Abstract
Objective:
The objective of this study was to examine whether childhood cardiorespiratory fitness attenuates or modifies the long-term cardiometabolic risks associated with childhood obesity.
Design and Methods:
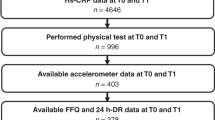
The study consisted of a 20-year follow-up of 1792 adults who participated in the 1985 Australian Schools Health and Fitness Survey when they were 7–15 years of age. Baseline measures included a 1.6-km run to assess cardiorespiratory fitness and waist circumference to assess abdominal adiposity. At follow-up, participants attended study clinics where indicators of Metabolic Syndrome (MetS) (waist circumference, blood pressure, fasting blood glucose and lipids) were measured and cardiorespiratory fitness was reassessed using a submaximal graded exercise test.
Results:
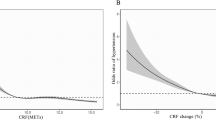
Both high waist circumference and low cardiorespiratory fitness in childhood were significant independent predictors of MetS in early adulthood. The mutually adjusted relative risk of adult MetS was 3.00 (95% confidence interval: 1.85–4.89) for children in the highest (vs lowest) third of waist circumference and 0.64 (95% confidence interval: 0.43–0.96) for children with high (vs low) cardiorespiratory fitness. No significant interaction between waist circumference and fitness was observed, with higher levels of childhood fitness associated with lower risks of adult MetS among those with either low or high childhood waist circumference values. Participants who had both high waist circumference and low cardiorespiratory fitness in childhood were 8.5 times more likely to have MetS in adulthood than those who had low waist circumference and high cardiorespiratory fitness in childhood. Regardless of childhood obesity status, participants with low childhood fitness who increased their relative fitness by adulthood had a substantially lower prevalence of MetS than those who remained low fit.
Conclusions:
Childhood waist circumference and cardiorespiratory fitness are both strongly associated with cardiometabolic health in later life. Higher levels of cardiorespiratory fitness substantially reduce the risk of adult MetS, even among those with abdominal obesity in childhood.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Wang Y, Lobstein T . Worldwide trends in childhood overweight and obesity. Int J Pediatr Obes 2006; 1: 11–25.
Ogden CL, Carroll MD, Curtin LR, Lamb MM, Flegal KM . Prevalence of high body mass index in US children and adolescents, 2007-2008. JAMA 2010; 303: 242–249.
Weiss R, Caprio S . The metabolic consequences of childhood obesity. Best Pract Res Clin Endocrinol Metab 2005; 19: 405–419.
Daniels SR . Complications of obesity in children and adolescents. Int J Obes (Lond) 2009; 33 (Suppl 1): S60–S65.
Schmidt MD, Dwyer T, Magnussen CG, Venn AJ . Predictive associations between alternative measures of childhood adiposity and adult cardio-metabolic health. Int J Obes (Lond) 2011; 35: 38–45.
Mattsson N, Ronnemaa T, Juonala M, Viikari JS, Raitakari OT . Childhood predictors of the metabolic syndrome in adulthood. The Cardiovascular Risk in Young Finns Study. Ann Med 2008; 40: 542–552.
Juonala M, Magnussen CG, Berenson GS, Venn A, Burns TL, Sabin MA et al. Childhood adiposity, adult adiposity, and cardiovascular risk factors. N Engl J Med 2011; 365: 1876–1885.
Venn AJ, Thomson RJ, Schmidt MD, Cleland VJ, Curry BA, Gennat HC et al. Overweight and obesity from childhood to adulthood: a follow-up of participants in the 1985 Australian Schools Health and Fitness Survey. Med J Aust 2007; 186: 458–460.
Singh AS, Mulder C, Twisk JW, van Mechelen W, Chinapaw MJ . Tracking of childhood overweight into adulthood: a systematic review of the literature. Obes Rev 2008; 9: 474–488.
LaMonte MJ, Barlow CE, Jurca R, Kampert JB, Church TS, Blair SN . Cardiorespiratory fitness is inversely associated with the incidence of metabolic syndrome: a prospective study of men and women. Circulation 2005; 112: 505–512.
LaMonte MJ, Blair SN . Physical activity, cardiorespiratory fitness, and adiposity: contributions to disease risk. Curr Opin Clin Nutr Metab Care 2006; 9: 540–546.
Sui X, Hooker SP, Lee IM, Church TS, Colabianchi N, Lee CD et al. A prospective study of cardiorespiratory fitness and risk of type 2 diabetes in women. Diabetes Care 2008; 31: 550–555.
Wei M, Kampert JB, Barlow CE, Nichaman MZ, Gibbons LW, Paffenbarger RS Jr et al. Relationship between low cardiorespiratory fitness and mortality in normal-weight, overweight, and obese men. JAMA 1999; 282: 1547–1553.
Church TS, Finley CE, Earnest CP, Kampert JB, Gibbons LW, Blair SN . Relative associations of fitness and fatness to fibrinogen, white blood cell count, uric acid and metabolic syndrome. Int J Obes Relat Metab Disord 2002; 26: 805–813.
Wei M, Gibbons LW, Mitchell TL, Kampert JB, Lee CD, Blair SN . The association between cardiorespiratory fitness and impaired fasting glucose and type 2 diabetes mellitus in men. Ann Intern Med 1999; 130: 89–96.
Wessel TR, Arant CB, Olson MB, Johnson BD, Reis SE, Sharaf BL et al. Relationship of physical fitness vs body mass index with coronary artery disease and cardiovascular events in women. JAMA 2004; 292: 1179–1187.
Boreham C, Twisk J, Murray L, Savage M, Strain JJ, Cran G . Fitness, fatness, and coronary heart disease risk in adolescents: the Northern Ireland Young Hearts Project. Med Sci Sports Exerc 2001; 33: 270–274.
Eisenmann JC, Welk GJ, Wickel EE, Blair SN . Combined influence of cardiorespiratory fitness and body mass index on cardiovascular disease risk factors among 8-18 year old youth: The Aerobics Center Longitudinal Study. Int J Pediatr Obes 2007; 2: 66–72.
Eisenmann JC, Wickel EE, Welk GJ, Blair SN . Relationship between adolescent fitness and fatness and cardiovascular disease risk factors in adulthood: The Aerobics Center Longitudinal Study (ACLS). Am Heart J 2005; 149: 46–53.
Silva G, Aires L, Martins C, Mota J, Oliveira J, Ribeiro JC . Cardiorespiratory fitness associates with metabolic risk independent of central adiposity. Int J Sports Med 2013; 34: 912–916.
Andersen LB, Sardinha LB, Froberg K, Riddoch CJ, Page AS, Anderssen SA . Fitness, fatness and clustering of cardiovascular risk factors in children from Denmark, Estonia and Portugal: the European Youth Heart Study. Int J Pediatr Obes 2008; 3 (Suppl 1):58–66.
Kwon S, Burns TL, Janz KF . Associations of cardiorespiratory fitness and fatness with cardiovascular risk factors among adolescents: The NHANES 1999-2002. J Phys Act Health 2010; 7: 746–753.
Carson V, Rinaldi RL, Torrance B, Maximova K, Ball GDC, Majumdar SR et al. Vigorous physical activity and longitudinal associations with cardiometabolic risk factors in youth. Int J Obes 2014; 38: 16–21.
Andersen LB, Bugge A, Dencker M, Eiberg S, El-Naaman B . The association between physical activity, physical fitness and development of metabolic disorders. Int J Pediatr Obes 2011; 6: 29–34.
Janz KF, Dawson JD, Mahoney LT . Increases in physical fitness during childhood improve cardiovascular health during adolescence: the Muscatine Study. Int J Sports Med 2002; 23 (Suppl 1):S15–S21.
Dwyer T, Gibbons LE . The Australian Schools Health and Fitness Survey. Physical fitness related to blood pressure but not lipoproteins. Circulation 1994; 89: 1539–1544.
George JD, Vehrs PR, Allsen PE, Fellingham GW, Fisher GA . VO2max estimation from a submaximal 1-mile track jog for fit college-age individuals. Med Sci Sports Exerc 1993; 25: 401–406.
Cureton KJ, Sloniger MA, O'Bannon JP, Black DN, McCormack WP . A generalized equation for prediction of VO2 peak from one-mile run/walk performance in youth. Med Sci Sports Exerc 1995; 27: 445–451.
Withers RT, Davies GJ, Crouch RG . A comparison of three W170 protocols. Eur J Appl Physiol Occup Physiol 1977; 37: 123–128.
Siri WE . The gross composition of the body. Adv Biol Med Phys 1956; 4: 239–280.
Durnin JV, Womersley J . Body fat assessed from total body density and its estimation from skinfold thickness: measurements on 481 men and women aged from 16 to 72 years. Br J Nutr 1974; 32: 77–97.
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA et al. Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009; 120: 1640–1645.
Dwyer T, Magnussen CG, Schmidt MD, Ukoumunne OC, Ponsonby AL, Raitakari OT et al. Decline in physical fitness from childhood to adulthood associated with increased obesity and insulin resistance in adults. Diabetes Care 2009; 32: 683–687.
Park MH, Falconer C, Viner RM, Kinra S . The impact of childhood obesity on morbidity and mortality in adulthood: a systematic review. Obes Rev 2012; 13: 985–1000.
NCEP. Executive summary of the third report of the national cholesterol education program (NCEP) expert panel on detection, elevation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA 2001; 285: 2486–2497.
Stevens J, Cai J, Evenson KR, Thomas R . Fitness and fatness as predictors of mortality from all causes and from cardiovascular disease in men and women in the lipid research clinics study. Am J Epidemiol 2002; 156: 832–841.
Lee S, Kuk JL, Katzmarzyk PT, Blair SN, Church TS, Ross R . Cardiorespiratory fitness attenuates metabolic risk independent of abdominal subcutaneous and visceral fat in men. Diabetes Care 2005; 28: 895–901.
Eisenmann JC, Welk GJ, Ihmels M, Dollman J . Fatness, fitness, and cardiovascular disease risk factors in children and adolescents. Med Sci Sports Exerc 2007; 39: 1251–1256.
Nyberg G, Ekelund U, Yucel-Lindberg TL, Mode RT, Marcus C . Differences in metabolic risk factors between normal weight and overweight children. Int J Pediatr Obes 2011; 6: 244–252.
Puder JJ, Schindler C, Zahner L, Kriemler S . Adiposity, fitness and metabolic risk in children: a cross-sectional and longitudinal study. Int J Pediatr Obes 2011; 6: e297–e306.
Telford RD, Cunningham RB, Telford RM, Kerrigan J, Hickman PE, Potter JM et al. Effects of changes in adiposity and physical activity on preadolescent insulin resistance: The Australian LOOK Longitudinal Study. Plos One 2012; 7: 6.
Carnethon MR, Gidding SS, Nehgme R, Sidney S, Jacobs DR Jr, Liu K . Cardiorespiratory fitness in young adulthood and the development of cardiovascular disease risk factors. JAMA 2003; 290: 3092–3100.
Twisk JW, Kemper HC, van Mechelen W . The relationship between physical fitness and physical activity during adolescence and cardiovascular disease risk factors at adult age. The Amsterdam Growth and Health Longitudinal Study. Int J Sports Med 2002; 23 (Suppl 1): S8–14.
Dollman JT, Olds S . Secular changes in fatness and fat distribution in Australian children matched for body size. Int J Pediatr Obes 2006; 1: 109–113.
Prentice AM . The emerging epidemic of obesity in developing countries. Int J Epidemiol 2006; 35: 93–99.
Tomkinson GR, Olds TS . Secular changes in pediatric aerobic fitness test performance: The global picture. Med Sport Sci 2007; 50: 46–66.
Bai Y, Saint-Maurice PF, Welk GJ, Allums-Featherston K, Candelaria N, Anderson K . Prevalence of youth fitness in the United States: Baseline results from the NFL PLAY 60 FITNESSGRAM partnership project. J Pediatr 2015; 167: 662–668.
Plowman SA . Muscular strength, endurance, and flexibility assessments. In: Plowman SA, Meredith MD (eds), Fitnessgram/Activitygram Reference Guide 4th ed. The Cooper Institute: Dallas, TX, USA, pp 8–55.
Hasselstrom H, Hansen SE, Froberg K, Andersen LB . Physical fitness and physical activity during adolescence as predictors of cardiovascular disease risk in young adulthood. Danish Youth and Sports Study. An eight-year follow-up study. Int J Sports Med 2002; 23 (Suppl 1): S27–S31.
Acknowledgements
The Childhood Determinants of Adult Health study was funded by grants from the Australian National Health and Medical Research Council, the Australian National Heart Foundation, the Tasmanian Community Fund, and Veolia Environmental Services. Financial support was also provided by Sanitarium Health Food Company, ASICS Oceania, and Target Australia. Dr Schmidt was supported by a National Heart Foundation of Australia postdoctoral fellowship. We gratefully acknowledge the contributions of the Childhood Determinants of Adult Health Study’s project manager, Marita Dalton, all other project staff and volunteers, and the study participants.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Schmidt, M., Magnussen, C., Rees, E. et al. Childhood fitness reduces the long-term cardiometabolic risks associated with childhood obesity. Int J Obes 40, 1134–1140 (2016). https://doi.org/10.1038/ijo.2016.61
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2016.61
This article is cited by
-
The Impact of Typical School Provision of Physical Education, Physical Activity and Sports on Adolescent Physical Health: A Systematic Literature Review and Meta-Analysis
Adolescent Research Review (2024)
-
Effects of Movement Behaviors on Overall Health and Appetite Control: Current Evidence and Perspectives in Children and Adolescents
Current Obesity Reports (2022)
-
The relationship between multiple perfluoroalkyl substances and cardiorespiratory fitness in male adolescents
Environmental Science and Pollution Research (2022)
-
Disparities in physical fitness of 6–11-year-old children: the 2012 NHANES National Youth Fitness Survey
BMC Public Health (2020)
-
Exercise-associated prevention of adult cardiovascular disease in children and adolescents: monocytes, molecular mechanisms, and a call for discovery
Pediatric Research (2020)