Abstract
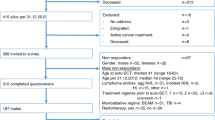
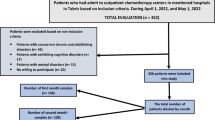
Chronic hepatitis C (CHC) patients often have altered quality of life. Few data are available about sexual impairment (SI) in CHC. From 2011 to 2013, we included consecutive CHC outpatients. Exclusion criteria were: antiviral therapy, co-infection, age <18 or >75, transplantation, alcohol consumption, Eastern Cooperative Oncology Group >1. Non-CHC subjects were healthy blood donors. Sexual questionnaires for men and women were adapted from the International Index of Erectile Function and Female Sexual Function Index, respectively, and concerned the past 30 days. Two hundred eighty-one patients were compared with 1086 blood donors. SI was more frequent in CHC patients. Men with CHC had worse desire, confidence, erections, climax and satisfaction (P<0.001). Women with CHC had worse desire, arousal, climax, satisfaction, lubrication and comfort (P<0.001). In multivariate analysis, factors associated with SI in men were CHC (odds ratio (OR)=4.45, 95% confidence interval (CI) 2.46–8.06), age (OR=1.06, 95% CI 1.03–1.09), no intercourse (OR=8.74, 95% CI 4.65–16.04) and unemployment (OR=2.14, 95% CI 1.16–3.95). Factors associated with a worse global sexual life in women were CHC (OR=7.96, 95% CI 4.07–15.58) and no intercourse (OR=21.39, 95% CI 11.03–41.48). The study results were corroborated by propensity score-matching analysis. Sexual life is impaired in men and women with CHC. In clinical practice, sexual quality of life should be evaluated and treated.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Soykan A, Boztas H, Idilman R, Ozel ET, Tuzun AE, Ozden A et al. Sexual dysfunctions in HCV patients and its correlations with psychological and biological variables. Int J Impot Res 2005; 17: 175–179.
Laumann EO, Paik A, Rosen RC . Sexual dysfunction in the United States: prevalence and predictors. JAMA 1999; 281: 537–544.
Ferri C, Bertozzi MA, Zignego AL . Erectile dysfunction and hepatitis C virus infection. JAMA 2002; 288: 698–699.
Danoff A, Khan O, Wan DW, Hurst L, Cohen D, Tenner CT et al. Sexual dysfunction is highly prevalent among men with chronic hepatitis C virus infection and negatively impacts health-related quality of life. Am J Gastroenterol 2006; 101: 1235–1243.
NIH Consensus Conference. Impotence. NIH Consensus Development Panel on Impotence. JAMA 1993; 270: 83–90.
Bacon CG, Mittleman MA, Kawachi I, Giovannucci E, Glasser DB, Rimm EB . Sexual function in men older than 50 years of age: results from the health professionals follow-up study. Ann Intern Med 2003; 139: 161–168.
Braun M, Wassmer G, Klotz T, Reifenrath B, Mathers M, Engelmann U . Epidemiology of erectile dysfunction: results of the 'Cologne Male Survey'. Int J Impot Res 2000; 12: 305–311.
Nicolosi A, Glasser DB, Moreira ED, Villa M . Prevalence of erectile dysfunction and associated factors among men without concomitant diseases: a population study. Int J Impot Res 2003; 15: 253–257.
Dove LM, Rosen RC, Ramcharran D, Wahed AS, Belle SH, Brown RS et al. Decline in male sexual desire, function, and satisfaction during and after antiviral therapy for chronic hepatitis C. Gastroenterology 2009; 137: 873–884, 884 e871.
Huyghe E, Kamar N, Wagner F, Capietto AH, El-Kahwaji L, Muscari F et al. Erectile dysfunction in end-stage liver disease men. J Sex Med 2009; 6: 1395–1401.
Gomez-Lobo V, Burgansky A, Kim-Schluger L, Berkowitz R . Gynecologic symptoms and sexual function before and after liver transplantation. J Reprod Med 2006; 51: 457–462.
Parolin MB, Rabinovitch I, Urbanetz AA, Scheidemantel C, Cat ML, Coelho JC . Impact of successful liver transplantation on reproductive function and sexuality in women with advanced liver disease. Transplant Proc 2004; 36: 943–944.
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A . The International Index of Erectile Function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 1997; 49: 822–830.
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R et al. The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 2000; 26: 191–208.
R Core Team 2014 R: a language and environment for statistical computing. R Foundation for Statistical Computing V, Austria. http://www.R-project.org/.
Acknowledgements
We thanks all the patients and blood donors who agreed to fill the questionnaire and to have their data analyzed, the whole team of the Etablissement Français du Sang of Bordeaux, France, and Janssen-Cilag Company, who funded this study.
Author contributions
Julien Vergniol: study concept and design, acquisition and management of data, statistical analysis and interpretation of results, drafting of the manuscript, statistical analysis. Sophie Duc: statistical analysis. Geneviève Hou: healthy blood donors recruitment and technical support. Jean-Baptiste Hiriart: acquisition of data and technical support. Juliette Foucher: acquisition of data and technical support. Florence Chenus: healthy blood donors recruitment and technical support. Carole Fabères: acquisition of data and technical support. Faiza Chermak: acquisition of data and technical support. Aude Lafournière: acquisition of data and technical support. Noui Souakri: acquisition of data and technical support. Victor de Lédinghen: study concept and design, statistical analysis, and study supervision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Victor de Lédinghen is a member of the Advisory board of BMS, MSD, Gilead, Janssen and Abbvie. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Vergniol, J., Duc, S., Hou, G. et al. Sexual quality of life is impaired in patients with chronic hepatitis C. Int J Impot Res 28, 68–73 (2016). https://doi.org/10.1038/ijir.2016.5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2016.5