Abstract
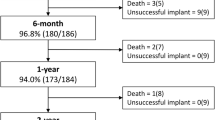
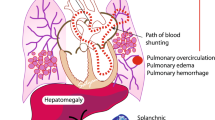
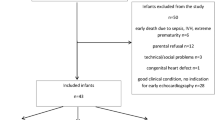
The purpose of this study was to investigate the application of trial balloon occlusion for permanent closure of patent ductus arteriosus (PDA) with severe pulmonary hypertension (PH) in adults, and to assess its immediate and short-term results. From September 1999 to September 2005, a total of ten adults (two males, ages ranging from 20 to 54 years) with PDA who met the criterion for severe PH (basal pulmonary vascular resistance > 8 Wood units) received trial balloon occlusion via an embolectomy balloon catheter. Post-occlusion hemodynamics, along with an overall clinical and hemodynamic assessment, was used to consider the indication of closure of PDA. Nine of the patients underwent successful transcatheter closure of PDA and subsequently used Amplatzer occluder devices. Chest X-ray, cardiography and echocardiography were used for follow-up evaluation of the treatment within 6 months after successful closure of PDA. No patient had a detectable residual shunt by color flow mapping or any other complications (device migration, hemolysis, endocarditis, etc.) at follow-up. In conclusion, trial balloon occlusion helps to determine anticipated hemodynamics after closure of PDA, so it is conducive to indicating permanent closure of adult PDA with reversible but severe PH. Furthermore, satisfactory immediate and short-term outcomes have proven this method to be safe and valid.
Similar content being viewed by others
Article PDF
References
Ewert P : Challenges encountered during closure of patent ductus arteriosus. Pediatr Cardiol 2005; 26: 224–229.
Bridges ND, Perry SB, Parness I, Keane JF, Lock JE : Transcatheter closure of a large patent ductus arteriosus with the clamshell septal umbrella. J Am Coll Cardiol 1991; 18: 1297–1302.
Roy A, Juneja R, Saxena A : Use of Amplazer duct occluder to close severely hypertensive ducts: utility of transient balloon occlusion. Indian Heart J 2005; 57: 332–336.
Lu C, Wei X, Huang C, Luo H, Tan W, Mao S : Amplatzer PDA occluder used in adult patent ductus arteriosus hypertension after testing balloon occlusion. Chin Med J 2002; 115: 461–462.
Aizawa K, Hanaoka T, Kasai H, et al: Long-term verdenafil therapy improves hemodynamics in patients with pulmonary hypertension. Hypertens Res 2006; 29: 123–128.
Bush A, Busst CM, Haworth SG, et al: Correlations of lung morphology, pulmonary vascular resistance, and outcome in children with congenital heart disease. Br Heart J 1988; 59: 480–485.
Wilson NJ, Seear MD, Taylor GP, LeBlanc JG, Sandor GG : The clinical value and risks of lung biopsy in children with congenital heart disease. J Thorac Cardiovasc Surg 1990; 99: 460–468.
Krichenko A, Benson LN, Burrows P, Moes CA, McLaughlin P, Freedom RM : Angiographic classification of the isolated, persistently patent ductus arteriosus and implications for percutaneous catheter occlusion. Am J Cardiol 1989; 63: 877–880.
Yamaki S, Mohri H, Haneda K, Endo M, Akimoto H : Indications for surgery based on lung biopsy in cases of ventricular septal defect and/or patent ductus arteriosus with severe pulmonary hypertension. Chest 1989; 96: 31–39.
Celermajer DS, Sholler GF, Hughes CF, Baird DK : Persistent ductus arteriosus in adults. A review of surgical experience with 25 patients. Med J Aust 1991; 155: 233–236.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Ji, Q., Feng, J., Mei, Y. et al. Transcatheter Closure of Adult Patent Ductus Arteriosus with Severe Pulmonary Hypertension. Hypertens Res 31, 1997–2002 (2008). https://doi.org/10.1291/hypres.31.1997
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.31.1997