Abstract
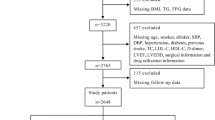
Metabolic syndrome (MS) is highly prevalent and an established key risk factor for coronary artery disease, regardless of the presence or absence of diabetes mellitus (DM). Long-term follow-up studies have addressed the influence of MS with and without DM on the prognosis of patients undergoing percutaneous coronary intervention (PCI). We classified 748 consecutive patients who had undergone PCI into four groups as follows: neither DM nor MS, DM alone, MS alone, and both DM and MS. Post hoc analyses were conducted using prospectively collected clinical data. Multivariate Cox regression was used to evaluate the risk within each group for all-cause mortality and composite cardiac events (cardiac death, non-fatal acute coronary syndrome), adjusting for age, gender, body mass index, low-density lipoprotein (LDL) cholesterol level, hypertension, smoking, prior coronary artery bypass graft, presentation of acute coronary syndrome, left ventricular ejection fraction, multivessel disease, and procedural success. The progress of 321 (42.9%) patients with neither DM nor MS, 109 (14.6%) patients with DM alone, 129 (17.2%) patients with MS alone, and 189 (25.3%) patients with both DM and MS was followed up for a mean of 12.0±3.6 years. Patients with both DM and MS had significant risk for increased all-cause mortality (2.10 [1.19–3.70]). Patients with MS alone (2.14 [1.31–3.50]) and with both DM and MS (1.87 [1.18–2.96]) were at significant risk for increased cardiac events. In conclusion, the risk of cardiac events is significantly increased in patients with metabolic syndrome following PCI, irrespective of DM.
Similar content being viewed by others
Article PDF
References
Takeuchi H, Saitoh S, Takagi S, et al: Metabolic syndrome and cardiac disease in Japanese men: applicability of the concept of metabolic syndrome defined by the National Cholesterol Education Program–Adult Treatment Panel III to Japanese Men—the Tanno and Sobetsu Study. Hypertens Res 2005; 28: 203–208.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults : Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001; 285: 2486–2497.
Grundy SM, Cleeman JI, Daniels SR, et al: Diagnosis and management of the metabolic syndrome: an American Heart Association/ National Heart, Lung and Blood Institute scientific statement. Circulation 2005; 112: 2735–2752.
Malik S, Wong ND, Franklin SS, et al: Impact of the metabolic syndrome on mortality from coronary heart disease, cardiovascular disease, and all causes in United States adults. Circulation 2004; 110: 1245–1250.
Isomaa B, Almgren P, Tuomi T, et al: Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care 2001; 24: 683–689.
Alexander CM, Landsman PB, Teutsch SM, Haffner SM : NCEP-defined metabolic syndrome, diabetes, and prevalence of coronary heart disease among NHANESIII participants age 50 years and older. Diabetes 2003; 52: 1210–1214.
Rana JS, Monraats PS, Zwinderman AH, et al: GENDER study. Metabolic syndrome and risk of restenosis in patients undergoing percutaneous coronary intervention. Diabetes Care 2005; 28: 873–877.
Nigam A, Bourassa MG, Fortier A, Guertin MC, Tardif JC : The metabolic syndrome and its components and the long-term risk of death in patients with coronary heart disease. Am Heart J 2006; 151: 514–521.
Kasai T, Miyauchi K, Kurata T, et al: Prognostic value of the metabolic syndrome for long-term outcomes in patients undergoing percutaneous coronary intervention. Circ J 2006; 70: 1531–1537.
Examination Committee of Criteria for ‘Obesity Disease’ in Japan, Japan Society for the Study of Obesity : New criteria for ‘obesity disease’ in Japan. Circ J 2002; 66: 987–992.
American Diabetes Association : Diagnosis and classification of diabetes mellitus. Diabetes Care 2007; 30 ( Suppl 1): S42–S47.
Alberti KG, Zimmet P, Shaw J : The metabolic syndrome—a new worldwide definition. Lancet 2005; 366: 1059–1062.
BARI Investigators : Influence of diabetes on 5-year mortality and morbidity in a randomized trial comparing CABG and PTCA in patients with multivessel disease: the Bypass Angioplasty Revascularization Investigation (BARI). Circulation 1997; 96: 1761–1769.
Kurbaan AS, Bowker TJ, Ilsley CD, Sigwart U, Rickards AF, CABRI Investigators (Coronary Angioplasty versus Bypass Revascularization Investigation) : Difference in the mortality of the CABRI diabetic and nondiabetic populations and its relation to coronary artery disease and the revascularization mode. Am J Cardiol 2001; 87: 947–950.
Barsness GW, Peterson ED, Ohman EM, et al: Relationship between diabetes mellitus and long-term survival after coronary bypass and angioplasty. Circulation 1997; 96: 2551–2556.
Seidell JC, Kahn HS, Williamson DF, Lissner L, Valdez R : Report from a Centers for Disease Control and Prevention Workshop on use of adult anthropometry for public health and primary health care. Am J Clin Nutr 2001; 73: 123–126.
Ko GTC, Chan JC, Cockram CS, Woo J : Prediction of hypertension, diabetes, dyslipidaemia or albuminuria using simple anthropometric indexes in Hong Kong Chinese. Int J Obes Relat Metab Disord 1999; 23: 1136–1142.
Shiwaku K, Anuurad E, Enkhmaa B, et al: Overweight Japanese with body mass indexes of 23.0 to 24.9 have higher risks for obesity associated disorders: a comparison of Japanese and Mongolians. Int J Obes Relat Metab Disord 2004; 28: 152–158.
Wong ND, Sciammarella MG, Polk D, et al: The metabolic syndrome, diabetes, and subclinical atherosclerosis assessed by coronary calcium. J Am Coll Cardiol 2003; 41: 1547–1553.
Janssen I, Katzmarzyk PT, Ross R : Body mass index, waist circumference, and health risk. Arch Intern Med 2002; 162: 2074–2079.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kasai, T., Miyauchi, K., Kurata, T. et al. Impact of Metabolic Syndrome among Patients with and without Diabetes Mellitus on Long-Term Outcomes after Percutaneous Coronary Intervention. Hypertens Res 31, 235–241 (2008). https://doi.org/10.1291/hypres.31.235
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.31.235