Abstract
Purpose
To design and produce a clamp that enables good handling of donor sclera-corneal disks, allows air to be injected in the corneal stroma and consistently provides pre-Descemets endothelial keratoplasty (PDEK) tissue by creation of a type-1 big bubble (BB) avoiding a type-2BB by shutting the fenestrations in the periphery of the pre-Descemets layer and preventing escape of air.
Patients and methods
A clamp with spring loaded handles attached to two rings of 9 mm diameter and 1 mm width with a side port for insertion of a needle for air injection was designed and produced. The clamp was tested in 20 human donor sclera-corneal disks and refined over three prototypes. The final design was used for PDEK in 8 patients.
Results
The clamp was able to prevent any escape of air or the formation of a type-2BB. By preventing air leak, it provided better control over the volume of air injected allowing for consistent formation of a type-1BB, which could be expanded to its full diameter by advancing the tip of the needle into the bubble cavity. Centration of tissue in the clamp was important. The clamp was used successfully to obtain PDEK tissue from 8 donor sclara-corneal disks for transplant in three eyes with pseudophakic bullous keratopathy and five eyes with pseudophakia and Fuchs’ endothelial dystrophy.
Conclusion
The PDEK clamp is a simple and useful instrument that will give surgeons the confidence of consistently obtaining PDEK tissue with ease and without the risk of separating the Descemets membrane in a type-2BB.
Similar content being viewed by others
Introduction
Lamellar corneal grafts have not only revolutionized corneal transplantation surgery but have also provided insights into posterior corneal anatomy.1, 2, 3, 4, 5 In most specialist centers, deep anterior lamellar keratoplasty (DALK) has replaced penetrating keratoplasty (PK) for indications related to corneal stromal pathology; and endothelial keratoplasty (EK) has become the procedure of choice for all indications related to corneal endothelial dysfunction. For EK, Descemets membrane EK (DMEK) is considered to be a major improvement over Descemets stripping EK but has certain limitations.1, 2, 3, 4 It is technically challenging both surgically and in donor tissue preparation. Younger corneas with associated high endothelial cell counts cannot usually be used due to the increased risk of tissue loss related to the firm adhesion of DM.6, 7, 8 Tight DM scrolls are difficult to unroll resulting to excessive endothelial cell loss during intraoperative handling.9
Pre-Descemets EK (PDEK) is the latest innovation in EK. The concept was introduced by Dua et al5 and the first case series was reported in 2014.10 It involves the intrastromal injection of air in a donor sclera-corneal disk to create a type-1 big bubble (BB).5 The wall of the BB, comprised of the pre-Descemets layer (Dua’s layer (PDL)),5 DM and endothelium is trephined or excised with scissors and used as the donor material for EK. Prior to this report,5 others had used pneumodissection to produce DMEK tissue.11 Inadvertently some had produced PDEK tissue but were unaware of this fact and had performed and reported the procedure as DMEK,11 as the knowledge of the difference between PDEK and DMEK tissue did not exist. A reference to the prevailing misunderstanding at the time has been made in the original publication on PDEK.10 PDEK tissue scrolls less than DMEK tissue,12 is easier to handle and unroll in the anterior chamber10 and can be harvested from very young donors.8 However, there are two limitations, the maximum diameter possible is between 7.5 and 8.5 mm and at times intrastromal injection or air can result in a type-2BB5 (separation of DM without PDL), enforcing conversion to DMEK for which the surgeon may not have the desirable experience.
We have demonstrated that during pneumodissection a type-2BB results from the escape of air through clusters of holes in the periphery of the PDL, along the circumference of the corneal periphery.13, 14 These holes allow air to pass through the PDL which is otherwise impermeable to air. Air injected in the corneal stroma, anterior to the PDL accesses the plane between PDL and DM, lifting the DM off to produce a type-2BB.13, 14 Based on this knowledge we designed a clamp to ensure that the chances of getting a type-2BB are markedly reduced if not entirely eliminated.
Materials and methods
Based on the observation that a type-2BB almost always starts at the periphery of the sclera-corneal disk and commencement of the BB correlates with the location of tiny perforations in PDL at the periphery, we hypothesized that by occluding the holes during air injection the probability of a type-2BB forming could be markedly reduced or eliminated. The aim was to design a clamp that shuts out the peripheral holes and prevents formation of a type-2BB; provides a firm grip on the donor sclera-corneal disk and easy access for insertion of the needle to inject air. We designed a PDEK clamp and partnered with e. Janach (Via Borgo Vico 35 22100 Como—Italy) to manufacture and develop a prototype.
PDEK clamp design
The PDEK clamp (Figure 1a) is made of steel and has a spring handle with two complementary rings (internal diameter of 9 mm) and a central locking screw for maintaining the clamp in a closed position. The rings are 1-mm wide with the opposing surfaces sand-blasted for a better grip (Figure 1b). At 45° from the attachment of the handle to the lower ring, which is thicker than the upper ring, is a side port of 0.7 mm × 1.7 mm (Figure 1c) with a corresponding small notch in the upper ring to give the port a dimension of about 0.9 mm in the closed position. The site of the port is marked by an etching on the upper ring (Figure 1c). In the fully open position the rings are 10 mm apart.
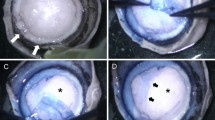
(a) The PDEK clamp with two rings of an internal diameter of 9 mm, in the closed position. When a sclera-corneal disk is placed between the rings and the clamp closed, the rings compress the peripheral holes and prevent escape of injected air in to the plane anterior to the DM. (b) The opposing surfaces of the ring are sand blasted to make the surface rough for a better grip. This is clearly seen on the under surface of the upper ring. (c) Illustrates the side port in the lower ring next to the handle. Its position is marked by an etching on the upper ring as the port cannot be directly visualized when the tissue is clamped between the rings. (d) A sclera-corneal disk that was clamped in the PDEK clamp to obtain a type-1BB. The central white area with a type-1BB represents the aerated corneal stroma. The surrounding clear circumferential zone is the part that was compressed in the PDEK clamp. No air entered this zone. The arrow marks the point of entry of the needle used for injecting air through the side port of the PDEK clamp. (e) Slit lamp diffuse image with cobalt blue filter of a cornea stained with fluorescein dye to illustrate the post-operative day-1 image of an eye treated with PDEK for bullous keratopathy. The bullae are visible in the central cornea and a partially absorbed air bubble injected during the procedure to tamponade the PDEK tissue is seen in the upper part of the anterior chamber. (f) The same cornea as in E, one month post-PDEK. The cornea is very clear and the edge of the PDEK graft is clearly visible in the superior temporal quadrant. The interface of the PDEK graft and host corneal stroma cannot be seen on a slit beam image (inset). (g) Optical coherence tomography image of the same eye at 1 month post-PDEK. A double contour line is seen at the posterior surface of the cornea (arrows) representing the PDEK tissue.
PDEK clamp use and validation
With the clamp fully open, the sclera-corneal disk, endothelial side up, is placed on the lower ring and centered. The transparency of the cornea allows visualization of the ring underneath and helps with centering. The clamp is then closed and the screw tightened. Under an operating microscope, the disk is held on a black plate (provided with the clamp) for better contrast and a 30-gauge needle, bent at 135°, attached to a 5 ml syringe filled with air, is inserted through the side port, starting in the scleral rim and advanced to the center of the cornea in mid-stroma. The clamped disk obscures visualization of the port but the etching on the upper ring indicates the point for insertion of the needle. Air is firmly but slowly injected into the stroma. When the stroma is fully aerated it becomes white and tiny bubbles form in the center under the PDL. These coalesce to form a type-1BB (Figure 1d). Once the BB has formed, the needle can be tilted and directed into the cavity of the bubble to expand it further by injection of more air (Supplementary video clip 1). The air is then aspirated to collapse the bubble and the clamp opened and the disk removed. Alternatively, with the bubble inflated, the clamp can be opened and the tissue withdrawn (Figure 1d).
The PDEK clamp was tested in 20 human eye bank donor eyes provided by the National Health Service Blood and Transplant Eye Banks and duly consented for research and development. Details of the donor eyes are given in Table 1. The use of air injection for lamellar corneal separation was approved by Nottingham research ethics committee-1 (06-Q2403-46).
Retrieval of PDEK tissue
PDEK tissue was retrieved in two ways as previously described.10 When air is aspirated to collapse the type-1BB, a circular disk of PDEK tissue can be punched out using a trephine of appropriate diameter. Alternatively, when the sclera-corneal disk is removed from the clamp with an inflated type-1BB, the wall of the bubble is incised with a sharp knife at the attachment to the stroma, the tissue is stained by injecting VisionBlue (Dutch ophthalmic, USA) in to the bubble, and the PDEK tissue is separated by cutting along the circumference of the BB (Supplementary video clip 2).
Results
The dimensions of the clamp were optimized over three versions. In the first version the diameter of the rings was set at 10 mm, and the width of the rings was 0.5 mm. This did not completely occlude all the peripheral holes and a type-2BB was formed in 2 of the 5 disks tested with this version. This version was not used to harvest PDEK tissue for human transplantation. In the second version, the inner diameter was reduced to 9 mm and the width of the rings increased to 1 mm. With this, no leakage of air was seen and the desired type-1BB formed in 13 of 13 sclera-corneal disks where the rings were accurately centered. However, in 2 samples a type-2BB formed. In both these instances the tissue was decentered in the clamp. This version confirmed that the desired objective of occluding the peripheral fenestrations was achieved and no escape of air occurred. However the side port was considered to be narrow as it restricted manipulation of the needle in the corneal stroma. This version too was not used to harvest PDEK tissue for human transplantation. In the third and final version, the dimension and trajectory of the side port were revised to allow insertion of the needle in the horizontal plane even though the slope of the rings is directed downwards (Figure 1c) and the size enlarged to 0.7 × 1.7 mm to allow easy manipulation of the needle compared to the previous version where it was smaller and the trajectory was directed slightly downwards. The width of the fully open clamp allowed removal of the sclera-corneal disk with an inflated type-1BB without any contact of the endothelial surface with the upper ring.
Only the final version presented here (Figure 1) was used to perform PDEK in 3 eyes with pseudophakic bullous keratopathy and 5 eyes with pseudophakia and Fuchs’ endothelial dystrophy. PDEK tissue was successfully obtained in all cases using the PDEK clamp and PDEK completed (Figure 1e–g).
Discussion
Air injection in the corneal stroma of patients was described initially by Anwar and Teichmann15 in the DALK procedure. However, the procedure was described as a ‘Descemets baring technique’,15, 16 which was later proved not to be the case and a distinct pre-Descemets layer, offering a cleavage plane during pneumodissection, was reported in a couple of international meetings.5, 14 Others reported ‘residual stroma’ on the anterior surface of the DM in both in vivo and ex vivo procedures.17, 18 A detailed description and characterization of the PDL and types of BB was published in 2013.5 Although the concept was initially challenged19 a number of publications have contributed to the further characterization of the PDL and its attributes. It is a very tough layer with a high bursting pressure such that phacoemulsification can be performed under this layer in the DALK-triple procedure.20 It is unique such that if ablated by excimer laser phototherapeuctic keratectomy air injection in the stroma does not result in the formation of a type-1BB,21 it is continuous at the periphery with the collagen core of the trabecular meshwork,22 has a higher concentration of elastin than the rest of the corneal stroma,23 and has a paucity or an absence of keratocytes.5, 24 A recent high-resolution optical coherence tomography study has demonstrated the layer in vivo in humans.24
Clinically there is no doubt that it forms an important part of the surgical anatomy of the cornea. Its ‘rough’ looking anterior surface enables intraoperative differentiation of a type-1 from a type-2BB.25 It offers a distinct surgical plane that can be exploited to complete successful DALK when a BB does not form14, 26 and also determines spread of infections.27 Spontaneous separation of the PDL from the deep stroma is seen in acute hydrops and following cataract surgery.28, 29 Besides the DALK-triple procedure,20 knowledge of PDL has been exploited in the management of acute hydrops in keratoconus29 and in the PDEK operation.10
In PDEK tissue, PDL splints the DM and limits the scrolling of the tissue and also facilitates handling and centration of the tissue both inside and outside the eye. Endothelial cell counts in PDEK tissue have been shown to be similar to that in DMEK tissue obtained by pneumodisscetion30 and one study has shown that both PDEK and DEMK tissue can be stored in organ culture for a week without affecting endothelial cell counts.31 Thus far in PDEK the predictability of consistently obtaining a type-1BB is limited because injected air escapes from natural fenestrations located on either side of the trabecular meshwork beyond the termination of the DM. Therefore, in order to obtain a critical intra-tissue pressure to produce a type-1BB the surgeon has to adjust the pressure on the plunger of the air filled syringe to compensate for the loss of air. If too much force is applied the bubble can form rapidly and burst. If too little force is applied a small type-1BB can form giving a PDEK tissue of variable diameter. Further, as hypothesized, when the fenestrations are central to the termination of the DM, a type-2BB can form. The PDEK clamp overcomes all the above limitations. The clamp completely shuts off the peripheral holes and all the air injected is retained in the corneal stroma and with no loss due to leakage. The intrastromal pressure can therefore be increased in a controlled manner until a BB has formed. The fenestrations in PDL anterior to the DM are also closed by the clamp and thus a type-2BB does not form. To ensure that the above advantages of the clamp are achieved proper centration of the tissue is important. The clamp also permits robust handling of the tissue without an assistant. Once a type-1BB has formed the needle can be maneuvered to advance the tip in the cavity of the bubble and more air can be injected to expand the diameter of the bubble by 0.5–1 mm thus enabling a larger diameter of PDEK tissue.
Sclera-corneal disks used for testing and developing the clamp were stored and supplied by NHSBT in tissue culture medium without dextran. These were comparatively thicker than the disks used for human transplantation, which were in medium containing dextran to deturgesce them. Apart from the extra care required during insertion of the needle to avoid perforation, there was no difference in the ability to obtain the desired type-1BB with the clamp, in the sclera-corneal disks stored with and without dextran. The PDEK clamp should prove to be a simple useful instrument that will give surgeons the confidence of consistently obtaining PDEK tissue without risk of creating a type-2BB.

References
Reinhart WJ, Musch DC, Jacobs DS, Lee WB, Kaufman SC, Shtein RM . Deep anterior lamellar keratoplasty as an alternative to penetrating keratoplasty: a report by the American Academy of Ophthalmology. Ophthalmology 2011; 118: 209–218.
Lee WB, Jacobs DS, Musch DC, Kaufman SC, Reinhart WJ, Shtein RM . Descemet’s stripping endothelial keratoplasty: safety and outcomes: a report by the American Academy of Ophthalmology. Ophthalmology 2009; 116: 1818–1830.
Coster DJ, Lowe MT, Keane MC, Williams KA . Australian Corneal Graft Registry Contributors. A comparison of lamellar and penetrating keratoplasty outcomes: a registry study. Ophthalmology 2014; 121: 979–987.
Park CY, Lee JK, Gore PK, Lim CY, Chuck RS . Keratoplasty in the United States: a 10-year review from 2005 through 2014. Ophthalmology 2015; 122: 2432–2442.
Dua HS, Faraj LA, Said DG, Gray T, Lowe J . Human corneal anatomy redefined: a novel pre Descemet’s layer (Dua’s layer). Ophthalmology 2013; 120: 1778–1785.
Heinzelmann S, Hüther S, Böhringer D, Eberwein P, Reinhard T, Maier P . Influence of donor characteristics on Descemet membrane endothelial keratoplasty. Cornea 2014; 33: 644–648.
Monnereau C, Quilendrino R, Dapena I, Liarakos VS, Alfonso JF, Arnalich-Montiel F et al. Multicenter study of Descemet membrane endothelial keratoplasty: first case series of 18 surgeons. JAMA Ophthalmol 2014; 132: 1192–1198.
Agarwal A, Agarwal A, Narang P, Kumar DA, Jacob S . Pre-Descemets endothelial keratoplasty with infant donor corneas: a prospective analysis. Cornea 2015; 34: 859–865.
Maier AK, Gundlach E, Schroeter J, Klamann MK, Gonnermann J, Riechardt AI et al. Influence of the difficulty of graft unfolding and attachment on the outcome in Descemet membrane endothelial keratoplasty. Graefes Arch Clin Exp Ophthalmol 2015; 253: 895–900.
Agarwal A, Dua HS, Narang P, Kumar DA, Agarwal A, Jacob S et al. Pre-Descemet's endothelial keratoplasty (PDEK). Br J Ophthalmol 2014; 98: 1181–1185.
Busin M, Scorcia V, Patel AK, Salvalaio G, Ponzin D . Pneumatic dissection and storage of donor endothelial tissue for Descemet’s membrane endothelial keratoplasty: a novel technique. Ophthalmology 2010; 117: 1517–1520.
Dua HS, Termote K, Kenawy MB, Said DG, Jayaswal R, Nubile M et al. Scrolling characteristics of pre-Descemets endothelial keratoplasty tissue: An ex vivo study. Am J Ophthalmol 2016; 166: 84–90.
Elalfy M, Faraj L, Said DG, Katamish T, Dua H . Dynamics of Big Bubble (BB) formation in DALK: in vitro studies. Acta Ophthalmol 2014; 92: s253.
Dua HS, Faraj LA, Said DG . Dua’s layer: discovery, characteristics, clinical applications, controversy and potential relevance to glaucoma. Expert Rev Ophthalmol 2015; 10: 531–547.
Anwar M, Teichmann KD . Big-bubble technique to bare Descemet’s membrane in anterior lamellar keratoplasty. J Cataract Refract Surg 2002; 28: 398–403.
Anwar M Descemets Membrane Baring Techniques, Big Bubble Techniquein Atlas Of Lamellar Surgery. In: Fontana L, Tassinari G (eds). Fabiano Editore: Canelli (AT), Italy, 2007, pp 125–136..
Jafarinasab MR, Rahmati-Kamel M, Kanavi MR, Feizi S . Dissection plane in deep anterior lamellar keratoplasty using the big-bubble technique. Cornea 2010; 29: 388–391.
McKee HD, Irion LC, Carley FM, Jhanji V, Brahma AK . Residual corneal stroma in big-bubble deep anterior lamellar keratoplasty: a histological study in eye-bank corneas. Br J Ophthalmol 2011; 95: 1463–1465.
Schlötzer-Schrehardt U, Bachmann BO, Tourtas T, Torricelli AA, Singh A, González S et al. Ultrastructure of the posterior corneal stroma. Ophthalmology 2015; 122: 693–699.
Zaki AA, Elalfy MS, Said DG, Dua HS . Deep anterior lamellar keratoplasty–triple procedure: a useful clinical application of the pre-Descemet’s layer (Dua’s layer). Eye 2015; 29: 323–326.
Dua HS, Mastropasqua L, Faraj L, Nubile M, Elalfy MS, Lanzini M et al. Big bubble deep anterior lamellar keratoplasty: the collagen layer in the wall of the big bubble is unique. Acta Ophthalmol 2015; 93: 427–430.
Dua HS, Faraj LA, Branch MJ, Yeung AM, Elalfy MS, Said DG et al. The collagen matrix of the human trabecular meshwork is an extension of the novel pre-Descemet's layer (Dua's layer). Br J Ophthalmol 2014; 98: 691–697.
Lewis PN, White TL, Young RD, Bell JS, Winlove CP, Meek KM . Three-dimensional arrangement of elastic fibers in the human corneal stroma. Exp Eye Res 2015; 146: 43–53.
Bizheva K, Haines L, Mason E, MacLellan B, Tan B, Hileeto D et al. In vivo imaging and morphometry of the human pre-Descemet's layer and endothelium with ultrahigh-resolution optical coherence tomography. Invest Ophthalmol Vis Sci 2016; 57: 2782–2787.
Dua HS, Katamish T, Said DG, Faraj LA . Differentiating type 1 from type 2 big bubbles in deep anterior lamellar keratoplasty. Clin Ophthalmol 2015; 9: 1155–1157.
Anwar DS, Kruger MM, Mootha VV . Blunt scissors stromal dissection technique for deep anterior lamellar keratoplasty. Clin Ophthalmol 2014; 8: 1849–1854.
Liu Z, Zhang P, Liu C, Zhang W, Hong J, Wang W . Split of Descemet’s membrane and pre-Descemet’s layer in fungal keratitis: new definition of corneal anatomy incorporating new knowledge of fungal infection. Histopathology 2015; 66: 1046–1049.
Dua HS, Said DG . Clinical evidence of the pre-Descemets layer (Dua's layer) in corneal pathology. Eye 2016; 30: 1144–1145.
Yahia Chérif H, Gueudry J, Afriat M, Delcampe A, Attal P, Gross H et al. Efficacy and safety of pre-Descemet’s membrane sutures for the management of acute corneal hydrops in keratoconus. Br J Ophthalmol 2015; 99: 773–777.
Altaan SL, Gupta A, Sidney LE, Elalfy MS, Agarwal A, Dua HS . Endothelial cell loss following tissue harvesting by pneumodissection for endothelial keratoplasty: an ex vivo study. Br J Ophthalmol 2015; 99: 710–713.
Gamaleldin SA, Salama MM, Elshazly MI . Seven-day storage of pneumatically dissected Descemet’s endothelial grafts with and without Dua’s layer. Acta Ophthalmol 2016; 94: e130–e134.
Acknowledgements
This work was supported by The Royal College of Surgeons, Edinburgh, Scotland and Royal blind, Scotland.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
HSD is the inventor of the PDEK clamp, which is manufactured by e. janach, Italy. The instrument is not patented and no money has been paid by the manufacturer to the inventor.
Additional information
Supplementary Information accompanies this paper on EYE website
Supplementary information
Rights and permissions
About this article
Cite this article
Dua, H., Said, D. Pre-Descemets endothelial keratoplasty: the PDEK clamp for successful PDEK. Eye 31, 1106–1110 (2017). https://doi.org/10.1038/eye.2017.10
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2017.10
This article is cited by
-
Effect of Air Injection Depth on Big-bubble Formation in Lamellar Keratoplasty: an Ex Vivo Study
Scientific Reports (2019)