Abstract
Purpose: To evaluate the safety and efficacy of recombinant human iduronate-2-sulfatase (idursulfase) in the treatment of mucopolysaccharidosis II.
Methods: Ninety-six mucopolysaccharidosis II patients between 5 and 31 years of age were enrolled in a double-blind, placebo-controlled trial. Patients were randomized to placebo infusions, weekly idursulfase (0.5 mg/kg) infusions or every-other-week infusions of idursulfase (0.5 mg/kg). Efficacy was evaluated using a composite endpoint consisting of distance walked in 6 minutes and the percentage of predicted forced vital capacity based on the sum of the ranks of change from baseline.
Results: Patients in the weekly and every-other-week idursulfase groups exhibited significant improvement in the composite endpoint compared to placebo (P = 0.0049 for weekly and P = 0.0416 for every-other-week) after one year. The weekly dosing group experienced a 37-m increase in the 6-minute-walk distance (P = 0.013), a 2.7% increase in percentage of predicted forced vital capacity (P = 0.065), and a 160 mL increase in absolute forced vital capacity (P = 0.001) compared to placebo group at 53 weeks. Idursulfase was generally well tolerated, but infusion reactions did occur. Idursulfase antibodies were detected in 46.9% of patients during the study.
Conclusion: This study supports the use of weekly infusions of idursulfase in the treatment of mucopolysaccharidosis II.
Similar content being viewed by others
Main
Mucopolysaccharidosis (MPS) II (Hunter syndrome) is an X-linked, lysosomal storage disease that is caused by a deficiency in iduronate-2-sulfatase (I2S), the lysosomal enzyme that catalyzes a step in the catabolism of glycosaminoglycans (GAG).1 MPS II occurs predominantly in males1 and has a reported incidence of typically >1 in 100,000 live births.2–5 The mutations responsible for the I2S enzyme deficiency range from missense and nonsense mutations to small insertions/deletions or complete deletion of the I2S gene6–10 located at Xq28.11
The phenotype of MPS II, which is thought to be due to accumulation of GAG within tissues and organs, includes developmental delay, hearing loss, enlarged tongue, abnormal dentition, upper airway obstruction, hepatosplenomegaly, valvular heart disease, decreased joint range of motion, short stature and skeletal deformities.1 Phenotypic expression varies considerably, with some patients exhibiting somatic involvement between two and four years of age with variable neurologic involvement leading to mental impairment.1 In these patients death occurs in the first or second decade of life, usually due to neurological complications associated with obstructive airway disease and/or cardiac failure.1 Other patients have minimal neurological involvement and survive into adulthood with normal intelligence, yet still exhibit joint, airway, and cardiac disease.1
Although the management of MPS II remains palliative, pre-clinical experiments with a mouse model of MPS II suggested that enzyme replacement therapy with I2S may be effective in reducing tissue GAG stores.12 The results of the Phase I/II initial clinical study of enzyme replacement therapy (ERT) with recombinant human I2S (idursulfase, Shire Human Genetic Therapies, Inc., Cambridge, MA) in 12 patients with MPS II showed persistent decreases in urinary GAG excretion and liver and spleen size (unpublished data, 2006). In this report the results of the randomized, double-blind, placebo-controlled Phase II/III clinical trial of idursulfase are presented and show that in addition to reducing organ size and urinary GAG excretion, weekly infusions of idursulfase increase walking distance and improve pulmonary function in MPS II patients.
MATERIALS AND METHODS
Patients
Patients between the ages of 5 and 31 years with a diagnosis of MPS II based on both clinical and biochemical criteria were enrolled in the study. Clinical criteria included having any one of the following MPS II-related abnormalities: hepatosplenomegaly, radiographic evidence of dysostosis multiplex, valvular heart disease, or evidence of obstructive airway disease. The biochemical evidence of MPS II included a documented deficiency in I2S enzyme activity of ≤10% of the lower limit of the normal range as measured in plasma, fibroblasts, or leukocytes combined with a normal enzyme activity level of another sulfatase. At baseline all patients were required to reproducibly perform pulmonary function testing and have an abnormal forced vital capacity (FVC) of <80% of predicted. Patients who had a tracheostomy or who had received a bone marrow or cord blood transplant were excluded from the study. All adult patients or the parents or guardians of patients under 18 years old gave written informed consent prior to enrollment.
Study design
This study was a randomized, double-blind, placebo-controlled, multicenter, multinational clinical trial. The study was conducted in compliance with international guidelines and appropriate local country regulations. The protocol and informed consent documents were reviewed and approved by the institutional review board and/or independent ethics committee at each site conducting the study. Adherence to good clinical practice in this international trial was achieved by having a standardized protocol, an investigators' brochure, an operational manual with detailed instructions on how to perform each assessment, an investigators' meeting prior to starting the trial reviewing all procedures and assessments, an initiation visit at each site by the sponsor with all local site study staff, a separate physical therapy training session, and ongoing independent monitoring to maintain the quality of data collected.
Patients were enrolled and randomized equally to 1 of 3 treatment arms: intravenous infusions of idursulfase either weekly or every-other-week (EOW) at a dose of 0.5 mg/kg, or weekly infusions of placebo. Patients randomized to EOW idursulfase dosing received placebo infusion during intervening weeks to maintain blinding. Randomization was stratified by age at baseline (strata of 5–11, 12–18, and 19–31 years) and by total disease score at baseline. Baseline disease score was calculated using the baseline results of the six-minute walk test (6MWT) and the percent predicted FVC (%FVC) as presented in Table 1.
Idursulfase
Idursulfase is produced at Shire Human Genetic Therapies, Inc., Cambridge, MA, using genetic engineering in a continuous human cell line that yields a glycosylated protein analogous to the native human enzyme. The idursulfase-producing cell line was generated by transfecting HT-1080 cells with an expression plasmid encoding the 550 amino acids of human iduronate-2-sulfatase, including a 25 amino acid signal sequence, which is cleaved in the secreted protein. The purified protein is >99.9% pure as assessed by a number of chromatographic and electrophoretic assays. The eight N-linked glycosylation sites are fully occupied and consist of two bis mannose-6-phosphate (M6P) containing glycans that enable high affinity receptor mediated cell uptake and targeting to the lysosomes via M6P receptors. In addition, purified idusulfase contains complex highly sialylated glycans that prolong the circulating half-life of the enzyme. The extent of post-translational modification of cysteine 59 to formylglycine, which is required for enzymatic activity, is approximately 50%.
Idursulfase was administered at a dose of 0.5 mg/kg diluted in normal saline to yield a total volume of 100 mL. Infusions were given over a three-hour period, starting at an infusion rate of 8 mL/h and increasing stepwise as follows: 16 mL/h at 15 minutes, 24 mL/h at 30 minutes, 32 mL/h at 45 minutes, and 40 mL/h at 60 minutes. Patients were closely monitored during each infusion and were discharged one hour after completing each infusion, provided that they remained clinically stable.
If a patient developed an infusion reaction (typically involving chills, fever, headache, and/or flushing) during an infusion, the investigator decided whether the infusion was to be terminated or continued. The first time that a patient had an infusion reaction, the infusion was typically stopped and not restarted. For subsequent infusions, patients were pre-medicated with antihistamines and/or corticosteroids and, if the reactions still occurred the infusion was stopped and restarted after the reaction resolved (typically 15–45 minutes) in a clinically stable patient. When subsequent infusions were without incident, pre-medications could be tapered.
Efficacy assessment
The primary efficacy assessment was a comparison between the placebo and weekly idursulfase group for the change from baseline to Week 53 in a single, two-component composite variable combining %FVC as a measure of respiratory function and 6MWT as a measure of physical functional capacity using the O'Brien procedure for analysis (see below).13 FVC was measured by spirometry according to standard methods, using the best effort of three determinations as the measure of FVC for that day.14,15 Two tests, typically one day apart, were performed during each evaluation and the best effort was used as the result for all analyses. FVC was expressed as percent predicted of normal, which was calculated based on published reference values that are based on current standing height and age.16,17 The 6MWT was conducted according to American Thoracic Society guidelines18 and measured the distance of unassisted walking achieved during six minutes. Patients walked back and forth between marks placed 15 m apart, and the total distance was recorded by an observer. Two tests, typically one day apart, were performed during each evaluation and the further distance was used as the result for all analyses. Both the pulmonary function test and the 6MWT were conducted by a professional who was not involved with any other aspects of the trial, usually a pulmonary function specialist and physical therapist, respectively.
Secondary efficacy variables included changes in the individual components of the composite endpoint (6MWT distance and %FVC), absolute FVC, liver and spleen volumes measured by abdominal MRI, urine GAG excretion and passive joint range of motion.
All measurements were made at baseline and at Weeks 18, 36, and 53. Urine GAG was measured by the method of De Jong et al.19 Hepatomegaly was defined as a liver volume (L) >3.5% of body weight (kg) in patients aged 5–12 years, >2.2% of body weight in patients aged 13–17 years, and >2.6% in patients more than 18 years old.20 Splenomegaly was defined as having a splenic volume greater than the 95th percentile of the normal distribution in children.21 Liver and spleen volumes were determined by magnetic resonance imaging (MRI) using the same imaging protocol at all sites. MRI images were sent to Bio-Imaging Technologies, Inc, Newtown, PA for determination of liver and spleen volumes. The error of repeated measure in determining liver and spleen volumes by MRI was 3–5% between observers. Passive joint range of motion was measured by a physical therapist using a goniometry on two different days at each evaluation visit. The joint measurements obtained on both days were averaged.
Safety assessments
A clinical assessment was done at every infusion visit. A physical examination, which included measurement of vital signs, height, weight, serum chemistry, complete blood count (CBC), urinalysis, and an electrocardiogram were performed every four months. Adverse events were monitored and recorded throughout the study. An infusion-related adverse event was defined to have occurred if the event occurred within the day after the infusion, began during or after the infusion, and was judged by the investigator to be possibly or probably related to study treatment. Blood samples were taken at baseline and periodically thereafter for measurement of serum idursulfase antibodies. Anti-idursulfase antibodies in plasma were detected by enzyme-linked immunosorbent assay (ELISA) and positive results were confirmed by radioimmunoprecipitation (RIP). If the initial screen was positive, the titer was determined by antibody titration. The assay sensitivity was approximately 135 μg/mL anti-idursulfase IgG for ELISA, and approximately 10.4 μg/mL anti-idursulfase IgG for RIP.
Analyses of results
The change from baseline to Week 53 in %FVC and 6MWT for each patient was calculated. Within each parameter the changes were ranked irrespective of treatment group, with the lowest change value assigned a rank of 1, the next lowest a rank or 2, and so forth. The two-component composite score for each patient was calculated by summing the ranks of the two individual components according to the procedure described by O'Brien.13 In the intent-to-treat (ITT) population (defined as all randomized patients), the treatment groups were compared using analysis of covariance on the sum of the ranks with the treatment groups and study region (North America, South America, Europe) fitted as factors and baseline patient age (3 stratification levels) and baseline disease score (3 stratification levels: scores 2, 3 or 4, 5 or 6) as covariates. Missing values were imputed using last rank carried forward. The primary comparison for the determination of idursulfase efficacy was between the placebo group and the weekly idursulfase group. Secondary endpoints were similarly analyzed by analysis of covariance, using last observation carried forward to impute missing values. Calculations were performed with SAS, Version 8.2 (Cary, NC). All values are expressed as mean ± standard error of the mean (SEM).
RESULTS
Study population
A total of 121 patients were screened for enrollment, and 96 eligible patients were randomized into the 3 treatment groups. Of the 25 patients who were not enrolled in the study, 19 had FVC >80% of predicted, 14 were unable to perform the testing required in the study, and 10 were unable to comply with or unlikely to complete the protocol (note that patients could have more than one reason for exclusion). Demographics and baseline characteristics of the randomized study participants are shown in Table 1. The groups were well balanced with respect to age, time since diagnosis of MPS II, and baseline disease characteristics.
Ninety-four (97.9%) of 96 patients completed 1 year of treatment. The two patients who did not complete one year of treatment died during the study: one patient in the placebo group and one patient in the idursulfase weekly group. Neither death was considered by the investigator to be related to the study drug (details presented below in Safety section). Treatment compliance was good; 44 patients (45.8%) received all planned infusions, and an additional 24 (25.0%) missed only one infusion. With the exception of the premature deaths, all patients received at least 80% of planned infusions, and no patient missed more than 4 consecutive infusions during the study. All patients completing the double-blind study elected to continue in the open-label extension study.
Primary efficacy outcome
The two-component composite score of the idursulfase 0.5 mg/kg weekly group was significantly higher than in the placebo group in the intent-to-treat population (treatment difference = 18.96 ± 6.47, P = 0.0049). A smaller difference was found for the idursulfase EOW compared to placebo groups in the intent-to-treat population (treatment difference = 12.86 ± 6.17, P = 0.0416). The responses between the two idursulfase treatment groups were not significantly different (treatment difference = 10.84 ± 7.11, P = 0.1329). Treatment effects based on the sum of ranked changes were seen in all age groups for both idursulfase weekly and EOW. These analyses were not significantly influenced by baseline age strata.
6MWT and FVC
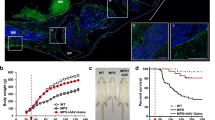
The effect of treatment on 6MWT distance and %FVC during the study are presented in Figure 1 and Table 2. After 53 weeks of treatment with weekly infusions of idursulfase (0.5 mg/kg), 6MWT distance was significantly increased compared to placebo (44.3 ± 12.3 m versus 7.3 ± 9.5 m, P = 0.0131). A smaller increase in walking distance was found for the idursulfase EOW group (30.3 ± 10.3 m) compared to the placebo group (P = 0.0732). After 53 weeks, %FVC had increased more in the weekly idursulfase group than in the placebo group (Table 2), with this difference approaching statistical significance (P = 0.0650). No difference was seen between idursulfase EOW and placebo (Table 2). Absolute FVC was however significantly increased from baseline in the weekly dosing group (0.22 ± 0.05 L) compared to both the placebo (0.06 ± 0.03 L, P = 0.0011) and EOW groups (0.07 ± 0.03 L, P = 0.0176) after 53 weeks (Fig. 2, Table 2).
The effect of treatment with idursulfase on 6MWT distance and %FVC in MPS II. All values are the observed means ± SEM. aP = 0.0131 compared with placebo at Week 53 (ANCOVA). N = 32 in each group. Two points at Week 18 are offset slightly for clarity. %%FVC, % predicted forced vital capacity; EOW, every-other-week.
Liver and Spleen Volumes
At baseline, liver volumes were similar in the three groups (Table 1). In addition, the number of patients with hepatomegaly at baseline was similar among the treatment groups (placebo, 23; idursulfase weekly, 25; idursulfase EOW, 25). Liver volume decreased by over 20% after 18 weeks of treatment in both idursulfase groups, whereas it remained unchanged in the placebo group. After 53 weeks in the ITT population, liver volume had decreased from baseline by 25.3 ± 1.6% in the idursulfase weekly group and by 24.0 ± 1.7% in the idursulfase EOW group (Table 2). The change in both groups was statistically significantly greater than the change in the placebo group (−0.8 ± 1.6%, P < 0.0001 compared to either idursulfase group). About eighty percent of the patients with baseline hepatomegaly who were treated with either dosing regimen of idursulfase had normal liver volume after 18 weeks and 53 weeks. In contrast only 1 of the 23 placebo-treated patients with baseline hepatomegaly had normal liver volume at Week 53.
The majority of patients had spleen volumes within normal limits at baseline, and baseline spleen volumes were similar in the three groups (Table 1). After 18 weeks of treatment, spleen volume had decreased by 21.5 ± 3.0% in the idursulfase weekly group and by 25.0 ± 3.5% in the idursulfase EOW group. The placebo group exhibited a 3.6 ± 3.9% increase in spleen volume. After 53 weeks in the ITT population, spleen volume remained significantly reduced in the idursulfase groups compared to placebo (−25.1 ± 2.4% in the idursulfase weekly group, −19.8 ± 3.2% in the idursulfase EOW group, and +7.2 ± 4.2% in the placebo group, P < 0.0001 for placebo compared to either idursulfase group) (Table 2).
Urine GAG Levels
As shown in Figure 3 and Table 2, urine GAG level decreased in patients treated with either dosing regimen of idursulfase and did not change significantly in patients treated with placebo. At Week 53, the GAG levels in the idursulfase groups were significantly different than that of the placebo group (P < 0.0001 for either group compared to placebo). The response in the idursulfase weekly group was significantly greater than that seen in the idursulfase EOW group (P = 0.0394). After 53 weeks of treatment with either regimen of idursulfase, 26 of 64 (40.6%) had normalized urine GAG levels, and the majority of the remainder of idursulfase-treated patients were approaching the upper end of the normal range (≤127 μg GAG/mg creatinine). No patients in the placebo group experienced normalization of urine GAG by 53 weeks.
The effect of treatment with idursulfase or placebo on urine GAG levels in MPS II. All values are the observed means ± SEM. aP < 0.0001 for both weekly and EOW idursulfase compared with placebo at Week 53 (ANCOVA). bP = 0.039 compared to EOW dosing (ANCOVA). EOW, every-other-week; GAG, glycosaminoglycans.
Joint Mobility
An improvement in elbow mobility between the weekly idursulfase group compared to placebo was observed (P = 0.0476). No other significant differences between treatment groups for any joint range of motion were found.
Safety
One year of treatment with idursulfase was well tolerated with the majority of adverse events (AEs) being consistent with those expected to be seen in an untreated MPS II population. The most frequently reported AEs included fever, headache, cough, pharyngitis, upper respiratory tract infection, nasal congestion, nausea, vomiting, abdominal pain, and diarrhea. The majority of AEs were mild or moderate in severity in all groups. Table 3 lists those treatment-emergent AEs that were reported during the study with an excess incidence of at least a 9% compared with placebo in either idursulfase-treated groups or in the weekly idursulfase-treated group.
Of the AEs considered possibly related to idursulfase treatment, the most common were infusion-related. An infusion-related adverse event was defined to have occurred if the event occurred within the day after the infusion, began during or after the infusion, and was judged by the investigator to be possibly or probably related to study treatment. A similar number of patients in each treatment group experienced one or more infusion-related adverse events during the study (placebo, 21; EOW, 22; weekly, 22). The total number of AEs was similar in each group (placebo, 992; Weekly, 1,063; EOW, 1,163) with the largest number being reported for the EOW group. The incidence of infusion-related adverse events was maximal between Weeks 4 and 12 and decreased in all three groups thereafter. Infusion-related adverse events reported in the placebo group were similar in nature and severity to those in the idursulfase-treated groups. No patient withdrew from the study because of infusion-related adverse events.
A total of 49 serious adverse events (SAEs) occurred in 26 patients during the study: Nine patients in the placebo group experienced a total of 18 SAEs, 8 patients in the idursulfase EOW group experienced a total of 18 SAEs, and 9 patients in the idursulfase weekly group experienced a total of 13 SAEs. The majority of these SAEs were considered unrelated to the blinded study medication, although three patients experienced SAEs that were considered by the investigators to be probably or possibly related to the study drug.
Two deaths occurred during the study. A 24-year-old male in the idursulfase weekly group, developed a pulmonary infection, respiratory insufficiency and had a cardiac arrest 5 days after his first infusion. Following resuscitation he remained in an intensive care unit, where he experienced a fatal cardiac arrest seven days later. A second patient (a 6-year-old male), who was randomized to placebo, developed streptococcus pneumonia following his 34th dose of blinded-study medication. He was admitted to an intensive care unit, where he was diagnosed with sepsis and disseminated intravascular coagulation. Eight days later the patient's pulmonary function worsened. He suffered a lung hemorrhage followed by fatal cardiac arrest. Neither death was considered related to blinded study medication by the investigator.
Antibodies
IgG anti-idursulfase antibodies were detected in 15 patients (46.9%) in the idursulfase weekly group and in 15 patients (46.9%) in the idursulfase EOW group. IgM antibodies occurred in 2 patients, one in each active treatment group. The highest prevalence of IgG antibodies was seen at Week 27 of the study, when 44.4% of the patients treated with idursulfase were antibody-positive. After 53 weeks, only 31.7% of patients in the idursulfase groups remained antibody-positive. The reduction in urine GAG levels in antibody-positive patients was about two-thirds of that seen in antibody-negative patients. In contrast, there was no association with the presence of antibodies and adverse events or with clinical assessments (such as 6MWT or FVC measurements). No anti-idursulfase IgE antibodies were detected in any patient during the study.
DISCUSSION
This study is the largest and longest, placebo-controlled trial of a therapy for a lysosomal storage disease, and its size allowed for the treatment groups to be well balanced with regard to patient age and baseline disease characteristics. The results demonstrate that weekly infusions of idursulfase (0.5 mg/kg) produced a clinical benefit based on significant improvements in the two-component composite endpoint, 6MWT distance, and %FVC compared to placebo. Although EOW idursulfase also improved the composite endpoint, the magnitude of the difference compared with placebo was about half of that seen with weekly dosing. These differences in responses between the weekly and EOW dosing regimens of idursulfase demonstrate that at the conclusion of the one year trial, weekly dosing was superior to EOW dosing in the treatment of MPS II.
The efficacy of idursulfase in the analysis of the composite outcome variable was primarily due to an improvement in the 6MWT distance rather than an improvement in %FVC (Fig. 1). The 6MWT measures the integrated function of at least 3 separate organ systems that are affected by MPS II: the respiratory, cardiovascular, and musculo-skeletal systems. The increase in 6MWT distance experienced by patients in the idursulfase weekly group (35.1 ± 13.7 m greater than in the placebo group) is similar to that observed in the phase I/II clinical study of idursulfase in MPS II (unpublished data, 2006) and to that reported after 6 months of enzyme replacement therapy in MPS I.22
The smaller effect on pulmonary function may reflect difficulties in accurately determining %FVC in patients with MPS II, because the formulae for predicted FVC16,17 assume both normal growth and the ability to accurately measure height. Neither of these assumptions applies to patients with MPS II. Compared to a normal male population,23 the height of the MPS II patients >9 years of age in this study was less than the 5th percentile for age, but patients ≤9 years of age were typically of normal stature. Whereas some of this difference appears to reflect a true reduction in linear growth, the inability of MPS II patients to stand erect because of contractures and joint disease also contributes. Thus if a patient who was randomized to idursulfase treatment experienced an improvement in joint flexibility, it is possible that such a patient would be able to stand straighter, leading to an increase in measured height and a subsequent increase in predicted FVC despite the fact that no actual linear growth had occurred. Thus any improvement in %FVC would be spuriously underestimated, potentially underestimating any measured treatment effect. When changes in absolute FVC were analyzed (Fig. 2), the group treated with weekly infusions of idursulfase showed a significant increase in FVC compared with either the placebo group or the EOW idursulfase group. This observation supports a benefit for idursulfase in improving pulmonary function in MPS II.
Enzyme replacement therapy has been previously developed for MPS I20,22 and MPS VI,24,25 as well as for other lysosomal storage diseases.26–28 Both MPS I and MPS VI are caused by deficiencies in single enzymes involved in the catabolism of GAG,1 and like MPS II, their phenotypic expression varies considerably.1 The spectrum of clinical disease in MPS I is similar to MPS II with somatic and neurological involvement. In contrast, MPS VI patients do not have primary neurological disease, but can develop severe somatic manifestations.
This study demonstrates the clinical benefit of idursulfase replacement therapy for MPS II is similar to ERT results for MPS I20,22 and MPS VI.24,25 In the MPS I double-blind, placebo-controlled phase III ERT study reported by Wraith and coworkers, 6 months of treatment with laronidase (recombinant α-L-iduronidase) significantly decreased urinary GAG, decreased liver and spleen volumes, improved %FVC (based on each patient's current height) by 4.3% (P = 0.022) and increase the 6MWT distance by 38 m (P = 0.066) compared to placebo.22 In the MPS VI double-blind phase, placebo-controlled phase III ERT study, 6 months of treatment with galsulfase (recombinant human N-acetylgalactosamine 4-sulfatase) decreased urinary GAG and the distance walked in 12 minutes showed a longitudinal model-derived mean difference of 92 ± 40 m (P = 0.025) in favor of galsulfase.25,29
The safety profile of idursulfase was similar to that reported for other enzyme replacement therapies.20,22,24–28 Overall, the number and severity of adverse events was similar in the three treatment arms. A similar number of patients in each treatment group experienced infusion-related adverse events, and most of these adverse events occurred during the first six months of the study, suggesting that patients experiencing infusion reactions developed tolerance to the infusions.
IgG antibodies were detected in 30 of the 64 patients (46.9%) who were treated with idursulfase, with no difference in the incidence rate between the weekly and EOW dosing groups. This rate of seroconversion is lower than has been reported for other forms of enzyme replacement therapy.20,22,24,25,27,30 Interestingly, in the present study about one-third of the patients who developed antibodies were antibody-negative after 1 year of treatment, suggesting the development of immunological tolerance similar to what has been reported for enzyme replacement therapy in Gaucher disease31 and Fabry disease.32
The current treatment of MPS II has focused on managing symptoms, since no therapy is available. Therapies targeted to provide sufficient enzyme activity to slow or stop the progression of the disease,33–35 such as hematopoietic cell transplantation, have been proposed,33–35 but no systematic studies have been performed and the limited reports have been disappointing.36
The results of the present study suggest that idursulfase may be the first treatment that can benefit patients with MPS II by addressing the underlying enzymatic defect. Intravenous administration of idursulfase has improved the somatic disease in MPS II, but is not expected to impact the CNS. Patients with the severe form of MPS II treated with idursulfase would be expected to have somatic stabilization, but the overall benefit will have to be evaluated depending of the somatic disease burden and rate of progression of the CNS disease.
Idursulfase was well-tolerated, and those patients treated with idursulfase 0.5 mg/kg administered weekly or EOW experienced a clinical benefit based on the significant improvement in the composite endpoint compared with placebo. In addition, treatment with idursulfase resulted in a substantial reduction in organomegaly and in urinary GAG excretion. Weekly dosing appeared to offer greater benefit compared to EOW dosing based on the larger improvement in the 6MWT, the improvement in absolute FVC, and the larger reduction in urine GAG levels. The benefits of increased endurance and the reversal of end-organ disease are clinically meaningful and may benefit patients with MPS II. The open-label extension of this study will determine if long-term use of weekly idursulfase will result in further clinical improvement in patients with MPS II.
References
Neufeld EF, Muenzer J . The mucopolysaccharidoses. In: Scriver CR, (Ed.). The metabolic and molecular bases of inherited disease. New York: McGraw-Hill, 2001; 3421–3452.
Meikle PJ, Hopwood JJ, Clague AE, Carey WF . Prevalence of lysosomal storage disorders. JAMA 1999; 281: 249–254.
Poorthuis BJHM, Wevers RA, Kleijer WJ, Groener JEM, et al. The frequency of lysosomal storage diseases in The Netherlands. Hum Genet 1999; 105: 151–156.
Baehner F, Schmiedeskamp C, Krummenauer F, Miebach E, et al. Cumulative incidence rates of the mucopolysaccharidoses in Germany. J Inherit Metab Dis 2005; 28: 1011–1017.
Young ID, Harper PS . Incidence of Hunter's syndrome. Hum Genet 1982; 60: 391–392.
Lissens W, Seneca S, Liebaers I . Molecular analysis in 23 Hunter disease families. J Inherit Metab Dis 1997; 20: 453–456.
Kim CH, Hwang HZ, Song SM, Paik KH, et al. Mutational spectrum of the iduronate 2 sulfatase gene in 25 unrelated Korean Hunter syndrome patients: identification of 13 novel mutations. Hum Mutat 2003; 21: 449–450.
Timms KM, Bondeson ML, Ansari-Lari MA, Lagerstedt K, et al. Molecular and phenotypic variation in patients with severe Hunter syndrome. Hum Mol Genet 1997; 6: 479–486.
Vafiadaki E, Cooper A, Heptinstall LE, Hatton CE, et al. Mutation analysis in 57 unrelated patients with MPS II (Hunter's disease). Arch Dis Child 1998; 79: 237–241.
Li P, Bellows AB, Thompson JN . Molecular basis of iduronate-2-sulphatase gene mutations in patients with mucopolysaccharidosis type II (Hunter syndrome). J Med Genet 1999; 36: 21–27.
Wilson PJ, Suthers GK, Callen DF, Baker E, et al. Frequent deletions at Xq28 indicate genetic heterogeneity in Hunter syndrome. Hum Genet 1991; 86: 505–508.
Muenzer J, Lamsa JC, Garcia A, Dacosta J, et al. Enzyme replacement therapy in mucopolysaccharidosis type II (Hunter syndrome): a preliminary report. Acta Paediatr Suppl 2002; 91: 98–99.
O'Brien PC . Procedures for comparing samples with multiple endpoints. Biometrics 1984; 40: 1079–1087.
American Thoracic Society. Standardization of Spirometry, 1994 Update. Am J Respir Crit Care Med 1995; 152: 1107–1136.
Quanjer PH, Tammeling GJ, Cotes JE, Pedersen OF, et al. Lung volumes and forced ventilatory flows. Report Working Party Standardization of Lung Function Tests, European Community for Steel and Coal. Official Statement of the European Respiratory Society. Eur Respir J Suppl 1993; 16: 5–40.
Hankinson JL, Odencrantz JR, Fedan KB . Spirometric reference values from a sample of the general U.S. population. Am J Respir Crit Care Med 1999; 159: 179–187.
Polgar G, Promadhat V . Pulmonary function testing in children: techniques and standards. W.B. Saunders and Company, 1971;
American Thoracic Society. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 2002; 166: 111–117.
de Jong JGN, Wevers RA, Laarakkers C, Poorthuis BJ . Dimethylmethylene blue-based spectrophotometry of glycosaminoglycans in untreated urine: a rapid screening procedure for mucopolysaccharidoses. Clin Chem 1989; 35: 1472–1477.
Kakkis ED, Muenzer J, Tiller GE, Waber L, et al. Enzyme-replacement therapy in mucopolysaccharidosis I. N Engl J Med 2001; 344: 182–188.
Schlesinger AE, Edgar KA, Boxer LA . Volume of the spleen in children as measured on CT scans: normal standards as a function of body weight. AJR American Journal of Roentgenology 1993; 160: 1107–1109.
Wraith JE, Clarke LA, Beck M, Kolodny EH, et al. Enzyme replacement therapy for mucopolysaccharidosis I: a randomized, double-blinded, placebo-controlled, multinational study of recombinant human alpha-L-iduronidase (laronidase). J Pediatr 2004; 144: 581–588.
McDowell MA, Fryar CD, Hirsch R, Ogden CL . Anthropometric reference data for children and adults: U.S. population, 1999-2002. Adv Data 2005; 1–5.
Harmatz P, Ketteridge D, Giugliani R, Guffon N, et al. Direct comparison of measures of endurance, mobility, and joint function during enzyme-replacement therapy of mucopolysaccharidosis VI (Maroteaux-Lamy syndrome): results after 48 weeks in a phase 2 open-label clinical study of recombinant human N-acetylgalactosamine 4-sulfatase. Pediatrics 2005; 115: e681–e689.
Harmatz P, Giugliani R, Schwartz I, Guffon N, et al. Enzyme replacement therapy for mucopolysaccharidosis VI: A phase 3, randomized, double-blind, placebo-controlled, multinational study of recombinant human N-acetylgalactosamine 4-sulfatase (recombinant human arylsulfatase B or RHASB) and follow-on, open-label extension study. J Pediatr 2006; 148: 533–539.
Barton NW, Brady RO, Dambrosia JM, Di Bisceglie AM, et al. Replacement therapy for inherited enzyme deficiency–macrophage-targeted glucocerebrosidase for Gaucher's disease. N Engl J Med 1991; 324: 1464–1470.
Eng CM, Guffon N, Wilcox WR, Germain DP, et al. Safety and efficacy of recombinant human α-galactosidase A replacement therapy in Fabry's disease. N Engl J Med 2001; 345: 9–16.
Schiffmann R, Kopp JB, Austin HAI, Sabnis S, et al. Enzyme replacement therapy in Fabry disease: a randomized controlled trial. JAMA 2001; 285: 2743–2749.
BioMarin Pharmaceutical I. Naglazyme (galsulfase) prescribing information. 2005. Novato, CA.
Wilcox WR, Banikazemi M, Guffon N, Waldek S, et al. Long-term safety and efficacy of enzyme replacement therapy for Fabry disease. Am J Hum Genet 2004; 75: 65–74.
Rosenberg M, Kingma W, Fitzpatrick MA, Richards SM . Immunosurveillance of–alglucerase enzyme therapy for Gaucher patients: induction of humoral tolerance in seroconverted patients after repeat administration. Blood 1999; 93: 2081–2088.
Schiffmann R, Ries M, Timmons M, Flaherty JT, et al. Long-term therapy with agalsidase alfa for Fabry disease: safety and effects on renal function in a home infusion setting. Nephrol Dial Transplant 2006; 21: 345–354.
Vellodi A, Young E, Cooper A, Lidchi V, et al. Long-term follow-up following bone marrow transplantation for Hunter disease. J Inherit Metab Dis 1999; 22: 638–648.
Coppa GV, Gabrielli O, Zampini L, Jetzequel AM, et al. Bone marrow transplantation in Hunter syndrome. J Inherit Metab Dis 1995; 18: 91–92.
Mullen CA, Thompson JN, Richard LA, Chan KW . Unrelated umbilical cord blood transplantation in infancy for mucopolysaccharidosis type IIB (Hunter syndrome) complicated by autoimmune hemolytic anemia. Bone Marrow Transplant 2000; 25: 1093–1097.
Peters C, Krivit W . Hematopoietic cell transplantation for mucopolysaccharidosis IIB (Hunter syndrome). Bone Marrow Transplant 2000; 25: 1097–1099.
Acknowledgements
This study was supported in part by a grant from the DHHS/FDA/ORD (Grant FD-R-002565-0, “Assessment of idursulfase in MPS II (AIM) pivotal trial”). This study was supported in part by a grant to the University of North Carolina at Chapel Hill (RR00046) from the General Clinical Research Centers program of the Division of Research Resources, National Institutes of Health. Shire Human Genetic Therapies, Inc. participated in the planning of this study and provided financial support for its conduct. We thank the MPS II patients and their families who participated in this study and the physicians who referred the subjects. We acknowledge the extraordinary efforts of the nurses, study coordinators and site staffs, who made this clinical trial possible.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Muenzer, J., Wraith, J., Beck, M. et al. A phase II/III clinical study of enzyme replacement therapy with idursulfase in mucopolysaccharidosis II (Hunter syndrome). Genet Med 8, 465–473 (2006). https://doi.org/10.1097/01.gim.0000232477.37660.fb
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1097/01.gim.0000232477.37660.fb
Keywords
This article is cited by
-
Analysis of caregiver perspectives on patients with mucopolysaccharidosis II treated with pabinafusp alfa: results of qualitative interviews in Japan
Orphanet Journal of Rare Diseases (2024)
-
Caregiver experiences and observations of intrathecal idursulfase-IT treatment in a phase 2/3 trial in pediatric patients with neuronopathic mucopolysaccharidosis II
Orphanet Journal of Rare Diseases (2024)
-
Natural progression of cardiac features and long-term effects of enzyme replacement therapy in Taiwanese patients with mucopolysaccharidosis II
Orphanet Journal of Rare Diseases (2021)
-
The multi-domain responder index: a novel analysis tool to capture a broader assessment of clinical benefit in heterogeneous complex rare diseases
Orphanet Journal of Rare Diseases (2021)
-
Biodegradable polyethylene glycol hydrogels for sustained release and enhanced stability of rhGALNS enzyme
Drug Delivery and Translational Research (2020)