Abstract
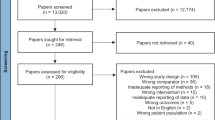
Understanding the physiological response to meal intake, of gut-derived appetite and satiety hormone signals, in obese compared with healthy-weight children may assist with informing strategies to help curtail the obesity epidemic. A systematic review and meta-analysis of studies investigating the acute postprandial response of gastrointestinal appetite hormones to meal intake in obese children was undertaken. Systematic searches of databases EMBASE, CINAHL Plus, OVID Medline and the Cochrane Library were performed. Inclusion criteria: a randomised controlled trial or experimental cross-sectional study following an acute test meal protocol with pre- and postprandial analysis of plasma or serum gastrointestinal hormone concentrations. Database searching retrieved 1001 papers for review. Nine studies met the inclusion criteria, collectively reporting on six appetite hormones yielding a total of 32 test meal–hormone comparisons. Meta-analyses compared the pooled estimate of the mean difference of the postprandial change in total ghrelin and total peptide YY (PYY). Obese compared with healthy-weight children had an attenuated change in ghrelin at 60 min (N=5 studies; n=129 participants) and 120 min postprandial (N=4 studies; n=100 participants) (P<0.05 for both time points). Obese compared with healthy-weight children also had an attenuated PYY response at 60 min (N=5 studies; n=128 participants) and 120 min postprandial (N=4 studies; n=100 participants). Insufficient studies reported on the postprandial time course of other appetite-related hormones, precluding a meta-analysis. Limited evidence notwithstanding, these findings indicate that PYY and ghrelin responses to a meal may be altered in obese children. This review has also identified a major gap in knowledge of hormonal appetite responses in childhood obesity. More comprehensive investigations of the homoeostatic regulation of gut-derived appetite and satiety hormone signals with behavioural and clinical outcomes are warranted to understand if there are consequences of these differences.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014; 384: 766–781.
Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS . The relation of childhood BMI to adult adiposity: the Bogalusa Heart Study. Pediatrics 2005; 115: 22–27.
Konturek PC, Konturek JW, Czesnikiewicz-Guzik M, Brzozowski T, Sito E, Konturek SJ . Neuro-hormonal control of food intake: basic mechanisms and clinical implications. J Physiol Pharmacol 2005; 56 (Suppl 6): 5–25.
Katzmarzyk PT, Barlow S, Bouchard C, Catalano PM, Hsia DS, Inge TH et al. An evolving scientific basis for the prevention and treatment of pediatric obesity. Int J Obes (Lond) 2014; 38: 887–905.
Delzenne N, Blundell J, Brouns F, Cunningham K, De Graaf K, Erkner A et al. Gastrointestinal targets of appetite regulation in humans. Obes Rev 2010; 11: 234–250.
Klok MD, Jakobsdottir S, Drent ML . The role of leptin and ghrelin in the regulation of food intake and body weight in humans: a review. Obes Rev 2007; 8: 21–34.
Batterham RL, Heffron H, Kapoor S, Chivers JE, Chandarana K, Herzog H et al. Critical role for peptide YY in protein-mediated satiation and body-weight regulation. Cell Metab 2006; 4: 223–233.
le Roux CW, Patterson M, Vincent RP, Hunt C, Ghatei MA, Bloom SR . Postprandial plasma ghrelin is suppressed proportional to meal calorie content in normal-weight but not obese subjects. J Clin Endocrinol Metab 2005; 90: 1068–1071.
Evidence Analysis Manual: Steps in the Academy Evidence Analysis Process. Academy of Nutrition and Dietetics: Chicago, IL, USA, 2012.
Higgins JPT, Green S . Cochrane Handbook for Systematic Reviews of Interventions. Version 5.1.0 Chichester. John Wiley & Sons Ltd: United Kingdom, 2011.
Vos RC, Pijl H, Wit JM, van Zwet EW, van der Bent C, Houdijk EC . The effect of multidisciplinary lifestyle intervention on the pre- and postprandial plasma gut peptide concentrations in children with obesity. ISRN Endocrinol 2011; 2011: 353756.
Galhardo J, Hunt LP, Lightman SL, Sabin MA, Bergh C, Sodersten P et al. Normalizing eating behavior reduces body weight and improves gastrointestinal hormonal secretion in obese adolescents. J Clin Endocrinol Metab 2012; 97: E193–E201.
Leidy HJ, Ortinau LC, Douglas SM, Hoertel HA . Beneficial effects of a higher-protein breakfast on the appetitive, hormonal, and neural signals controlling energy intake regulation in overweight/obese, ‘breakfast-skipping,’ late-adolescent girls. Am J Clin Nutr 2013; 97: 677–688.
Patel BP, Anderson GH, Vien S, Bellissimo N, McCrindle BW, Hamilton JK . Obesity, sex and pubertal status affect appetite hormone responses to a mixed glucose and whey protein drink in adolescents. Clin Endocrinol (Oxf) 2014; 81: 63–70.
Shen C, Yu T, Tang ZH, Wu KM . Changes in ghrelin and obestatin levels before and after a meal in children with simple obesity and anorexia. Horm Res Paediatr 2013; 79: 341–346.
Baldelli R, Bellone S, Castellino N, Petri A, Rapa A, Vivenza D et al. Oral glucose load inhibits circulating ghrelin levels to the same extent in normal and obese children. Clin Endocrinol (Oxf) 2006; 64: 255–259.
Lanyi E, Csernus K, Erhardt E, Toth K, Urban B, Lenard L et al. Plasma levels of acylated ghrelin during an oral glucose tolerance test in obese children. J Endocrinol Invest 2007; 30: 133–137.
Martos-Moreno GA, Barrios V, Martinez G, Hawkins F, Argente J . Acylated ghrelin levels in pre-pubertal obese children at diagnosis and after weight reduction: effect of oral glucose ingestion. J Endocrinol Invest 2011; 34: 117–123.
Prodam F, Trovato L, Demarchi I, Busti A, Petri A, Moia S et al. Unacylated, acylated ghrelin and obestatin levels are differently inhibited by oral glucose load in pediatric obesity: association with insulin sensitivity and metabolic alterations. e-SPEN 2011; 6: e109–e115.
Roth CL, Bongiovanni KD, Gohlke B, Woelfle J . Changes in dynamic insulin and gastrointestinal hormone secretion in obese children. J Pediatr Endocrinol 2010; 23: 1299–1309.
Soriano-Guillen L, Barrios V, Martos G, Chowen JA, Campos-Barros A, Argente J . Effect of oral glucose administration on ghrelin levels in obese children. Eur J Endocrinol 2004; 151: 119–121.
Lomenick JP, Clasey JL, Anderson JW . Meal-related changes in ghrelin, peptide YY, and appetite in normal weight and overweight children. Obesity 2008; 16: 547–552.
Lomenick JP, White JR, Smart EJ, Clasey JL, Anderson JW . Glucagon-like peptide 1 and pancreatic polypeptide responses to feeding in normal weight and overweight children. J Pediatr Endocrinol Metab 2009; 22: 493–500.
Gil-Campos M, Aguilera CM, Ramirez-Tortosa MC, Canete R, Gil A . Fasting and postprandial relationships among plasma leptin, ghrelin, and insulin in prepubertal obese children. Clin Nutr 2010; 29: 54–59.
Lomenick JP, Melguizo MS, Mitchell SL, Summar ML, Anderson JW . Effects of meals high in carbohydrate, protein, and fat on ghrelin and peptide YY secretion in prepubertal children. J Clin Endocrinol Metab 2009; 94: 4463–4471.
Misra M, Tsai PM, Mendes N, Miller KK, Klibanski A . Increased carbohydrate induced ghrelin secretion in obese vs. normal-weight adolescent girls. Obesity 2009; 17: 1689–1695.
Mittelman SD, Klier K, Braun S, Azen C, Geffner ME, Buchanan TA . Obese adolescents show impaired meal responses of the appetite-regulating hormones ghrelin and PYY. Obesity 2010; 18: 918–925.
Tomasik P, Sztefko K, Starzyk J . Entero-insular axis in children with simple obesity. Pediatr Endocrinol Diabetes Metab 2009; 15: 63–69.
Sysko R, Devlin MJ, Schebendach J, Tanofsky-Kraff M, Zimmerli E, Korner J et al. Hormonal responses and test meal intake among obese teenagers before and after laparoscopic adjustable gastric banding. Am J Clin Nutr 2013; 98: 1151–1161.
Stock S, Leichner P, Wong ACK, Ghatei MA, Kieffer TJ, Bloom SR et al. Ghrelin, peptide YY, glucose-dependent insulinotropic polypeptide, and hunger responses to a mixed meal in anorexic, obese, and control female adolescents. J Clin Endocrinol Metab 2005; 90: 2161–2168.
le Roux CW, Batterham RL, Aylwin SJ, Patterson M, Borg CM, Wynne KJ et al. Attenuated peptide YY release in obese subjects is associated with reduced satiety. Endocrinology 2006; 147: 3–8.
Batterham RL, Cohen MA, Ellis SM, Le Roux CW, Withers DJ, Frost GS et al. Inhibition of food intake in obese subjects by peptide YY3-36. N Engl J Med 2003; 349: 941–948.
Batterham RL, Cowley MA, Small CJ, Herzog H, Cohen MA, Dakin CL et al. Gut hormone PYY(3-36) physiologically inhibits food intake. Nature 2002; 418: 650–654.
Gibbons C, Caudwell P, Finlayson G, Webb DL, Hellstrom PM, Naslund E et al. Comparison of postprandial profiles of ghrelin, active GLP-1, and total PYY to meals varying in fat and carbohydrate and their association with hunger and the phases of satiety. J Clin Endocrinol Metab 2013; 98: E847–E855.
Blom WA, Lluch A, Stafleu A, Vinoy S, Holst JJ, Schaafsma G et al. Effect of a high-protein breakfast on the postprandial ghrelin response. Am J Clin Nutr 2006; 83: 211–220.
Tong J, Tschop MH, Aulinger BA, Davis HW, Yang Q, Liu J et al. The intestinal lymph fistula model–a novel approach to study ghrelin secretion. Am J Physiol Gastrointest Liver Physiol 2010; 298: G474–G480.
Tschop M, Smiley DL, Heiman ML . Ghrelin induces adiposity in rodents. Nature 2000; 407: 908–913.
Reinehr T, de Sousa G, Roth CL . Obestatin and ghrelin levels in obese children and adolescents before and after reduction of overweight. Clin Endocrinol (Oxf) 2008; 68: 304–310.
Tschop M, Weyer C, Tataranni PA, Devanarayan V, Ravussin E, Heiman ML . Circulating ghrelin levels are decreased in human obesity. Diabetes 2001; 50: 707–709.
English PJ, Ghatei MA, Malik IA, Bloom SR, Wilding JP . Food fails to suppress ghrelin levels in obese humans. J Clin Endocrinol Metab 2002; 87: 2984–2987.
de Graaf C, Blom WA, Smeets PA, Stafleu A, Hendriks HF . Biomarkers of satiation and satiety. Am J Clin Nutr 2004; 79: 946–961.
Foster-Schubert KE, Overduin J, Prudom CE, Liu J, Callahan HS, Gaylinn BD et al. Acyl and total ghrelin are suppressed strongly by ingested proteins, weakly by lipids, and biphasically by carbohydrates. J Clin Endocrinol Metab 2008; 93: 1971–1979.
Bowen J, Noakes M, Trenerry C, Clifton PM . Energy intake, ghrelin, and cholecystokinin after different carbohydrate and protein preloads in overweight men. J Clin Endocrinol Metab 2006; 91: 1477–1483.
Sumithran P, Prendergast LA, Delbridge E, Purcell K, Shulkes A, Kriketos A et al. Long-term persistence of hormonal adaptations to weight loss. N Engl J Med 2011; 365: 1597–1604.
Jensen DE, Nguo K, Baxter KA, Cardinal JW, King NA, Ware RS et al. Fasting gut hormone levels change with modest weight loss in obese adolescents. Pediatr Obes 2015; 10: 380–387.
Samat A, Malin SK, Huang H, Schauer PR, Kirwan JP, Kashyap SR . Ghrelin suppression is associated with weight loss and insulin action following gastric bypass surgery at 12 months in obese adults with type 2 diabetes. Diabetes Obes Metab 2013; 15: 963–966.
Dirksen C, Jorgensen NB, Bojsen-Moller KN, Kielgast U, Jacobsen SH, Clausen TR et al. Gut hormones, early dumping and resting energy expenditure in patients with good and poor weight loss response after Roux-en-Y gastric bypass. Int J Obes (Lond) 2013; 37: 1452–1459.
Jacobsen SH, Olesen SC, Dirksen C, Jorgensen NB, Bojsen-Moller KN, Kielgast U et al. Changes in gastrointestinal hormone responses, insulin sensitivity, and beta-cell function within 2 weeks after gastric bypass in non-diabetic subjects. Obes Surg 2012; 22: 1084–1096.
Whatmore AJ, Hall CM, Jones J, Westwood M, Clayton PE . Ghrelin concentrations in healthy children and adolescents. Clin Endocrinol (Oxf) 2003; 59: 649–654.
Lloyd B, Ravi P, Mendes N, Klibanski A, Misra M . Peptide YY levels across pubertal stages and associations with growth hormone. J Clin Endocrinol Metab 2010; 95: 2957–2962.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Author contributions
The authors’ responsibilities were as follows: KN, CEH, MB designed the PICO, conducted the literature search analysis and meta-analysis, and wrote the first draft of the manuscript; KN and KZW extracted the data and performed the quality assessment (independently). KN, CEH: interpreted the data, KN, CEH, MB, KZW: revised subsequent drafts and approved the final version for publication.
Supplementary Information accompanies this paper on International Journal of Obesity website
Rights and permissions
About this article
Cite this article
Nguo, K., Walker, K., Bonham, M. et al. Systematic review and meta-analysis of the effect of meal intake on postprandial appetite-related gastrointestinal hormones in obese children. Int J Obes 40, 555–563 (2016). https://doi.org/10.1038/ijo.2015.256
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2015.256