Abstract
DNA damage occurs more often in hypertensive patients than in non-hypertensive individuals. We sought to investigate lymphocyte DNA damage and total antioxidant status (TAS) levels in patients with dipper hypertension (DH) and non-dipper hypertension (NDH). Thirty-three patients with NDH (NDH group), 31 patients with DH (DH group) and 20 healthy volunteers (control group) were included in the study. Measurements from ambulatory blood pressure monitoring were obtained for all subjects. DNA damage was assessed in peripheral lymphocytes by comet assay, and plasma TAS levels were determined using an automated measurement method. The mean DNA damage value of the NDH group was higher than that of both the DH and control groups (P=0.002 and P<0.001, respectively). The mean DNA damage value of the DH group was higher than that of the control group (P<0.001). The mean TAS level of the NDH group was lower than that of both the DH and control groups (P=0.001 and P<0.001, respectively), and the mean TAS level of the DH group was lower than that of the control group (P<0.001). DNA damage was negatively associated with TAS level (r=−0.692, P<0.001) and positively associated with high sensitive c-reactive protein level (r=0.315, P=0.012). DNA damage increased in the NDH group compared with both the DH group and control group. This condition may be related to increased oxidative stress in the NDH group compared with the DH and control groups.
Similar content being viewed by others
Introduction
The incidence of atherosclerotic cardiovascular disease is strongly related to the elevation of blood pressure (BP).1 In hypertensive patients, BP is characterized by rhythm alterations over 24 h periods.2 It has been shown that 24 h ambulatory BP monitoring (ABPM) is a better predictor of subsequent complications than spot measurements of BP.3
ABPM has shown that BP is highest during the day and lowest at night in both normotensives and hypertensives.4 Mean BP values are 10–20% lower at night than in the day. This condition is called ‘dipper’ change. However, in some hypertensives, in contrast to this normal change, nighttime BP lowering does not occur or shows a decrease of <10%, which is called ‘non-dipper’ change.5 Endothelial dysfunction and target organ injury are more severe in non-dipper hypertensive (NDH) patients than in dipper hypertensive (DH) patients, and NDH itself is a risk factor for increased mortality.6, 7, 8, 9
Increased oxidative stress is known to be involved in the pathogenesis of hypertension (HT) and cardiovascular disease.10, 11, 12, 13 Oxidative stress occurs when the level of reactive oxygen species (ROS) exceeds the level of the antioxidant defense systems.13 Previous studies have shown that patients with essential HT have a decreased antioxidant capacity and increased amounts of ROS.14, 15 The effects of ROS on vascular function and the development of HT have been investigated previously.10, 11 Superoxide rapidly inactivates endothelium-derived nitric oxide.12, 16, 17 Thus, oxidative stress may account for endothelial dysfunction in patients with HT.18
DNA damage frequently occurs in cells exposed to oxidative stress. Increased oxidative stress may initiate lipid peroxidation in cell membranes, damage membrane proteins or cause DNA fragmentation.19, 20, 21 DNA damage caused by ROS occurs more often in hypertensive patients than normotensive patients.22 The measurement of DNA damage in lymphocytes is a valuable marker of oxidative stress.21, 23 In this study, we sought to investigate lymphocyte DNA damage in patients with DH and NDH.
Methods
Subjects
The overall study population consisted of 64 consecutive patients: 33 subjects with NDH (NDH group) and 31 patients with DH (DH group). Twenty healthy volunteers were also included in the study as a control group. The study patients had newly diagnosed, untreated mild to moderate HT. The inclusion criteria were being 18–55 years of age and, for women, having a regular menstrual cycle. The control group had multiple BP measurements <140/90 mm Hg over the 1-month period and were in the same age and gender range as the hypertensive patients. These subjects were non-medical staff from our hospital or their relatives. For inclusion in the control group, subjects had to have no known coronary risk factors or cardiac symptoms and normal electrocardiographic and echocardiographic examinations.
Exclusion criteria included the presence of neoplastic disease, recent major surgical procedures, dyslipidemia, concomitant inflammatory diseases such as infections and autoimmune disorders, liver and kidney disease, extreme-dipper type HT, use of regular medication for any reason, alcohol use and smoking habit. Patients suffering from organic coronary artery disease, vasospastic angina, heart failure, idiopathic hypertrophic and dilated cardiomyopathy, secondary and malignant HT, serum creatinine>1.5 mg dl−1 or with a history of diabetes were also excluded from participation in the study. Subjects had not previously taken antihypertensive therapy. Subjects using any vasoactive drug and having ST segment or T-wave changes specific for myocardial ischemia, Q waves or incidental left bundle branch block on ECG were excluded from the study.
The study was conducted according to the recommendations set forth by the Declaration of Helsinki on Biomedical Research Involving Human Subjects. The Institutional Ethics Committee approved the study protocol, and each participant provided written, informed consent.
BP measurement and ABPM
BP was measured using a mercury sphygmomanometer in an office setting. Systolic BP (SBP) and diastolic BP (DBP) were taken. Noninvasive 24 h ABPM was performed with a portable, compact digital recorder (Tracker NIBP2, Delmar Reynolds Ltd., Hertford, UK) and analyzed using customized analytical software (Delmar Reynolds Medical Inc., Model 2169, Hertford, UK). All subjects wore an ABPM device for a single 24 h period. The device was programmed to inflate and record BP at pre-specified intervals (every 15 min during daytime hours and every 30 min during nighttime hours), which provided ∼80 BP recordings during the 24 h period. The display of the ABPM was inactivated so that viewing each BP reading did not distract the subjects. For the analysis of the data reports, reports generated from a session of ABPM contained BP recordings for the entire 24 h, heart rate, mean arterial pressure and BP load, as well as summary statistics for the overall 24 h, daytime and nighttime periods. When the readings exceeded at least 80% of the total readings programmed for the testing period, the recording was considered valid and satisfactory.
Diagnosis of HT
In each subject, BP was measured on at least three separate days after 15 min of sitting comfortably and was then averaged. Each subject then underwent 24 h ABPM. Individuals who had SBP ⩾140 mm Hg and/or a DBP ⩾90 mm Hg in the office setting, and in ABPM, an average 24 h SBP>130 mm Hg and/or DBP >80 mm Hg, an average daytime SBP >135 mm Hg and/or DBP >85 mm Hg or an average nighttime SBP >125 mm Hg and/or DBP >75 mm Hg were diagnosed as hypertensive.24 In addition, the subjects who had a <10% reduction in BP from the daytime to the nighttime period were defined as NDH, and the subjects who had a BP reduction ⩾10% from the daytime to the nighttime period were considered DH.5
Blood sampling protocol
After the HT diagnosis based on ABPM, peripheral venous blood samples were taken into heparinized tubes from all subjects in a fasting state between 0700 and 0800 hours. One milliliter of blood was immediately pipetted into another tube to measure DNA damage. The remaining blood was centrifuged at 3000 r.p.m. for 10 min for plasma separation. Plasma samples were stored at −80 °C until the analysis of total antioxidant status (TAS), hsCRP, triglyceride, total cholesterol, low-density lipoprotein, high-density lipoprotein and fasting glucose. hsCRP levels were measured with an otoanalyser (Aeroset, Abbott, Holliston, MN, USA) using a commercial spectrophotometric kit (Scil Diagnostics GmbH, Sunnyvale, CA, USA).
DNA Damage determination by alkaline comet assay
Lymphocyte isolation for the comet assay was performed using Histopaque 1077 (Sigma Chemical Co. Ltd., Seoul, Korea). One milliliter of heparinized blood was carefully layered over 1 ml histopaque and centrifuged for 35 min at 500 g at 25 °C. The interface bands containing lymphocytes were washed with phosphate-buffered saline and then collected by 15 min centrifugation at 400 g. The resulting pellets were re-suspended in phosphate-buffered saline to obtain 20 000 cells in 10 μl. Membrane integrity was assessed by means of the trypan blue exclusion method.
The endogenous lymphocytes’ DNA damage was analyzed by alkaline comet assay according to the procedures outlined by Singh et al.,25 with minor modifications. Ten microliters of fresh lymphocyte cell suspension (around 20 000 cells) was mixed with 80 μl of 0.7% low-melting-point agarose (Sigma-Aldrich, St Louis, MO, USA) in phosphate-buffered saline at 37 °C. Subsequently, 80 μl of this mixture was layered onto slides that had previously been coated with 1.0% hot (60 °C) normal-melting-point agarose and covered with a coverslip at 4 °C for at least 5 min to allow the agarose to solidify. After removing the coverslips, the slides were submerged in freshly prepared, cold (4 °C) lysing solution (2.5 M NaCl, 100 mM EDTA-2Na; 10 mM Tris–HCl, pH 10–10.5; 1% Triton X-100 and 10% DMSO added just before use) for at least 1 h. Slides were then immersed in freshly prepared, alkaline electrophoresis buffer (0.3 mol l−1 NaOH and 1 mmol l−1 Na2 EDTA, pH>13) at 4 °C for unwinding (40 min) and then electrophoresed (25 V/300 mA, 25 min). All of the above steps were conducted under red light or without direct light to prevent additional DNA damage. After electrophoresis, the slides were stained with ethidium bromide (2 μg ml−1 in distilled H2O; 70 μl per slide), covered with a coverslip and analyzed using a fluorescence microscope (Nikon, Tokyo, Japan) equipped with a rhodamine filter, using the epi-flurescence method. The images of 100 randomly chosen nuclei (50 cells from each of two replicate slides) were visually analyzed. Each image was classified according to the intensity of the fluorescence in the comet tail and was given a value of 0, 1, 2, 3 or 4 (from undamaged class 0 to maximally damaged class 4) (Figure 1) so that the total scores of the slide were between 0 and 400 arbitrary units. All procedures were completed by the same biochemistry staff, and DNA damage was detected by a single observer who was not aware of the subjects’ diagnoses.
Measurement of TAS
TAS of serum was determined using an automated measurement method.26 In this method, hydroxyl radical is produced. In the assay, ferrous ion solution, which is present in reagent 1, is mixed with hydrogen peroxide, which is present in reagent 2. The sequentially produced radicals, such as the brown-colored dianisidinyl radical cation produced by the hydroxyl radical, are also potent radicals. In this assay, the antioxidative effect of the sample against the potent free radical reactions is measured. The assay has excellent precision values, which are lower than 3%. The results are expressed as mmol Trolox equivalents per l.
Statistical analysis
Results are presented as mean±s.d. or frequency expressed as a percent. Categorical variables were compared using the χ2-test. For continuous variables, differences between two groups were assessed using the unpaired t-test. Comparisons among multiple groups were performed by one-way analysis of variance test for continuous variables. Associations between other variables and lymphocyte DNA damage properties were assessed by the Pearson’s correlation coefficient. A P-value <0.05 was considered statistically significant.
Results
Demographic and clinical characteristics
The demographic and clinical characteristics of the groups are shown in Table 1. The SBP and DBP in the office setting were similar in DH and NDH subjects. The SBP and DBP of both the DH and NDH groups in the office setting were higher than those of the control group.
ABPM analysis
The measurements from ABPM are shown in Table 2. By definition, the average daytime SBP and DBP did not differ between non-dippers and dippers. In contrast, the average nighttime SBP and DBP were significantly higher in the non-dipper HT group than in the dipper group or the control group.
Analysis of antioxidant status and DNA damage
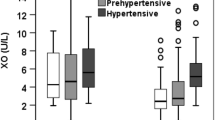
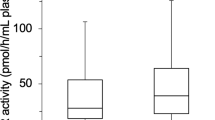
The mean DNA damage values and hsCRP levels were higher in the NDH group than in the DH group or the control group. Additionally, the mean DNA damage value of the NDH group was higher than that of the DH group (P<0.001). The mean TAS levels of both the DH and NDH groups were lower than that of the control group (P<0.001, for both). The mean TAS level of the NDH group was also lower than that of the DH group (P<0.001). The analyses of antioxidant status and DNA damage are shown in Table 3.
Correlation analysis
In the patient groups, lymphocyte DNA damage was negatively correlated with TAS level (r=−0.692, P<0.001), whereas lymphocyte DNA damage was positively correlated with age (r=0.479, P<0.001), hsCRP level (r=0.315, P=0.012), total cholesterol level (r=0.382, P=0.002), low-density lipoprotein cholesterol level (r=0.331, P=0.008), average night-time SBP (r=0.260, P=0.038) and average nighttime DBP (r=0.258, P=0.039) in the bivariate analysis Table 4.
Discussion
To the best of our knowledge, the present study is the first in to evaluate lymphocyte DNA damage and TAS in patients with DH and NDH. The main findings of this study are the following:1 the mean lymphocyte DNA damage and hsCRP levels of all patient groups were higher than those of the control group;2 the mean lymphocyte DNA damage and hsCRP levels were higher in the NDH group than the DH group;3 the mean TAS levels of both the NDH and DH groups were lower than that of the control group; and the mean TAS levels of the NDH group were lower than those of the DH group;4 lymphocyte DNA damage was negatively correlated with TAS and positively correlated with hsCRP.
Previous studies have shown that left ventricular hypertrophy, the risk of cardiovascular mortality,6, 7 silent cerebrovascular disease8 and the progression of nephropathy9 are greater in subjects with non-dipper BP than in patients with dipper BP.6, 7, 8, 9 At the same time, endothelium-dependent vasodilation induced by acetylcholine is impaired and the production of nitric oxide is reduced to a greater extent in non-dippers than in dippers.9
In the present study, lymphocyte DNA damage increased in hypertensive patients. This result is consistent with that of a previous study by Subash et al.22 They reported that increased DNA damage was related to a decreased TAS level. However, in that study, lymphocyte DNA damage was not investigated separately in patients with NDH and DH.22 In our study, the extent of lymphocyte DNA damage was greater in the NDH group than in the DH group.
DNA damage frequently occurs in cells exposed to oxidative stress. Increased oxidative status may initiate lipid peroxidation in cell membranes, damage membrane proteins, or cause DNA fragmentation.27 Antioxidant systems prevent the damage of DNA.9 Honda et al.28 have also reported that reduced activity of antioxidant enzymes is associated with increased levels of oxidative DNA damage. In the present study, lymphocyte DNA damage was significantly negatively correlated with TAS level. Thus, increased lymphocyte DNA damage in patients with NDH can be explained by decreased TAS levels, which are a marker of increased oxidative stress.
Lymphocyte DNA damage is one of the more reliable markers of oxidative stress. The most widely used techniques to investigate DNA damage are the comet assay and measurement of 7-hydroxy-8-oxo-2V-deoxyguanosine (8-oxodG). The comet assay detects single-stranded breaks in DNA.29, 30 8-oxodG can be measured by using several chromatographic techniques or non-chromatographic enzymic methods. There is a large variation in the measured levels of 8-oxodG between these assays, partly because 8-oxodG is artificially generated in these assays;31 however, either approache can be used.30 In this study, to detect DNA damage in lymphocytes, we used the comet assay, which is a cheap, simple and very sensitive method.32
Maeda et al.33 demonstrated that oxidative stress generated by peripheral blood mononuclear cells was increased in hypertensives with an extreme-dipper pattern and/or a morning surge in BP. Recently, Ermis et al.34 investigated serum GGT levels, a marker of oxidative stress, and inflammatory activity in patients with DH and NDH and found that both serum GGT and CRP levels were increased in patients with NDH. They also reported that increased GGT activity was correlated with CRP levels. Yildiz et al.35 also showed increased signs of oxidative stress in patients with NDH compared with DH. Decreased antioxidant levels have been interpreted as evidence of increased oxidative stress. Additionally, the plasma TAS level is an accurate index of oxidative stress, which provides a measure of the total plasma defenses against ROS.22, 36 In the present study, we showed increased hsCRP levels and reduced TAS levels, a marker of increased oxidative stress, in the NDH group. It has been shown that increased pressure on vascular walls can induce ROS release and increase the level of oxidative stress.37, 38, 39 In the present study, the nocturnal SBP was higher in non-dippers than in dippers. Higher nocturnal BP may represent the primary mechanism of increased oxidative stress in patients with NDH. Thus, increased lymphocyte DNA damage in patients with NDH can be explained by increased oxidative stress.
Study limitations
The comet assay is ideally suited for human investigations and can be easily applied. Normally, the lymphocytes that are used do not require tissue disaggregation, as they are obtained in a relatively noninvasive way, and they behave well in the comet assay. However, lymphocytes may not adequately reflect the damage to other organs in human subjects.32, 40 Sometimes, human tissue removed at surgery can be investigated for elevated levels of damage; however, the necessary control tissue from healthy individuals is more difficult to obtain. In this study, we chose to use freshly isolated lymphocytes.
The lymphocyte DNA damage score in healthy control groups varies between 7.6 and 19.9 arbitrary units in the literature.41, 42, 43 This indicates that DNA damage evaluated by comet assay may vary depending on physicians and/or experimental conditions at measurement, such as pH, duration of alkaline treatment, length of electrophoresis or types of cells used in single-cell gel electrophoresis.44 The optimization of experimental parameters for measuring lymphocyte DNA damage in the comet assay is necessary. In addition, there is no universally accepted cutoff value for the lymphocyte DNA damage score. To limit the variance, the lymphocyte DNA damage score can be confirmed by measuring 8-oxodG in patients with DH and NDH. However, the comet assay is a well-established, simple and sensitive method for measuring DNA damage and is commonly used in human trials.44 In this study, lymphocyte DNA damage was measured by alkaline comet assay, following the method of Singh et al.25
In conclusion, lymphocyte DNA damage increased in patients with NDH compared with patients with DH and the control group. The increased lymphocyte DNA damage, reduced TAS levels and increased hsCRP levels in patients with NDH might reflect increased oxidative stress and inflammatory activity, which have a crucial role in the development of cardiovascular disease. Lymphocyte DNA damage may be a parameter to consider in the treatment of HT.
References
Stokes J, Kannel WB, Wolf PA, D’Agostino RB, Cupples LA . Blood pressure as a risk factor for cardiovascular disease. The Framingham Study—30 years of follow-up. Hypertension 1989; 13: 113–118.
O’Brien ET, Murphy J, Tyndall A, Atkins N, Mee F, McCarthy G, Staessen J, Cox J, O’Mally K . Twenty-four-hour ambulatory blood pressure in men and women aged 17 to 80 years: the Allied Irish Bank Study. J Hypertens 1991; 9: 355–360.
Staessen JA, Thijs L, Fagard R, O’Brien ET, Clement D, de Leeuw PW, Mancia G, Nachev C, Palatini P, Parati G, Tuomilehto J, Webster J . Predicting cardiovascular risk using conventional vs ambulatory blood pressure in older patients with systolic hypertension: systolic hypertension in Europe trial investigators. JAMA 1999; 282: 539–546.
Mancia G, Ferrari A, Gregorini L, Parati G, Pomidossi G, Bertinieri G, Grassi G, di Rienzo M, Pedotti A, Zanchetti A . Blood pressure and heart rate variabilities in normotensive and hypertensive human beings. Circ Res 1983; 53: 96–104.
Verdecchia P, Schillaci G, Porcellati C . Dippers versus non-dippers. J Hypertens 1991; 9: 42–48.
Yamamoto Y, Akiguchi I, Oiwa K, Hayashi M, Kimura J . Adverse effect of nighttime blood pressure on the outcome of lacunar infarct patients. Stroke 1998; 29: 570–576.
Ohkubo T, Imai Y, Tsuji I, Nagai K, Watanabe N, Minami N, Kato J, Kikuchi N, Nishiyama A, Aihara A, Sekino M, Satoh H, Hisamichi S . Relation between nocturnal decline in blood pressure and mortality. The Ohasama Study. Am J Hypertens 1997; 10: 1201–1207.
Timio M, Venanzi S, Lolli S, Lippi G, Verdura C, Monarca C, Guerrini E . ‘Non-dipper’ hypertensive patients and progressive renal insufficiency: a 3-year longitudinal study. Clin Nephrol 1995; 43: 382–387.
Higashi Y, Nakagawa K, Kimura M, Noma K, Hara K, Sasaki S, Goto C, Oshima T, Chayama K, Yoshizumi M . Circadian variation of blood pressure and endothelial function in patients with essential hypertension:a comparison of dippers and non-dippers. J Am Coll Cardiol 2002; 40: 2039–2043.
Lassègue B, Griendling K . Reactive oxygen species in hypertension. An update. Am J Hypertens 2004; 17: 852–860.
Touyz RM, Schiffrin EL . Reactive oxygen species in vascular biology: implications in hypertension. Histochem Cell Biol 2004; 122: 339–352.
Rodrigo R, Prat H, Passalacqua W, Araya J, Guichard C, Bächler JP . Relationship between oxidative stress and essential hypertension. Hypertens Res 2007; 30: 1159–1167.
Park YK, Lee SH, Park E, Kim JS, Kang MH . Changes in antioxidant status, blood pressure, and lymphocyte DNA damage from grape juice supplementation. Ann NY Acad Sci 2009; 1171: 385–390.
Russo C, Olivieri O, Girelli D, Faccini G, Zenari ML, Lombardi S, Corrocher R . Anti-oxidant status and lipid peroxidation in patients with essential hypertension. J Hypertens 1998; 16: 1267–1271.
Prabha PS, Das UN, Koratkar R, Sagar PS, Ramesh G . Free radical generation, lipid peroxidation and essential fatty acids in uncontrolled essential hypertension. Prostaglandins Leukot Essent Fatty Acids 1990; 41: 27–33.
Dusting GJ, Akita K, Hickey H, Smith M, Gurevich V . Cyclosporin A and tacrolimus (FK506) suppress expression of inducible nitric oxide synthase in vitro by different mechanisms. Br J Pharmacol 1999; 128: 337–344.
Zicha J, Dobesova Z, Kunes J . Relative deficiency of nitric oxide-dependent vasodilation in salt-hypertensive Dahl rats: the possible role of superoxide anions. J Hypertens 2001; 19: 247–254.
John S, Schmieder RE . Potential mechanisms of impaired endothelial function in arterial hypertension and hypercholesterolemia. Curr Hypertens Rep 2003; 5: 199–207.
Harangi M, Remenyik EE, Seres I, Varga Z, Katona E, Paragh G . Determination of DNA damage induced by oxidative stress in hyperlipidemic patients. Mutat Res 2002; 513: 17–25.
Halliwell B, Aruoma O . DNA damage by oxygen-derived species: its mechanism and measurement in mammalian systems. FEBS Lett 1991; 281: 9–19.
Gedik CM, Boyle SP, Wood SG, Vaughan NJ, Collins AR . Oxidative stress in humans: validation of biomarkers of DNA damage. Carcinogenesis 2002; 23: 1441–1446.
Subash P, Premagurumurthy K, Sarasabharathi A, Cherian KM . Total antioxidant status and oxidative DNA damage in a South Indian population of essential hypertensives. J Hum Hypertens 2010; 24: 475–482.
Collins AR, Olmedilla B, Southon S, Granado F, Duthie SJ . Serum carotenoids and oxidative DNA damage in human lymphocytes. Carcinogenesis 1998; 19: 2159–2162.
Stergiou GS, Salgami EV . World Health Organization-International Society of Hypertension (WHO-ISH); USA Joint National Committee on prevention, detection, evalutiaon, and treatment of high blood pressure (JNC-7); European Soceity of Hypertension-European Society of Cardiology (ESH-ESC). New European, American and International guidelines for hypertension management: agreement and disagreement. Expert Rev Cardiovasc Ther 2004; 2: 359–368.
Singh PN, McCoy MT, Tice RR, Schneider EL . A simple technique for quantitation of low levels of DNA damage in individual cells. Exp Cell Res 1988; 175: 184–191.
Erel O . A novel automated method to measure total antioxidant response against potent free radical reactions. Clin Biochem 2004; 37: 112–119.
Chen LY, Nichols WW, Hendricks J, Mehta JL . Myocardial neutrophil infiltration, lipid peroxidation, and antioxidant activity after coronary artery thrombosis and thrombolysis. Am Heart J 1995; 129: 211–218.
Honda M, Yamada Y, Tomonaga M, Ichinose H, Kamihira S . Correlation of urinary 8-hydroxy-2-de-oxyguanosine (8-OHdG), a biomarker of oxidative DNA damage, and clinical features of hematological disorders: a pilot study. Leuk Res 2000; 24: 461–468.
Collins AR, Dusinska M, Gedik CM, Stetina R . Oxidative damage to DNA: do we have a reliable biomarker? Environ Health Perspect 1996; 4: 465–469.
Gedik CM, Wood SG, Collins AR . Measuring oxidative damage to DNA; HPLC and the comet assay compared. Free Radic Res 1998; 29: 609–615.
Møller P, Loft S . Oxidative DNA damage in human white blood cells in dietary antioxidant intervention studies. Am J Clin Nutr 2002; 76: 303–310.
Collins AR . The comet assay for DNA damage and repair: principles, applications, and limitations. Mol Biotechnol 2004; 26: 249–261.
Maeda K, Yasunari K, Watanabe T, Nakamura M . Oxidative stress by peripheral blood mononuclear cells is increased in hypertensives with an extreme-dipper pattern and/or morning surge in blood pressure. Hypertens Res 2005; 28: 755–761.
Ermis N, Yagmur J, Acikgoz N, Cansel M, Cuglan B, Pekdemir H, Ozdemir R . Serum gamma-glutamyl transferase (GGT) levels and inflammatory activity in patients with non-dipper hypertension. Clin Exp Hypertens 2012; 34: 311–315.
Yildiz A, Gur M, Demirbag R, Yilmaz R, Akyol S, Aslan M, Erel O . Paraoxonase and arylesterase activities in untreated dipper and non-dipper hypertensive patients. Clin Biochem 2008; 41: 779–784.
Dounousi E, Papavasiliou E, Makedou A, Ioannou K, Katopodis KP, Tselepis A, Siamopoulos KC, Tsakiris D . Oxidative stress is progressively enhanced with advancing stages of CKD. Am J Kidney Dis 2006; 48: 752–760.
Alexander RW . Theodore Cooper Memorial Lecture. Hypertension and the pathogenesis of atherosclerosis. Oxidative stress and the mediation of arterial inflammatory response: a new perspective. Hypertension 1995; 25: 155–161.
Landmesser U, Harrison DG . Oxidative stress and vascular damage in hypertension. Coron Artery Dis 2001; 12: 455–461.
Kario K . Vascular damage in exaggerated morning surge in blood pressure. Hypertension 2007; 49: 771–772.
Müller WU, Bauch T, Stüben G, Sack H, Streffer C . Radiation sensitivity of lymphocytes from healthy individuals and cancer patients as measured by the comet assay. Radiat Environ Biophys 2001; 140: 83–89.
Altindag O, Karakoc M, Kocyigit A, Celik H, Soran N . Increased DNA damage and oxidative stress in patients with rheumatoid arthritis. Clin Biochem 2007; 40: 167–171.
Baysal Z, Cengiz M, Ozgonul A, Cakir M, Celik H, Kocyigit A . Oxidative status and DNA damage in operating room personnel. Clin Biochem 2009; 42: 189–193.
Gur M, Yildiz A, Demirbag R, Yilmaz R, Koçyigit A, Celik H, Aksoy N . Increased lymphocyte deoxyribonucleic acid damage in patients with cardiac syndrome X. Mutat Res 2007; 617: 8–15.
Szeto Y, Lee A, Benzie I, Obied H . Optimized noninvasive procedures to measure DNA damage in comet assay. Hum Exp Toxicol, (e-pub ahead of print 31 May 2012; doi: 10.1177/0960327112446816).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Gür, M., Elbasan, Z., Yıldıray Şahin, D. et al. DNA damage and oxidative status in newly diagnosed, untreated, dipper and non-dipper hypertensive patients. Hypertens Res 36, 166–171 (2013). https://doi.org/10.1038/hr.2012.156
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2012.156
Keywords
This article is cited by
-
Association between DNA damage, dietary patterns, nutritional status, and non-communicable diseases in coal miners
Environmental Science and Pollution Research (2019)
-
Oxidative DNA damage in diabetic and mild gestational hyperglycemic pregnant women
Diabetology & Metabolic Syndrome (2015)
-
CYBA (p22phox) variants associate with blood pressure and oxidative stress markers in hypertension: a replication study in populations of diverse altitudes
Hypertension Research (2015)
-
Dynamic regulation of the angiotensinogen gene by DNA methylation, which is influenced by various stimuli experienced in daily life
Hypertension Research (2015)