Abstract
A finite element model of the temporomandibular joint (TMJ) and the human mandible was fabricated to study the effect of abnormal loading, such as awake and asleep bruxism, on the articular disc. A quasilinear viscoelastic model was used to simulate the behaviour of the disc. The viscoelastic nature of this tissue is shown to be an important factor when sustained (awake bruxism) or cyclic loading (sleep bruxism) is simulated. From the comparison of the two types of bruxism, it was seen that sustained clenching is the most detrimental activity for the TMJ disc, producing an overload that could lead to severe damage of this tissue.
Similar content being viewed by others
Introduction
The term bruxism is defined as a repetitive jaw muscle activity characterized by clenching or grinding of the teeth and/or by bracing or thrusting of the mandible.1 A rhythmic or sustained contraction of the jaw closing muscles produces tooth movement without patient awareness. It is believed that there are two types of bruxism with different etiopathogenesis: asleep and awake bruxism.2,3,4 The first is a repetitive sleep movement disorder primarily characterized by rhythmic masticatory muscle activity and by occasional tooth grinding and is associated with brief cardiac and brain reactivation.5 Instead, awake bruxism is characterized by only clenching-type activity and is associated with psychosocial factors.6 Bruxism is a very common condition and it is estimated that 85%–90% of the population will, at some time, grind or clench the teeth to some degree.2 Bruxism may also entail temporomandibular disorders (TMDs) or chronic myofascial pain in the masticatory muscles.7,8,9
Even though bruxism as a whole is commonly considered the most harmful parafunctional activity of the temporomandibular joint (TMJ), there are many unsolved issues concerning the actual causal relationship between bruxism and TMD.6,10 The main uncertainties are due to lack of knowledge on the aetiology and diagnosis of bruxism and TMD.6 While many studies support that there is a cause and effect relationship,2,11,12,13 the non-unique characterisation of each makes that relation controversial. At present, there exists a validated diagnostic criterion to define sleep bruxism, but as pointed out in,14 it requires the muscle activity to be recorded in a controlled laboratory. For awake bruxism, there is not even any definite criterion.14 For these reasons, the ability to gather sound data on bruxism is quite limited.
Damage to the articular disc can be a cause of TMD. Some researchers have shown that acute mechanical overloads in vivo can cause severe cartilage damage.15,16 Apart from the deterioration that the stresses can cause in the material, additional damage could be induced because it is a living material and its capacity to repair itself can be put in jeopardy. Particularly, the application of shear stress was seen to induce molecular changes associated with apoptosis.17 Articular cartilage consists of scattered chondrocytes surrounded by an extracellular matrix composed of a highly organized macromolecular framework filled with water. Chondrocytes create the molecular framework from three classes of molecules: collagens, proteoglycans and noncollagenous proteins.18 In experimental works, it was demonstrated that shear stresses increased the release of nitric oxide that acts as reactive oxygen metabolite implicated in joint pathogenesis.17 The increase in nitric oxide was associated with an increase in chondrocyte apoptosis. Although the precise mechanism by which mechanical stress alters chondrocyte metabolism remains to be established, this alteration might facilitate the damage caused by shear stresses in the cartilage.
Such shear stresses are the main focus of this study, which tries to shed light on the possible relationship between bruxism and TMD caused by mechanical overloading. These abnormal loads will be evaluated with a finite element (FE) model. The experimental measurement of in vivo joint loads is difficult to perform, and no such studies have been reported. Then, FE analysis constitutes an adequate framework to explore the interaction between the disc and masticatory dynamics. To simulate bruxism in the FE model, muscle forces are needed. However, from a literature review, it is difficult to precisely define the activation of masticatory muscles during bruxism. Experimentally, some authors have identified a bruxism episode when the muscle activation is beyond 10% of the maximum voluntary contraction (MVC),19 while other authors have set the activation threshold to 20% of the MVC.13,20,21 Because there is no standard criterion to define a bruxism episode, different muscle activation levels were studied to analyse the effect on the joint.
Awake bruxism, characterized by clenching-type activity, has been studied by other authors to investigate the stress distribution in the joint.22,23,24,25,26 However, some of those authors applied muscle forces,22,24,26 while others forced a displacement on the condyle23,25 to simulate clenching. Moreover, only a few works considered the viscoelastic nature of the articular disc to analyse the effect of sustained clenching.22,23,24 Furthermore, the loading phase, during which the muscles are being activated, was not considered in any of those studies. Instead, those authors assumed that the onset of clenching occurred instantaneously. This simplification is analysed here by studying the influence of the activation rate of the masticatory muscles.
As discussed previously, an excessive loading of the hard and soft tissues of the joint is suggested to be the cause of joint disorders. Thus, prolonged clenching can cause degenerative changes due to the overloading induced with time. To observe this effect, the viscoelasticity of the disc must be considered. Sustained muscle forces produce a relevant increase in the shear stresses developed in the disc due to the creep deformation produced by the compression of the disc. In this regard, forcing a displacement of the condyle is not equivalent to applying sustained muscle forces.
A comparison of the effect of awake and asleep bruxism in the TMJ does not exist in the literature. In this sense, a rigorous comparison between the two types of bruxism is made in the current study to establish if their repercussions on the joint are different. Thus, the aim of this study is to further investigate the two types of bruxism, particularly the stress state they can induce in the joint, which can eventually produce damage in articular disc and TMD. Different features of bruxism are studied, such as the muscle activation level, the muscle activation rate and the type of muscle contraction (rhythmic or sustained), in order to analyse their effect in the stresses in the articular disc. Another objective is to determine which type of activity is more dangerous in terms of the stresses it produces in the disc.
Materials and methods
FE model
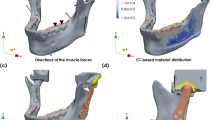
A FE model of the mandible and temporomandibular joint was created using the commercial software Abaqus FEA v6.10. The mandible model was adapted from a previous work27 in which the TMJ, not included in that study, has been incorporated. The FE model was created from the mandible of a human cadaver. The teeth geometry was approximated and a layer of elements with a thickness of 0.2 mm surrounding the teeth was used to simulate the periodontal ligament, similarly to Ref. 28. The mandible, teeth and periodontal ligament were meshed with linear eight-noded hexahedral elements (type C3D8 of the elements library of Abaqus FEA). The geometry of the articular disc and ligaments of the joint was approximated in a manner similar to that used by Pérez del Palomar and Doblaré.25 The TMJ components were meshed with linear eight-noded, hybrid hexahedral elements (type C3D8H). The complete model, shown in Figure 1, has a total of 77 490 type C3D8 elements, 3 978 type C3D8H elements and 93 584 nodes.
The TMJ was modelled by including the articular disc, the collateral and temporomandibular ligaments, the temporal bone (as a rigid surface) and the posterior part of the articular capsule. The human TMJ disc has a biconcave profile in the anteroposterior axis. The thinner central region, designated as an intermediate zone, has a thickness ranging from 1 to 1.2 mm, while the maximum thicknesses of the anterior and posterior bands were approximately 2.4 and 2.9 mm, respectively. In Figure 1, the TMJ components are shown in more detail.
Boundary and loading conditions
The forces exerted by the masticatory muscles were imposed as external loads, distributed over the insertion area of each muscle, as performed in a previous work.27 The orientation of these forces were taken from a similar model made by Korioth et al.,28 and the magnitude was adapted from the same source used by these authors.29
To simulate different activities, the muscles’ forces were estimated using the data from Ref. 29 and varying the level of activation (percentage of the maximum voluntary contraction or MVC).
Sustained clenching and rhythmic masticatory muscle activity (RMMA) were simulated by applying the muscle activation pattern described in Figure 2a and 2b, respectively. RMMA was simulated as a cyclic loading using the characterisation provided by Lavigne et al.,21 with the electromyogram burst lasting 0.65 s.
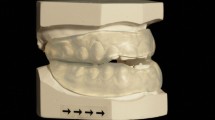
A simultaneous activation of the jaw closing muscles (medial and lateral pterygoid, masseter and temporalis) from 0 to M was assumed in both activities, where M is the maximum muscle activation level (given as a percentage of MVC), 20% in Figure 2.23,24 The effect of sustained clenching in the TMJ was studied by maintaining the muscle activation for 5 min, as performed in other works.23,24 Additionally, the displacement of the nodes on the occlusal surface of the right and left molars was constrained in the craniocaudal direction to simulate the clenching against a cast placed between the upper and lower molars.27 The temporal bone and the insertion areas of the ligaments in the cranium were considered to be fixed.
As mentioned previously, the muscle activation level defined to diagnose bruxism is not precisely estimated.6 It seems to be a controversial point because different activation thresholds have been established to define a bruxism episode.6,13,19,20,21 Therefore, two different levels, M: 10% and 20% of the MVC, were analysed.
Because there are no available data describing the rate of activation of the jaw closing muscles, three different loading rates were simulated for the sustained clenching task. In other words, the same activation level (20%) was reached at three different times, termed ta: 0.001, 0.01 and 0.1 s. In the RMMA, it was assumed that the activation was reached in ta=0.01 s. In the numerical studies of clenching found in the literature,22,23,24 it was assumed that the onset of clenching occurs instantaneously, so the loading phase, during which the muscle activation was neglected; this may be too profound of a simplification in a model with a viscoelastic material such as the articular disc.
Material properties
The mechanical properties of the bone of the mandible depend on the bone density and anisotropy and were estimated in Reina et al.27
The mechanical behaviour of the articular disc is modelled with a quasilinear viscoelastic formulation, proposed by Fung30 and previously used to describe a large number of soft tissues.31,32 In the quasilinear viscoelastic formulation, the history of the stress response to a step stretch, called the relaxation function, σ(λ,t), is factorized using a normalized function of time, called the reduced relaxation function,  (Equation (2)), and a function of the stretch, λ, called the elastic response, T(e)(λ), thus giving:
(Equation (2)), and a function of the stretch, λ, called the elastic response, T(e)(λ), thus giving:

where

is normalized such that g∞+g1+g2+g3+g4=1. The elastic response, T(e)(λ), is derived from the following strain energy function, ψ:

used in previous works to describe the behaviour of soft tissues,33 leading to the following elastic response (see Ref. 34 for further details):

Finally, the stress response to a general stretch history, λ(t), is given by:

These equations have been implemented in a user material subroutine of Abaqus FEA. The material constants were obtained in stress relaxation tests performed in articular discs of pigs (Commisso MS, PhD thesis, 2012, unpubl. data) using the algorithm described in Ref. 34. In this model, the following constants were used to define the viscoelastic function: g1=0.28, g2=0.37, g3=0.27, g4=0.08, τ1=0.01 s, τ2=0.1 s, τ3=1 s and τ3=10 s, and A=0.16 MPa, B=4.18 and D1=0.01 MPa−1 for the elastic function. The material constants (particularly the viscoelastic constant) are similar to those obtained in Koolstra et al.35 A friction coefficient of μ=0.015 was assumed in the contact between the disc and the bony parts.36
A transversely isotropic hyperelastic model was used to describe the behaviour of the ligaments.37 So, the strain energy function is described as:

The three terms represent the contribution of the matrix (F1), the collagen fibres (F2) and the tissue volumetric response. The matrix is assumed in that model to behave as neo-Hookean materials, therefore:

with  representing the deviatoric first invariant of the right Cauchy–Green tensor. The derivatives of the fibre strain energy function were defined as a function of the isochoric fibre stretch,37
representing the deviatoric first invariant of the right Cauchy–Green tensor. The derivatives of the fibre strain energy function were defined as a function of the isochoric fibre stretch,37  , which depends on the fibre direction, a0,
, which depends on the fibre direction, a0,

Due to the lack of experimental data describing the mechanical behaviour of the TMJ ligaments, the properties obtained by Gardiner and Weiss37 for the medial collateral ligament of the knee were used for the articular capsule and ligaments of the TMJ. The constants are: C10=1.44 MPa, D2=0.01 MPa−1, C3=2.4 MPa, C4=30.6 MPa, C5=323.7 MPa, C6=−331.0 MPa and λ*=1.055. The fibre directions, a0, were defined for each element following the main direction of each ligament and can be seen in Figure 1.
Results
Because the muscle forces applied and the model are symmetric, only the results of the right half of the mandible are analysed.
Sustained clenching
Figure 3 shows the distribution of the maximum and minimum principal stresses and the maximum shear stresses in this case. At the onset of clenching (Figure 3a), the maximum compressive stresses, σmin, are located at the anterior and intermediate zone of the disc and more precisely in the medial part within the intermediate zone. The maximum tensile stress, σmax, appears at the anterior and posterior bands of the superior surface and at the intermediate zone of the inferior surface due to the contact pressure applied by the condyle. The minimum principal stress found on the inferior surface is −4.8 MPa and the maximum principal stress is 3.6 MPa, while on the superior surface, where the contact interaction is softer,25,26 the minimum principal stress is −1.4 MPa and the maximum principal stress is 0.3 MPa. The maximum shear stresses, τmax, are distributed similarly to the maximum compressive stresses, being the highest stresses concentrated at the anterior and intermediate region of the inferior surface.
After 5 min of sustained clenching, the maximum tensile, compressive and shear stresses are concentrated at the intermediate zone (Figure 3b) and a slight shift of the disc in anterior direction was observed. In the lateral and medial parts of the intermediate zone, the stresses relax to 20%–30% of the stress value at the onset.
The maximum shear stress was estimated for representative nodes at different locations of the disc, plotted in Figure 4. At the onset of clenching, it was observed that the maximum shear stress is located at the anterior region, followed by the intermediate region. However, after prolonged clenching, the shear stress at the intermediate region increases noticeably (Figure 4). The shear stresses at the anterior region are relaxed after the onset of clenching, but a slight increase is also observed after 100 s. The shear stresses at the posterior, lateral and medial regions are very low during sustained clenching.
Clenching at different levels
As previously mentioned, different muscle activation levels were attempted for sustained clenching. In Figure 5, the shear stresses in the points plotted in Figure 4 can be seen for different activation levels. The maximum shear stress obtained is not directly related to the muscle activation level due to the nonlinearity of the viscoelastic model.
Clenching at different rates
In Figure 6, the evolution of the maximum and minimum principal stresses in the intermediate zone of the disc can be seen for the two extreme values of the activation rate. The influence of the loading rate is negligible after sustained clenching.
RMMA
In Figure 7, the evolution of the maximum shear stress obtained in different regions of the disc is shown for a RMMA with an activation level of 20%.
Maximum shear stresses in the anteroposterior axis of the disc for a rhythmic mastication muscle activation of 20% of the MVC. Only the EMG burst, lasting 0.65 s is shown. When the muscular activity ceases, the shear stresses tend to zero (not shown). EMG, electromyogram; MVC, maximum voluntary contraction.
Rhythmic muscle activation was simulated, reaching two different activation levels: 10% and 20% of the MVC. To compare the stress state in the disc in both cases, only the peaks of the maximum shear stress are plotted together in Figure 8 (in contrast to Figure 7, where the complete cycles were represented).
Discussion
During awake bruxism (sustained clenching), the intermediate zone is mainly subjected to compressive stresses at the onset of clenching. The distribution of shear stresses is similar to that of the principal stresses, being higher in the anterior and intermediate zones, mainly due to the high compressive stresses observed in those zones. Additionally, the inferior surface suffers the highest shear stresses because the tensile and compressive stresses are higher in that surface.
After 5 min of sustained clenching, the tensile, compressive and shear stresses in the TMJ disc are higher than those at the beginning. This result is in accordance with the measurements made by Kuboki et al.,38 where clenching induced a significant reduction of the joint space and the sustained condition remarkably increased that change. This increase is particularly high on the superior surface, where the maximum shear stresses rose from 0.6 MPa at the onset, to 5.15 MPa at 300 s. On the contrary, the extension of the area subjected to high shear stresses decreases with time. Some authors have reported that the degeneration of soft tissues occurs due to high shear stresses,39 and in the case of the articular disc, perforations may be related to that type of load.40,41
The evolution of the shear stresses in different regions of the disc (Figures 4 and 5) shows that the anterior region is the most affected zone at the onset of clenching; however, the stresses in this region relax with time, with the intermediate zone becoming the most loaded area.
Sustained clenching at two different activation levels was considered. It was observed that the relationship between the applied muscle activation and the shear stress obtained in the articular disc is not proportional. For example, in the anterior region, the maximum shear stress obtained is approximately 0.45 MPa when the activation level reached is 10% of MVC and 0.75 MPa for 20%. After 5 min of sustained clenching, the differences between the two cases are even greater, with the increase in the shear stresses being greater when the muscle activation level was 20%. At this level, the shear stress in the intermediate zone is 4.2 MPa, while at the same location, the shear stress for sustained clenching at 10% of MVC is approximately 1 MPa. This is due to the nonlinearity of the viscoelastic model. An important conclusion from the simulation of awake bruxism is that there are almost no differences in clenching at 0.001 or 0.1 s, except for the loading phase. For example, the minimum principal stresses observed after sustained clenching presented differences lower than 0.05 MPa.
In RMMA, like in sustained clenching, the anterior region is subjected to the highest maximum shear stresses at the beginning of the movement, and as more cycles of RMMA are applied, the stresses in this region relax and the intermediate region becomes the region subjected to the highest shear stresses. The posterior region is barely subjected to stresses. Nevertheless, as it occurs at the anterior region, the stresses in the posterior region relax even further as more cycles of RMMA are applied.
If the RMMA at two different activation levels are compared, the maximum shear stresses are not proportional to the activation level, as occurred in sustained clenching. The shear stresses in the first peak are the same obtained at the onset of clenching, with the shear stresses at 20% of activation being 67% higher than that obtained at 10% of activation. After 30 cycles of RMMA (reached at t≈0.6 s), the shear stresses obtained in the intermediate zone are approximately 0.28 MPa for 10% and 0.52 MPa for 20% of activation; thus, the difference between the two cases increases with the number of cycles.
By comparing the two simulated tasks, sustained clenching and RMMA, the first one is clearly the most detrimental situation to the TMJ, at least in the case analysed here. While in RMMA, the maximum shear stress is approximately 0.8 MPa, in sustained clenching, that stress is exceeded five times over.
A comment on the clinical relevance of this work should be made at this point. Joint pain and occasional headaches produced by bruxism can be explained by overloading the temporomandibular joint,5 and more precisely by shear stresses in the articular disc, which constitute the source of the damage induced to chondrocytes.17 The results presented here are in agreement with these medical observations. Bruxism, especially sustained clenching, produces a noticeable increase in the shear stress in the disc. Detamore and Athanasiou42 estimated an ultimate tensile strength of 2.02–2.62 MPa for the articular disc. The maximum tensile stresses estimated here for a clenching task sustained for 5 min can double that limit. Although a duration of 5 min was also assumed in other works,23,24 it may seem to be too long for a real sustained clenching. Nonetheless, the ultimate tensile strength was exceeded only after 50 s of sustained clenching at 20% of MVC. This fact can produce irreversible damage to the disc, which may lead to temporomandibular disorders.
Regarding the limitations of this study, although biomechanical models may provide an adequate framework to explore the functioning of the TMJ without several of the drawbacks that accompany experimental studies, the validity of this type of study should be analysed with care. FE studies are conditioned by the intrinsic nature of the numerical method and by the hypothesis made in the model, like the mechanical behaviour of the tissues, simplified geometry and modelling of the loads applied by the muscles. All this is somehow limiting the generalisation of the present results to immediate clinical conclusions, although they can still be valid from a qualitative point of view.
Conclusions
This work presents a numerical tool to study temporomandibular disorders. In this study, we focused on bruxism, but this tool could be applied to different pathologies.
It was observed that the stress level observed in the disc is not proportional to the muscle activation level due to the nonlinear behaviour of the articular disc. Additionally, different activation rates seem to produce no significant changes in the stress level.
The shear stresses estimated in this work for any type of bruxism, but especially those obtained in sustained clenching, can induce damage in the articular disc, which, in turn, can lead to TMDs.
As a numerical model, many assumptions and hypotheses were needed, but in light of the results, the most influential is a good characterisation of the articular disc. In this regard, it seems very important to consider the nonlinear viscoelastic behaviour of the articular disc.
References
Lobbezoo F, Ahlberg J, Glaros AG et al. Bruxism defined and graded: an international consensus. J Oral Rehabil 2013; 40( 1): 2–4.
Bader G, Lavigne GJ . Sleep bruxism: an overview of an oromandibular sleep movement disorder. Sleep Med Rev 2000; 4( 1): 27–43.
Manfredini D, Lobbezoo F . Role of psychosocial factors in the etiology of bruxism. J Orofac Pain 2009; 23( 2): 153–166.
Lavigne GJ, Kato T, Kolta A et al. Neurobiological mechanisms involved in sleep bruxism. Crit Rev Oral Biol Med 2003; 14( 1): 30–46.
Lavigne GJ, Huynh N, Kato T et al. Genesis of sleep bruxism: motor and autonomic-cardiac interactions. Arch Oral Biol 2007; 52( 4): 381–384.
Manfredini D, Lobbezoo F . Relationship between bruxism and temporomandibular disorders: a systematic review of literature from 1998 to 2008. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; 109( 6): e26–e50.
Kato T, Lavigne GJ . Sleep bruxism: a sleep-related movement disorder. Sleep Med Clin 2010; 5( 1): 9–35.
Lavigne GJ, Khoury S, Abe S et al. Bruxism physiology and pathology: an overview for clinicians. J Oral Rehabil 2008; 35( 7): 476–494.
Huang GJ, LeResche L, Critchlow CW et al. Risk factors for diagnostic subgroups of painful temporomandibular disorders (TMD). J Dent Res 2002; 81( 4): 284–288.
Lobbezoo F, Lavigne GJ . Do bruxism and temporomandibular disorders have a cause- and-effect relationship? J Orofac Pain 1997; 11( 1): 15–23.
Israel HA, Diamond B, Saed-Nejad F et al. The relationship between parafunctional masticatory activity and arthroscopically diagnosed temporomandibular joint pathology. J Oral Maxillofac Surg 1999; 57( 9): 1034–1039.
Baba K, Haketa T, Sasaki Y et al. Association between masseter muscle activity levels recorded during sleep and signs and symptoms of temporomandibular disorders in healthy young adults. J Orofac Pain 2005; 19( 3): 226–231.
Camparis CM, Formigoni G, Teixeira MJ et al. Sleep bruxism and temporomandibular disorder: clinical and polysomnographic evaluation. Arch Oral Biol 2006; 51( 9): 721–728.
Manfredini D, Winocur E, Guarda-Nardini L et al. Epidemiology of bruxism in adults: a systematic review of the literature. J Orofac Pain 2013; 27( 2): 99–110.
Radin EL, Martin RB, Burr DB et al. Effects of mechanical loading on the tissues of the rabbit knee. J Orthop Res 1984; 2( 3): 221–234.
Thompson RC, Oegema TR, Lewis JL et al. Osteoarthrotic changes after acute transarticular load: an animal model. J Bone Joint Surg 1991; 73( 7): 990–1001.
Smith RL, Carter DR, Schurman DJ . Pressure and shear differentially alter human articular chondrocyte metabolism: a review. Clin Orthop Relat Res 2004; 427( Suppl): S89–S95.
Woo SL, Buckwalter JA . Injury and repair of the musculoskeletal soft tissues. J Orthop Res 1988; 6( 6): 907–931.
Romprè PH, Daigle-Landry D, Guitard F et al. Identification of a sleep bruxism sub-group with a higher risk of pain. J Dent Res 2007; 86( 9): 837–842.
Rossetti LM, Pereira de Araujo Cdos R, Rossetti PH et al. Association between rhythmic masticatory muscle activity during sleep and masticatory myofascial pain: a polysomnographic study. J Orofac Pain 2008; 22( 3): 190–200.
Lavigne GJ, Romprè PH, Poirier G et al. Rhythmic masticatory muscle activity during sleep in humans. J Dent Res 2001; 80( 2): 443–448.
Hirose M, Tanaka E, Tanaka M et al. Three-dimensional finite-element model of the human temporomandibular joint disc during prolonged clenching. Eur J Oral Sci 2006; 114( 5): 441–448.
Mori H, Horiuchi S, Nishimura S et al. Three-dimensional finite element analysis of cartilage tissues in human temporomandibular joint during prolonged clenching. Arch Oral Biol 2010; 55( 11): 879–886.
Tanaka E, Hirose M, Koolstra JH et al. Modeling of the effect of friction in the temporomandibular joint on displacement of its disc during prolonged clenching. J Oral Maxillofac Surg 2008; 66( 3): 462–468.
Pérez del Palomar A, Doblaré M . The effect of collagen reinforcement in the behavior of the temporomandibular joint disc. J Biomech 2006; 39( 6): 1075–1085.
Nagahara K, Murata S, Nakamura S et al. Displacement and stress distribution in the temporomandibular joint during clenching. Angle Orthod 1999; 69( 4): 372–379.
Reina JM, García-Aznar JM, Domínguez J et al. Numerical estimation of bone density and elastic constants distribution in a human mandible. J Biomech 2007; 40( 4): 828–836.
Korioth TWP, Romilly DP, Hannam AG . Three-dimensional finite element stress analysis of the dentate human mandible. Am J Phys Anthropol 1992; 88( 1): 69–96.
Nelson GJ . Three dimensional computer modeling of human mandibular biomechanics. PhD thesis, University of British Columbia, Vancouver, Canada, 1986.
Fung YC . Biomechanics: mechanical properties of living tissues. New York: Springer-Verlag, 1993.
Carew EO, Talman EA, Boughner DR et al. Quasi-linear viscoelastic theory applied to internal shearing of porcine aortic valve leaflets. J Biomech Eng 1999; 121( 4): 386–392.
Drapaca CS, Tenti G, Rohlf K et al. A quasi-linear viscoelastic constitutive equation for the brain: application to hydrocephalus. J Elast 2006; 85( 1): 65–83.
Weiss JA, Gardiner JC, Bonifasi-Lista C . Ligament material behavior is nonlinear, viscoelastic and rate-independent under shear loading. J Biomech 2002; 35( 7): 943–950.
Commisso MS, Martínez-Reina J, Mayo J et al. Numerical simulation of a relaxation test designed to fit a quasi-linear viscoelastic model for temporomandibular joint discs. Proc Inst Mech Eng H 2013; 227( 2): 190–199.
Koolstra JH, van Eijden TM . Consequences of viscoelastic behavior in the human temporomandibular joint disc. J Dent Res 2007; 86( 12): 1198–1202.
Tanaka E, Kawai N, Tanaka M et al. The frictional coefficient of the temporomandibular joint and its dependency on the magnitude and duration of joint loading. J Dent Res 2004; 83( 5): 404–407.
Gardiner JC, Weiss JA . Subject-specific finite element analysis of the human medial collateral ligament during valgus knee loading. J Orthop Res 2003; 21( 6): 1098–1106.
Kuboki T, Azuma Y, Orsini MG et al. Effect of sustained unilateral clenching on the temporomandibular joint space. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1996; 82( 6): 616–624.
Werner JA, Tillman B, Schleicher A . Functional anatomy of the temporomandibular joint. Anat Embryol 1991; 183( 1): 89–95.
Oberg T, Carlsson GE, Fajers CM . The temporomandibular joint. A morphologic study on human autopsy material. Acta Odontol Scand 1971; 29( 3): 349–384.
Stratmann U, Schaarschmidt K, Santamaria P . Morphologic investigation of condylar cartilage and disc thickness in the human temporomandibular joint: significance for the definition of osteoarthrotic changes. J Oral Pathol Med 1996; 25( 5): 200–205.
Detamore MS, Athanasiou KA . Structure and function of the temporomandibular joint disc: implications for tissue engineering. J Oral Maxillofac Surg 2003; 61( 4): 494–506.
Acknowledgements
Funding was provided by the Junta de Andalucía for the research project P07-TEP-03115 titled Biomecánica de la Mandíbula Humana, for which this article has been prepared.
Author information
Authors and Affiliations
Corresponding author
Additional information
Note: Supplementary Information for this article can be found on Light: Science & Applications' website
Supplementary information
FigureA1.gif
Figure where the insertion of the different portions of jaw closing muscles is shown and in the table orientation and magnitude of the maximum muscle force exerted by the muscles. (GIF 125 kb)
sustained_clench.mpg
Video of the evolution of the maximum shear stress in the articular disc during sustained clenching. (MPG 970 kb)
rhythmic.mpg
Video of the evolution of the maximum shear stress in the articular disc during RMMA. (MPG 920 kb)
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Commisso, M., Martínez-Reina, J. & Mayo, J. A study of the temporomandibular joint during bruxism. Int J Oral Sci 6, 116–123 (2014). https://doi.org/10.1038/ijos.2014.4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijos.2014.4
Keywords
This article is cited by
-
The association of self-reported awake bruxism and sleep bruxism with temporomandibular pain and dysfunction in adult patients with temporomandibular disorders
Clinical Oral Investigations (2023)
-
Prevalence of awake bruxism in the adult population: a systematic review and meta-analysis
Clinical Oral Investigations (2023)
-
Quasi-Linear Viscoelastic Model of the Articular Disc of the Temporomandibular Joint
Experimental Mechanics (2016)