Abstract
Purpose: Congenital hyperinsulinism of infancy (OMIM# 256450) is a devastating disease most commonly caused by dominant or recessive mutations in either ABCC8 or KCNJ11, the genes that encode for the β-cell adenosine triphosphate-regulated potassium channel. A unique combination of a paternally inherited germline mutation and somatic loss-of-heterozygosity causes the focal form of the disease (Focal-congenital hyperinsulinism of infancy [Focal-CHI]), the incidence of which in genetically susceptible individuals is not known.
Methods: We genotyped 21,122 Ashkenazi Jewish individuals for two previously identified ABCC8 founder mutations and utilized a clinical database of 61 unrelated Ashkenazi patients with congenital hyperinsulinism of infancy to obtain an estimate of the risk of Focal-CHI in a genetically susceptible fetus.
Results: The combined mutation carrier rate in Ashkenazi Jews was 1:52, giving an estimated frequency of homozygosity or compound heterozygosity of 1:10,816 in this population. The risk of Focal-CHI is 1:540 per pregnancy in offspring of carrier fathers.
Conclusion: We recommend that these mutations be included in the genetic screening program for the Ashkenazi Jewish population. As the risk of Focal-CHI is not expected to be mutation specific, the data reported in this study are useful for counseling all families in which the father was found to carry a recessive ABCC8 or KCNJ11 mutation.
Similar content being viewed by others
Main
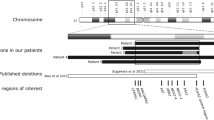
Congenital hyperinsulinism of infancy (CHI), also known as familial hyperinsulinemic hypoglycemia-1 (OMIM# 256450), is a devastating disease that can lead to irreversible brain damage if not diagnosed early and treated aggressively.1,2 The incidence of CHI has been estimated at approximately 1:30–40,000 live births in most populations,3,4 although much higher incidence rates have been reported in certain population isolates.4,5 To date, mutations in at least six different genes have been reported in patients with neonatal or infantile hyperinsulinism, although most are caused by mutations in one of the two genes that encode for the major components of the β-cell adenosine triphosphate (ATP)-regulated potassium channel (ABCC8 and KCNJ11). Although dominant inactivating mutations have been described in these genes, most of the mutations are recessive. In patients carrying two recessive mutations or a single dominant mutation, all pancreatic β-cells are affected and all hypersecrete insulin despite the presence of hypoglycemia (Diffuse-CHI). In contrast, some patients have a focal form of the disease in which a discrete region of adenomatous hyperplasia of β-cells is responsible for the abnormal insulin secretion. These patients carry a single, recessive ABCC8 or KCNJ11 mutation on the paternally inherited allele. A somatic mutation occurs in a pancreatic β-cell precursor during development resulting in loss of the normal maternal distal short arm of chromosome 11 causing an imbalance of imprinted genes such as IGF2, H19, and CDKN1C, all located in this region of chromosome 11. The mutant precursor, which lacks a normal ABCC8 or KCNJ11 allele, undergoes clonal expansion, resulting in a discrete focal region of β-cells lacking functional KATP channels.6,7 The clinical presentation of patients with Focal-CHI is similar to that of Diffuse-CHI, but in contrast to Diffuse-CHI, this form of the disease can be cured by selective resection of the focal lesion.8 The risk of Focal-CHI in an individual inheriting a recessive mutation is estimated to be low as the disease has not been reported in heterozygous siblings of patients with Diffuse-CHI caused by recessive gene mutations. A more precise estimate of risk is needed for genetic counseling in couples in which the father is known to carry an ABCC8 or KCNJ11 mutation.
In the Ashkenazi Jewish population, two founder mutations, c.3989-9g>a and p.F1387del, in the ABCC8 gene account for the majority of mutations found in patients with Diffuse- and Focal-CHI.9 In this study, we genotyped a large number of Ashkenazi Jewish individuals to determine the allele frequency of these two mutations and used these data to estimate the risk of Focal-CHI in genetically at-risk pregnancies.
MATERIALS AND METHODS
Peripheral blood samples were obtained with informed consent from individuals requesting carrier screening in the “Dor Yeshorim” program.10 This group included 21,122 individuals of Ashkenazi origin, 915 Jews of non-Ashkenazi (Sephardic) origin, and 1985 individuals of mixed origin (Ashkenazi and non-Ashkenazi). DNA was extracted from the blood samples and tested for the two mutations, c.3989-9g>a and p.F1387del, in the ABCC8 gene using allele-specific polymerase chain reaction. Amino acid and nucleotide numbering is based on alternative splice isoform Q09428-1. The corresponding numbers for the Q09428-2 isoform, which were frequently used in previous publications, are c.3992-9g>a and p.F1388del.
CHI patients
Anonymous data were obtained from the clinical database of Endocrinology and Metabolism Service, Hadassah Medical Center, where clinical testing for CHI mutation is routinely performed. The mutation status of all Ashkenazi Jewish patients with clinical diagnosis of CHI was recorded. CHI was diagnosed by the presence of hypoglycemia in the neonatal period associated with inappropriately elevated insulin levels, high glucose requirement, and, when available, increased glycemic response to glucagon. In families with multiple affected siblings, the sibling that was diagnosed first was selected for analysis. Although there were numerous families with multiple affected siblings each carrying two ABCC8 mutations, there were no families in which one individual had two ABCC8 mutations and another affected individual had only a single mutation. Similarly, there were no families with more than one affected individual carrying only a single ABCC8 mutation. Anonymous results of the genetic analyses were made available for this study.
Determination of Focal-CHI versus Diffuse-CHI
Because only a small minority of patients underwent pancreatectomy, the incidence of Focal-CHI was estimated by determining the excess prevalence of patients with a single paternally inherited mutation (see below).
Calculation of risk of Focal-CHI
All patients diagnosed with Focal-CHI were from unrelated families. The relative prevalence of presumed Focal-CHI was calculated by dividing the number of patients with a single paternally inherited mutation, minus the number of patients with a single maternally inherited mutation, by the total number of CHI probands. The risk of CHI in an individual who inherited an ABCC8 mutation on the paternal allele was calculated by dividing the prevalence of Focal-CHI by 0.5 × mutation carrier rate.
RESULTS
A total of 24,022 individuals were genotyped as part of premarital genetic testing (Table 1). Among the 21,122 Ashkenazi Jewish individuals genotyped, 351 were carriers of the mutation c.3989g>a and 55 of the mutation p.F1387del. None carried two mutant alleles. The combined mutation carrier rate for these two mutations was 1:52 (CI, 1:57-1:47). In the individuals of mixed ethnic background, 16 of 1985 were carriers of c.3989g>a, whereas none carried p.F1387del. Neither mutation was found in any of the Sephardic Jewish individuals tested.
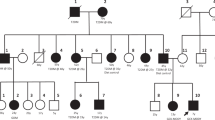
The genotypes of 61 unrelated Ashkenazi Jewish patients with CHI who underwent clinical testing in our laboratory were analyzed (Table 2). Most patients did not undergo surgery, so definitive diagnosis of Diffuse- or Focal-CHI was not possible. No mutations were identified in three cases, two of which had a phenotype that differed markedly from that typically seen in CHI patients with ABCC8 or KCNJ11 gene mutations. The third underwent comprehensive mutation analysis of all exons, exon-intron boundaries, and proximal promoter regions of ABCC8 and KCNJ11, as well as the coding sequences of GCK and SCHAD genes. As it is very likely that these three patients had disease caused by mutations in other, as yet unidentified, genes, these three patients were excluded from further analysis. Of the remaining 58 patients with ABCC8-CHI, two mutant alleles were identified in 40 patients, who were thus diagnosed with Diffuse-CHI (Table 2). In 18 patients, a single mutation was identified (14 c.3989-9g>a and 4 p.F1387del), which was inherited on the paternal allele in 17 and on the maternal allele in 1. The highly significant bias toward paternally inherited mutations (P = 0.007, Fisher exact test) suggests that most, if not all, of these individuals did have Focal-CHI. However, some of these patients may carry a second, unidentified mutation on the maternal allele and such an unidentified mutation could be inherited from the mother or the father at equal frequencies. Therefore, a conservative estimate of the number of Focal-CHI cases can be made by assuming that those with a single, maternally inherited mutation and an equal number of those with a single, paternally inherited mutation may carry an unidentified mutation in the other allele. As there was only one patient identified with a single, maternally inherited mutation, it can be estimated that 16 of 17 patients with paternal-only mutations have Focal-CHI, and the relative prevalence of Focal-CHI among all CHI patients is 16/58 = 0.276. This analysis also suggests that two founder mutations, c.3989-9g>a and p.F1387del, account for 97% of the CHI-associated ABCC8 mutations in the Ashkenazi population.
Because the combined allele frequency of the two founder mutations is 0.0096 (carrier rate = 1/52, CI, 1:57-1:47), the prevalence of Diffuse-CHI is estimated at ∼1:10,800 (CI, 1:13,211-1:8,984), and assuming that 50% of the mutation carriers inherited the mutant allele from the father, approximately 1:104 (CI, 1:115-1:95) are at risk of developing Focal-CHI. The actual prevalence of Focal-CHI can be calculated based on our finding described above that 27.6% of all CHI cases had presumed focal disease (absolute prevalence of Focal-CHI = 0.276 × [1/10,800]/[1 − 0.276] = 0.0000351 = 1:28,330 [CI, 1:34,680-1:23,584]). Thus, the risk of a fetus who carries a paternally inherited ABCC8 mutation actually developing CHI can be estimated by dividing the prevalence of Focal-CHI by the prevalence of paternally inherited ABCC8 mutation, yielding a risk of Focal-HI in a genetically susceptible fetus of 1:270 or 0.37% (CI, 0.33–0.40%).
DISCUSSION
In this study, we determined the carrier rate of two ABCC8 founder mutations in the Ashkenazi Jewish population.11 Because some of the patients with CHI have focal disease because of a single, paternally inherited mutation, knowledge of the mutant allele frequency is not sufficient to allow for effective genetic counseling. We therefore used our clinical database of Ashkenazi CHI patients to estimate the risk of Focal-CHI in a fetus carrying a paternally inherited ABCC8 mutation. This estimate is expected to be applicable to all ABCC8 and KCNJ11 mutations, not only those found in the Ashkenazi population.
The carrier rate of the two ABCC8 founder mutations (0.0083 for c.3989-9g>a mutation and 0.0013 for p.F1387del) in our Israeli study population is somewhat higher than that recently reported by Scott et al.12 in an Ashkenazi Jewish population based in New York City (0.006 and 0.0012, P = 0.016 for combined mutation rate). The reason for this difference is not clear, but may be spurious, because of the differences in sample size, or may reflect minor differences in the population base that seeks genetic counseling in the two countries.
Based on our data reported in this study, we estimate that the two founder mutations account for approximately 97% of the ABCC8 mutations in the Ashkenazi population. This estimate is higher than that previously reported by Nestorowicz et al.9 in 1996, because at the time of that publication, the existence of Focal-CHI and the genetic mechanism that causes this unique form of the disease were not known. Therefore, in that study, all patients with only a single mutation were assumed to carry another mutation on the second allele. In our study group of Ashkenazi Jewish patients with CHI, of those in whom only a single mutation was identified, in all but one the mutation was on the paternal allele. As it is extremely unlikely that this preponderance of paternally inherited mutations is due to chance (P = 0.007), the most likely explanation is that most, if not all, of these patients have Focal-CHI, and thus the maternally inherited allele is normal. As most patients with CHI treated in Israel are treated medically, we are unable to provide unequivocal proof of this. Recently, F-Dopa positron emission tomography scanning has been shown to reliably localize Focal-CHI13; however, this modality was only recently developed and is not currently available in Israel. Furthermore, radionuclide scanning is not ethically justified unless surgical intervention is contemplated.
One individual in our study population had classical, clinical CHI, yet inherited a single mutation on the maternal allele. This patient underwent full Sanger Sequencing of all exons, exon-intron boundaries, and the proximal promoters of both ABCC8 and KCNJ11. Although there are several possible explanations for this, we believe that the most likely explanation is that a second mutation was present on the paternal allele. This mutation could have been missed by the sequencing technique used, which is not 100% sensitive.14 Alternatively, variants under the primers used for sequencing or major deletions could have resulted in allele drop-out. An attempt to exclude this possibility was made using quantitative polymerase chain reaction; however, the sensitivity of the method used was not determined so that this possibility cannot be considered entirely excluded (data not shown). Another possibility is that this patient is mosaic for an interstitial recombination event that reduced a pancreatic precursor to maternal uniparental disomy at the ABCC8 locus without affecting the imprinted genes telomeric to this locus. Such a situation has been previously described, albeit with a paternally inherited mutation.15 For the purpose of our analysis in this study, we assumed that the paternal allele contained a mutation that was missed because we believe that this is the most likely situation and the most conservative approach when attempting to estimate the likelihood of Focal-CHI in patients with single, paternally inherited mutations.
To estimate the risk of Focal-CHI in an offspring of a couple where only the father carries a mutation, we made two assumptions. First, as no parent-of-origin preference is expected in Diffuse-CHI caused by an unidentified mutation on the second allele, and as it is highly unlikely that a single maternally inherited mutation alone could cause CHI, we assumed that for every affected individual with a single, maternally inherited mutation (and a hypothesized unidentified paternal mutation), there was one patient with an identified paternally inherited mutation who also had an unidentified mutation on the maternal allele. The remaining paternal-only single mutation cases were assumed to have Focal-CHI. Next, we assumed that maternal and paternal mutations are inherited equally, so that 50% of mutation carriers inherited their mutations from their fathers. This assumption was previously confirmed by testing unaffected family members of a subset of the patients with Diffuse-CHI (data not shown). Based on these assumptions and the data presented in this study, we estimate that the risk of Focal-CHI in a fetus carrying a paternally inherited mutation is approximately 0.0037 (1:270). The risk of Focal-CHI in offspring of couple in which the father carries a mutant allele is 1:540 per pregnancy because only 50% will inherit the mutant allele. This estimate is about twice that recently published by Ismail et al.16; however, in their calculations, these authors failed to take into consideration that only 50% of the mutation carriers have a mutation on their paternal allele and thus are at risk of Focal-CHI. Making this correction in their calculations, the risk of Focal-CHI in a carrier fetus of a paternally inherited ABCC8 mutation is 1:300, similar to our estimate (1:270).
Our data suggest that the two founder mutations studied here explain at least 97% of the mutations responsible for KATP gene mutation-associated disease in this population. Therefore, the residual risk of Diffuse-CHI because of KATP channel gene mutations is approximately 1:14,000 in a couple carrying only a single founder mutation and 1:12 × 106 in a couple not carrying either of the two founder mutations. Similarly, the risk of Focal-CHI due to an ABCC8 mutation other than these two founder mutations is extremely low in Ashkenazi Jewish couples. If the carrier rate of such unknown mutations is 0.029% (1:3500), the frequency of Focal-CHI caused by such a mutation can be estimated at 1.05 × 10−6 (1:950,000).
In addition to the residual risk of Diffuse-CHI and Focal-CHI described above, the possibility of phenocopies must be considered during genetic counseling. Mutations in at least four different genes (GLUD1, GCK, HADH, and SLC16A1) can cause hyperinsulinemic hypoglycemia in infancy and childhood. The incidence of disease caused by mutations in these four genes is not known, but in the Ashkenazi population, it is much lower than that of ABCC8 mutations. In our Ashkenazi patient population, we have identified only a single case of GLUD1-CHI and none with HADH- or GCK-CHI.
In the context of genetic counseling, the severity of the clinical disease must be considered. In this respect, the ABCC8 c.3989-9g>a mutation is unique, in that it has been associated with both very severe and very mild disease (Landau and Glaser, personal communication). Even within the same family, the disease severity can vary tremendously between haploidentical siblings. Another factor that must be considered is that this disease is treatable, and with early diagnosis and aggressive treatment a good long-term outcome is likely. Therefore, parents at risk of having a child with CHI may elect to continue a pregnancy. In this case, prenatal genetic diagnosis is still warranted, as prior knowledge of increased risk of an affected child will influence the perinatal care and can significantly improve long-term outcome. Fetal growth must be carefully monitored, and early delivery or elective cesarean section should be considered if macrosomia is diagnosed. Furthermore, intensive monitoring of blood glucose levels and aggressive treatment of hypoglycemia with intravenous glucose are needed immediately after birth to prevent irreversible brain damage. The decision of whether to attempt medical therapy or proceed with surgical therapy during the neonatal period is dependent on the clinical picture, including the family's ability to cope with intensive glucose management. A full discussion of this very difficult clinical dilemma is beyond the scope of this report.
In conclusion, we estimate that the carrier rate of CHI-associated founder mutations in the Ashkenazi Jewish population is 1:52. Given the severity of this disease, the potential long-term sequelae, and the good response to treatment if the diagnosis is made early and aggressive treatment initiated early, we recommend that Ashkenazi Jewish couples undergo testing for these two ABCC8 founder mutations as part of the genetic screening program designed for this population, even if pregnancy termination or preimplantation genetic diagnosis is not considered. To enhance cost-effectiveness, the prospective father should be tested first. If he is negative, then the risk of disease is extremely low and further testing is not warranted. If, however, the father is positive, the mother should be tested. If the mother is negative, the couple should be informed of the low but present risk of Focal-CHI. The very low risk to the fetus does not warrant prenatal testing of the fetus; however, if genetic testing is performed for other reasons, it is reasonable to test the fetus for the presence of the paternal ABCC8 mutation because this will differentiate between a fetus with a 1:270 risk and one with no risk at all of Focal-CHI. In pregnancies with a risk for Focal-CHI, as definitive prenatal genetic testing for Focal-CHI is not possible, clinical testing should be recommended as described earlier in the text. The risk of Focal-CHI in a genetically susceptible family is not expected to be mutation specific. Therefore, this information can be used to counsel all families in which an inactivating ABCC8 or KCNJ11 mutation was identified.
REFERENCES
Aynsley-Green A . Nesidioblastosis of the pancreas in infancy. Dev Med Child Neurol 1981; 23: 372–379.
Glaser B, Landau H, Permutt MA . Neonatal hyperinsulinism. Trends Endocrinol Metab 1999; 10: 55–61.
de Lonlay P, Fournet JC, Touati G, et al. Heterogeneity of persistent hyperinsulinaemic hypoglycaemia. A series of 175 cases. Eur J Pediatr 2002; 161: 37–48.
Otonkoski T, Ammälä C, Huopio H, et al. A point mutation inactivating the sulfonylurea receptor causes the severe form of persistent hyperinsulinemic hypoglycemia of infancy in Finland. Diabetes 1999; 48: 408–415.
Mathew PM, Young JM, Abu-Osba YK, et al. Persistent neonatal hyperinsulinism. Clin Pediatr (Phila) 1988; 27: 148–151.
Verkarre V, Fournet JC, de Lonlay P, et al. Paternal mutation of the sulfonylurea receptor (SUR1) gene and maternal loss of 11p15 imprinted genes lead to persistent hyperinsulinism in focal adenomatous hyperplasia. J Clin Invest 1998; 102: 1286–1291.
Ryan F, Devaney D, Joyce C, et al. Hyperinsulinism: molecular aetiology of focal disease. Arch Dis Child 1998; 79: 445–447.
Fékété CN, de Lonlay P, Jaubert F, Rahier J, Brunelle F, Saudubray JM . The surgical management of congenital hyperinsulinemic hypoglycemia in infancy. J Pediatr Surg 2004; 39: 267–269.
Nestorowicz A, Wilson BA, Schoor KP, et al. Mutations in the sulonylurea receptor gene are associated with familial hyperinsulinism in Ashkenazi Jews. Hum Mol Genet 1996; 5: 1813–1822.
Abeliovich D, Quint A, Weinberg N, et al. Cystic fibrosis heterozygote screening in the Orthodox Community of Ashkenazi Jews: the Dor Yesharim approach and heterozygote frequency. Eur J Hum Genet 1996; 4: 338–341.
Glaser B, Furth J, Stanley CA, Baker L, Thornton PS, Landau H, et al. Intragenic single nucleotide polymorphism haplotype analysis of SUR1 mutations in familial hyperinsulinism. Hum Mut 1999; 14: 23–29.
Scott SA, Edelmann L, Liu L, Luo M, Desnick RJ, Kornreich R . Experience with carrier screening and prenatal diagnosis for 16 Ashkenazi Jewish genetic diseases. Hum Mutat 2010; 31: 1240–1250.
Otonkoski T, Nantö-Salonen K, Seppänen M, et al. Noninvasive diagnosis of focal hyperinsulinism of infancy with [18f]-DOPA positron emission tomography. Diabetes 2006; 55: 13–18.
Bonnefond A, Durand E, Sand O, et al. Molecular diagnosis of neonatal diabetes mellitus using next-generation sequencing of the whole exome. PLoS One 2010; 5: e13630.
Hussain K, Flanagan SE, Smith VV, et al. An Abcc8 gene mutation and mosaic uniparental isodisomy resulting in atypical diffuse congenital hyperinsulinism. Diabetes 2008; 57: 259–263.
Ismail D, Smith VV, de Lonlay P, et al. Familial focal congenital hyperinsulinism. J Clin Endocrinol Metab 2011; 96: 24–28.
Acknowledgements
The authors thank the patients with CHI and their families for their help and cooperation over the past two decades, allowing them to obtain a better understanding of the genetic and clinical aspects of this disease.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure: The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Glaser, B., Blech, I., Krakinovsky, Y. et al. ABCC8 mutation allele frequency in the Ashkenazi Jewish population and risk of focal hyperinsulinemic hypoglycemia. Genet Med 13, 891–894 (2011). https://doi.org/10.1097/GIM.0b013e31821fea33
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1097/GIM.0b013e31821fea33