Abstract
Background:
Obese individuals are more likely to have either lower blood concentrations or lower bioavailability of minerals and/or vitamins. However, there are limited data on the effects of nutritional supplementation on body weight (BW) control, energy homeostasis and lipid metabolism in obese subjects.
Objective:
The purpose of this study is to evaluate the effects of supplementation with multivitamin and multimineral on adiposity, energy expenditure and lipid profiles in obese Chinese women.
Design:
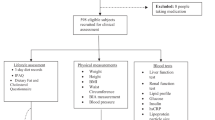
A total of 96 obese Chinese women (body mass index (BMI) 28 kg m−2) aged 18–55 years participated in a 26-week randomized, double-blind, placebo-controlled intervention study. Subjects were randomized into three groups, receiving either one tablet of multivitamin and mineral supplement (MMS), or calcium 162 mg (Calcium) or identical placebo daily during the study period. BW, BMI, waist circumference (WC), fat mass (FM), fat-free mass, resting energy expenditure (REE), respiratory quotient (RQ), blood pressure, fasting plasma glucose and serum insulin, total cholesterol (TC), low- and high-density lipoprotein-cholesterol (LDL-C and HDL-C) and triglycerides (TGs) were measured at baseline and 26 weeks.
Results:
A total of 87 subjects completed the study. After 26 weeks, compared with the placebo group, the MMS group had significantly lower BW, BMI, FM, TC and LDL-C, significantly higher REE and HDL-C, as well as a borderline significant trend of lower RQ (P=0.053) and WC (P=0.071). The calcium group also had significantly higher HDL-C and lower LDL-C levels compared with the placebo group.
Conclusion:
The results suggest that, in obese individuals, multivitamin and mineral supplementation could reduce BW and fatness and improve serum lipid profiles, possibly through increased energy expenditure and fat oxidation. Supplementation of calcium alone (162 mg per day) only improved lipid profiles.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
National Task Force on the Prevention and Treatment of Obesity. Overweight obesity health risk. Arch Intern Med 2000; 160: 898–904.
World Health Organization. Obesity and Overweight Available at: http://www.who.int/dietphysicalactivity/publications/facts/obesity/en/ (accessed 13 May 2009).
Cheng TO . The current state of cardiology in China. Int J Cardiol 2004; 96: 425–439.
Li LM, Rao KQ, Kong LZ, Yao CH, Xiang HD, Zai FY et al. A description on the Chinese national nutrition and health survey in 2002. Chin J Epidemiol 2005; 26: 478–484.
Mokdad AH, Ford ES, Bowman BA, Dietz WH, Vinicor F, Bales VS et al. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA 2003; 289: 76–79.
Zemel MB . Nutritional and endocrine modulation of intracellular calcium: implications in obesity, insulin resistance and hypertension. Mol Cell Biochem 1998; 188: 129–136.
Albarracin C, Fuqua B, Geohas J, Juturu V, Finch MR, Komorowski JR . Combination of chromium and biotin improves coronary risk factors in hypercholesterolemic type 2 diabetes mellitus: a placebo-controlled, double-blind randomized clinical trial. J Cardiometab Syndr 2007; 2: 91–97.
Maccubbin D, Bays HE, Olsson AG, Elinoff V, Elis A, Mitchel Y et al. Lipid-modifying efficacy and tolerability of extended-release niacin/laropiprant in patients with primary hypercholesterolaemia or mixed dyslipidaemia. Int J Clin Pract 2008; 62: 1959–1970.
Lim HJ, Choi YM, Choue R . Dietary intervention with emphasis on folate intake reduces serum lipids but not plasma homocysteine levels in hyperlipidemic patients. Nutr Res 2008; 28: 767–774.
Kumar MV, Sunvold GD, Scarpace PJ . Dietary vitamin A supplementation in rats: suppression of leptin and induction of UCP1 mRNA. J Lipid Res 1999; 40: 824–829.
Sun CH, Sun WG, Fu RX, Yu XF . The effect of iron on the expression of uncoupling protein gene in skeletal muscle of obese rats. Acta Nutr Sinica 2003; 25: 344–348.
Wang HY, Sun CH, Zhou XR, Song SL, Jiang LY . Mechanism of dietary calcium on reducing body weight of obese rats induced by diets. Chin J Public Health 2004; 20: 1046–1047.
Ames BN, Atamna H, Killilea DW . Mineral and vitamin deficiencies can accelerate the mitochondrial decay of aging. Mol Aspects Med 2005; 26: 363–378.
Kaidar-Person O, Person B, Szomstein S, Rosenthal RJ . Nutritional deficiencies in morbidly obese patients: a new form of malnutrition? Part A: vitamins. Obes Surg 2008; 18: 870–876.
Kaidar-Person O, Person B, Szomstein S, Rosenthal RJ . Nutritional deficiencies in morbidly obese patients: a new form of malnutrition? Part B: minerals. Obes Surg 2008; 18: 1028–1034.
Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF . Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr 2000; 72: 690–693.
Aasheim ET, Hofso D, Hjelmesaeth J, Birkeland KI, Bohmer T . Vitamin status in morbidly obese patients: a cross-sectional study. Am J Clin Nutr 2008; 87: 362–369.
Nachtigal MC, Patterson RE, Stratton KL, Adams LA, Shattuck AL, White E . Dietary supplements and weight control in a middle-age population. J Altern Complement Med 2005; 11: 909–915.
Jiang LY, Sun CH, Zhou XR, Wang HY, Ren LN . Effect of dietary mineral nutrients and vitamins on metabolism of rat fed with high fat. Wei Sheng Yan Jiu 2004; 33: 447–449.
Cooperative Meta-Analysis Group of China Obesity Task Force. Predictive values of body mass index and waist circumference to risk factors of related diseases in Chinese adult population. Chin J Epidemiol 2002; 23: 5–10.
Chinese Nutrition Society. Chinese Dietary Reference Intakes. China Light Industry Press: Peking, China, 2002. p 15.
Hao L, Li Z, Willett W . The method of food frequency questionnaire. The reproducibility and validity of FFQ. In: Willett W, Elizabeth L (eds) Nutritional Epidemiology (Translation). People’s Medical Publishing House: Peking, China, 2006. pp 69–142.
Friedewald WT, Levy RI, Fredrickson DS . Estimation of the concentration of low-density lipoprotein cholesterol in plasma without use of preparative ultracentrifuge. Clin Chem 1972; 18: 499–502.
Sun CH, Yu XF, Li Y, Liu R, Wang HY . Effects of dietary calcium on the blood glucose, blood lipid and hormone of rat fed a high fat diet. J Hygiene Res 2004; 33: 164–166.
Major GC, Doucet E, Jacqmain M, St-Onge M, Bouchard C, Tremblay A . Multivitamin and dietary supplements, body weight and appetite: results from a cross-sectional and a randomized double-blind placebo-controlled study. Br J Nutr 2008; 99: 1157–1167.
Costford SR, Chaudhry SN, Salkhordeh M, Harper ME . Effects of the presence, absence, and overexpression of uncoupling protein-3 on adiposity and fuel metabolism in congenic mice. Am J Physiol Endocrinol Metab 2006; 290: E1304–E1312.
Schrauwen P, Hesselink M . UCP2 and UCP3 in muscle controlling body metabolism. J Exp Biol 2002; 205: 2275–2285.
Tanaka T, Sohmiya K, Kono T, Terasaki F, Horie R, Ohkaru Y et al. Thiamine attenuates the hypertension and metabolic abnormalities in CD36-defective SHR: uncoupling of glucose oxidation from cellular entry accompanied with enhanced protein O-GlcNAcylation in CD36 deficiency. Mol Cell Biochem 2007; 299: 23–35.
Dakshinamurti K, Paulose CS, Viswanathan M . Vitamin B6 and hypertension. Ann N Y Acad Sci 1990; 575: 241–249.
Hornig B, Arakawa N, Kohler C, Drexler H . Vitamin C improves endothelial function of conduit arteries in patients with chronic heart failure. Circulation 1998; 97: 363–368.
Hatton DC, McCarron DA . Dietary calcium and blood pressure in experimental models of hypertension. Hypertension 1994; 4: 513–530.
Barbagallo M, Dominguez LJ, Galioto A, Ferlisi A, Cani C, Malfa L et al. Role of magnesium in insulin action, diabetes and cardio-metabolic syndrome X. Mol Aspects Med 2003; 24: 39–52.
Singh RB, Niaz MA, Rastogi SS, Bajaj S, Gaoli Z, Shoumin Z . Current zinc intake and risk of diabetes and coronary artery disease and factors associated with insulin resistance in rural and urban populations of North India. J Am Coll Nutr 1998; 17: 564–570.
Camastra S, Manco M, Mari A, Baldi S, Gastaldelli A, Greco AV et al. Beta-cell function in morbidly obese subjects during free living: long-term effects of weight loss. Diabetes 2005; 54: 2382–2389.
Volek JS, Gómez AL, Love DM, Weyers AM, Hesslink JR, Wise JA et al. Effects of an 8-week weight-loss program on cardiovascular disease risk factors and regional body composition. Eur J Clin Nutr 2002; 56: 585–592.
Acknowledgements
This study was supported by a grant from the Natural Science Foundation of China (30771804). We thank the researchers and medical personnel of Harbin Medical University for their efforts and collaboration in this study. Professor Chang-Hao Sun was responsible for the conception, design and data interpretation of the study and is the principal investigator of the grant for the study; Ying Li and Cheng Wang were responsible for data collection, data analysis, data interpretation and writing of this paper; Kun Zhu was responsible for data interpretation and writing of this paper; Ren-Nan Feng was responsible for performing clinical procedures, data collection and writing of this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Li, Y., Wang, C., Zhu, K. et al. Effects of multivitamin and mineral supplementation on adiposity, energy expenditure and lipid profiles in obese Chinese women. Int J Obes 34, 1070–1077 (2010). https://doi.org/10.1038/ijo.2010.14
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2010.14
Keywords
This article is cited by
-
The effect of prepregnancy body mass index on maternal micronutrient status: a meta-analysis
Scientific Reports (2021)
-
Acute and chronic effects of multivitamin/mineral supplementation on objective and subjective energy measures
Nutrition & Metabolism (2020)
-
Effects of school-based physical activity and multi-micronutrient supplementation intervention on growth, health and well-being of schoolchildren in three African countries: the KaziAfya cluster randomised controlled trial protocol with a 2 × 2 factorial design
Trials (2020)
-
Multivitamins and minerals modulate whole-body energy metabolism and cerebral blood-flow during cognitive task performance: a double-blind, randomised, placebo-controlled trial
Nutrition & Metabolism (2016)
-
Effects of Zinc supplementation on serum lipids: a systematic review and meta-analysis
Nutrition & Metabolism (2015)