Abstract
Exercise training has an important role in the prevention and treatment of hypertension, but its effects on the early metabolic and hemodynamic abnormalities observed in normotensive offspring of hypertensive parents (FH+) have not been studied. We compared high-intensity interval (aerobic interval training, AIT) and moderate-intensity continuous exercise training (CMT) with regard to hemodynamic, metabolic and hormonal variables in FH+ subjects. Forty-four healthy FH+ women (25.0±4.4 years) randomized to control (ConFH+) or to a three times per week equal-volume AIT (80–90% of VO2MAX) or CMT (50–60% of VO2MAX) regimen, and 15 healthy women with normotensive parents (ConFH−; 25.3±3.1 years) had their hemodynamic, metabolic and hormonal variables analyzed at baseline and after 16 weeks of follow-up. Ambulatorial blood pressure (ABP), glucose and cholesterol levels were similar among all groups, but the FH+ groups showed higher insulin, insulin sensitivity, carotid-femoral pulse wave velocity (PWV), norepinephrine and endothelin-1 (ET-1) levels and lower nitrite/nitrate (NOx) levels than ConFH− subjects. AIT and CMT were equally effective in improving ABP (P<0.05), insulin and insulin sensitivity (P<0.001); however, AIT was superior in improving cardiorespiratory fitness (15 vs. 8%; P<0.05), PWV (P<0.01), and BP, norepinephrine, ET-1 and NOx response to exercise (P<0.05). Exercise intensity was an important factor in improving cardiorespiratory fitness and reversing hemodynamic, metabolic and hormonal alterations involved in the pathophysiology of hypertension. These findings may have important implications for the exercise training programs used for the prevention of inherited hypertensive disorder.
Similar content being viewed by others
Introduction
Essential arterial hypertension (HPT) is the most common risk factor for cardiovascular morbidity and mortality and is associated with substantial health-care expenditures.1, 2 Consequently, primary prevention for individuals at high risk for HPT has been emphasized.3 Among the population at high risk for HPT, those who have hypertensive parents (FH+) are worthy of special attention. It has been well established that a positive family history of HPT is a strong risk factor for future HPT in nonhypertensive offspring, independent of other risk factors.4 Moreover, hemodynamic, metabolic and hormonal abnormalities, as well as concentrations of biomarkers that may have a key role in the development of HPT, are increased in nonhypertensive offspring of parents with HPT.5, 6, 7
Higher levels of physical activity8, 9 and cardiorespiratory fitness9 have been shown to reduce the risk of HPT in healthy normotensive persons. Acute10, 11 and chronic12, 13, 14 exercise can also reduce resting blood pressure (BP) in hypertensive adults. Moreover, exercise training has been shown to improve several factors involved in the pathophysiology of HPT, including sympathetic activity,15 endothelial function,16 pulse wave velocity (PWV)14 and insulin sensitivity.12, 15, 16 However, relatively little attention has been given to the physiological adaptations following exercise training in FH+ subjects. A small number of studies have suggested the presence of an exercise-induced reduction in the cardiovascular response to stress17, 18 and sympathetic activity19, 20 in FH+ individuals, but because of the cross-sectional nature of these studies, it is not possible to infer direct causality.
Moderate-intensity continuous exercise training (CMT) has been traditionally recommended for healthy21 and hypertensive subjects.22 However, the optimal exercise frequency, intensity, time, and type for HPT treatment and prevention need to be more precisely defined to optimize its benefits.22 Several studies have shown that high-intensity aerobic interval training (AIT) is superior to CMT for improving cardiorespiratory fitness in healthy subjects23 and in patients with cardiovascular disease.16, 24 Moreover, AIT has shown to be more effective for reducing the PWV of HPT patients,14 as well as for improving endothelial function, insulin sensitivity, and blood glucose and high-density lipoprotein (HDL) cholesterol in subjects with metabolic syndrome.16 However, longitudinal studies analyzing the effects of AIT, or even CMT, on the hemodynamic, metabolic and hormonal profile of FH+ subjects are still lacking. Therefore, the aim of this study was to assess the effects of AIT vs. CMT on the hemodynamic, metabolic and hormonal status of young normotensive FH+ women. We hypothesized that AIT is superior to CMT for improving these variables in FH+ subjects.
Methods
Population and study design
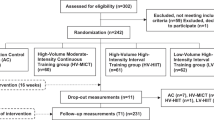
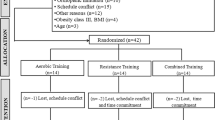
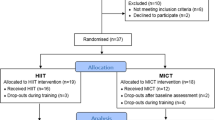
We studied 44 healthy young FH+ college women, randomly assigned to the AIT (n=16), CMT (n=16) or control groups (ConFH+; n=12). Fifteen healthy young college women with normotensive parents and a negative family history of HPT made up the second control group (ConFH−). All women were 20–30 years old, had BP below 130/80 mm Hg (measurements on two different occasions in triplicate at 2-min intervals) and had regular menstrual cycle, as confirmed by a questionnaire. Positive family history of HPT was defined as treatment for essential HPT for at least 2 years, confirmed by records of the parents’ physicians. A negative family history of HPT was defined as the absence of any evidence of HPT (BP below 130/85 mm Hg) or history of cardiovascular disease in both parents, confirmed by a questionnaire sent to the parents, by records of the parents’ physicians and by measurement of parents’ BP (measurements on two different occasions in triplicate at 2-min intervals). Exclusion criteria included use of medication or oral contraceptives, presence of any kind of disease (based on history, medical examination and exercise stress testing) and smoking. Pregnancy or lactation and involvement in regular physical activity or exercise program during the previous 12 months were also exclusion criteria. After a thorough explanation of the study design and protocol, written informed consent was obtained from each subject before participation, as required by the ethics committee at our institution. The subjects’ characteristics at inclusion are summarized in Table 1.
Following a 12-h overnight fast, subjects had their weight, height, waist circumference and waist-to-hip ratio determined. After being seated for at least 5 min, venous blood was taken for analyses of insulin, glucose and lipids. Between 1400 and 1500 hours on the day after the first visit, subjects had their BP and pulse rate determined by three measurements with 2-min intervals and after a 15-min seated rest. Carotid-femoral PWV was then measured, and 24-h ambulatory BP (ABP) monitoring was initiated at the end of this visit. At 2 days after the second visit (between 0800 and 1100 hours), a maximal graded exercise test (GXT) with blood sampling for norepinephrine, endothelin-1 (ET-1) and nitrite/nitrate (NOx) measurements was carried out. All measurements were carried out in a quiet air-conditioned (21–24 °C) room during the follicular phase of the volunteers’ menstrual cycle, before and after 16 weeks of follow-up.
ABP monitoring
We used a Spacelab 9207 device (Spacelabs Medical Inc, Redmond, WA, USA) to evaluate 24-h ABP. BP was recorded at 15-min intervals during the day and 20-min intervals at night. The averages of the 24-h, daytime, and nighttime systolic and diastolic BP were analyzed.
PWV
Volunteers were asked to refrain from strenuous physical activities and from caffeine or alcohol intake for 24 h, and to have a light meal at least 3 h before the test. Carotid-femoral PWV was analyzed with a noninvasive automatic device (Complior; Colson, Garges les Gonesses, France) by an experienced observer blinded to the group assignments. Briefly, common carotid artery and femoral artery pressure waveforms were recorded noninvasively using a pressure-sensitive transducer (TY-306-Fukuda; Fukuda, Tokyo, Japan). The distance between the recording sites (D) was measured in a straight line with a flexible meter, and PWV was automatically calculated as PWV=D/t, where (t) means pulse transit time.25 Measurements were repeated over 10 different cardiac cycles, and the mean was used for the final analysis.
Exercise testing
Volunteers were asked to refrain from strenuous physical activities and from caffeine- or alcohol-containing beverages for 24 h before the GXT. As plasma NOx levels can be influenced by diet,26 volunteers were also asked to follow a low-nitrite/nitrate diet for 5 days before the GXT. Subjects’ last meals before testing were ingested at least 4 h before the start of the GXT. Testing was carried out in the morning (between 0900 and 1200 hours) and after 1 h of rest in the supine position. A 20-gauge elastic tube was inserted into the antecubital vein before the beginning of the resting period. Blood sampling was performed at the end of the resting period (resting), immediately after GXT (exercise), and 10 min after cessation of GXT (recovery) to evaluate plasma norepinephrine, ET-1 and NOx levels. GXT was carried out on a programmable treadmill (TMX425 Stress Treadmill; TrackMaster, Newton, KS, USA) in a temperature-controlled room (21–23 °C) using a ramp protocol until exhaustion and with monitoring of cardiac rhythm (CardioSoft 6.5; GE Medical Systems IT, Milwaukee, WI, USA) and BP (Tango Stress BP; SunTech Medical Inc, Morrisville, NC, USA) as previously described.7 Ventilation (VE), oxygen uptake (VO2) and carbon dioxide output (VCO2) were measured breath-by-breath using a computerized system (Vmax Encore29; SensorMedics Corp., Yorba Linda, CA, USA). The respiratory exchange ratios were recorded as the averaged samples obtained during each stage of the protocol. The highest VO2 uptake level was considered the maximal value (VO2MAX). Anaerobic threshold was determined by the V-slope method, and the respiratory compensation point (RCP) was determined as the point at which a rapid rise in VE/VCO2 and a fall in partial pressure of CO2 were observed.27 Anaerobic threshold and RCP were identified by two experienced observers who were blinded to the subjects’ group and used for exercise prescription. When there was divergence between the two observers, a third observer was consulted to reach a consensus.
Blood analyses
All blood samples were immediately placed on ice and centrifuged at 2000 r.p.m. for 15 min at 4 °C and plasma and serum were stored at −80 °C until they were assayed. Serum glucose, total cholesterol and fractions, and triglycerides were analyzed by standard methods using a Dimension RXL Max automatic analyzer (Dade Behring, Newark, DE, USA). Serum insulin and ET-1 were measured by radioimmunoassay as previously described.7 Plasma NOx levels were measured by spectrophotometry using a commercially available kit (Colorimetric Nitric Oxide Assay Kit; Calbiochem, San Diego, CA, USA) according to the method described by Green et al.28 Norepinephrine was extracted from the plasma by aluminum oxide and measured by high-performance liquid chromatography. To estimate insulin sensitivity, the homeostasis model assessment (HOMA) was used.
Exercise training protocol
Both exercise groups performed an endurance training program (walking/running on a treadmill) three times a week for 16 weeks under the supervision of an exercise specialist. All subjects were instructed not to add any leisure exercise during the study period. The exercise sessions consisted of 5 min of warm-up, 40 min of endurance exercise (AIT or CMT) and 15 min of calisthenics. Endurance exercise intensity was determined according to the workload reached during the GXT and was prescribed to promote the same cardiovascular workload for both AIT and CMT. AIT consisted of 2 min of walking at the anaerobic threshold (50–60% of VO2MAX) alternating with 1 min of walking/running at CRP (80–90% of VO2MAX) for 40 min. CMT consisted of 40 min of walking at 60–70% of VO2MAX, representing the same total training load as the AIT. All subjects exercised using a heart rate-monitoring device during every training session to ensure that the subjects were training on their corresponding heart rate relative to VO2MAX. The speed of the treadmill was continually adjusted as training adaptations occurred to ensure that all training sessions were carried out at the desired heart rate throughout the 16-week training period. An exercise training compliance of 70% was set as a criterion for completing the study.
Statistical analyses
All data are reported as means±s.d. The statistical program SPSS 12.0 for Windows (SPSS Inc, Chicago, IL, USA) was used to perform statistical analysis. The Kolmogorov–Smirnov test was applied to ensure a Gaussian distribution of the results. One-way analysis of variance (ANOVA) was used to analyze differences in the subjects’ characteristics at baseline. Inter- and intragroup comparisons of the variables were made by two-way ANOVA (group vs. time) with repeated measurements. Bonferroni post hoc analysis was used to determine significance of data that was indicated by one-way or two-way ANOVA. The unpaired t-test was used to compare the post-exercise cardiorespiratory fitness (VO2MAX) improvements. The significance level was set at P<0.05.
To obtain an estimate of the effect size we might expect for the variables in our sample, we relied on the results of exercise training studies similar to ours.16, 23, 24 Considering that the results of those studies produced a 5.5–35% increase in VO2MAX, with the lower increases being promoted by continuous moderated exercise (5.5–16%), we estimated that an overall sample of 12 subjects for each group would be required to provide a power of 85% to detect a VO2MAX change of 10% with a two-sided α of <0.05.
Results
Subjects’ characteristics and exercise compliance
Age, weight, body mass index, waist circumference, waist-to-hip ratio and office BP were similar between groups at baseline (Table 1). During the experimental period, 13 volunteers were unable to complete the study: seven were unable to complete the exercise program for personal reasons (four AIT group), three did not have the minimal exercise training compliance of 70% (one AIT group) and three were unable to perform follow-up tests for personal reasons (all in the ConFH− group). There were no significant differences for the baseline characteristics between the subjects who completed the study and those who did not (data not shown).
After follow-up, weight, body mass index, waist circumference, waist-to-hip ratio and office BP did not change significantly in any group. Exercise training compliance did not differ between the AIT (83.2±6.3%) and CMT groups (83.7±3.9%).
Lipids, glucose and insulin assays
Total cholesterol and fractions, triglycerides and glucose levels were similar between groups at baseline and did not change significantly after 16 weeks of follow-up. The ConFH− group showed lower insulin and higher insulin sensitivity (HOMA) levels than the AIT, CMT and ConFH+ groups at baseline (P<0.01). However, the AIT and CMT groups improved insulin and insulin sensitivity levels after follow-up (P<0.001). With the improvement, the AIT group (but not the CMT group) insulin and insulin sensitivity levels after the follow-up period were similar to the ConFH− group and better than the ConFH+ group (P<0.05). Insulin and insulin sensitivity did not change significantly in the ConFH− and ConFH+ groups after the follow-up period (Table 2).
PWV
PWV was lower in the ConFH− group compared with the AIT, CMT and ConFH+ groups at baseline (P<0.001). After follow-up, the AIT group has reduced PWV (P<0.01) to levels similar to those observed in the ConFH− group, and lower than those seen in the ConFH+ group. The CMT group also showed lower PWV levels after the follow-up, but the reduction was not significant (P=0.06). PWV did not change significantly in the ConFH− and ConFH+ groups after follow-up (Table 3). There were no significant differences among all four groups in the BP and heart rate measured before the PWV assessment, before and after the experimental protocol.
Cardiorespiratory fitness and BP response to exercise
Cardiovascular and ventilatory variables were similar among all four groups at baseline (Table 4). The AIT and CMT groups had increased VO2MAX after the follow-up period, but the increase in the AIT group was greater than that in the CMT group (AIT=15.8±6.3%; CMT=8.0±6.1%; P<0.05). Heart rate did not change significantly for any group after the follow-up period (Table 4). However, the AIT and CMT groups improved their BP response to exercise after follow-up. Recovery systolic and diastolic BP, as well as resting and exercise diastolic BP, were reduced in the AIT group after the follow-up period (P<0.01). In the CMT group, only recovery systolic BP and exercise diastolic BP were reduced after the follow-up (P<0.05). With the reduction, exercise diastolic BP was lower in the AIT group than that in the ConFH+ group (P<0.05) after follow-up (Figure 1).
Norepinephrine, ET-1 and Nox
At baseline, the ConFH− group had lower levels of norepinephrine (resting, exercise and recovery) and ET-1 (resting and exercise) and higher levels of NOx (resting, exercise and recovery) than the three FH+ groups (P<0.05). On the other hand, AIT reduced resting, exercise and recovery norepinephrine (P<0.05), reduced resting and exercise ET-1 (P<0.05), and increased resting, exercise and recovery NOx (P<0.01). In the CMT group, only resting and exercise norepinephrine, resting ET-1, and exercise and recovery NOx improved after follow-up (P<0.05). With these improvements, the AIT group (but not the CMT group) showed lower norepinephrine and ET-1 levels and higher NOx levels than the ConFH+ group after follow-up (P<0.05). Norepinephrine, ET-1 and NOx levels did not change significantly in the ConFH− and ConFH+ groups after the follow-up period (Figure 2).
Norepinephrine (a), endothelin-1 (b) and NOx (c) before and after the experimental protocol. 1: resting; 2: exercise; 3: recovery. *Different from AIT, CMT and ConFH+ before follow-up (P<0.05); #different from ConFH+ after follow-up (P<0.05); different from after follow-up in the same group (♦P<0.05; ♦♦P<0.01).
ABP
The 24-h daytime and nighttime ABP were not significantly different among all four groups at baseline. Both AIT and CMT were beneficial to the ABP, reducing systolic and diastolic 24-h and nighttime BP after the follow-up period (P<0.05). ABP levels did not change significantly in the ConFH− and ConFH+ groups after the follow-up period (Table 3).
Discussion
The primary finding of this study is that exercise intensity is an important factor for improving cardiorespiratory fitness and restoring the hemodynamic, metabolic and hormonal abnormalities of nonhypertensive women offspring of HPT parents, including PWV, BP response to exercise, and norepinephrine, ET-1 and NOx levels. To the best of our knowledge, this is a pioneering study in evaluating the effects of exercise intensity in FH+ women.
Lipids, glucose and insulin
The existence of early abnormalities of glucose and insulin metabolism has been shown among healthy FH+ subjects.7, 29 In our study, the three FH+ groups showed higher insulin levels and insulin sensitivity than the ConFH− group. On the other hand, both the AIT and the CMT groups reduced insulin levels and insulin sensitivity to levels similar to those of the ConFH− group. The mechanism involved in these reductions was not investigated. However, the improvement in insulin metabolism by exercise training has been shown to be a function of greater signaling and insulin action in muscle,16, 30 resulting from a decreased intracellular accumulation of triglycerides and increased fatty acid oxidation.16, 31 In contrast to our results, high-intensity interval exercise has been shown to be more effective than moderate-intensity exercise for insulin and insulin sensitivity.16 In this study, only interval exercise improved insulin levels and insulin sensitivity in middle-aged and older subjects with metabolic syndrome after 16 weeks of follow-up. Thus, it is possible that in subjects with greater insulin and metabolic abnormalities, only the high-intensity promoted by interval exercise may improve insulin action, while moderate-intensity exercise may be sufficient for healthy women.
Exercise training has also been shown to increase HDL cholesterol as well as reduce triglycerides and low-density lipoprotein (LDL) cholesterol. Results from the HERITAGE Study,32 including 675 normolipidemic subjects (376 women), showed that women increased HDL cholesterol by 1.4 mg per 100 ml (3%), and reduced triglycerides and LDL cholesterol by 0.6 mg per 100 ml (0.6%) and 4.4 mg per 100 ml (4%), respectively, after 5 months of exercise training. Our study showed that AIT increased HDL cholesterol by 2.3 mg per 100 ml (3.8%) and reduced triglycerides and LDL cholesterol by 0.7 mg per 100 ml (0.9%) and 12.3 mg per 100 ml (11.7%), respectively, whereas CMT increased HDL cholesterol by 3.6 mg per 100 ml (6.3%) and reduced LDL cholesterol (but not triglycerides) by 6.0 mg per 100 ml (5.6%). However, these improvements were not statistically significant.
PWV
There is a progressive increase in arterial stiffness with aging,33, 34 with greater increases observed in HPT subjects.34 Moreover, healthy FH+ subjects have been shown to have increased arterial stiffness before any increase in BP.6, 7 In agreement with these results, the three FH+ groups in our study showed higher PWV levels than the ConFH− group. On the other hand, regular aerobic exercise has been shown to attenuate age-associated arterial stiffness and to reduce established arterial stiffness.35 However, moderate-intensity exercise has failed to improve the arterial stiffness of isolated systolic HPT subjects.36 A recent study from our group has shown that AIT, but not CMT, reduced arterial stiffness of HPT women after 16 weeks of follow-up.14 This study showed a significant reduction of the PWV after 16 weeks of AIT (P<0.01), whereas only a tendency toward reduction was observed after 16 weeks in the CMT group (P=0.06). These apparently conflicting results among the studies may be explained by the exercise intensity and the subjects’ health status. The mechanisms involved in age-related arterial stiffness increase include degradation of elastic matrix, endothelial dysfunction, hypertrophy and hyperplasia of smooth muscle cells, and increase of collagen content, which seems to be accelerated in the presence of HPT.37 Thus, exercise training programs of higher intensity (that is, interval exercise) may be more effective in reducing arterial stiffness in populations that already have some alterations in this variable. Improvements in the endothelial function and sympathetic activity for the arterial smooth muscle cells are possible mechanisms involved in arterial stiffness reduction induced by exercise training.37 Although both exercise training programs improved norepinephrine levels, only AIT improved plasma NOx, a biomarker of endothelial function.38 Thus, it seems reasonable to suggest that AIT was more effective in reducing PWV by improving endothelial function, as well as by indirectly reducing the sympathetic tonus induced by an increase of the nitric oxide inhibitory effect.39
Cardiorespiratory fitness and BP response to exercise
AIT increased VO2MAX to a higher degree than CMT. This is in line with previous studies that showed greater efficiency of high-intensity interval training over moderate-intensity exercise in improving cardiorespiratory fitness of healthy subjects,23 as well as in coronary artery disease,24 heart failure,40 metabolic syndrome16 and intermittent claudication patients.41 The superiority of high-intensity interval training for improving cardiorespiratory fitness has important clinical implications because there is a strong association between low cardiorespiratory fitness and incidence of HPT.9 Of all established risk factors, low cardiorespiratory fitness seems to be the strongest predictor of mortality.42 Increases in central O2 delivery (cardiac output) and peripheral O2 uptake (arteriovenous oxygen difference) contribute to training-induced improvements in cardiorespiratory fitness.40 As most evidence suggests that stroke volume is the main factor that limits cardiorespiratory fitness, the interval training design, characterized by short work periods at higher intensities alternating with low-intensity exercise periods, promotes a greater challenge for the pumping ability of the heart than that done by lower exercise intensities.16
Beside cardiorespiratory fitness, BP response to exercise has important implications for HPT prognosis, as supported by the association between exaggerated BP response to exercise and incidence of future HPT.43 A greater BP response to exercise among normotensive women offspring of hypertensive parents when compared with normotensive subjects with normotensive parents has also been shown.7 In this study, the three groups with positive family histories of HPT showed a 2–17 mm Hg greater (but not statistically significant) baseline BP response to exercise when compared with the ConFH− group. On the other hand, the AIT group also showed greater effects on the BP response to exercise. Lower levels of resting diastolic BP, exercise diastolic BP, and recovery systolic and diastolic BP were observed after 16 weeks of AIT. With these improvements, the AIT group showed lower exercise diastolic BP when compared with the ConFH+ group. In the CMT group, only exercise diastolic BP and recovery systolic BP were reduced in CMT. The greater improvements in the norepinephrine, ET-1 and NOx response to exercise observed after AIT are possible explanations for the differences in BP response to exercise between groups.
Norepinephrine, ET-1 and NOx
Although the precise mechanism is not completely understood, increased activation of the sympathetic nervous system and impaired endothelial vasodilator function probably have a key role in the pathogenesis of essential HPT.7 A recent study from our group has shown that young normotensive women with positive family history of HPT show increased norepinephrine and ET-1 levels, as well as lower NOx levels, both at rest and in response to exercise.7 Moreover, women with two HPT parents showed higher norepinephrine and ET-1 levels, as well as higher NOx levels, when compared with women with only one HPT parent. The increased norepinephrine and ET-1 response to exercise and the lower NOx response to exercise observed in the three groups with positive family history of HPT are in line with our previous study. On the other hand, relatively little attention has been given to the importance of physiological adaptations after exercise in FH+ subjects. Few studies using cross-sectional design with aerobically trained and untrained FH+ and FH− subjects have examined whether physical fitness modifies the disturbances in the sympathetic nervous system and endothelial function associated with FH+. Although negative findings have been shown,44 the studies have generally suggested that there is an exercise-induced reduction in the sympathetic nervous system and ET-1 levels in FH+ subjects.19, 20, 45 However, because of the cross-sectional nature of the studies, it is not possible to infer direct causality. This study confirms the important role of exercise training in reversing the sympathetic nervous system and endothelial function alteration associated with FH+, which has been suggested by the cross-sectional studies. We demonstrated that the AIT and CMT groups improved norepinephrine, ET-1 and NOx response to exercise, with better results seen after AIT. After the experimental protocol, the AIT group showed reduced resting, exercise and recovery norepinephrine, reduced resting and exercise ET-1, and increased resting, exercise and recovery NOx. In the CMT group, only resting and exercise norepinephrine, resting ET-1, and exercise and recovery NOx were improved after the follow-up period. With these results, only the AIT group showed lower norepinephrine and ET-1 levels and higher NOx levels than the ConFH+ group after follow-up. The reason for these differences in ET-1 and NOx response to exercise between groups is not fully understood, but it seems reasonable to suggest that the low- and high-intensity training exercise programs affect shear stress in the arterial wall differently during exercise training and that this may yield differences in molecular responses.
ABP
A recent meta-analysis has shown mean reductions of 0.3/0.1 and 2.5/3.1 mm Hg for systolic/diastolic daytime and nighttime ABP of normotensive subjects, respectively.13 The data are in line with the results of this study, which showed no significant reductions of 0.8/0.8 and 1.9/1.0 mm Hg for systolic/diastolic daytime ABP and significant reductions of 3.9/3.5 and 3.5/3.0 mm Hg for systolic/diastolic nighttime ABP in the AIT and CMT groups, respectively. In accordance with previous studies analyzing post-exercise effects on the ABP of HPT patients,10, 14 this study did not find any difference in the ABP reduction between high-intensity interval training and moderate-intensity continuous exercise.
Study limitations
Sympathetic activity was assessed indirectly by measuring plasma norepinephrine. Despite being an indirect technique, the measure of plasma norepinephrine is one of the preferred tests for analyzing the acute effects of stress tests and gives results similar to those observed with microneurography.46 The marker NOx is a metabolite of nitric oxide and may not be the best measure of nitric oxide production/availability because of the effects that diet may have on its measurement. However, women were advised to follow a low-nitrite/nitrate diet for the 5 days preceding the GXT, which has been shown to minimize the effects of diet on NOx measurement.26 Moreover, plasma NOx after GXT is related to endothelial function.38
Clinical implications
HPT is an important risk factor associated with all-cause and cardiovascular mortality, as well as a greater life expectance without cardiovascular disease.2, 47 Moreover, BP is strong and linearly associated with coronary heart disease and stroke,2 which are the most common causes of mortality among women.48 Preventing or delaying the onset of HPT may therefore have a large impact on public health, mainly in individuals at high risk for HPT.49 On the other hand, this study showed for the first time that young normotensive FH+ women may reverse hemodynamic, metabolic and hormonal alterations that are involved in the pathophysiology of HPT by participating in an exercise program, with greater improvements being observed after AIT. In addition to the superiority of AIT for improving arterial stiffness and BP, ET-1 and NOx response to exercise, the greater exercise-induced increase in cardiorespiratory fitness observed after AIT has also important implications because of all established risk factors, low cardiorespiratory fitness seems to be the strongest predictor of mortality.42
In summary, the results of this study showed that in young normotensive women offspring of hypertensive patients, high-intensity interval training was superior to moderate-intensity exercise in reversing hemodynamic, metabolic and hormonal alterations that are involved in the pathophysiology of HPT. These findings may have important implications in the design of exercise programs for the prevention of an inherited hypertensive disorder. Although multicenter prospective studies using high-intensity interval training for preventing HPT in women with higher familial risk are needed to advance our conclusions, the results of this study suggest that high-intensity interval training programs may yield more favorable results than moderate-intensity programs.
References
Lawes CM, Vander Hoorn S, Rodgers A . Global burden of blood pressure-related disease, 2001. Lancet 2008; 371: 1513–1518.
Chobanian AV, Bakris GL, Black HR, Cushiman WC, Green LA, Izzo JI, Jones DW, Materson BW, Oparil S, Wright Jr JT, Rochella EJ . The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42: 1206–1252.
Whelton PK, He J, Appel LJ, Cutler JA, Havas S, Kotchen TA, Roccella EJ, Stout R, Vallbona C, Winston MC, Karimbakas J . Primary prevention of hypertension: clinical and public health advisory from the National High Blood Pressure Education Program. JAMA 2002; 288: 1882–1888.
Wang NY, Young JH, Meoni LA, Ford DE, Erlinger TP, Klag MJ . Blood pressure change and risk of hypertension associated with parental hypertension: the Johns Hopkins Precursors Study. Arch Intern Med 2008; 168: 643–648.
Lieb W, Pencina MJ, Wang TJ, Larson MG, Lanier KJ, Benjamin EJ, Levy D, Tofler GH, Meigs JB, Newton-Cheh C, Vasan RS . Association of parental hypertension with concentrations of select biomarkers in nonhypertensive offspring. Hypertension 2008; 52: 381–386.
Kucerová J, Filipovsky J, Staessen JA, Cwynar M, Wojciechowska W, Stolarz K, Kuznetsova T, Gasowski J, Dolejsová M, Grodzicki T, Kawecka-Jaszcz K, Fagard R . Arterial characteristics in normotensive offspring of parents with or without a history of hypertension. Am J Hypertens 2006; 19: 264–269.
Ciolac EG, Bocchi EA, Bortolotto LA, Carvalho VO, Greve JM, Guimarães GV . Hemodynamic, metabolic, and neuro-humoral abormalities in young normotensive women at high familial risk for hypertension. J Hum Hypertens 2010; doi 10.1038/jhh.2010.21.
Hayashi T, Tsumura K, Suematsu C, Okada K, Fujii S, Endo G . Walking to work and the risk for hypertension in men: the Osaka Health Survey. Ann Intern Med 1999; 131: 21–26.
Chase NL, Sui X, Lee D, Blair S . The association of cardiorespiratory fitness and physical activity with incidence of hypertension in men. Am J Hypertens 2009; 22: 417–424.
Ciolac EG, Guimarães GV, D’Ávila VM, Bortolotto LA, Doria EL, Bocchi EA . Acute effects of continuous or interval aerobic exercise on 24-h ambulatory blood pressure of long-term treated hypertensive. Int J Cardiol 2009; 133: 381–387.
Ciolac EG, Guimarães GV, D’Ávila VM, Dória E, Bocchi EA . Acute aerobic exercise reduces 24-h ambulatory blood pressure levels in long-term-treated hypertensive patients. Clinics 2008; 63: 753–758.
Ciolac EG, Guimarães GV . Physical exercise and metabolic syndrome. Rev Bras Med Esporte 2004; 10: 325–330.
Pescatello LS, Kulikowich JM . The aftereffects of dynamic exercise on ambulatory blood pressure. Med Sci Sports Exerc 2001; 33: 1855–1861.
Guimarães GV, Ciolac EG, Carvalho VO, D’Ávila VM, Bortolotto LA, Bocchi EA . Effects of continuous versus interval exercise training on the blood pressure and arterial stiffness in treated hypertensive subjects: a randomized controlled study. Hypert Res 2010; doi:10.1038/hr.2010.42.
Cornelissen VA, Fagard RH . Effects of endurance training on blood pressure, blood pressure-regulating mechanisms, and cardiovascular risk factors. Hypertension 2005; 46: 667–675.
Tjønna AE, Lee SJ, Rognmo Ø, Stølen TO, Bye A, Haram PM, Loennechen JP, Al-Share QY, Skogvoll E, Slørdahl SA, Kemi OJ, Najjar SM, Wisløff U . Aerobic interval training versus continuous moderate exercise as a treatment for the metabolic syndrome. A pilot study. Circulation 2008; 118: 346–354.
Holmes DS, Cappo BM . Prophylactic effect of aerobic fitness on cardiovascular arousal among individuals with a family history of hypertension. J Psychosom Res 1987; 31: 601–605.
Jackson EM, Dishman RK . Hemodynamic responses to stress among black women: fitness and parental hypertension. Med Sci Sports Exerc 2002; 34: 1097–1104.
Buckworth J, Dishman RK, Cureton KJ . Autonomic responses of women with parental hypertension: effects of physical activity and fitness. Hypertension 1994; 24: 576–584.
Lénárd Z, Studinger P, Mersich B, Pavlik G, Kollai M . Cardiovagal autonomic function in sedentary and trained offspring of hypertensive parents. J Physiol 2005; 565: 1031–1038.
Haskell WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA, Macera CA, Heath GW, Thompson PD, Bauman A . Physical activity and public health. Updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Circulation 2007; 116: 1081–1093.
American College of Sports Medicine. ACSM Stand Position on Exercise and Hypertension. Med Sci Sporsts Exerc 2004; 36: 533–553.
Helgerud J, Hoydal K, Wang E, Karlsen T, Berg P, Bjerkaas M, Simonsen T, Helgesen C, Hjorth N, Bach R, Hoff J . Aerobic high intensity intervals improve VO2max more than moderate training. Med Sci Sports Exerc 2007; 39: 665–671.
Rognmo O, Hetland E, Helgerud J, Hoff J, Slordahl SA . High intensity aerobic interval exercise is superior to moderate intensity exercise for increasing aerobic capacity in patients with coronary artery disease. Eur J Cardiovasc Prev Rehabil 2004; 11: 216–222.
Asmar R, Benetos A, Topouchian J, Laurent P, Pannier B, Brisac AM, Target R, Levy BI . Assessment of arterial distensibility by automatic pulse wave velocity measurement: validation and clinical application studies. Hypertension 1995; 26: 485–490.
Wang J, Brown MA, Tam SH . Effects of diet on measurement of nitric oxide metabolites. Clin Exp Pharm Physiol 1997; 24: 418–420.
Wasserman K, Hansen JE, Sue D, Whipp BJ, Casaburi R . Principles of Exercise Testing and Interpretation. 4th edn. Lippincott Williams & Wilkins: Philadelphia, 2004, 32–35.
Green LC, Wagner DA, Glogowski J, Skipper PL, Wishnok JS, Tannenbaum SR . Analysis of nitrate, nitrite and [15N]nitrate in biological fluids. Anal Biochem 1982; 126: 131–138.
Goldstein IB, Shapiro D, Weiss RE . How family history and risk factors for hypertension relate to ambulatory blood pressure in healthy adults. J Hypertens 2008; 26: 276–283.
Koval JA, Maezono K, Patti ME, Pendergrass M, DeFronzo RA, Mandarino LJ . Effects of exercise and insulin on insulin signaling proteins in human skeletal muscle. Med Sci Sports Exerc 1999; 31: 998–1004.
Bonen A, Dohm GL, van Loon LJ . Lipid metabolism, exercise and insulin action. Essays Biochem 2006; 42: 47–59.
Leon AS, Rice T, Mandel S, Després JP, Bergeron J, Gagnon J, Rao DC, Skinner JS, Wilmore JH, Bouchard C . Blood lipid response to 20 weeks of supervised exercise in a large biracial population: the HERITAGE Family Study. Metabolism 2000; 49: 513–520.
Vaitkevicious PV, Fleg JL, Engel JH, O’Connor FC, Wright JG, Lakatta LE, Yin FCP, Lakatta EG . Effects of age and aerobic capacity on arterial stiffness in healthy adults. Circulation 1993; 88: 1456–1462.
Benetos A, Adamopoulos C, Bureau JM, Temmar M, Labat C, Bean K, Thomas F, Pannier B, Asmar R, Zureik M, Safar M, Guize L . Determinants of accelerated progression of arterial stiffness in normotensive subjects and in treated hypertensive subjects over a 6-Year period. Circulation 2002; 105: 1202–1207.
Tanaka H, Dinenno FA, Monahan KD, Clevenger CM, DeSouza CA, Seals DR . Aging, habitual exercise, and dynamic arterial compliance. Circulation 2000; 102: 1270–1275.
Ferrier KE, Waddell TK, Gatzka CD, Cameron JD, Dart AM, Kingwell BA . Aerobic exercise training does not modify large-artery compliance in isolated systolic hypertension. Hypertension 2001; 38: 222–226.
Zieman SJ, Melenovsky V, Kass DA . Mechanism, pathophysiology, and therapy of arterial stiffness. Artherioscler Thromb Vasc Biol 2005; 25: 932–943.
Allen JD, Cobb FR, Kraus WE, Gow AJ . Total nitrogen oxide following exercise testing reflects endothelial function and discriminates health status. Free Radic Biol Med 2006; 41: 740–747.
Zanzinger J . Role of nitric oxide in the neural control of cardiovascular function. Cardiovasc Res 1999; 43: 639–649.
Wisloff U, Stoylen A, Loennechen JP, Bruvold M, Rognmo O, Haram PM, Tjønna AE, Helgerud J, Slørdahl SA, Lee SJ, Videm V, Bye A, Smith GL, Najjar SM, Ellingsen O, Skjærpe T . Superior cardiovascular effect of aerobic interval training versus moderate continuous training in heart failure patients: a randomized study. Circulation 2007; 115: 3086–3094.
Slordahl SA, Wang E, Hoff J, Kemi OJ, Amundsen BH, Helgerud J . Effective training for patients with intermittent claudication. Scand Cardiovasc J 2005; 39: 244–249.
Myers J, Prakash M, Froelicher V, Do D, Partington S, Atwood JE . Exercise capacity and mortality among men referred for exercise testing. N Engl J Med 2002; 346: 793–801.
Sharabi Y, Ben-Cnaan R, Hanin A, Martonovitch G, Grossman E . The significance of hypertensive response to exercise as a predictor of hypertension and cardiovascular disease. J Hum Hyperten 2001; 15: 353–356.
Hamer M, Boutcher YN, Boutcher SH . Cardiovascular and renal responses to mental challenge in highly and moderately active males with family history of hypertension. J Hum Hypert 2002; 16: 319–326.
Tanzilli G, Barillà F, Pannitteri G, Greco C, Comito C, Schiariti M, Papalia U, Mangieri E . Exercise training counteracts the abnormal release of plasma endothelin-1 in normal subjects at risk for hypertension. Ital Heart J 2003; 4: 107–112.
Grassi G, Seravalle G, Bolla G, Quarti-Trevano F, Dell’Oro R, Arenare F, Mancia G . Heart rate as a sympathetic marker during acute adrenergic challenge. J Hypertens 2008; 26: 70–75.
Franco OH, Peeters A, Bonneux L, Laet C . Blood pressure in adulthood and life expectancy with cardiovascular disease in men and women: life course analysis. Hypertension 2005; 46: 1–7.
Barrios V, Escobar C, Echarri R, Matalí A . Gender and blood pressure control. Hypertension 2008; 51: e58.
Mosca L, Appel LJ, Benjamin EJ, Berra K, Chandra-Strobos N, Fabunmi RP, Grady D, Haan CK, Hayes SN, Judelson DR, Keenan NL, McBride P, Oparil S, Ouyang P, Oz MC, Mendelsohn ME, Pasternak RC, Pinn VW, Robertson RM, Schenck-Gustafsson K, Sila CA, Smith Jr SC, Sopko G, Taylor AL, Walsh BW, Wenger NK, Williams CL . Evidence-based guidelines for cardiovascular disease prevention in women. Circulation 2004; 109: 672–693.
Acknowledgements
This work was supported by the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP # 2004/00568-8). Dr Emmanuel G Ciolac was supported by the Sociedade de Cardiologia do Estado de São Paulo, and Dr Guilherme V Guimarães was supported by the Conselho Nacional de Pesquisa (CNPq # 304733/2008-3).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Ciolac, E., Bocchi, E., Bortolotto, L. et al. Effects of high-intensity aerobic interval training vs. moderate exercise on hemodynamic, metabolic and neuro-humoral abnormalities of young normotensive women at high familial risk for hypertension. Hypertens Res 33, 836–843 (2010). https://doi.org/10.1038/hr.2010.72
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2010.72
Keywords
This article is cited by
-
Acute effects of low-volume intermittent versus higher-volume continuous exercise on arterial stiffness in healthy young men
Scientific Reports (2022)
-
The effect of 8 weeks of combined interval (resistance-interval training) and combined endurance (endurance-resistance training) on plasma levels of adropin and nitric oxide in males with high blood pressure
Irish Journal of Medical Science (1971 -) (2022)
-
Modulation of Insulin Sensitivity by Exercise Training: Implications for Cardiovascular Prevention
Journal of Cardiovascular Translational Research (2021)
-
Effectiveness of High-Intensity Interval Training Versus Moderate-Intensity Continuous Training in Hypertensive Patients: a Systematic Review and Meta-Analysis
Current Hypertension Reports (2020)
-
Extremely short duration sprint interval training improves vascular health in older adults
Sport Sciences for Health (2019)