Abstract
Background/Objectives:
Unhealthy dietary choices are a major contributor to harmful weight gain and obesity. This study interrogated the brain substrates of unhealthy versus healthy food choices in vivo, and evaluated the influence of hunger state and body mass index (BMI) on brain activation and connectivity.
Subjects/Methods:
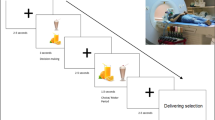
Thirty adults (BMI: 18–38 kg m−2) performed a food-choice task involving preference-based selection between beverage pairs consisting of high-calorie (unhealthy) or low-calorie (healthy) options, concurrent with functional magnetic resonance imaging (fMRI). Selected food stimuli were delivered to participants using an MRI-compatible gustometer. fMRI scans were performed both after 10-h fasting and when sated. Brain activation and hypothalamic functional connectivity were assessed when selecting between unhealthy–healthy beverage pairings, relative to unhealthy–unhealthy and healthy–healthy options. Results were considered significant at cluster-based family-wise error corrected P<0.05.
Results:
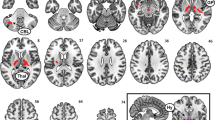
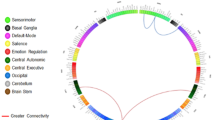
Selecting between unhealthy and healthy foods elicited significant activation in the hypothalamus, the medial and dorsolateral prefrontal cortices, the anterior insula and the posterior cingulate. Hunger was associated with higher activation within the ventromedial and dorsolateral prefrontal cortices, as well as lower connectivity between the hypothalamus and both the ventromedial prefrontal cortex and dorsal striatum. Critically, people with higher BMI showed lower activation of the hypothalamus—regardless of hunger state—and higher activation of the ventromedial prefrontal cortex when hungry.
Conclusions:
People who are overweight and obese have weaker activation of brain regions involved in energy regulation and greater activation of reward valuation regions while making choices between unhealthy and healthy foods. These results provide evidence for a shift towards hedonic-based, and away from energy-based, food selection in obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014; 384: 766–781.
Hruby A, Manson JE, Qi L, Malik VS, Rimm EB, Sun Q et al. Determinants and consequences of obesity. Am J Public Health 2016; 106: 1656–1662.
Zhou B, Gao W, Lv J, Yu C, Wang S, Liao C et al. Genetic and environmental influences on obesity-related phenotypes in chinese twins reared apart and together. Behav Genet 2015; 45: 427–437.
Crino M, Sacks G, Vandevijvere S, Swinburn B, Neal B . The influence on population weight gain and obesity of the macronutrient composition and energy density of the food supply. Curr Obes Rep 2015; 4: 1–10.
Levy DJ, Glimcher PW . Comparing apples and oranges: using reward-specific and reward-general subjective value representation in the brain. J Neurosci 2011; 31: 14693–14707.
Waterson MJ, Horvath TL . Neuronal regulation of energy homeostasis: beyond the hypothalamus and feeding. Cell Metab 2015; 22: 962–970.
Stuber GD, Wise RA . Lateral hypothalamic circuits for feeding and reward. Nat Neurosci 2016; 19: 198–205.
Dietrich MO, Horvath TL . Hypothalamic control of energy balance: insights into the role of synaptic plasticity. Trends Neurosci 2013; 36: 65–73.
Sternson SM, Atasoy D, Betley JN, Henry FE, Xu S . An emerging technology framework for the neurobiology of appetite. Cell Metab 2016; 23: 234–253.
Krashes MJ, Lowell BB, Garfield AS . Melanocortin-4 receptor-regulated energy homeostasis. Nat Neurosci 2016; 19: 206–219.
Arana FS, Parkinson JA, Hinton E, Holland AJ, Owen AM, Roberts AC . Dissociable contributions of the human amygdala and orbitofrontal cortex to incentive motivation and goal selection. J Neurosci 2003; 23: 9632–9638.
Hare TA, Malmaud J, Rangel A . Focusing attention on the health aspects of foods changes value signals in vmPFC and improves dietary choice. J Neurosci 2011; 31: 11077–11087.
Malik S, McGlone F, Bedrossian D, Dagher A . Ghrelin modulates brain activity in areas that control appetitive behavior. Cell Metab 2008; 7: 400–409.
Farooqi IS, Bullmore E, Keogh J, Gillard J, O'Rahilly S, Fletcher PC . Leptin regulates striatal regions and human eating behavior. Science 2007; 317: 1355.
Zheng H, Corkern M, Stoyanova I, Patterson LM, Tian R, Berthoud HR . Peptides that regulate food intake: appetite-inducing accumbens manipulation activates hypothalamic orexin neurons and inhibits POMC neurons. Am J Physiol Regul Integr Comp Physiol 2003; 284: R1436–R1444.
Polania R, Moisa M, Opitz A, Grueschow M, Ruff CC . The precision of value-based choices depends causally on fronto-parietal phase coupling. Nature Commun 2015; 6: 8090.
Hare TA, Camerer CF, Rangel A . Self-control in decision-making involves modulation of the vmPFC valuation system. Science 2009; 324: 646–648.
Brooks SJ, Cedernaes J, Schiöth HB . Increased prefrontal and parahippocampal activation with reduced dorsolateral prefrontal and insular cortex activation to food images in obesity: a meta-analysis of fMRI studies. PLoS One 2013; 8: e60393.
Kennedy J, Dimitropoulos A . Influence of feeding state on neurofunctionaldifferences between individuals who are obese and normal weight: a meta-analysis of neuroimaging studies. Appetite 2014; 75: 103–109.
Demos KE, Heatherton TF, Kelley WM . Individual differences in nucleus accumbens activity to food and sexual images predict weight gain and sexualbehavior. J Neurosci 2012; 32: 5549–5552.
Medic N, Ziauddeen H, Forwood SE, Davies KM, Ahern AL, Jebb SA et al. The presence of real food usurps hypothetical health value judgment in overweight people. eNeuro 2016; 3: (pii: ENEURO.0025-16.2016) doi:10.1523/ENEURO.0025-16.2016.
Val-Laillet D, Aarts E, Weber B, Ferrari M, Quaresima V, Stoeckel LE et al. Neuroimaging and neuromodulation approaches to study eating behavior and prevent and treat eating disorders and obesity. Neuroimage Clin 2015; 8: 1–31.
Clemmensen C, Muller TD, Woods SC, Berthoud HR, Seeley RJ, Tschop MH . Gut–brain cross-talk in metabolic control. Cell 2017; 168: 758–774.
Morrison CD, Berthoud HR . Neurobiology of nutrition and obesity. Nutr Rev 2007; 65 (Part 1): 517–534.
Volkow ND, Wang GJ, Baler RD . Reward, dopamine and the control of food intake: implications for obesity. Trends Cogn Sci 2011; 15: 37–46.
Ziauddeen H, Alonso-Alonso M, Hill JO, Kelley M, Khan NA . Obesity and the neurocognitive basis of food reward and the control of intake. Adv Nutr 2015; 6: 474–486.
McLaren DG, Ries ML, Xu G, Johnson SC . A generalized form of context-dependent psychophysiological interactions (gPPI): a comparison to standard approaches. Neuroimage 2012; 61: 1277–1286.
Stice E, Yokum S . Gain in body fat is associated with increased striatal response to palatable food cues, whereas body fat stability is associated with decreased striatal response. J Neurosci 2016; 36: 6949–6956.
Berthoud HR . The neurobiology of food intake in an obesogenic environment. Proc Nutr Soc 2012; 71: 478–487.
van der Laan LN, de Ridder DT, Viergever MA, Smeets PA . The first taste is always with the eyes: a meta-analysis on the neural correlates of processing visual food cues. Neuroimage 2011; 55: 296–303.
Stice E, Burger K, Yokum S . Caloric deprivation increases responsivity of attention and reward brain regions to intake, anticipated intake, and images of palatable foods. Neuroimage 2013; 67: 322–330.
Goldstone AP, Prechtl CG, Scholtz S, Miras AD, Chhina N, Durighel G et al. Ghrelin mimics fasting to enhance human hedonic, orbitofrontal cortex, and hippocampal responses to food. Am J Clin Nutr 2014; 99: 1319–1330.
Verdejo-Garcia A, Verdejo-Roman J, Rio-Valle JS, Lacomba JA, Lagos FM, Soriano-Mas C . Dysfunctional involvement of emotion and reward brain regions on social decision making in excess weight adolescents. Hum Brain Mapp 2015; 36: 226–237.
Murray RJ, Debbane M, Fox PT, Bzdok D, Eickhoff SB . Functional connectivity mapping of regions associated with self- and other-processing. Hum Brain Mapp 2015; 36: 1304–1324.
O'Doherty JP . Contributions of the ventromedial prefrontal cortex to goal-directed action selection. Ann NY Acad Sci 2011; 1239: 118–129.
Dimitropoulos A, Tkach J, Ho A, Kennedy J . Greater corticolimbic activation to high-calorie food cues after eating in obese vs normal-weight adults. Appetite 2012; 58: 303–312.
Martin LE, Holsen LM, Chambers RJ, Bruce AS, Brooks WM, Zarcone JR et al. Neural mechanisms associated with food motivation in obese and healthyweight adults. Obesity 2010; 18: 254–260.
Blechert J, Klackl J, Miedl SF, Wilhelm FH . To eat or not to eat: effects of food availability on reward system activity during food picture viewing. Appetite 2016; 99: 254–261.
Lawrence NS, Hinton EC, Parkinson JA, Lawrence AD . Nucleus accumbens response to food cues predicts subsequent snack consumption in women and increased body mass index in those with reduced self-control. Neuroimage 2012; 63: 415–422.
Acknowledgements
This study was funded by a Medical Research Grant from the Ian Potter Foundation (2015) and a Strategic Grant from the Faculty of Medicine, Monash University (Strategic Grant Scheme, 2015) (to AVG). IHH supported by Australian National Health and Medical Research Council Fellowship (1106533). ZBA supported by Australian National Health and Medical Research Council Fellowship (1084344). CSM supported by a Miguel Servet contract from the Carlos III Health Institute (CPII16/00048). We would like to acknowledge Helen Truby and Alastair Kwok for developing the beverages used in the task, the Monash Instrumentation Office for developing the gustometer, and Erynn Christensen and Sarah Giles for invaluable help with data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Rights and permissions
About this article
Cite this article
Harding, I., Andrews, Z., Mata, F. et al. Brain substrates of unhealthy versus healthy food choices: influence of homeostatic status and body mass index. Int J Obes 42, 448–454 (2018). https://doi.org/10.1038/ijo.2017.237
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.237
This article is cited by
-
Neural underpinnings of food choice and consumption in obesity
International Journal of Obesity (2022)
-
Human Taste-Perception: Brain Computer Interface (BCI) and Its Application as an Engineering Tool for Taste-Driven Sensory Studies
Food Engineering Reviews (2022)
-
A systematic review of resting-state functional connectivity in obesity: Refining current neurobiological frameworks and methodological considerations moving forward
Reviews in Endocrine and Metabolic Disorders (2022)
-
Neural network modelling reveals changes in directional connectivity between cortical and hypothalamic regions with increased BMI
International Journal of Obesity (2021)
-
Reliability of neural food cue-reactivity in participants with obesity undergoing bariatric surgery: a 26-week longitudinal fMRI study
European Archives of Psychiatry and Clinical Neuroscience (2021)