Abstract
Microsatellite instability (MSI) plays an important biological role in various types of cancers, and especially in colorectal cancers. This study aimed to develop a simple, efficient, new method for robust MSI analysis. DNA was extracted from 175 (105 proximal colon and 70 distal colorectal) cancer samples and matched normal tissues, and five Bethesda microsatellite markers (BAT-25, BAT-26, D5S346, D2S123, and D17S250) were examined for MSI by denaturing high-performance liquid chromatography (DHPLC) analysis at a temperature of 50°C and a flow rate of 0.9 ml/min. It took just 9 min per PCR product to determine MSI or microsatellite stability (MSS) using the new protocol. The DHPLC results were confirmed with conventional gel-based electrophoresis and capillary-based sequencing method. Of 175 samples, 45 (26%) showed high microsatellite instability (MSI-H), 12 (7%) showed low microsatellite instability (MSI-L), and 118 (67%) showed MSS. All MSI samples were deletion mutants and all 12 MSI-L cases had MSI in dinucleotide markers (D5S346, D2S123, and D17S250). MSI was significantly associated with proximal colon cancers (p<0.0001), as previously reported. The MSI-H tumors were also associated with tumor node metastasis (TNM) I/II stages (p=0.05) and high-grade tumors (p<0.01). Here, we propose a DHPLC-based method as an alternative for MSI analysis.
Similar content being viewed by others
Introduction
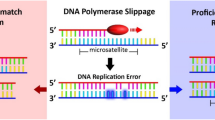
Colorectal cancer is one of major causes of cancer death in the Western population and is becoming more prevalent in Asian countries. MSI is caused by a failure of the mismatch repair (MMR) system to repair errors that occur during DNA replication. In the case of cancers, MSI is characterized by the identification of a microsatellite allele in the DNA of cancer tissue that is not found in matching normal tissue DNA (Aaltonen et al. 1993; Boland et al. 1998; Thibodeau et al. 1993). Association between MSI and hereditary nonpolyposis colorectal cancer (HNPCC) was first reported in 1993, followed by identification of similar concordances in the majority of cancer types, i.e., colorectal, gastric, endometrial, breast, thyroid, lung, and prostate cancers (Boland et al. 1998; Sood et al. 2001). MSI is found in ~90% of HNPCC patients and 10–15% of sporadic colorectal, gastric, and endometrial cancers (Duval and Hamelin 2002). HNPCC is caused by germline mutations in MMR genes, especially hMLH1 and hMSH2 (Loukola et al. 2001; Park et al. 2002; Shin et al. 2002). Thus, as a hallmark of MMR deficiency, MSI is a good marker of hMLH1 and hMSH2 mutation in these cancers (Loukola et al. 2001; Wahlberg et al. 2002).
In general, MSI status has several biological significances, and it is well established that colorectal cancer patients with MSI have a better prognosis (Samowitz et al. 2001). Because MSI-H colorectal cancers have distinct characteristics compared with MSI-L/MSS colorectal cancers, it is clinically important to classify colorectal cancers based on the absence or presence of MSI (Laiho et al. 2002). In addition, significant relationships have been noted between MSI status and proximal tumor location, female gender, age at diagnosis, poor histological differentiation, and low tumor stage (Samowitz et al. 2001; Thibodeau et al. 1993). MSI tumors are generally associated with a low mutation frequency of the p53 and APC genes and a high mutation frequency of β-catenin (Gonzalez-Garcia et al. 2000; Kim et al. 2003). Also, patients with MSI show better survival after chemotherapy. Therefore, it is clinically relevant to determine whether patient prognoses and responses to chemotherapy can be predicted by MSI analysis (Elsaleh et al. 2000).
Five microsatellite markers, known as the Bethesda panel, have been proposed as efficient determinants of the MSI status of colorectal cancers: BAT-25, BAT-26, D5S346, D2S123, and D17S250 (Boland et al. 1998). MSI-H cancers are defined as having MSI in ≥30–40% of the markers examined (or ≥2 of the five Bethesda panel markers), and MSI-L cancers show MSI in ≤30% (or MSI in only one of the five markers) (Boland et al. 1998). However, despite the importance of MSI analysis, techniques have not markedly improved (Sood et al. 2001). Thus, a simple automatic method would facilitate the investigation of MSI in cancer patients.
Denaturing high-performance liquid chromatography (DHPLC) was initially devised to detect mutation or single nucleotide polymorphisms (SNPs) by heteroduplex formation (Xiao and Oefner 2001). The most distinct advantage of DHPLC is that automatic high-throughput analysis is feasible using its computer-controlled systems. Here, we propose a new DHPLC-based method for efficient MSI analysis.
Materials and methods
Samples and DNA extraction
A total of 175—105 proximal colon (cecum to splenic flexure) cancers; 70 distal colorectal (splenic flexure to rectum) cancers—and matched normal tissues were collected from Seoul National University Hospital and the National Cancer Center of Korea. One-hundred-sixty-one samples were sporadic cases and fourteen were HNPCC cases. Informed consents were obtained from all patients prior to their inclusion in this study. DNA was extracted from frozen tumor specimens (containing >50% cancer cells) and matched normal tissues using the Trizol reagent (Invitrogen, Carlsbad, CA, USA) according to the manufacturer's instructions. Tumors were classified as low grade (well- or moderately-differentiated adenocarcinoma) or high grade (poorly differentiated, undifferentiated, or mucinous adenocarcinoma). Tumor stages were also classified according to the tumor node metastasis (TNM) staging system.
Gel-based MSI analysis
PCR primer sequences for amplifying the five microsatellite markers (BAT-25, BAT-26, D2S123, D5S346, and D17S250) were obtained from the Genome Database (www.gdb.org). PCR primer sequences for five MSI markers are shown in Table 1. PCR amplification was performed with 100 ng of genomic DNA, 1× PCR buffer supplemented with 1.5 mM of MgCl2, 10 pmol/µl of each primer, 50 µM each dNTP, 12.5 µM [α-32P]-dCTP, and 0.25 U of Taq polymerase (GeneCraft, Germany) in a total volume of 10 µl. PCR reactions were amplified as follows: 5 min at 94°C, followed by 35 cycles of 30 s at 94°C; 30 s at 55°C (BAT-25, D2S123, and D5S346), 50°C (BAT-26) or 52°C (D17S250); 1 min at 70°C, followed by a final elongation of 7 min at 70°C. PCR products were then denatured for 5 min at 94°C and then electrophoresed on 6 M urea+6% polyacrylamide gels at 1,800 volts for 2 h. The gels were transferred onto 3 MM Whatman paper, and dried and autoradiographed.
Capillary-based MSI analysis
Two markers, BAT-25 and BAT-26, were evaluated by a capillary-based sequencing analysis. PCR was performed as described above, except that forward primers were labeled with fluorescent dye (FAM), and the labeled samples were run on an ABI 3100 sequencer (Applied Biosystems Inc., Foster City, CA, USA). Genescan software (Genotyper 2.1, ABI, Foster City, CA, USA) was used to calculate the size of each fluorescent PCR products (Loukola et al. 2001).
MSI analysis using DHPLC
PCR primers and conditions were the same as above. PCR amplification for DHPLC analysis was performed with 100 ng of genomic DNA, 1× PCR buffer supplemented with 1.5 mM of MgCl2, 10 pmol/µl of each primer, 50 µM each dNTP, and 0.25 U of Taq polymerase in a total volume of 25 µl. For heteroduplex formation, crude PCR products were denatured at 95°C for 5 min followed by gradual cooling to 25°C over a period of 1 h. DHPLC was performed using a fully automated system (WAVE, Transgenomic Inc., Omaha, NE, USA). The cooled samples (5 µl) were automatically injected into a DNASepcartridge (Transgenomic Inc., Omaha, NE, USA) and eluted at a flow rate of 0.9 ml/min through a linear gradient of acetonitrile containing 0.1 M triethylammonium acetate (TEAA). Buffer A (0.1 M TEAA solution) and buffer B (0.1 M TEAA containing 25% acetonitrile solution) were automatically adjusted to produce optimal running conditions (Table 2), and the system oven was set to 50°C, which is recommended for double-strand DNA analysis in WAVEMAKER software (Transgenomic Inc., Omaha, NE, USA) (Kang et al. 2002). UV detection was performed at 260 nm.
Statistics
Statistical analyses were performed using the ϰ2 or Fisher's exact tests to determine the strength of the correlations between MSI status, gender, tumor location, tumor grade, and tumor stage. The Student's t test was used to assess the statistical significance of relationships between MSI status and age; α=0.05 was set as the significance level using the STATISTICA software (StatSoft Inc., Tulsa, OK, USA).
Results
MSI frequency
The 175 cancer and matched normal samples were analyzed by the new DHPLC-based protocol, capillary-based sequencing method (for BAT-25 and BAT-26), and by traditional gel-based radioactive electrophoresis (Fig. 1 and 2). The results were 100% concordant for these three methods. The BAT-25 marker showed MSI in 24% (42/175) and the BAT-26 showed MSI in 25% (43/175). In terms of the polymorphic patterns of BAT-25 and BAT-26, none of the DNAs from 175 matched normal samples showed polymorphic BAT-25 and BAT-26 patterns. In the dinucleotide markers, MSI was found at D2S123 (19%, 34/175), D5S346 (15%, 26/175), and D17S250 (18%, 32/175) (Fig. 3). Out of 175 samples, 45 (26%) were MSI-H, 12 (7%) were MSI-L, and 118 (67%) were MSS. Fifty-seven (33%) samples showed MSI in one or more markers. Thirteen (12%) out of 105 proximal samples and none of 71 distal colorectal cancers showed MSI in all five markers. Forty-two of 45 (93%) MSI-H tumors showed MSI at BAT-25, and 43 (96%) showed MSI in BAT-26. All samples showing MSI were caused by deletion mutations in the five markers.
Microsatellite instability (MSI) analysis using BAT-25. The MSI results of four different tumor samples are shown: a BAT-25 MSI results from denaturing high-performance liquid chromatography (DHPLC) analysis. Chromatograms of four different tumor DNAs are shown. The arrows indicate the left-shifted MSI pattern. The arrowed samples show heterozygous alterations. The other two samples show microsatellite stability (MSS). b Radioactive gel-based MSI analysis of the same samples in (a) above. The marked samples show MSI in BAT-25. c Capillary-based MSI analysis. The marked samples show MSI in BAT-25
Microsatellite instability (MSI) analysis using BAT-26. a Denaturing high-performance liquid chromatography (DHPLC) results of BAT-26 MSI. The arrowed tumor samples show homozygous alterations (MSI) in BAT-26. The other two tumors were microsatellite stability (MSS). b Radioactive gel-based MSI analysis of the samples in (a) above. The marked samples showed MSI in BAT-26. c Capillary-based MSI analysis. The marked samples show MSI in BAT-26
Microsatellite instability (MSI) analysis of the dinucleotide markers D2S123, D5S346, and D17S250. Denaturing high-performance liquid chromatography (DHPLC) chromatograms of the matched normal and cancer tissues are shown. Each figure, (a–d), contains two different sample sets in the order—'normal-cancer, normal-cancer', from top to bottom. The arrow indicates the MSI. a MSI analysis of D2S123 by DHPLC; b MSI analysis of D5S346 by DHPLC; c MSI analysis of D17S250 by DHPLC; d Radioactive gel-based electrophoresis of D2S123
Clinical characterization based on MSI status
MSI-H tumors have been reported to be associated with high-grade tumors (Park et al. 2003). This was confirmed in our data, which drew a significant association between MSI-H and high-grade (p<0.01), TNM I/II stage (p=0.05) tumors. MSI was significantly associated with proximal colon cancers (p<0.0001), as previously well defined (Loukola et al. 2001) (Table 3). No significant correlations between gender, age, and MSI status were found.
MSI analysis by DHPLC
DHPLC-based MSI analysis took an average of 9 min per amplified DNA sample by DHPLC. As no matched normal tissue DNA was required for analysis of the monomorphic markers (BAT-25 and BAT-26), MSI status of these markers could be determined in 9 min. In the cases of the polymorphic markers (D2S123, D5S346, and D17S250), DNA samples were required from cancer tissues and matched normal tissues, meaning that determination of MSI took an average of 18 min. The MSI results were displayed by the WAVEMAKER software (Transgenomic, Omaha, NE, USA) in real time. No additional adducts (i.e., radioisotopes or fluorescent-labeled PCR primers) or extra software were required.
Discussion
Traditionally, radioactive gel-based electrophoresis and fluorescent-labeled sequencing analysis have been used for MSI analysis. Gel-based radioactive electrophoresis is the most popular method because it does not require a complicated protocol or expensive equipment. However, this method is time consuming and labor intensive, the use of radioisotopes limits one-off experimentation, and the protocol involves several experimental steps (i.e., gel fabrication, PCR with radioisotope, sample loading, gel drying, and autoradiography), which are not compatible with high-throughput analysis. Moreover, it is sometimes difficult to interpret the results of quasimonomorphic markers, such as BAT-25 and BAT-26, as their band sizes are similar in MSS samples and boundaries between samples may become blurred. Some of these drawbacks are overcome with fluorescent detection using a capillary-based automatic sequencer. However, fluorescent technology requires the use of expensive, photolabile fluorescent PCR primers and additional software, i.e., GeneScan 3.1 and Genotyper 2.5 (Applied Biosystems, Foster City, CA, USA) (Laiho et al. 2002).
Over the years, DHPLC has been widely used for genetic analysis. Here we have used it to develop a new method for MSI analysis. DHPLC uses the heteroduplex principle of altered DNA, namely temperature-modulated heteroduplex analysis (TMHA) (Xiao and Oefner 2001), to separate PCR products that differ by as little as a few base pairs. PCR products differing by a single base pair are distinguishable at 50°C by ion-pair, reversed-phase, liquid chromatography (Xiao and Oefner 2001). The main advantage of DHPLC is its ability to perform automatic high-throughput analysis under computer control (Xiao and Oefner 2001). In general, the use of DHPLC for detection of a mutation or novel SNP requires an additional sequencing step to analyze the abnormal chromatograms. However, MSI determination depends only on the presence of a novel allele in cancer DNA that is not present in the corresponding normal tissue, which means that DHPLC analysis of MSI is a simple, efficient process.
BAT-25 and BAT-26 are known to be quasimonomorphic, and the other three markers are polymorphic. BAT-25 and BAT-26 polymorphisms have been reported in 18.4% and 12.6% respectively of African Americans and in 0.8% of Caucasians (Suraweera et al. 2002). This possible germline alteration in the MSI marker requires corresponding normal tissue for MSI analysis, which increases costs and labor requirements two fold. However, in 175 normal tissue samples from our Korean patients, no polymorphisms were detected in BAT-25 or -26, suggesting that the markers are monomorphic in the Korean population. This enabled us to perform high-throughput MSI analysis without corresponding normal tissues. By DHPLC, a single left-shifted peak corresponded to a homozygous deletion while two peaks (one for normal size and another for the MSI) corresponded to a heterozygous deletion. In addition, we screened three dinucleotide markers, D5S346, D2S123, and D17S250, all of which showed the expected highly polymorphic patterns. Interestingly, all 12 MSI-L samples had an MSI in one of the dinucleotide markers (D5S346, D2S123, and D17S250).
In this work, we established a new protocol for robust MSI analysis using five representative MSI markers from the Bethesda panel for colorectal cancers. The use of standard experimental conditions allows robust MSI analysis and ensures that consistent results may be obtained in a variety of research applications.
References
Aaltonen LA, Peltomaki P, Leach FS, Sistonen P, Pylkkanen L, Mecklin JP, Jarvinen H, Powell SM, Jen J, Hamilton SR (1993) Clues to the pathogenesis of familial colorectal cancer. Science 260:812–816
Boland CR, Thibodeau SN, Hamilton SR, Sidransky D, Eshleman JR, Burt RW, Meltzer SJ, Rodriguez-Bigas MA, Fodde R, Ranzani GN, Srivastava SR (1998) A National Cancer Institute Workshop on microsatellite instability for cancer detection and familial predisposition: development of international criteria for the determination of microsatellite instability in colorectal cancer. Cancer Res 58:5248–5257
Duval A, Hamelin R (2002) Mutations at coding repeat sequences in mismatch repair-deficient human cancers: toward a new concept of target genes for instability. Cancer Res 62:2447–2454
Elsaleh H, Joseph D, Grieu F, Zeps N, Spry N, Iacopetta B (2000) Association of tumour site and sex with survival benefit from adjuvant chemotherapy in colorectal cancer. Lancet 355:1745–1750
Gonzalez-Garcia I, Moreno V, Navarro M, Marti-Rague J, Marcuello E, Benasco C, Campos O, Capella G, Peinado MA (2000) Standardized approach for microsatellite instability detection in colorectal carcinomas. J Natl Cancer Inst 92:544–549
Kang HC, Kim IJ, Park JH, Kwon HJ, Won YJ, Heo SC, Lee SY, Kim KH, Shin Y, Noh DY, Yang DH, Choe KJ, Lee BH, King SB, Park JG (2002) Germline mutations of BRCA1 and BRCA2 in Korean breast and/or ovarian cancer families. Hum Mutat 20:235
Kim IJ, Kang HC, Park JH, Shin Y, Ku JL, Lim SB, Park SY, Jung SY, Kim HK, Park JG (2003) Development and applications of a β-catenin oligonucleotide microarray: β-catenin mutations are dominantly found in the proximal colon cancers with microsatellite instability. Clin Cancer Res 9:2920–2925
Laiho P, Launonen V, Lahermo P, Esteller M, Guo M, Herman JG, Mecklin JP, Jarvinen H, Sistonen P, Kim KM, Shibata D, Houlston RS, Aaltonen LA (2002) Low-level microsatellite instability in most colorectal carcinomas. Cancer Res 62:1166–1170
Loukola A, Eklin K, Laiho P, Salovaara R, Kristo P, Jarvinen H, Mecklin JP, Launonen V, Aaltonen LA (2001) Microsatellite marker analysis in screening for hereditary nonpolyposis colorectal cancer (HNPCC). Cancer Res 61:4545–4549
Park JG, Vasen HF, Park YJ, Park KJ, Peltomaki P, de Leon MP, Rodriguez-Bigas MA, Lubinski J, Beck NE, Bisgaard ML, Miyaki M, Wijnen JT, Baba S, Lindblom A, Madlensky L, Lynch HT (2002) Suspected HNPCC and Amsterdam criteria II: evaluation of mutation detection rate, an international collaborative study. Int J Colorectal Dis 17:109–1014
Park J, Betel D, Gryfe R, Michalickova K, Di Nicola N, Gallinger S, Hogue CW, Redston M (2003) Mutation profiling of mismatch repair-deficient colorectal cancers using an in silico genome scan to identify coding microsatellites. Cancer Res 62:1284–1288
Samowitz WS, Curtin K, Ma KN, Schaffer D, Coleman LW, Leppert M, Slattery ML (2001) Microsatellite instability in sporadic colon cancer is associated with an improved prognosis at the population level. Cancer Epidemiol Biomarkers Prev 10:917–923
Shin KH, Shin JH, Kim JH, Park JG (2002) Mutational analysis of promoters of mismatch repair genes hMSH2 and hMLH1 in hereditary nonpolyposis colorectal cancer and early onset colorectal cancer patients: identification of three novel germ-line mutations in promoter of the hMSH2 gene. Cancer Res 62:38-42
Sood AK, Holmes R, Hendrix MJ, Buller RE (2001) Application of the National Cancer Institute international criteria for determination of microsatellite instability in ovarian cancer. Cancer Res 61:4371–4374
Suraweera N, Duval A, Reperant M, Vaury C, Furlan D, Leroy K, Seruca R, Iacopetta B, Hamelin R (2002) Evaluation of tumor microsatellite instability using five quasimonomorphic mononucleotide repeats and pentaplex PCR. Gastroenterology 23:1804–1811
Thibodeau SN, Bren G, Schaid D (1993) Microsatellite instability in cancer of the proximal colon. Science 260:816–819
Wahlberg SS, Schmeits J, Thomas G, Loda M, Garber J, Syngal S, Kolodner RD, Fox E. (2002) Evaluation of microsatellite instability and immunohistochemistry for the prediction of germ-line MSH2 and MLH1 mutations in hereditary nonpolyposis colon cancer families. Cancer Res 62:3485–3492
Xiao W, Oefner PJ (2001) Denaturing high-performance liquid chromatography: A review. Hum Mutat 17:439–474
Acknowledgements
This work was supported by a research grant from the National Cancer Center, Korea, and the BK21 Project for Medicine, Dentistry, and Pharmacy.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was presented in part at the meeting of AACR Oncogenomics 2003, Phoenix, AZ, USA, January 2003.
Rights and permissions
About this article
Cite this article
Kim, IJ., Shin, Y., Kang, H.C. et al. Robust microsatellite instability (MSI) analysis by denaturing high-performance liquid chromatography (DHPLC). J Hum Genet 48, 525–530 (2003). https://doi.org/10.1007/s10038-003-0070-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10038-003-0070-y
Keywords
This article is cited by
-
Microsatellite instability typing in serum and tissue of patients with colorectal cancer: comparing real time PCR with hybridization probe and high-performance liquid chromatography
Molecular Biology Reports (2014)
-
GSTT2 promoter polymorphisms and colorectal cancer risk
BMC Cancer (2007)
-
Mutational analysis of OGG1, MYH, MTH1 in FAP, HNPCC and sporadic colorectal cancer patients: R154H OGG1 polymorphism is associated with sporadic colorectal cancer patients
Human Genetics (2004)