Abstract
Background/objectives:
Numbers of epidemiological studies assessing coffee consumption and serum lipids have yielded inconsistent results. We aimed to evaluate the effects of coffee intake on serum lipids.
Subjects/methods:
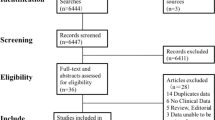
We searched several English and Chinese electronic databases up to September 2011 for randomized controlled trials of coffee on serum lipids. Weighted mean effect size was calculated for net changes in serum lipids by using random-effect models or fixed-effect models. Subgroup and meta-regression analyses were conducted to explore possible explanations for heterogeneity among trials.
Results:
Twelve studies conducted in Western countries with a total of 1017 subjects were identified. Meta-analyses showed, on average, drinking coffee for 45 days was associated with an increase of 8.1 mg/dl (95% confidence interval (CI): 4.5, 11.6; P<0.001) for total cholesterol (TC), 5.4 mg/dl (95% CI: 1.4, 9.5; P=0.009) for low-density lipoprotein cholesterol (LDL-C) and 12.6 mg/dl (95% CI: 3.5, 12.6; P=0.007) for triglyceride (TG). The increase in TC were greater in trials using unfiltered coffee and caffeinated coffee as the treatment group. Those who had hyperlipidemia were more sensitive to the cholesterol-raising effect of coffee. Meta-regression analysis revealed a positive dose-response relation between coffee intake and TC, LDL-C and TG.
Conclusion:
The intake of coffee especially unfiltered coffee is contributed significantly to the increase in TC, LDL-C and TG, and the changes were related to the level of intake. Studies of coffee intake on serum lipids in Asian populations should be performed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Butt MS . Sultan MT. Coffee and its consumption: benefits and risks. Crit Rev Food Sci Nutr 2011; 51: 363–373.
Yamashita K, Yatsuya H, Muramatsu T, Toyoshima H, Murohara T, Tamakoshi K . Association of coffee consumption with serum adiponectin, leptin, inflammation and metabolic markers in Japanese workers: a cross-sectional study. Nutrition and Diabetes 2012; 2: e33.
Balk L, Hoekstra T, Twisk J . Relationship between long-term coffee consumption and components of the metabolic syndrome: the Amsterdam Growth and Health Longitudinal Study. Eur J Epidemiol 2009; 24: 203–209.
Naidoo N, Chen C, Rebello SA, Speer K, Tai ES, Lee J et al. Cholesterol-raising diterpenes in types of coffee commonly consumed in Singapore, Indonesia and India and associations with blood lipids: a survey and cross sectional study. Nutr J 2011; 10: 48.
Nystad T, Melhus M, Brustad M, Lund E . The effect of coffee consumption on serum total cholesterol in the Sami and Norwegian populations. Public Health Nutr 2010; 13: 1818–1825.
Jee SH, He J, Appel LJ, Whelton PK, Suh I, Klag MJ . Coffee consumption and serum lipids: a meta-analysis of randomized controlled clinical trials. Am J Epidemiol 2001; 153: 353–362.
D'Amicis A, Scaccini C, Tomassi G, Anaclerio M, Stornelli R, Bernini A . Italian style brewed coffee: effect on serum cholesterol in young men. Int J Epidemiol 1996; 25: 513–520.
Caan B, Limb ES, Sweetnam MP, Fehily AM, Amarah L, Hutchings A . Instant coffee and cholesterol: A randomised controlled trial. Eur J Clin Nutr 1995; 49: 779–784.
Fried RE, Levine DM, Kwiterovich PO, Diamond EL, Wilder LB, Moy TF et al. The effect of filtered-coffee consumption on plasma lipid levels. Results of a randomized clinical trial. JAMA 1992; 267: 811–815.
Superko HR, Bortz WJ, Williams PT, Albers JJ, Wood PD . Caffeinated and decaffeinated coffee effects on plasma lipoprotein cholesterol, apolipoproteins, and lipase activity: a controlled, randomized trial. Am J Clin Nutr 1991; 54: 599–605.
Van Dusseldorp M, Katan MB, Van Vliet T, Demacker PNM, Stalenhoef AFH . Cholesterol-raising factor from boiled coffee does not pass a paper filter. Arterioscler Thromb 1991; 11: 586–593.
Rosmarin PC, Applegate WB, Somes GW . Coffee consumption and serum lipids: a randomized, crossover clinical trial. Am J Med 1990; 88: 349–356.
Burr ML, Gallacher JE, Butland BK, Bolton CH, Downs LG . Coffee blood pressure and plasma lipids: a randomized controlled trial. Eur J Clin Nutr 1989; 43: 477–483.
Bak AA, Grobbee DE . The effect on serum cholesterol levels of coffee brewed by filtering or boiling. N Engl J Med 1989; 321: 1432–1437.
Aro A, Tuomilehto J, Kostiainen E, Uusitalo U, Pietinen P . Boiled coffee increases serum low density lipoprotein concentration. Metabolism 1987; 36: 1027–1030.
Forde OH, Knutsen SF, Arnesen E, Thelle DS . The Tromso heart study: coffee consumption and serum lipid concentrations in men with hypercholesterolaemia: an randomised intervention study. Br Med J (Clin Res Ed) 1985; 290: 893–895.
Aro A, Kostiainen E, Huttunen JK, Seppala E, Vapaatalo H . Effects of coffee and tea on lipoproteins and prostanoids. Atherosclerosis 1985; 57: 123–128.
Christensen B, Mosdol A, Retterstol L, Landaas S, Thelle DS . Abstention from filtered coffee reduces the concentrations of plasma homocysteine and serum cholesterol--a randomized controlled trial. Am J Clin Nutr 2001; 74: 302–307.
McAnlis GT, McEneny J, Pearce J, Young IS . Black tea consumption does not protect low density lipoprotein from oxidative modification. Eur J Clin Nutr 1998; 52: 202–206.
Grubben MJ, Boers GH, Blom HJ, Broekhuizen R, de Jong R, van Rijt L et al. Unfiltered coffee increases plasma homocysteine concentrations in healthy volunteers: a randomized trial. Am J Clin Nutr 2000; 71: 480–484.
Higgins J, Green S Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.0 [updated February 2008]. The Cochrane Collaboration, 2008 Available from www.cochrane-handbook.org.
Wei M, Macera CA, Hornung CA, Blair SN . The impact of changes in coffee consumption on serum cholesterol. J Clin Epidemiol 1995; 48: 1189–1196.
Bai Z, Gao X, Han H, Bian Y . Effects of noise and caffeine on serum lipids. Occup Med 1992; 6: 326–327.
Mathias S, Garland C, Barrett-Connor E, Wingard DL . Coffee plasma cholesterol, and lipoproteins. A population study in an adult community. Am J Epidemiol 1985; 121: 896–905.
Shirlow MJ, Mathers CD . Caffeine consumption and serum cholesterol levels. Int J Epidemiol 1984; 13: 422–427.
Du Y, Melchert HU, Knopf H, Braemer-Hauth M, Gerding B, Pabel E . Association of serum caffeine concentrations with blood lipids in caffeine-drug users and nonusers—results of German National Health Surveys from 1984 to 1999. Eur J Epidemiol 2005; 20: 311–316.
Ranheim T, Halvorsen B . Coffee consumption and human health--beneficial or detrimental? --Mechanisms for effects of coffee consumption on different risk factors for cardiovascular disease and type 2 diabetes mellitus. Mol Nutr Food Res 2005; 49: 274–284.
Urgert R, Katan MB . The cholesterol-raising factor from coffee beans. Annu Rev Nutr 1997; 17: 305–324.
Cornelis MC, El-Sohemy A . Coffee caffeine, and coronary heart disease. Curr Opin Lipidol 2007; 18: 13–19.
Higdon JV, Frei B . Coffee and health: a review of recent human research. Crit Rev Food Sci Nutr 2006; 46: 101–123.
Lopez-Garcia E, Van Dam RM, Willett WC, Rimm EB, Manson JE, Stampfer MJ et al. Coffee consumption and coronary heart disease in men and women: a prospective cohort study. Circulation 2006; 113: 2045–2053.
Kawachi I, Colditz GA, Stone CB . Does coffee drinking increase the risk of coronary heart disease? Results from a meta-analysis. Br Heart J 1994; 72: 269–275.
Reis JP, Loria CM, Steffen LM, Zhou X, van Horn L, Siscovick DS et al. Coffee, decaffeinated coffee, caffeine, and tea consumption in young adulthood and atherosclerosis later in life: the CARDIA study. Arterioscler Thromb Vasc Biol 2010; 30: 2059–2066.
Larsson SC, Orsini N . Coffee consumption and risk of stroke: a dose-response meta-analysis of prospective studies. Am J Epidemiol 2011; 174: 993–1001.
Cornelis MC, El-Sohemy A . Coffee caffeine, and coronary heart disease. Curr Opin Clin Nutr Metab Care 2007; 10: 745–751.
Butt MS . Sultan MT. Coffee and its consumption: benefits and risks. Crit Rev Food Sci Nutr 2011; 51: 363–373.
Corti R, Sudano I, Spieker L, Binggeli C, Hermann F, Toenz D et al. Coffee--poison or medicine? Ther Umsch 2005; 62: 629–633.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Cai, L., Ma, D., Zhang, Y. et al. The effect of coffee consumption on serum lipids: a meta-analysis of randomized controlled trials. Eur J Clin Nutr 66, 872–877 (2012). https://doi.org/10.1038/ejcn.2012.68
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2012.68
Keywords
This article is cited by
-
A high Diabetes Risk Reduction Score (DRRS) is associated with a better cardio-metabolic profile among obese individuals
BMC Endocrine Disorders (2023)
-
Coffee intake and hypertension in Korean adults: results from KNHANES 2012–2016
Clinical Hypertension (2023)
-
Effect of Caffeine Consumption on Cardiovascular Disease: An Updated Review
Pharmaceutical Medicine (2023)
-
Incidence of diabetes and its predictors in the Greater Beirut Area: a five-year longitudinal study
Diabetology & Metabolic Syndrome (2022)
-
Causal relationship from coffee consumption to diseases and mortality: a review of observational and Mendelian randomization studies including cardiometabolic diseases, cancer, gallstones and other diseases
European Journal of Nutrition (2022)