Abstract
Purpose: Genetic counseling may help counselees understand their genetic risk of developing breast/ovarian cancer. However, many studies have shown that their perception of their risks is inaccurate. Information-oriented variables often predicted the level of accuracy, focusing on specific processes of receiving and processing risks. We examined counselee-oriented predictors about how counselees embed cancer risks in their lives. These predictors reflect the personal meaning of genetic risks and are expected to explain/mediate the impact of genetic counseling on risk-perception-accuracy.
Method: We analyzed 248 questionnaires of a prospective study, filled in by probands with breast/ovarian cancer and pathogenic mutations, unclassified variants, or uninformative results (n = 30, 16, and 202, respectively). Mediation regression analyses were performed to examine whether counselee predictors mediated/explained the influence of information predictors on the accuracy. Information-oriented predictors regarded presentation format, communicated information, question format, education, pedigree information, cancer experience, and cognitive processes/heuristics. Counselee-oriented predictors regarded their self/personality, life/existence, and need for certainty about DNA test result, heredity, and cancer.
Results: Both information-oriented and counselee-oriented variables significantly predicted the accuracy of the counselees' risk perception, with moderate to large effect sizes. Counselee-oriented variables completely mediated/explained the effects of information-oriented variables on the accuracy.
Discussion: Counselees seemed to transform objective cancer risks into personally relevant information. Only through this personal meaning of genetic information, information-oriented processes seemed to cause inaccurate perceptions. Genetic counselors are suggested to focus communication on these personal processes.
Similar content being viewed by others
INACCURACY OF RISK PERCEPTION
Genetic counseling can be described as the “process of helping people understand and adapt to the medical, psychological, and familial implications of genetic contributions to disease.”1 This includes the communication of risk information and medical options based on these risks. These risks are calculated on the basis of a pathogenic mutation (PM) DNA test result, or on the basis of pedigree information, in combination with the counselees' cancer history.
On the basis of current literature, we can conclude that genetic counseling slightly improves the counselees' understanding of cancer risks. Overall, counselees seem to have a better perception after counseling than before counseling.2–4 However, Smerecnik et al.2 concluded in their review that only approximately 25% (range: 2–55%) of all counselees estimated their risk more correctly after counseling, from an average of 42% precounseling to an average of 58% postcounseling.2 On average, 25% (range: 5–76%) continued to overestimate and 19.5% (range: 7–55%) continued to underestimate their risk even after counseling.2 Others have concluded that women often have an inaccurate perception when their risk estimates are compared with objective estimate of their risk.5
Thus, many counselees do not bring their own subjective ideas and feelings about their own cancer risks in agreement with the actually communicated genetic information, i.e., the former differs from what has been communicated. Despite being inaccurate in many counselees, the perception of the communicated risks seems to be a better predictor of their medical decisions and distress than the actually communicated risks.6-8 Overestimations lead some individuals to inappropriate uptake of medical surveillance and preventive measures5,6,9,10 and poorer psychological functioning.6–9
PREDICTORS OF UNDERSTANDING
Because of the role of risk perception and its importance in predicting the impact of genetic counseling, it is relevant to understand how counselees create their own perception and especially why it deviates from the actual communicated risks. We differentiate between two kinds of possible causes of the inaccuracy: information-oriented and counselee-oriented predictors. Most previous studies have been information-oriented. Several studies suggest that this orientation should be broadened with counselee-oriented predictors (see “Counselee-oriented approach”).
Information-oriented predictors focus on how specific genetic information is communicated by the genetic counselor, how it is received, processed, and reproduced by the counselee, and how these processes are influenced by knowledge-related variables such as education and numeracy skills. These predictors focus on the processing of specific genetic information and not on broad and fundamental processes such as the counselees' personality, and integration of the DNA test results in their lives in general. In “Information-oriented approach: an overview of variables,” (see below) we describe the following information-oriented predictors: what information is communicated, levels of education and innumeracy, presence of specific information about cancer in relatives and in counselees, and specific cognitive processes regarding the processing of specific information.
Counselee-oriented predictors focus on how the genetic information is experienced and fundamentally embedded in the life of the counselee. In “Counselee-oriented approach,” we describe variables about the self, existential concerns, and need for certainty.
Counselee-oriented variables may be important in explaining why counselees have an inaccurate perception of their cancer risks. Counselees do not perceive their cancer risks from a cognitive, decontextualized distance but experience cancer risks as meaningful for themselves. We suggest that person-oriented predictors about the self, existence, and need for certainty influence their risk perception and its accuracy.
The difference between information-oriented and counselee-oriented predictors could also be described with the difference between the “function” and “meaning” of a process. Information-oriented predictors describe how the communication/receipt/inner processes function in counselees and the counselee-oriented predictors provide an understanding of the existential meaning of this information for the counselee (cf. difference between the spelling/grammar and the meaning of a sentence). In “Research questions,” we will hypothesize that counselee-oriented predictors explain (i.e., in statistical terms: “mediate”) why information-oriented variables influence the counselees' perception.
INFORMATION-ORIENTED APPROACH: AN OVERVIEW OF VARIABLES
Presentation format
The format in which cancer risks are presented by the genetic counselor may influence the accuracy of the counselees' perception.11–13 Genetic risks can be presented as proportions (X out of Y), percentages, and/or in graphical format; risks can be communicated as life-time risks or related to the current age of the counselee (residual risk, risk over the next 10 years) and can be mirrored (e.g., 80% at risk implies 20% not at risk).12 Genetic counselors prefer communication of numerical formats, but few studies provide empirical evidence for its efficacy.14 Explaining general figures of population risks may cause overestimation,15 counselees may feel a 50–50 risk,16 and the denominator of proportions are often inaccurately understood.16 Verbal labels or categories are interpreted too subjectively.16
Communicated information
Cancer risks may be perceived more accurately when a PM is communicated and not an uninformative result (UR) or unclassified variant (UV), but results are inconsistent.10,17–19 There is a large variation in the information communicated during genetic counseling sessions, which may influence risk perception.2 When family history, heredity, and personal risk estimates are all communicated, the counselees' perception of these risks (risk perception) is more accurate than when only the family history, heredity, or personal risk is communicated.2 However, we found that counselees may not be able to distinguish the meaning of the DNA test result from pedigree information,20 especially after the communication of ambiguous DNA test results such as UVs.10
Question format
In line with the presentation format as described earlier, also how risk perceptions are measured/formulated by the researcher (i.e., the instrument) may influence their accuracy.5 Katapodi et al.5 concluded in their review that the use of percentage scales causes larger differences between subjective and objective lifetime risk than Likert-type scales.5 This could be explained by the fact that categorical or Likert-type scales may be more in line with the counselees' own way of describing risks.21 However, percentage scales may result in the measurement of more accurate perception of 5-year risk.22 The accuracy could be improved by using scales with seven categories instead of visual analog scales,23 comparing own risks with general population risks,23–25 timing,9 and ordering risk items in the questionnaire correctly.26 Recent studies suggested that the counselees' medical decisions and distress are better predicted and confirm the counselees' own experiences, when the risk instruments do not only include cognitive items but also affective items,21 and focus on their interpretations.6,10,20
Information-related sociodemographics
Lower educated counselees are more unaware of their risks,5 and innumeracy may lead to misunderstanding.9,16,27,28
Family history
The majority of studies showed that counselees with a positive family history, defined as having at least one first or second-degree relative with breast cancer, were more likely to recall/interpret higher cancer risks than other women, irrespective of their communicated risks.5,29 It has been suggested that family history functions similar to an “availability heuristic.”29 Several risk perception studies included the number/percentage of affected and deceased relatives as predictors. In contrast, the counselee-centered “lived experience” and personal meaning of being a member of a family with many patients with cancer have received little attention.30,31
Cancer experience
Affected women seem to interpret their genetic risk in the context of their previous cancer experiences,32 such as recurrence of cancer, surgery, and current surveillance. The influence of the counselee-centered meaning of these medical facts on the counselees' perception has hardly been studied.
Cognitive processes
Risk perception accuracy has also been suggested to be influenced by cognitive information processes of counselees, such as appraisal, coping, and personal theories of inheritance.19,33 Many individuals think in non-Mendelian terms about genetics29 and use their own rule-of-thumb/heuristics and mental models of inheritance and causes of disease to interpret and assimilate the risk information they have received.34,35 Counselees have created their own cognitive and emotional representation of the causes, identity, timeline, cure/controllability, and consequences of hereditary breast/ovarian cancer.9 These representations may function independently from and/or parallel to rational, factual information,9,36 for instance, due to biases of availability, representativeness, anchoring, influence of incidences on risk perception, emotions, and emotional forecasting.16,37 Biases may help people to process information faster,33 cope with health problems, reduce stress,38,39 and defend themselves, their self-worth and self-integrity.36 However, the extent to which illness representations in counselees at increased risk differ from healthy individuals may be small.40
COUNSELEE-ORIENTED APPROACH
Possibly, previous studies have focused one sidedly on the communication of probabilities and have not sufficiently taken into account the personal context and meaning of genetic counseling for the counselee.41 When confronted with risk information, counselees have to translate the probabilistic statements into terms with personal meaning.42 “Taken together … risk information is rarely taken up as value neutral objective truth, but rather risk information is deeply subjective, interiorized against a preexisting sense of self.”43
In our previous studies, we developed questions to measure risk perception that reflected the counselees' own meaning-making process better, instead of risk perception questions that merely focused on the communication and linear psychological processing of probabilities. We asked counselees about their own interpretations of the meaning of the DNA test result for their cancer risks, regardless of what the genetic counselor has actually communicated.6–8,20,44 These interpretations were better predictors of their medical decisions and well-being than their recollections of what the genetic counselor had actually communicated.
Self
Counselees have to integrate the DNA test result flexibly in the general life story of who they are.45 They may ask questions about their sense of self such as: Am I a mutation carrier or not? Am I a potential cancer patient or not? And what does this mean? Does this change who I am? Communication of risks may influence/change their identity, and their identity may influence/change risk perception.46,47 A study in elderly counselees showed that their perception of genetic risks had been influenced by affect-related personality traits, such as extraversion, optimism, and locus of control.48 Other studies showed that trait optimism influenced risk perception.49
Existence
The counselees' self may be fundamentally involved in risk perception. Risk communication may evoke questions about existential concerns in life, such as death, freedom, responsibility, isolation, and meaninglessness.50 Existential feelings may be evoked, such as responsibility for undergoing and disclosing DNA testing to provide relatives with risk information,51–54 guilt about transmitting pathogenic genes to offspring,55 shame, and stigma.56,57 As a secondary appraisal process, counselees have to integrate, adjust, or accommodate the risk information in their general sense of meaning.58 Counselees have reported that obtaining certainty during the genetic counseling process had enhanced their lives59; 83% experienced at least one positive life change60 and 42% of counselees with UV results reported large changes in their existential view on life.10
Need for certainty
Counselees do not ask for DNA testing to understand probabilities accurately,59,61,62 but they want to receive information that provides them with certainty,34,59 e.g., about their own and their relatives' cancer risks, to know which medical decisions to make.59,61–64 However, DNA testing does not provide immediate certainty on demand. Counselees often have to wait for the results for a long time. DNA test result may be ambiguous, such as UV/URs. Surgery of ovaries and breasts may not be offered after UR/UV. Indeed, counselees have reported that many expectations about genetic counseling are not met.65–68 The counselees' need for certainty often collides with their perceived lack of certainty in the actual situation, causing uncertainty.33,69–75
The counselees' need for certainty seems to reflect how the DNA test result is embedded in their lives. Their unfulfilled need for certainty regarding the DNA test result, heredity likelihood, and cancer may influence how they perceive cancer risks. Counselees who do not receive certain genetic information may reinterpret this information in such ways that they do perceive certainty. Therefore, many counselees seem to value their own opinion more than the opinion of their genetic counselor.10,20
These counselee-oriented processes may also explain why the information-oriented processes influence their perception. That is, the presentation and question format, the communicated information, sociodemographics, and family history may influence the counselees' perception because of the meaning of this information for their selves, their existence, and fulfillment of their needs for certainty. The counselee-oriented processes may motivate them to use cognitive techniques; for instance, counselees with a large need for certainty but who perceived uncertainty over the DNA test result may distort the information in their perception to perceive certainty. In summary, we expect that counselee-oriented variables predict the accuracy of their perception with equal or larger effect sizes than information-oriented variables and completely mediate the effects of information-oriented variables on this accuracy.
RESEARCH QUESTIONS
-
1
Do counselee-oriented variables regarding the self, existence, and the unfulfilled need for certainty significantly predict the accuracy of the counselees' perception?
-
2
Is perception accuracy also significantly predicted by information-oriented predictors?
-
3
Do counselee-oriented variables significantly explain the effect of information-oriented variables on the accuracy of the counselees' perception; more specifically, when counselee-oriented variables are included, do the effects of the information-oriented variables on the accuracy of the counselees' risk perception become nonsignificant?
METHOD
Procedure and design
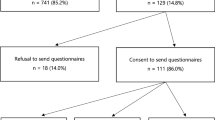
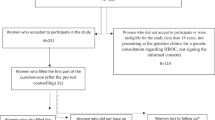
Eligible participants were women with breast and/or ovarian cancer who had requested a BRCA1/2 test in the period 2006–2009 at the Departments of Clinical Genetics of the Leiden University Medical Center, Maastricht University Medical Center, University Medical Central Groningen, Erasmus Medical Center Rotterdam, or the VU Medical Center Amsterdam. Eligible counselees received two questionnaires: immediately after the first genetic counseling session (T1) and 3 months after the second genetic counseling session in which the DNA test result was disclosed (T2). Usually, genetic counselors disclosed the following information: DNA test result category, heredity likelihood, cancer risks for female relatives and for the counselee, and risk management options (surgery, surveillance) for relatives and counselees, including the possibility for relatives to undergo DNA testing when applicable. Table 1 lists the most frequently communicated information; more details on procedure, design, and population are described elsewhere.8
Instruments
All instruments are presented for T2 only. Using counselee-oriented and/or information-oriented predictors at T1 yielded similar results (data not shown).
The accuracy of the counselees' risk perception was measured as difference between the counselees' interpretation of their own cancer risks and the cancer risks actually communicated by the genetic counselor. We decided to use their interpretations and not their recollections of cancer risks,20 because previous analyses in the same sample showed that their interpretations did not differ significantly from and correlated strongly with their recollections but did predict psychological and medical outcomes better than recollections.6,8 Interpreted cancer risks were measured by the question “regardless of what your genetic counselor has communicated, what are your own thoughts and ideas of your risks to develop cancer?” Counselees could answer on a 1–7 Likert scale ranging from 1 (not at risk) to 7 (complete at risk), which had the least number of missing values compared with percentage scales and showed the most accurate perception.6,20 Actual communicated risks had been derived from a checklist filled in after each session by the genetic counselor, medical files, and summary letters that counselees received within 3 months after the DNA result; actual risks were rescaled to the 1–7 Likert scale to match the counselees' interpretation. We used absolute difference scores (i.e., regardless of the direction of the difference) because of the explorative nature of the study, the small sample size, and missing values; moreover, unpresented data analyses did not show different results when we did not use absolute differences.
Items about the self were measured by the Ryff-well-being questionnaire, which was shown to be a reliable and valid scale to measure positive, existential well-being; we used the scales autonomy, mastery, vitality, inner strength, and self-acceptance.76–78 In addition, we used the Revised Life Optimism Scale to measure trait optimism, which was shown to be a reliable, valid instrument.79,80
Existential items were measured with the purpose-in-life-scale of the Ryff well-being scale.76–78 Further, we asked counselees to rate on three 1–7 Likert scales (1, very seldom and 7, very often): how often they had been wondering how many years they still have to live, what the meaning of their life is, and how often they actually experienced their life as meaningful during the last 2 weeks.
Need for certainty was measured with the Need for Structure Scale, which is a reliable, valid instrument to measure one's desire for structure and response to lack of structure.81 We asked them about the number of experiences with uncertainties in life before genetic counseling and the number of certainties; answers were given on 1–7 semantic differentials (1, little experiences and 7, many experiences). In another article, we describe how we developed items about the Unfulfilled Need for Certainty regarding the domains of DNA test result, heredity, cancer, and self (unpublished data). We asked counselees to rate on 7-point scales to what extent they wished to receive certainty about these domains; from this need for certainty, we subtracted the level of certainty that they perceived during last 2 weeks.
Information-oriented variables were developed on the basis of literature and of the experience of involved genetic counselors. Table 2 describes instruments for presentation format, communicated information, sociodemographics, family history, cancer experience, and cognitive processes. Specific coping styles were measured with the COPE83 regarding coping with the DNA test result. Regarding the question format, we only present Likert scales in this article. We have also asked counselees to recall and interpret their risks in percentage scales, and we compared this with actually communicated cancer risks; this did not result in different study outcomes.
Statistics
Missing values were imputed by using multiple imputation methods. Population variables are described with frequencies and means.
-
Question 1—We performed regression analyses with one counselee-oriented predictor (X) at a time (standardized β = R) to predict the perception accuracy (Y); because of multicollinearity and the relatively small sample, we could not use multiple predictor analyses.
-
Question 2—We did the same for information-oriented variables (X). Differences in X and Y between DNA test results (i.e., moderation) were tested with Kruskal-Wallis tests; DNA test results were included as moderators in regression analyses to test differences in the relationships between X and Y; only significant differences between DNA test results (i.e., moderation) are presented in this article, and otherwise, we show overall results.
-
Question 3—We did mediation analyses85,86 as we described elsewhere.6,8 We did one analysis for each information-oriented variable. The information-oriented variable was the predictor (X), and the predicted variable was the perception accuracy (Y). Mediators were the counselee-oriented variables (M). Mediation is assumed to be present when four criteria are met: (1) X and M correlate; (2) X predicts Y; (3) M predicts Y; and (4) when both X and M are included in prediction of Y, and we compare these results with criterion 2, the predictive value of X decreases (i.e., partial mediation) or becomes nonsignificant (i.e., complete mediation). For example, the communication of a UV result instead of PM/UR correlates with a strong unfulfilled need for certainty about the DNA test result (step 1); both the UV result and the unfulfilled need for certainty predict a more inaccurate perception (steps 2 and 3); and when the unfulfilled need for certainty is included in analyses, the UV result does not significantly predict the accuracy anymore, which suggests complete mediation (step 4).
We did multiple mediation analyses. First, we did mediation analyses with all counselee-oriented variables together as mediators, but for some information-oriented variables, this resulted in a very small number of participants per analysis due to missing values or multicollinearity. Second, we did mediation analyses with only autonomy, purpose in life, and unfulfilled need for certainty about the DNA test result together as mediators; these variables correlated strongest with both the significant information-oriented predictors and the accuracy; the number of participants per cell was large enough to calculate this. Third, we did analysis for each of these three counselee-oriented variables separately, to make the number of participants in each analysis as large as possible. For presentation purpose, we only present data with P values <0.01 and standardized β > 0.20 and only show tables for mediation criteria 2 and 3. Criterion 4 is not presented because we only found complete mediation. Significance level was defined as P < 0.01. This level reflected a balance between the explorative nature of this study (suggesting to set a high P value to avoid type II error) and the large number of tests (suggesting a low P value to avoid type I error).
RESULTS
Population
We approached 654 women who had undergone BRCA1/2 testing. Of them, 467 (71%) filled in the T1 questionnaire and 248 (53%) the T2 questionnaire. Mean time since cancer diagnosis was 5 years; 94% had had breast cancer and 6% ovarian cancer. Metastases were present in 26% of all participants. Before DNA testing, 56% had undergone symptomatic mastectomy, 6% symptomatic bilateral salpingo oophorectomy, and 5% presymptomatic bilateral salpingo oophorectomy. Mean age was 56 years, 42% had visited high school or higher, 84% were married, and 87% had children. More information is published elsewhere.8 Missing value analyses did not show significant results.
Counselee-oriented predictors
Self
Counselees had a more accurate perception when they were more autonomous, felt more mastery, vitality, self-acceptance, optimism, and inner strength. Effect sizes were moderate to large (Table 3).
Existence
Counselees perceived their cancer risks as more accurate when they had a stronger experience of purpose in life, less frequently wondered how many years they still can live and what the meaning in their life is, and currently experienced living a more meaningful life. Effect sizes were moderate to large.
Need for certainty
Counselees perceived their cancer risks as more accurate when they were more experienced with uncertainties in life, desired less structure, and reacted more positively to a lack of structure. Accuracy was also higher when counselees reported less needs for certainty, perceived more certainty, and experienced more fulfillment of their needs for certainty about cancer, DNA test result, and heredity. Effect sizes were moderate to large.
Information-oriented predictors
Table 4 presents the significant information-oriented predictors (P < 0.01; standardized β > 0.20).
Approximately half of the tested information-oriented variables were significant predictors (cf. Table 2). All significant effects were moderate to large.
Presentation format
The counselees' perception was more accurate when risks for UV/URs had not been communicated in words or in multiple formats. The perception was also more accurate when the cancer risks for UV/URs had not been mirrored (e.g., 80% at risk = 20% not at risk) and when these risks for PM results had been mirrored.
Communicated information
The counselees' perception was more accurate when a PM and not an UR or UV had been communicated, when cancer risks were higher, when counseling was face-to-face and a flyer had been provided, and when the possibility of finding an UV had been mentioned during the intake.
Cognitive processes
The higher the cancer risks and heredity likelihood were in the counselee's recollections and/or expectations, the more accurate was their risk perception. The perception was more accurate when counselees expected that the duration of their cancer would be shorter, cancer was less severe, and when they used active, accepting, priority taking, and planning coping styles, and did not use renaming or avoidance as coping.
Mediation analyses
When we included counselee-oriented variables as mediators (M) in regression analyses, information-oriented variables (X) did not significantly predict the level of accuracy of the counselees' perception any more (Y), and the counselee-oriented variables were the only significant predictors of Y (cf. Table 3). Information-oriented variables became nonsignificant when we used them as mediators. These results where measured with all counselee-variables, the three strongest variables (autonomy, purpose, and unfulfilled need for certainty about DNA test result), and each of these variables separately.
DISCUSSION
This study showed that both counselee-oriented and information-oriented variables predicted the accuracy of the counselees' risk perception. The amounts of variance explained by counselee-oriented and by information-oriented variables were similar (cf. Tables 3 and 4).
We found that several information-oriented variables influenced the accuracy of the counselees' risk perception. Counselees with UV/URs were less accurate than PM carriers, possibly because this information was less clear; communication of additional information in words and/or in multiple formats seemed to have confused these counselees even more (cf. Ref. 9). PM carriers and counselees with high risks (actually communicated and recalled) had a more accurate perception, possibly due to the clarity of pathogenic results which may be easier to perceive accurately. As expected, their perception was more accurate when counselees were younger,5 counseling was face-to-face, and flyers were provided.87 Moreover, counselees had a more accurate perception when they had active coping styles and did not have passive coping styles, negative expectations, and distress, which confirms other studies.15,87
The influence of information-oriented variables was completely mediated/explained by counselee-oriented variables. We found that the counselees' risk perception was directly influenced, and was completely mediated, by the following variables: positive existential personality characteristics, experience of meaning/purpose in life, previous experiences with uncertainties in life, their general need for structure, and their specific needs for certainty about the DNA test result, about heredity of cancer in their family, and about their own cancer. These counselee-oriented variables completely explained the effect of the information-oriented variables.
The information-oriented variables influenced the counselees' perception because they evoked a personal process in the counselee, which involved her self/personality, her existential concerns in life, and her needs regarding the DNA test result, her cancer, and the heredity of cancer in the family. For instance, the presentation format and the actual communicated DNA test result have influenced the counselees' risk perception, only by (i.e., through the mediation of) the personal and existential meaning that this information inherently has for the counselees. More specifically, the communication of a PM (i.e., information oriented) created a feeling of certainty over the genetic cause of cancer in the counselee (i.e., counselee oriented); subsequently, this feeling of certainty influenced the counselees' perception and created an indirect relationship between the communication of the PM and the perception.
The results also suggest that the counselees' cognitions, such as their cognitive illness representations, influence their risk perception through the personal and existential meaning of these cognitions. Thus, the counselees' risk perception is not determined by merely rationally knowing “I am at risk” but by the personal and existential meaning of knowing this. Thus, when counselees are confronted with risk information, they translate the probabilistic statements into terms with personal meaning42 and try to embed this information in the general story of their lives.45 By subjectively translating and embedding this information, counselees seem to distort the originally communicated cancer risks, i.e., creating their inaccurate perception.
Counselee-oriented approach
The counselee-oriented predictors that we propose in this article are not intended to replace the information-oriented predictors. Our approach is integrative and is intended to understand/explain how information-oriented processes do influence the accuracy of the counselees' risk perception. First, we described the impact of actual communicated genetic information on the counselees' perception and described how counselees function psychologically, such as using biases and heuristics. Subsequently, we explained by mediation analyses why counselees experienced these information-oriented influences.
We suggest that the perception of cancer risks is not a sum of decontextualized41 representations, biases, rules, or schemas. Risk perception is the result of a counselee putting the communicated risks in the lived experience and broad context of her life, which includes how she manages existential concerns and needs and what kind of person she is. Because of her fundamental needs, she may use cognitive techniques and misinterpret the communicated risks.
The counselee-oriented approach seems to be a less normative approach than the information-oriented approach. To be in line with other studies, we used the term “inaccurate perception.” However, words such as “inaccuracy” and “inadequate counseling” seem to suggest that the counselee and/or genetic counselor are “wrong.” However, even if a counselee may be “inaccurate” from an information-oriented point of view, she could feel justified from her own point of view and from her own needs and drives. Thus, having an inaccurate perception may not necessarily mean that counselees want to be provided with additional “correct information.” It could be argued that letting counselees have their own inaccurate perception, i.e., respecting their autonomy, may sometimes be more ethically justified than paternalistically forcing them “to think adequately.”
The counselee-oriented approach is in line with the general trend in psycho-oncology to pay more attention to the role of meaning and spirituality in patients with cancer.88 For instance, patients with cancer who experience meaning in life seem to be better adjusted to cancer.89–92 They also experience a better quality of life and well-being and up to 50% less depression.89,93–96 Terminal patients with high spiritual well-being also experience a lower desire for hastened death, less depression, and less suicidal ideation.94,97 Moreover, patients who are able to reengage in meaningful goals and focus on pleasant issues experience more positive affect.98 These meaning-making processes may be influenced by the way that physicians communicate with patients.99,100
Limitations and implications
Our study is based on a relatively small sample size in the moderately short follow-up time after DNA test result disclosure. The study may be biased by the fact that we have only included women affected with cancer. However, elements in their cancer history—such as having metastases—did not predict the level of accuracy of the counselees' perception and were also not significant as moderators in unpresented interaction analyses. We suggest replicating this study in other genetic disorders, in both sexes, and in patients affected and unaffected with cancer.
Subsequent studies should also focus on the social construction of the meaning of genetic information, because friends and relatives are part of the counselees' context and may influence their interpretations.16,101,102 Such social studies should not focus on the open communication of genetic information per se103 but on the experience and the meaning of this communication for the counselee, such as perceived social support. More counselee-oriented instruments could be developed and used. For instance, interview studies could be performed to ask counselees what the communicated information fundamentally means to them, similar to before-mentioned qualitative studies. Moreover, future studies should also examine which variables (dynamically) limit the counselee from sharing their subjective ideas and feelings in an information-driven counseling session.
Regression mediation analyses strongly indicated the presence of mediation effects but did not definitely prove this, because this was not an intervention study.104 However, the design of the study and the nature of the mediators made mediation likely.104 These mediation results confirmed our theoretical expectations and previous qualitative studies. T2 accuracy was predicted by T1 predictors. The communication of DNA test results did actually influence the mediators like an intervention (as described elsewhere).8 Questionnaires/items about the self also showed to be flexible instead of being an unchangeable trait, which would suggest moderation instead of mediation; because we found significant differences between T1 and T2 in the self-items (d > 0.4), suggesting that the DNA test result may have altered the counselees' self-experience which is in line with our hypotheses (cf. Refs. 42, 46, and 50). We suggest performing intervention studies to determine and influence these mediation effects.
From our counselee-oriented perspective, we suggest focusing on developing assessment instruments and interventions regarding the psychological/existential needs and motivations of counselees to undergo genetic counseling. Genetic counselors could explicitly ask counselees about their reasons to request DNA testing and assess the role of this request in their actual life situation.
Subsequently, genetic counselors could use this counselee-oriented assessment to explore together with counselees the decision to undergo DNA testing or not. DNA testing may not be suitable for all counselees in all personal/existential situations, and some counselees may first need psychological counseling. Different stages of readiness to undergo DNA testing may exist.105 For instance, does a counselee have (too) high expectations of DNA testing as a way to cope with her cancer? Could some of them benefit more from first referring them for intensive medical and/or psychological help to learn to live with cancer, instead of immediately undergoing DNA testing? When counselees receive counseling at an optimal stage, their perception of genetic information and its consequences may be better adjusted to the actual medical situation. Current theories and instruments about stages of readiness should be developed to include counselee-oriented elements.
The counselee-oriented assessment could also be used in tailoring the format of risk communication, for instance, by focusing on the personal consequences of the DNA test result.41 Such assessments before DNA testing could include the question how counselees think and feel about their cancer risks; the actual risks could be tailored to this pretesting risk perception. Such interventions seem to make the counselees' risk perception more accurate.106 To assess their understanding after DNA test result disclosure, counselees could be asked to repeat the communicated information in their own words. To explore their interpretations, counselees could be asked about “their own ideas and feelings, regardless of the communicated information” and about the medical consequences they have in mind.6,8,20
Counselees could be provided with additional information if necessary. However, as our study suggests, information provision alone cannot be expected to improve their perception much. Therefore, tailored risk communication may also include discussion of the fundamental subjective meaning that the DNA test result may have for counselees and the ways how they can embed the result in their lives. For instance, a counselee could explore together with her genetic counselor what she can do with this risk information, what she can tell her relatives, and how this information feels, and how she copes with uncertainty and vulnerability related to this result.
To help counselees in creating a realistic meaning of the DNA test result, it may be explained beforehand what counselees can realistically expect from genetic counseling and what not. This regards both medical and psychological aspects, including both certainties and uncertainties. Currently, patient information is often unbalanced in the Netherlands, because flyers and websites seem to pay much attention to certainties and little to uncertainties that may arise after DNA testing. Nuanced patient information could help counselees to have realistic expectations of the certainties they may obtain, which may subsequently improve their perception of the communicated information.
More rigorous interventions to improve the counselees-oriented variables include training in coping with hereditary cancer107 and (continue) finding meaning in life despite one's cancer experience, physical limitations, and (genetic) uncertainties.108 Several existential psychotherapeutic interventions for patients with cancer have been developed, showing moderate effects on distress and well-being109,110; these effect sizes are comparable with other psychological interventions for patients with cancer.111–113 More recent meaning-oriented interventions have shown to have large effects.108,114,115
Our advice to develop counselee-oriented interventions is in line with the review of Edwards et al.87 They showed that previous interventions, both information oriented and counselee oriented, have not been effective because of their information-oriented elements but because of their counselee-oriented elements, i.e., focus on emotions and support.87 It has been advised to develop genetic counseling into a personal, two-directional/reciprocal process116 with explicit focus on the counselee. This may help counselees in their search for certainty, may improve their perception of genetic information, and make their medical decisions more well informed.
REFERENCES
Resta R, Biesecker BB, Bennett RL, et al. A new definition of genetic counseling: National Society of Genetic Counselors' Task Force Report. J Genet Couns 2006; 15: 77–83.
Smerecnik CM, Mesters I, Verweij E, De Vries NK, de Vries H . A systematic review of the impact of genetic counseling on risk perception accuracy. J Genetic Couns 2009; 18: 217–228.
Meiser B, Halliday JL . What is the impact of genetic counselling in women at increased risk of developing hereditary breast cancer? A meta-analytic review. Soc Sci Med 2002; 54: 1463–1470.
Butow PN, Lobb EA, Meiser B, Barratt A, Tucker KM . Psychological outcomes and risk perception after genetic testing and counselling in breast cancer: a systematic review. Med J Aust 2003; 178: 77–81.
Katapodi MC, Lee KA, Facione NC, Dodd MJ . Predictors of perceived breast cancer risk and the relation between perceived risk and breast cancer screening: a meta-analytic review. Prev Med 2004; 38: 388–402.
Vos J, Gomez-Garcia EB, Oosterwijk JC, et al. Opening the psychological black box in genetic counseling. The psychological impact of DNA-testing is predicted by the counsellees' perception, the medical impact by the pathogenic or uninformative BRCA1/2-result. Psychooncology [ published online ahead of print November 10, 2010]. DOI: 10.1002/pon.1864.
Vos J, Jansen AM, Menko FH, van Asperen CJ, Stiggelbout AM, Tibben A . Family communication matters: the impact of telling relatives about non-pathogenic DNA-test results depends on the proband's non-verbal communication and the relatives' subjective perception. Genet Med 2011; 13: 333–341.
Vos J, Oosterwijk JC, Gomez-Garcia E, et al. Explaining the short-term impact of DNA-testing: the counselees' perception matters, the actual BRCA1/2-result does not. Patient Educ Couns [ published online ahead of print June 17, 2011]. DOI: j.pec.2011.04.017.
Sivell S, Elwyn G, Gaff CL, et al. How risk is perceived, constructed and interpreted by clients in clinical genetics, and the effects on decision making: systematic review. J Genet Couns 2008; 17: 30–63.
Vos J, Otten W, van Asperen C, Jansen A, Menko F, Tibben A . The counsellees' view of an unclassified variant in BRCA1/2: recall, interpretation, and impact on life. Psychooncology 2008; 17: 822–830.
Timmermans DR . What clinicians can offer: assessing and communicating probabilities for individual patient decision making. Horm Res 1999; 51: 58–66.
Ockhuysen-Vermey CF, Henneman L, van Asperen CJ, Oosterwijk JC, Menko FH, Timmermans DR . Design of the BRISC study: a multicentre controlled clinical trial to optimize the communication of breast cancer risks in genetic counselling. BMC Cancer 2008; 8: 283.
Waldron CA, Van der Weijden T, Ludt S, Gallacher J, Elwyn G . What are effective strategies to communicate cardiovascular risk information to patients? A systematic review. Patient Educ Couns 2011; 82: 169–181.
Henneman L, Marteau T, Timmermans DR . Clinical geneticists' and genetic counselors' views on the communication of genetic risks: a qualitative study. Patient Educ Couns 2008; 73: 42–49.
Timmermans DR, Ockhuysen-Vermey CF, Henneman L . Presenting health risk information in different formats: the effects on participants' cognitive and emotional evaluations and decisions. Patient Educ Couns 2008; 73: 443–447.
Klein WM, Stefanek ME . Cancer risk elicitation and communication: lessons from the psychology of risk perception. Cancer J Clin 2007; 57: 147–167.
Heshka JT, Palleschi C, Howley H, Wilson B, Wells PS . A systematic review of perceived risks, psychological and behavioral impacts of genetic testing. Genet Med 2008; 10: 19–32.
Dorval M, Gauthier G, Maunsell E, et al. No evidence of false reassurance among women with an inconclusive BRCA1/2 genetic test result. Cancer Epidemiol Biomarkers Prev 2005; 14: 2862–2867.
van Dijk S, Otten W, Timmermans DR, et al. What's the message? Interpretation of an uninformative BRCA1/2 test result for women at risk of familial breast cancer. Genet Med 2005; 7: 239–245.
Vos J, Oosterwijk JC, Gomez-Garcia EB, et al. Perceiving cancer-risks and heredity-likelihood in genetic-counseling: the analysis of the counselees' recollections and interpretations of BRCA1/2-test results. Clin Genet 2011; 79: 207–218.
van Dijk S, Otten W, van Asperen CJ, et al. Feeling at risk: how women interpret their familial breast cancer risk. Am J Med Genet A 2004; 131A: 42–49.
Schapira MM, Davids SL, McAuliffe TL, Nattinger AB . Agreement between scales in the measurement of breast cancer risk perceptions. Risk Anal 2004; 24: 665–673.
Eibner F, Barth J, Helmes A, Bengel J . Variations in subjective breast cancer risk estimations when using different measurments for assessing breast cancer risk perception. Health Risk Soc 2006; 2006: 2–197.
Woloshin S, Schwartz LM, Black WC, Welch HG . Women's perceptions of breast cancer risk: how you ask matters. Med Decis Making 1999; 19: 221–229.
Gurmankin Levy A, Shea J, Williams SV, Quistberg A, Armstrong K . Measuring perceptions of breast cancer risk. Cancer Epidemiol Biomarkers Prev 2006; 15: 1893–1898.
Taylor KL, Shelby RA, Schwartz MD, et al. The impact of item order on ratings of cancer risk perception. Cancer Epidemiol Biomarkers Prev 2002; 11: 654–659.
Hanoch Y, Miron-Shatz T, Himmelstein M . Genetic testing and risk interpretation: how do women understand lifetime risk results?. Judgment Decis Making 2010; 5: 116–123.
Wright AJ, Whitwell SC, Takeichi C, Hankins M, Marteau M . The impact of innumeracy on reactions to different graphic risk presentation formats: an experimental analogue study. Br J Health Psychol 2009; 14: 107–125.
Hopwood P . Breast cancer risk perception: what do we know and understand?. Breast Cancer Res 2000; 2: 387–391.
Revenson TA . A contextual approach to treatment decision making among breast cancer survivors. Health Psychol 2005; 24: 93–98.
Kenen R, Ardern-Jones A, Eeles R . Family stories and the use of heuristics: women from suspected hereditary breast and ovarian cancer (HBOC) families. Sociol Health Illn 2003; 25: 838–865.
Hallowell N, Foster C, Eeles R, Ardern-Jones A, Watson M . Accommodating risk: responses to BRCA1/2 genetic testing of women who have had cancer. Soc Sci Med 2004; 59: 553–565.
Etchegary H . Psychological aspects of predictive genetic-test decisions: what do we know so far?. Analyses Social Issues Public Policy 2004; 4: 13–31.
Shiloh S, Gerad L, Goldman B . Patient's information needs and decision-making processes: what can be learned from genetic counselees?. Health Psychol 2006; 25: 211–219.
McAllister M . Personal theories of inheritance, coping strategies, risk perception and engagement in hereditary non-polyposis colon cancer families offered genetic testing. Clin Genet 2003; 64: 179–189.
Etchegary H, Perrier C . Information processing in the context of genetic risk: implications for genetic-risk communication. J Genet Couns 2007; 16: 419–432.
Peters E, McCaul KD, Stefanek M, Nelson W . A heuristics approach to understanding cancer risk perception: contributions from judgment and decision-making research. Ann Behav Med 2006; 31: 45–52.
Decruyenaere M, Evers-Kiebooms G, Welkenhuysen M, Denayer L, Claes E . Cognitive representations of breast cancer. Emotional distress and preventive health behaviour: a theoretical perspective. Psychooncology 2000; 9: 528–536.
Shiloh S, Drori E, Orr-Urtregger A . Being ‘at-risk’ for developing cancer: cognitive representations and psychological outcomes. J Behav Med 2009; 32: 197–208.
Rees G, Fry A, Cull A, Sutton S . Illness perceptions and distress in women at increased risk of breast cancer. Psychol Health 2004; 19: 749–765.
Julian-Reynier C, Welkenhuysen M, Hagoel L, Decruyenaere M, Hopwood P, CRISCOM Working Group. Risk communication strategies: state of the art and effectivenes in the context of cancer genetics services. Eur J Hum Genet 2003; 11: 725–736.
Kavanagh AM, Broom DH . Embodied risk: my body, myself?. Soc Sci Med 1998; 46: 437–444.
Lee SJ . Uncertain futures: individual risk and social context in decision-making in cancer screening. Health Risk Soc 2010; 12: 101–117.
Vos J, Jansen AM, Menko FH, van Asperen CJ, Stiggelbout AM, Tibben A . A whisper-game perspective on the family communication of DNA-test results. Fam Cancer 2011; 10: 87–96.
Anderson G . Storytelling: a holistic foundation for genetic nursing. Holist Nurs Pract 1998; 12: 64–76.
Klitzman R . “Am I my genes?”: questions of identity among individuals confronting genetic disease. Genet Med 2009; 11: 880–889.
Robertson A . Embodying risk, embodying political rationality: women's accounts of risks for breast cancer. Health Risk Soc 2010; 2: 219–235.
Gerend MA, Aiken LS, West SG . Personality factors in older women's perceived susceptibility to diseases of aging. J Pers 2004; 72: 243–270.
Radcliffe NM, Klein WM . Dispositional, unrealistic, and comparative optimism: differential relations with the knowledge and processing of risk information and beliefs about personal risk. Pers Soc Psychol Bull 2002; 28: 836–846.
Langford IH . An existential approach to risk perception. Risk Anal 2002; 22: 101–120.
Hallowell N . Doing the right thing: genetic risk and responsibility. Sociol Health Illn 1999; 21: 597–621.
Agincourt-Canning L . Experiences of genetic risk: disclosure and the gendering of responsibility. Bioethics 2001; 15: 231–247.
Hallowell N, Foster C, Eeles R, Ardern-Jones A, Murday V, Watson M . Balancing autonomy and responsibility: the ethics of generating and disclosing genetic information. J Med Ethics 2003; 29: 74–79.
MacKenzie A, Patrick-Miller L, Bradbury AR . Controversies in communication of genetic risk for hereditary breast cancer. Breast J 2009; 15: S25–S32.
Tibben A, VegtervanderVlis M, Skraastad MI, et al. DNA-testing for Huntington's disease in the Netherlands—a retrospective study on psychosocial effects. Am J Med Genet 1992; 44: 94–99.
Esplen MJ, Stuckless N, Hunter J, et al. The development of a self-concept scale for BRCA1 and BRCA2 carriers. Psychooncology 2000; 9: S4.
Esplen MJ, Stuckless N, Hunter J, et al. The BRCA Self-Concept Scale: a new instrument to measure self-concept in BRCA1/2 mutation carriers. Psychooncology 2009; 18: 1216–1229.
Park CL, Folkman S . Meaning in the context of stress and coping. Rev General Psychol 1997; 1: 115–144.
Skirton H . The client's perspective of genetic counseling—a grounded theory study. J Genet Couns 2001; 10: 311–329.
Low CA, Bower JE, Kwan L, Seldon J . Benefit finding in response to BRCA1/2 testing. Ann Behav Med 2008; 35: 61–69.
van Asperen CJ, van Dijk S, Zoeteweij MW, et al. What do women really want to know? Motives for attending familial breast cancer clinics. J Med Genet 2002; 39: 410–414.
Brandt R, Hartmann E, Ali Z, Tucci R, Gilman P . Motivations and concerns of women considering genetic testing for breast cancer: a comparison between affected and at-risk probands. Genet Test 2002; 6: 203–205.
Klitzman RL . Misunderstandings concerning genetics among patients confronting genetic disease. J Genet Couns 2010; 19: 430–446.
Thorne S, Hislop TG, Kuo M, Armstrong EA . Hope and probability: patient perspectives of the meaning of numerical information in cancer communication. Qual Health Res 2006; 16: 318–336.
Davey A, Rostant K, Harrop K, oldblatt J, O'Leary P . Evaluating genetic counseling: client expectations, psychological adjustment and satisfaction with service. J Genet Couns 2005; V14: 197–206.
Foster C, Eeles R, Ardern-Jones A, Moynihan C, Watson M . Juggling roles and expectations: dilemmas faced by women talking to relatives about cancer and genetic testing. Psychol Health 2004; 19: 439–455.
Henneman L, Timmermans DR, van der Wal G . Public experiences, knowledge and expectations about medical genetics and the use of genetic information. Community Genet 2004; 7: 33–43.
Press NA, Yasui Y, Reynolds S, Durfy SJ, Burke W . Women's interest in genetic testing for breast cancer susceptibility may be based on unrealistic expectations. Am J Med Genet 2001; 99: 99–110.
Baty BJ, Dudley WN, Musters A, Kinney AY . Uncertainty in BRCAI cancer susceptibility testing. Am J Med Genet Part C Semin Med Genet 2006; 142C: 241–250.
Sammarco A . Perceived social support, uncertainty, and quality of life of younger breast cancer survivors. Cancer Nurs 2001; 24: 212–219.
Giarelli E . Spiraling out of control: one case of pathologic anxiety as a response to a genetic risk of cancer. Cancer Nurs 1999; 22: 327–339.
Smith JA, Michie S, Allanson A, Elwy R . Certainty and uncertainty in genetic counselling: a qualitative case study. Psychol Health 2000; 15: 1–12.
Bennett P, Wilkinson C, Turner J, et al. Psychological factors associated with emotional responses to receiving genetic risk information. J Genet Couns 2008; 17: 234–241.
Braithwaite D, Sutton S, Steggles N . Intention to participate in predictive genetic testing for hereditary cancer: the role of attitude toward uncertainty. Psychol Health 2002; 17: 761–772.
Cella D, Hughes C, Peterman A, et al. A brief assessment of concerns associated with genetic testing for cancer: the Multidimensional Impact of Cancer Risk Assessment (MICRA) questionnaire. Health Psychol 2002; 21: 564–572.
Ryff CD . Happiness is everything, or is it—explorations on the meaning of psychological well-being. J Pers Soc Psychol 1989; 57: 1069–1081.
van Dierendonck D . The construct validity of Ryff's Scales of Psychological Well-being and its extension with spiritual well-being. Pers Individ Dif 2004; 36: 629–643.
Schmutte PS, Ryff CD . Personality and well-being: reexamining methods and meanings. J Pers Soc Psychol 1997; 73: 549–559.
Scheier MF, Carver CS . Effects of optimism on psychological and physical well-being—theoretical overview and empirical update. Cogn Ther Res 1992; 16: 201–228.
Scheier MF, Carver CS, Bridges MW . Distinguishing optimism from neuroticism (and Trait Anxiety, Self-Mastery, and Self-Esteem)—a reevaluation of the life orientation test. J Pers Soc Psychol 1994; 67: 1063–1078.
Neuberg SL, Newsom JT . Personal need for structure: individual differences in the desire for simple structure. J Pers Soc Psychol 1993; 65: 113–131.
Weinman J, Petrie KJ, MossMorris R, Horne R . The illness perception questionnaire: a new method for assessing the cognitive representation of illness. Psychol Health 1996; 11: 431–445.
Kleijn WC, Van Heck GL, Van Waning A . Ervaringen met een Nederlandse bewerking van de COPE copingvragenlijst: de COPE-easy. Gedrag Gezondheid 2000; 28: 213–226.
Horowitz M, Wilner N, Alvarez W . Impact of event scale—measure of subjective stress. Psychosom Med 1979; 41: 209–218.
Baron RM, Kenny DA . The moderator mediator variable distinction in social psychological-research—conceptual, strategic, and statistical considerations. J Pers Soc Psychol 1986; 51: 1173–1182.
Preacher KJ, Hayes AF . Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behav Res Methods 2008; 40: 879–889.
Edwards A, Gray J, Clarke A, et al. Interventions to improve risk communication in clinical genetics: systematic review. Patient Educ Couns 2008; 71: 4–25.
Breitbart WS, Alici Y . Psycho-oncology. Harv Rev Psychiatry 2009; 17: 361–376.
Brady MJ, Peterman AH, Fitchett G, Mo M, Cella D . A case for including spirituality in quality of life measurement in oncology. Psychooncology 1999; 8: 417–428.
Thompson SC, Sobolewshubin A, Galbraith ME, Schwankovsky L, Cruzen D . Maintaining perceptions of control—finding perceived control in low-control circumstances. J Pers Soc Psychol 1993; 64: 293–304.
Taylor SE . Factors associated with meaning in life among people with recurrent cancer. Oncol Nurs Forum 1993; 20: 1399–1407.
Taylor SE . Adjustment to threatening events—a theory of cognitive adaptation. Am Psychol 1983; 38: 1161–1173.
McClain CS, Rosenfeld B, Breitbart W . Effect of spiritual well-being on end-of-life despair in terminally-ill cancer patients. Lancet 2003; 361: 1603–1607.
Nelson CJ, Rosenfeld B, Breitbart W, Galietta M . Spirituality, religion, and depression in the terminally ill. Psychosomatics 2002; 43: 213–220.
Lethborg C, Aranda S, Cox S, Kissane D . To what extent does meaning mediate adaptation to cancer? The relationship between physical suffering, meaning in life, and connection to others in adjustment to cancer. Palliat Support Care 2007; 5: 377–388.
Coward DD, Kahn DL . Transcending breast cancer: making meaning from diagnosis and treatment. J Holist Nurs 2005; 23: 264–283.
Breitbart WS, Rosenfeld B, Pessin H, et al. Depression, hopelessness and desire for death in terminally ill cancer patients. Psychosomatics 2001; 42: 194.
Schroevers M, Kraaij V, Garnefski N . How do cancer patients manage unattainable personal goals and regulate their emotions?. Br J Health Psychol 2008; 13: 551–562.
Chochinov HM . Dignity-conserving care—a new model for palliative care. JAMA 2002; 287: 2253–2260.
Chochinov HM, Hack TF, McClement S, Kristjanson LJ, Harlos M . Dignity in the terminally ill: a developing empirical model. Soc Sci Med 2002; 54: 433–443.
Hopwood P . Psychosocial aspects of risk communication and mutation testing in familial breast-ovarian cancer. Curr Opin Oncol 2005; 17: 340–344.
Kasper J, Geiger F, Freiberger S, Schmidt A . Decision-related uncertainties perceived by people with cancer—modelling the subject of shared decision making. Psychooncology 2008; 17: 42–48.
van Oostrom I, Meijers-Heijboer EJ, Duivenvoorden H, et al. Family system characteristics and psychological adjustment to cancer susceptibility genetic testing: a prospective study. Clin Genet 2007; 71: 35–42.
MacKinnon DP, Krull JL, Lockwood CM . Equivalence of the mediation, confounding and suppression effect. Prev Sci 2000; 1: 173–181.
O'Neill SC, Peters JA, Vogel VG, Feingold E, Rubinstein WS . Referral to cancer genetic counseling: are there stages of readiness?. Am J Med Genet Part C Semin Med Genet 2006; 142C: 221–231.
Stam P, Van der Looiu E, Voorendt M, Van der Burgt I, Hoogerbrugge N . Overestimated lifetime cancer risk can be reduced by feedback on preexisting estimation. Eur J Hum Genet 2010; 18.
Landsbergen K, Verhaak C, Kraaimaat F, Hoogerbrugge N . Genetic uptake in BRCA-mutation families is related to emotional and behavioral communication characteristics of index patients. Fam Cancer 2005; 4: 115–119.
Breitbart W, Rosenfeld B, Gibson C, et al. Meaning-centered group psychotherapy for patients with advanced cancer: a pilot randomized controlled trial. Psychooncology 2010; 19: 21–28.
Henoch I, Danielson E . Existential concerns among patients with cancer and interventions to meet them: an integrative literature review. Psychooncology 2009; 18: 225–236.
LeMay K, Wilson KG . Treatment of existential distress in life threatening illness: a review of manualized interventions. Clin Psychol Rev 2008; 28: 472–493.
Lepore SJ, Coyne JC . Psychological interventions for distress in cancer patients: a review of reviews. Ann Behav Med 2006; 32: 85–92.
Williams S, Dale J . The effectiveness of treatment for depression/depressive symptoms in adults with cancer: a systematic review. Br J Cancer 2006; 94: 372–390.
Trijsburg RW, van Knippenberg FC, Rijpma S . Effects of psychological treatment on cancer patients: a critical review. Psychosom Med 1992; 54: 489–517.
Chochinov HM, Hack TF, Hassard T, Kristjanson LJ, McClement S, Harlos M . Dignity therapy: a novel psychotherapeutic intervention for patients near the end of life. J Clin Oncol 2005; 23: 5520–5525.
Kang K-A, Im J-I, Kim H-S, Kim S-J, Song M-K, Sim S . The effect of logotherapy on the suffering, finding meaning, and spiritual well-being of adolescents with terminal cancer. J Korean Acad Child Health Nurs 2009; 15: 136–144.
McCarthy Veach P, Bartels DM, LeRoy BS . Coming full circle: a reciprocal-engagement model of genetic counseling practice. J Genet Couns 2007; 16: 713–728.
Acknowledgements
This work was supported by the Dutch Cancer Society (Grant no. UL2005-3214).
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure: The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Vos, J., Stiggelbout, A., Oosterwijk, J. et al. A counselee-oriented perspective on risk communication in genetic counseling: Explaining the inaccuracy of the counselees' risk perception shortly after BRCA1/2 test result disclosure. Genet Med 13, 800–811 (2011). https://doi.org/10.1097/GIM.0b013e31821a36f9
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1097/GIM.0b013e31821a36f9
Keywords
This article is cited by
-
Cancer patients’ understandings of genetic variants of uncertain significance in clinical care
Journal of Community Genetics (2022)
-
Communication about genetic testing with breast and ovarian cancer patients: a scoping review
European Journal of Human Genetics (2019)
-
How Can We Reach At-Risk Relatives? Efforts to Enhance Communication and Cascade Testing Uptake: a Mini-Review
Current Genetic Medicine Reports (2018)
-
Emotional impact on the results of BRCA1 and BRCA2 genetic test: an observational retrospective study
Hereditary Cancer in Clinical Practice (2017)
-
Population-based genetic risk prediction and stratification for ovarian cancer: views from women at high risk
Familial Cancer (2015)