Abstract
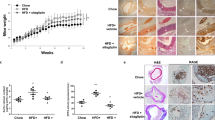
The combined effect of an angiotensin II type 1 receptor blocker and a 3-hydroxy-3-methylglutaryl-coenzyme A (HMG-CoA) reductase inhibitor on vascular lesion formation in the insulin-resistant state has not been examined. We tested whether or not combined treatment is superior to single-drug treatment for inhibiting vascular lesion formation in insulin-resistant rats. The rats were maintained on a fructose-rich diet for 4 weeks and then treated with olmesartan (1 mg/kg/day) and/or pravastatin (10 mg/kg/day) for 3 weeks. After 1 week of drug treatment, balloon injury of the carotid arteries was performed. Two weeks later, the injured arteries were harvested for morphometry and immunostaining. Olmesartan and pravastatin each modestly attenuated neointimal formation without significant changes in blood pressure or serum lipid levels. The combination of olmesartan and pravastatin significantly suppressed the neointimal formation compared with either monotherapy. The number of terminal deoxynucleotidyl transferase–mediated dUTP nick end-labeling (TUNEL)−positive cells was increased by olmesartan but not by pravastatin. Olmesartan and pravastatin each decreased the number of Ki-67−positive cells, which indicates cell proliferation, to the same extent. The combined treatment increased the number of TUNEL-positive cells but did not affect the number of Ki-67−positive cells. The combined treatment decreased the insulin level and increased the number of circulating endothelial progenitor cells. These results suggest that the combination of olmesartan and pravastatin is beneficial for the treatment of vascular diseases in the insulin-resistant state independently of blood pressure or cholesterol levels.
Similar content being viewed by others

Article PDF
References
Stumvoll M, Goldstein BJ, van Haeften TW : Type 2 diabetes: principles of pathogenesis and therapy. Lancet 2005; 365: 1333–1346.
Grundy SM : Metabolic syndrome: connecting and reconciling cardiovascular and diabetes worlds. J Am Coll Cardiol 2006; 47: 1093–1100.
Ford ES : Risks for all-cause mortality, cardiovascular disease, and diabetes associated with the metabolic syndrome: a summary of the evidence. Diabetes Care 2005; 28: 1769–1778.
de Gasparo M, Catt KJ, Inagami T, Wright JW, Unger T : International union of pharmacology. XXIII. The angiotensin II receptors. Pharmacol Rev 2000; 52: 415–472.
Pfeffer MA, McMurray JJ, Velazquez EJ, et al: Valsartan, captopril, or both in myocardial infarction complicated by heart failure, left ventricular dysfunction, or both. N Engl J Med 2003; 349: 1893–1906.
Pfeffer MA, Swedberg K, Granger CB, et al: Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet 2003; 362: 759–766.
Barnett AH, Bain SC, Bouter P, et al: Angiotensin-receptor blockade versus converting-enzyme inhibition in type 2 diabetes and nephropathy. N Engl J Med 2004; 351: 1952–1961.
Dahlof B, Sever PS, Poulter NR, et al: Prevention of cardiovascular events with an antihypertensive regimen of amlodipine adding perindopril as required versus atenolol adding bendroflumethiazide as required, in the Anglo-Scandinavian Cardiac Outcomes Trial-Blood Pressure Lowering Arm (ASCOT-BPLA): a multicentre randomised controlled trial. Lancet 2005; 366: 895–906.
Wilt TJ, Bloomfield HE, MacDonald R, et al: Effectiveness of statin therapy in adults with coronary heart disease. Arch Intern Med 2004; 164: 1427–1436.
Jain MK, Ridker PM : Anti-inflammatory effects of statins: clinical evidence and basic mechanisms. Nat Rev Drug Discov 2005; 4: 977–987.
Horiuchi M, Cui TX, Li Z, et al: Fluvastatin enhances the inhibitory effects of a selective angiotensin II type 1 receptor blocker, valsartan, on vascular neointimal formation. Circulation 2003; 107: 106–112.
Li Z, Iwai M, Wu L, et al: Fluvastatin enhances the inhibitory effects of a selective AT1 receptor blocker, valsartan, on atherosclerosis. Hypertension 2004; 44: 758–763.
Nishikawa H, Miura S, Shimomura H, et al: Combined treatment with statin and angiotensin-receptor blocker after stenting as a useful strategy for prevention of coronary restenosis. J Cardiol 2005; 45: 107–113.
Morawietz H, Erbs S, Holtz J, et al: Endothelial protection, AT1 blockade and cholesterol-dependent oxidative stress: the EPAS trial. Circulation 2006; 114: I296–I301.
Togashi N, Ura N, Higashiura K, Murakami H, Shimamoto K : Effect of TNF-alpha–converting enzyme inhibitor on insulin resistance in fructose-fed rats. Hypertension 2002; 39: 578–580.
Kim S, Izumi Y, Izumiya Y, Zhan Y, Taniguchi M, Iwao H : Beneficial effects of combined blockade of ACE and AT1 receptor on intimal hyperplasia in balloon-injured rat artery. Arterioscler Thromb Vasc Biol 2002; 22: 1299–1304.
Li C, Yang CW, Park JH, et al: Pravastatin treatment attenuates interstitial inflammation and fibrosis in a rat model of chronic cyclosporine-induced nephropathy. Am J Physiol Renal Physiol 2004; 286: F46–F57.
Tokunou T, Shibata R, Kai H, et al: Apoptosis induced by inhibition of cyclic AMP response element–binding protein in vascular smooth muscle cells. Circulation 2003; 108: 1246–1252.
Simper D, Wang S, Deb A, et al: Endothelial progenitor cells are decreased in blood of cardiac allograft patients with vasculopathy and endothelial cells of noncardiac origin are enriched in transplant atherosclerosis. Circulation 2003; 108: 143–149.
D'Angelo G, Elmarakby AA, Pollock DM, Stepp DW : Fructose feeding increases insulin resistance but not blood pressure in Sprague-Dawley rats. Hypertension 2005; 46: 806–811.
Okada K, Hirano T, Ran J, Adachi M : Olmesartan medoxomil, an angiotensin II receptor blocker ameliorates insulin resistance and decreases triglyceride production in fructose-fed rats. Hypertens Res 2004; 27: 293–299.
Yamakawa T, Tanaka S, Numaguchi K, et al: Involvement of Rho-kinase in angiotensin II–induced hypertrophy of rat vascular smooth muscle cells. Hypertension 2000; 35: 313–318.
Begum N, Sandu OA, Ito M, Lohmann SM, Smolenski A : Active Rho kinase (ROK-alpha) associates with insulin receptor substrate-1 and inhibits insulin signaling in vascular smooth muscle cells. J Biol Chem 2002; 277: 6214–6222.
Martin G, Duez H, Blanquart C, et al: Statin-induced inhibition of the Rho-signaling pathway activates PPARalpha and induces HDL apoA-I. J Clin Invest 2001; 107: 1423–1432.
Morikawa-Futamatsu K, Adachi S, Maejima Y, et al: HMG-CoA reductase inhibitor fluvastatin prevents angiotensin II–induced cardiac hypertrophy via Rho kinase and inhibition of cyclin D1. Life Sci 2006; 79: 1380–1390.
Negre-Aminou P, van Vliet AK, van Erck M, van Thiel GC, van Leeuwen RE, Cohen LH : Inhibition of proliferation of human smooth muscle cells by various HMG-CoA reductase inhibitors; comparison with other human cell types. Biochim Biophys Acta 1997; 1345: 259–268.
Weiss RH, Ramirez A, Joo A : Short-term pravastatin mediates growth inhibition and apoptosis, independently of Ras, via the signaling proteins p27Kip1 and P13 kinase. J Am Soc Nephrol 1999; 10: 1880–1890.
Walter DH, Rittig K, Bahlmann FH, et al: Statin therapy accelerates reendothelialization: a novel effect involving mobilization and incorporation of bone marrow–derived endothelial progenitor cells. Circulation 2002; 105: 3017–3024.
Yamamoto E, Yamashita T, Tanaka T, et al: Pravastatin enhances beneficial effects of olmesartan on vascular injury of salt-sensitive hypertensive rats, via pleiotropic effects. Arterioscler Thromb Vasc Biol 2007; 27: 556–563.
Tanaka K, Sata M, Hirata Y, Nagai R : Diverse contribution of bone marrow cells to neointimal hyperplasia after mechanical vascular injuries. Circ Res 2003; 93: 783–790.
Strehlow K, Werner N, Berweiler J, et al: Estrogen increases bone marrow–derived endothelial progenitor cell production and diminishes neointima formation. Circulation 2003; 107: 3059–3065.
Trovati M, Anfossi G : Influence of insulin and of insulin resistance on platelet and vascular smooth muscle cell function. J Diabetes Complications 2002; 16: 35–40.
Koyama H, Bornfeldt KE, Fukumoto S, Nishizawa Y : Molecular pathways of cyclic nucleotide–induced inhibition of arterial smooth muscle cell proliferation. J Cell Physiol 2001; 186: 1–10.
Hsueh WA, Law RE : Insulin signaling in the arterial wall. Am J Cardiol 1999; 84: 21J–24J.
Zeng G, Quon MJ : Insulin-stimulated production of nitric oxide is inhibited by wortmannin. Direct measurement in vascular endothelial cells. J Clin Invest 1996; 98: 894–898.
Aizawa T, Wei H, Miano JM, Abe J, Berk BC, Yan C : Role of phosphodiesterase 3 in NO/cGMP-mediated antiinflammatory effects in vascular smooth muscle cells. Circ Res 2003; 93: 406–413.
Bloomgarden ZT : Inflammation, atherosclerosis, and aspects of insulin action. Diabetes Care 2005; 28: 2312–2319.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, M., Ichiki, T., Ohtsubo, H. et al. Inhibition of Balloon Injury–Induced Neointimal Formation by Olmesartan and Pravastatin in Rats with Insulin Resistance. Hypertens Res 30, 971–978 (2007). https://doi.org/10.1291/hypres.30.971
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.30.971
Keywords
This article is cited by
-
Stimulation of endothelial progenitor cells: a new putative effect of several cardiovascular drugs
European Journal of Clinical Pharmacology (2010)