 2003; Birch et al. 2001). According to the IARC (International Agency for Research on Cancer) database, gastric cancer has been reported in up to 2.8% of LFS families (Olivier et al. 2003). With this low frequency of gastric cancers in LFS, it is easy to overlook the possibility of LFS in families that appear to segregate gastric cancer. As no clinical symptom of sarcoma had been seen in family SNU-G2, we had previously reported this family, containing six gastric cancer patients and one brain tumor patient, as affected with HDGC. Based on our mutational and clinical analysis, however, we suggest that this family may additionally suffer from LFS.
TP53 germline mutations have been identified in about 70% (Olivier et al. 2003) of LFS patients; more than 70% of the mutations are missense mutations (Chompret 2002; Olivier et al. 2003), and up to 90% of the missense mutations are located in exons 5–8 (Chompret 2002), which is thought to comprise the DNA-binding domain. The cancer risk in mutation carriers has been reported to be as high as 73% in males and almost 100% in females due to the breast cancer risk (Chompret 2002). The E287X mutation found in family SNU-G2 was located in exon 8 near one of the hotspot codons, 282. TP53 null mutations are a poor prognostic indicator in lung cancer (de Anta et al. 1997), and mutations in exons 7 and 8 are also predictive of poor prognosis (Huang et al. 1998; Mitsudomi et al. 2000) although the latter has been disputed (Vega et al. 1997). Thus, it is possible that the HDGC/LFS phenotype in family SNU-G2 may be due to an aggressive nonsense mutation (E287X) in exon 8. Consistent with the previous report, no p53 nuclear protein accumulation was detected (Fenoglio-Preiser et al. 2003). It has been reported that p53 IHC fails to detect nonsense, splice, or null mutation gene products (Mitsudomi et al. 2000). It was previously reported that familial breast cancers could occur simultaneously with LFS, as breast cancer is a major component of LFS (Martin et al. 2003). Although a TP53 germline missense mutation was previously reported in a case of LFS presenting with a non-FGC (Sugano et al. 1999), this is the first report of a large family with a TP53 germline mutation associated with both HDGC and LFS. However, it is not clear whether the gastric cancer common in family SNU-G2 is due to LFS or whether it was inherited irrespective of LFS. The proband’s father died of a brain tumor, which is one of the major cancers in LFS, whereas the proband’s mother died of gastric cancer. Thus, it is possible that in this family, the LFS originated from the paternal allele and the HDGC came from the maternal allele. In support of this, it has been suggested that the less prevalent tumors in LFS, such as gastric cancers, might occur by chance; it is not clear whether the TP53 germline mutations contributed to these cancers (Olivier et al. 2003). As gastric cancer is the most common cancer in Korea (Shin et al. 2004), the mother of the proband and/or some members of family SNU-G2 might suffer from sporadic, nonheritable gastric cancers. On the other hand, it is possible that the gastric cancer might result from LFS in family SNU-G2. We could not confirm these possibilities because samples were not available from the parents or siblings of the SNU-G2 proband. Among 14 offspring in the third generation (descended from the siblings of the proband), one each was affected by a brain tumor and leiomyosarcoma. These two cancer phenotypes have been related with LFS, and these two members harbored the TP53 E287X germline mutation. As the other six members of the third generation carrying the mutation are younger than 35, they should be closely watched for further development of both LFS-related tumors and gastric cancer.
In summary, we identified a E287X TP53 germline mutation in a large family whose criteria are compatible with both HDGC and LFS. This is the first report of simultaneous concurrence of HDGC and LFS and suggests that researchers should be cautious in screening FGC families for mutations in TP53, as TP53 mutation-carrying FGC families may also develop LFS-related phenotypes.
References
de Anta JM, Jassem E, Rosell R, Martinez-Roca M, Jassem J, Martinez-Lopez E, Monzo M, Sanchez-Hernandez JJ, Moreno I, Sanchez-Cespedes M (1997) TP53 mutational pattern in Spanish and Polish non-small cell lung cancer patients: null mutations are associated with poor prognosis. Oncogene 15:2951–2958
Bakkar AA, Wallerand H, Radvanyi F, Lahaye JB, Pissard S, Lecerf L, Kouyoumdjian JC, Abbou CC, Pairon JC, Jaurand MC, Thiery JP, Chopin DK, de Medina SG (2003) FGFR3 and TP53 gene mutations define two distinct pathways in urothelial cell carcinoma of the bladder. Cancer Res 63:8108–8112
Birch JM, Alston RD, McNally RJ, Evans DG, Kelsey AM, Harris M, Eden OB, Varley JM (2001) Relative frequency and morphology of cancers in carriers of germline TP53 mutations. Oncogene 20:4621–4628
Caldas C, Carneiro F, Lynch HT, Yokota J, Wiesner GL, Powell SM, Lewis FR, Huntsman DG, Pharoah PD, Jankowski JA, MacLeod P, Vogelsang H, Keller G, Park KG, Richards FM, Maher ER, Gayther SA, Oliveira C, Grehan N, Wight D, Seruca R, Roviello F, Ponder BA, Jackson CE (1999) Familial gastric cancer: overview and guidelines for management. J Med Genet 36:873–880
Chompret A (2002) The Li-Fraumeni syndrome. Biochimie 84:75–82
Fenoglio-Preiser CM, Wang J, Stemmermann GN, Noffsinger A (2003) TP53 and gastric carcinoma: a review. Hum Mutat 21:258–270
Guilford P, Hopkins J, Harraway J, McLeod M, McLeod N, Harawira P, Taite H, Scoular R, Miller A, Reeve AE (1998) E-cadherin germline mutations in familial gastric cancer. Nature 392:402–405
Huang CL, Taki T, Adachi M, Konishi T, Higashiyama M, Kinoshita M, Hadama T, Miyake M (1998) Mutations of p53 and K-ras genes as prognostic factors for non-small cell lung cancer. Int J Oncol 12:553–563
Iida S, Akiyama Y, Ichikawa W, Yamashita T, Nomizu T, Nihei Z, Sugihara K, Yuasa Y (1999) Infrequent germ-line mutation of the E-cadherin gene in Japanese familial gastric cancer kindreds. Clin Cancer Res 5:1445–1447
Keller G, Vogelsang H, Becker I, Plaschke S, Ott K, Suriano G, Mateus AR, Seruca R, Biedermann K, Huntsman D, Doring C, Holinski-Feder E, Neutzling A, Siewert JR, Hofler H (2004) Germline mutations of the E-cadherin (CDH1) and TP53 genes rather than of RUNX3 and HPP1 contribute to genetic predisposition in german gastric cancer patients. J Med Genet 41:e89
Kim HC, Wheeler JM, Kim JC, Ilyas M, Beck NE, Kim BS, Park KC, Bodmer WF (2000) The E-cadherin gene (CDH1) variants T340A and L599V in gastric and colorectal cancer patients in Korea. Gut 47:262–267
Kim IJ, Park JH, Kang HC, Shin Y, Lim SB, Ku JL, Yang HK, Lee KU, Park JG (2003) A novel germline mutation in the MET extracellular domain in a Korean patient with the diffuse type of familial gastric cancer. J Med Genet 40:e97
Lee JH, Han SU, Cho H, Jennings B, Gerrard B, Dean M, Schmidt L, Zbar B, Vande Woude GF (2000) A novel germ line juxtamembrane Met mutation in human gastric cancer. Oncogene 19:4947–4953
Li FP, Fraumeni JF Jr, Mulvihill JJ, Blattner WA, Dreyfus MG, Tucker MA, Miller RW (1988) A cancer family syndrome in twenty-four kindreds. Cancer Res 48:5358–5362
Martin AM, Kanetsky PA, Amirimani B, Colligon TA, Athanasiadis G, Shih HA, Gerrero MR, Calzone K, Rebbeck TR, Weber BL (2003) Germline TP53 mutations in breast cancer families with multiple primary cancers: is TP53 a modifier of BRCA1? J Med Genet 5358–5362:e34
Mitsudomi T, Hamajima N, Ogawa M, Takahashi T (2000) Prognostic significance of p53 alterations in patients with non-small cell lung cancer: a meta-analysis. Clin Cancer Res 6:4055–4063
Oliveira C, Bordin MC, Grehan N, Huntsman D, Suriano G, Machado JC, Kiviluoto T, Aaltonen L, Jackson CE, Seruca R, Caldas C (2002) Screening E-cadherin in gastric cancer families reveals germline mutations only in hereditary diffuse gastric cancer kindred. Hum Mutat 19:510–517
Olivier M, Goldgar DE, Sodha N, Ohgaki H, Kleihues P, Hainaut P, Eeles RA (2003) Li-Fraumeni and related syndromes: correlation between tumor type, family structure, and TP53 genotype. Cancer Res 63:6643–6650
Shin HR, Jung KW, Won YJ, Park JG (2002) Annual report of the Korea central cancer registry: based on registered data from 139 hospitals (2004). Cancer Res Treat 36:103–114
Sugano K, Taniguchi T, Saeki M, Tsunematsu Y, Tomaru U, Shimoda T (1999) Germline p53 mutation in a case of Li-Fraumeni syndrome presenting gastric cancer. Jpn J Clin Oncol 29:513–516
Vega FJ, Iniesta P, Caldes T, Sanchez A, Lopez JA, de Juan C, Diaz-Rubio E, Torres A, Balibrea JL, Benito M (1997) p53 exon 5 mutations as a prognostic indicator of shortened survival in non-small-cell lung cancer. Br J Cancer 76:44–51
Yabuta T, Shinmura K, Tani M, Yamaguchi S, Yoshimura K, Katai H, Nakajima T, Mochiki E, Tsujinaka T, Takami M, Hirose K, Yamaguchi A, Takenoshita S, Yokota J (2002) E-cadherin gene variants in gastric cancer families whose probands are diagnosed with diffuse gastric cancer. Int J Cancer 101:434–441
Yoon KA, Ku JL, Yang HK, Kim WH, Park SY, Park JG (1999) Germline mutations of E-cadherin gene in Korean familial gastric cancer patients. J Hum Genet 44:177–180
Acknowledgements
This work was supported by a research grant from the National Cancer Center, Korea, and the BK21 project for Medicine, Dentistry, and Pharmacy.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, IJ., Kang, H.C., Shin, Y. et al. A TP53-truncating germline mutation (E287X) in a family with characteristics of both hereditary diffuse gastric cancer and Li-Fraumeni syndrome. J Hum Genet 49, 591–595 (2004). https://doi.org/10.1007/s10038-004-0193-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10038-004-0193-9
Keywords
This article is cited by
-
Detection of E2A-PBX1 fusion transcripts in human non-small-cell lung cancer
Journal of Experimental & Clinical Cancer Research (2013)
-
Searching for E-cadherin gene mutations in early onset diffuse gastric cancer and hereditary diffuse gastric cancer in Korean patients
Familial Cancer (2013)
-
Familial gastric cancer: update for practice management
Familial Cancer (2011)
-
TP53 germline mutations in Portugal and genetic modifiers of age at cancer onset
Familial Cancer (2009)
-
Hereditary diffuse gastric cancer: association with lobular breast cancer
Familial Cancer (2008)