Abstract
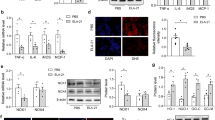
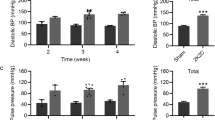
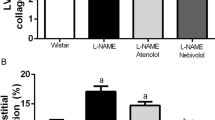
Although the lipophilicities of the various angiotensin II receptor blockers (ARBs) are very different, the relationship between lipophilicity and the protective effect against vascular remodeling is unclear. In this study, we compared the protective effects of a highly lipophilic ARB, telmisartan, and an ARB with low lipophilicity, losartan, on vascular function and oxidative stress in stroke-prone spontaneously hypertensive rats (SHR-SP). SHR-SP received oral placebo, 1 mg/kg telmisartan, or 10 mg/kg losartan for 2 weeks. The blood pressure (BP) in SHR-SP was significantly higher than that in Wistar-Kyoto (WKY) rats before treatment, and the BP was reduced equally in telmisartan- and losartan-treated SHR-SP compared to placebo-treated SHR-SP. Acetylcholine-induced vasorelaxation in isolated carotid arteries was significantly weaker in SHR-SP than in WKY rats, but in both telmisartan- and losartan-treated SHR-SP, acetylcholine-induced vasorelaxation was significantly higher than in placebo-treated SHR-SP. Moreover, acetylcholine-induced vasorelaxation in telmisartan-treated rats was significantly stronger than in losartan-treated SHR-SP. The expression of the endothelial nitric oxide synthase gene was significantly higher in telmisartan- and losartan-treated rats than in placebo-treated SHR-SP, and was significantly higher in telmisartan-treated rats than in losartan-treated rats. In contrast, the expression of the NAD(P)H oxidase subunit p22phox gene in telmisartan-treated SHR-SP was significantly lower than that in losartan-treated SHR-SP. Immunohistochemistry showed that angiotensin II expression in the aorta was significantly lower in telmisartan-treated SHR-SP than in losartan-treated SHR-SP. In conclusion, a highly lipophilic ARB, telmisartan, may be useful for preventing NAD(P)H oxidase activity, and thereby for conferring vascular protection.
Similar content being viewed by others
Article PDF
References
Unger T, Culman J, Gohlke P : Angiotensin II receptor blockade and end-organ protection: pharmacological rationale and evidence. J Hypertens Suppl 1998; 16: S3–S9.
Wienen W, Entzeroth M, van Meel JC, et al: A review on telmisartan: a novel, long-acting angiotensin II-receptor antagonist. Cardiovasc Drug Rev 2000; 18: 127–156.
Unger T, Ganten D, Lang RE, Scholkens BA : Persistent tissue converting enzymeinhibition following chronic treatment with Hoe498 and MK421 in spontaneously hypertensive rats. J Cardiovasc Pharmacol 1985; 7: 36–41.
Miyazaki M, Kawamoto T, Okunishi H : Vascular affinity of trandolapril. Am J Hypertens 1995; 8: 63S–67S.
Pilote L, Abrahamowicz M, Rodrigues E, Eisenberg MJ, Rahme E : Mortality rates inelderly patients who take different angiotensin-converting enzyme inhibitors after acute myocardial infarction: a class effect? Ann Intern Med 2004; 141: 102–112.
Takai S, Jin D, Sakaguchi M, Miyazaki M : Significant target organs for hypertension and cardiac hypertrophy by angiotensin-converting enzyme inhibitors. Hypertens Res 2004; 27: 213–219.
Jin D, Ueda H, Takai S, et al: Effect of chymase inhibition on the arteriovenous fistula stenosis in dog. J Am Soc Nephrol 2005; 16: 1024–1034.
Fukui T, Ishizaka N, Rajagopalan S, et al: p22phox mRNA expression and NADPH oxidase activity are increased in aortas from hypertensive rats. Circ Res 1997; 80: 45–51.
Ulker S, McMaster D, McKeown PP, Bayraktutan U : Impaired activities of antioxidant enzymes elicit endothelial dysfunction in spontaneous hypertensive rats despite enhanced vascular nitric oxide generation. Cardiovasc Res 2003; 59: 488–500.
Hamilton CA, Brosnan MJ, Al-Benna S, Berg G, Dominiczak AF : NAD(P)H oxidase inhibition improves endothelial function in rat and human blood vessels. Hypertension 2002; 40: 755–762.
Brosnan MJ, Hamilton CA, Graham D, Lygate CA, Jardine E, Dominiczak AF : Irbesartan lowers superoxide levels and increases nitric oxide bioavailability in blood vessels from spontaneously hypertensive stroke-prone rats. J Hypertens 2002; 20: 281–286.
van der Giet M, Erinola M, Zidek W, Tepel M : Captopril and quinapril reduce reactive oxygen species. Eur J Clin Invest 2002; 32: 732–737.
Pitt B, Poole-Wilson PA, Segal R, et al: Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial—the Losartan Heart Failure Survival Study ELITE II. Lancet 2000; 355: 1582–1587.
Cohn JN, Tognoni G : A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N Engl J Med 2001; 345: 1667–1675.
Pfeffer MA, McMurray JJ, Velazquez EJ, et al: Valsartan, captopril, or both in myocardial infarction complicated by heart failure, left ventricular dysfunction, or both. N Engl J Med 2003; 349: 1893–1906.
Julius S, Kjeldsen SE, Weber M, et al: Outcomes in hypertensive patients at high cardiovascular risk treated with regimens based on valsartan or amlodipine: the VALUE randomised trial. Lancet 2004; 363: 2022–2031.
McInnes GT : Angiotensin II antagonism in clinical practice: experience with valsartan. J Cardiovasc Pharmacol 1999; 33 ( Suppl 1): S29–S32.
Stopher DA, Beresford AP, Macrae PV, Humphrey MJ : The metabolism and pharmacokinetics of amlodipine in humans and animals. J Cardiovasc Pharmacol 1988; 12 ( Suppl 7): S55–S59.
Burnier M, Maillard M : The comparative pharmacology of angiotensin II receptor antagonists. Blood Press 2001; 1 ( Suppl): 6–11.
Lo MW, Goldberg MR, McCrea JB, Lu H, Furtek CI, Bjornsson TD : Pharmacokinetics of losartan, an angiotensin II receptor antagonist, and its active metabolite EXP3174 in humans. Clin Pharmacol Ther 1995; 58: 641–649.
Jinno T, Iwai M, Li Z, et al: Calcium channel blocker azelnidipine enhances vascular protective effects of AT1 receptor blocker olmesartan. Hypertension 2004; 43: 263–269.
Hashimoto Y, Kurosawa Y, Minami K, Fushimi K, Narita H : A novel angiotensin II-receptor antagonist, 606A, induces regression of cardiac hypertrophy, augments endothelium-dependent relaxation and improves renal function in stroke-prone spontaneously hypertensive rats. Jpn J Pharmacol 1998; 76: 185–192.
Kerr S, Brosnan MJ, McIntyre M, Reid JL, Dominiczak AF, Hamilton CA : Superoxide anion production is increased in a model of genetic hypertension: role of the endothelium. Hypertension 1999; 33: 1353–1358.
Kimoto-Kinoshita S, Nishida S, Tomura TT : Decrease of endothelial nitric oxide synthase in stroke-prone spontaneously hypertensive rat cerebral cortex. Neurosci Lett 2000; 288: 103–106.
Tanabe A, Naruse M, Seki T, et al: Gene expression of endothelin-1 and endothelial-type nitric oxide synthase in cardiovascular tissues of stroke-prone spontaneously hypertensive rats/Izm: effects of the angiotensin-converting enzyme inhibitor aracepril. J Cardiovasc Pharmacol 1998; 31 ( Suppl 1): S395–S398.
Umemoto S, Tanaka M, Kawahara S, et al: Calcium antagonist reduces oxidative stress by upregulating Cu/Zn superoxide dismutase in stroke-prone spontaneously hypertensive rats. Hypertens Res 2004; 27: 877–885.
Vaziri ND, Ni Z, Oveisi F : Upregulation of renal and vascular nitric oxide synthase in young spontaneously hypertensive rats. Hypertension 1998; 31: 1248–1254.
Crabos M, Coste P, Paccalin M, et al: Reduced basal NO-mediated dilation and decreased endothelial NO-synthase expression in coronary vessels of spontaneously hypertensive rats. J Mol Cell Cardiol 1997; 29: 55–65.
Seshiah PN, Weber DS, Rocic P, Valppu L, Taniyama Y, Griendling KK : Angiotensin II stimulation of NAD(P)H oxidase activity: upstream mediators. Circ Res 2002; 91: 406–413.
Ying CJ, Xu JW, Ikeda K, Takahashi K, Nara Y, Yamori Y : Tea polyphenols regulate nicotinamide adenine dinucleotide phosphate oxidase subunit expression and ameliorate angiotensin II-induced hyperpermeability in endothelial cells. Hypertens Res 2003; 26: 823–828.
Touyz RM, Yao G, Schiffrin EL : c-Src induces phosphorylation and translocation of p47phox: role in superoxide generation by angiotensin II in human vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 2003; 23: 981–987.
Touyz RM, Chen X, Tabet F, et al: Expression of a functionally active gp91phox-containing neutrophil-type NAD(P)H oxidase in smooth muscle cells from human resistance arteries: regulation by angiotensin II. Circ Res 2002; 90: 1205–1213.
Takai S, Sakonjo H, Miyazaki M : Beneficial effect of trandolapril on the lifespan of a severe hypertensive model. Hypertens Res 2001; 24: 559–564.
Morishita R, Higaki J, Nakamura F, et al: Regression of hypertension-induced vascular hypertrophy by an ACE inhibitor and calcium antagonist in the spontaneously hypertensive rat. Blood Press Suppl 1992; 3: 41–47.
Fernandez-Alfonso MS, Kreutz R, Zeh K, Liu Y, Ganten D, Paul M : Differential regulation of vascular angiotensin I-converting enzyme in hypertension. Hypertension 1994; 24: 280–286.
Wagner J, Drab M, Bohlender J, Amann K, Wienen W, Ganten D : Effects of AT1 receptor blockade on blood pressure and the renin-angiotensin system in spontaneously hypertensive rats of the stroke prone strain. Clin Exp Hypertens 1998; 20: 205–221.
Mizuno K, Niimura S, Katoh K, Fukuchi S : TCV-116, a newly developed angiotensin II receptor antagonist, induces regression of cardiac hypertrophy through suppression of the tissue renin-angiotensin system in spontaneously hypertensive rats. Life Sci 1994; 54: 1987–1994.
Izumi Y, Kim S, Murakami T, Yamanaka S, Iwao H : Cardiac mitogen-activated protein kinase activities are chronically increased in stroke-prone hypertensive rats. Hypertension 1998; 31: 50–56.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Takai, S., Kirimura, K., Jin, D. et al. Significance of Angiotensin II Receptor Blocker Lipophilicities and Their Protective Effect against Vascular Remodeling. Hypertens Res 28, 593–600 (2005). https://doi.org/10.1291/hypres.28.593
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.28.593
Keywords
This article is cited by
-
RETRACTED ARTICLE: Mechanisms Involved in Superiority of Angiotensin Receptor Blockade over ACE Inhibition in Attenuating Neuropathic Pain Induced in Rats
Neurotherapeutics (2020)
-
Powerful vascular protection by combining cilnidipine with valsartan in stroke-prone, spontaneously hypertensive rats
Hypertension Research (2013)
-
Renoprotective mechanisms of telmisartan on renal injury and inflammation in SHRSP.Z-Leprfa/IzmDmcr rats
Clinical and Experimental Nephrology (2013)
-
Comparative effect of olmesartan and candesartan on lipid metabolism and renal function in patients with hypertension: a retrospective observational study
Cardiovascular Diabetology (2011)
-
Candesartan and amlodipine combination therapy provides powerful vascular protection in stroke-prone spontaneously hypertensive rats
Hypertension Research (2011)