Abstract
Background/Objectives:
Gut hormones have been shown to influence energy intake (EI). To our knowledge, no study has investigated the effects of dietary patterns aimed at optimizing fullness on EI, appetite and gut hormones.
Subject/Methods:
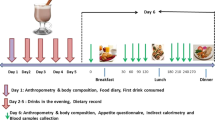
To determine whether individually timing high-protein preloads would impact EI, appetite, and peptide YY and glucagon-like peptide-1 (GLP-1) levels. Ten men (body mass index=25.5±2.6 kg/m2) participated in a randomized crossover trial. The three conditions consisted of the self-selection of snacks (condition 1), or the consumption of a preload (300 kcal: 40% protein, 40% carbohydrates and 20% fat) at either 15 min (condition 2) or ∼ 50 min (individually set) (condition 3) before lunch and dinner. During each condition, a standardized breakfast was served, whereas lunch and dinner were self-selected from a five-item menu, and eaten ad libitum. Mealtime and daily EI were measured. Appetite, peptide YY and GLP-1 were sampled over 9 h.
Results:
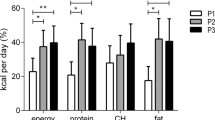
No differences in daily EI were noted across conditions (1=3078±720 kcal; 2=2929±264 kcal; 3=2998±437 kcal; not significant). For the most part, daily profiles as well as premeal levels of peptide YY and GLP-1 were not different between conditions. Desire to eat, hunger and prospective food consumption were found to be lowest during condition 1 (P<0.05).
Conclusions:
According to these results, it would seem that individually timing high-protein preloads does not reduce daily EI in healthy human subjects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Adrian TE, Ferri GL, Bacarese-Hamilton AJ, Fuessl HS, Polak JM, Bloom SR (1985). Human distribution and release of a putative new gut hormone, peptide YY. Gastroenterology 89, 1070–1077.
Batterham RL, Cowley MA, Small CJ, Herzog H, Cohen MA, Dakin CL et al. (2002). Gut hormone PYY(3-36) physiologically inhibits food intake. Nature 418, 650–654.
Batterham RL, Cohen MA, Ellis SM, Le Roux CW, Withers DJ, Frost GS et al. (2003). Inhibition of food intake in obese subjects by peptide YY3-36. N Engl J Med 349, 941–948.
Batterham RL, Heffron H, Kapoor S, Chivers JE, Chandarana K, Herzog H et al. (2006). Critical role for peptide YY in protein-mediated satiation and body-weight regulation. Cell Metab 4, 223–233.
Challis BG, Pinnock SB, Coll AP, Carter RN, Dickson SL, O’Rahilly S (2003). Acute effects of PYY3-36 on food intake and hypothalamic neuropeptide expression in the mouse. Biochem Biophys Res Commun 311, 915–919.
Chan JL, Mun EC, Stoyneva V, Mantzoros CS, Goldfine AB (2006). Peptide YY levels are elevated after gastric bypass surgery. Obesity (Silver Spring) 14, 194–198.
Cummings DE, Weigle DS, Frayo RS, Breen PA, Ma MK, Dellinger EP et al. (2002). Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med 346, 1623–1630.
Degen L, Oesch S, Casanova M, Graf S, Ketterer S, Drewe J et al. (2005). Effect of peptide YY3-36 on food intake in humans. Gastroenterology 129, 1430–1436.
Doucet E, Cameron J (2007). Appetite control after weight loss: what is the role of bloodborne peptides? Appl Physiol Nutr Metab 32, 523–532.
Doucet E, Laviolette M, Imbeault P, Strychar I, Rabasa-Lhoret R, Prud’homme D (2008). Total peptide YY is a correlate of postprandial energy expenditure but not of appetite or energy intake in healthy women. Metabolism 57, 1458–1464.
Drapeau V, King N, Hetherington M, Doucet E, Blundell J, Tremblay A (2007). Appetite sensations and satiety quotient: Predictors of energy intake and weight loss. Appetite 48, 159–166.
Elliott RM, Morgan LM, Tredger JA, Deacon S, Wright J, Marks V (1993). Glucagon-like peptide-1 (7-36) amide and glucose-dependent insulinotropic polypeptide secretion in response to nutrient ingestion in man: acute post-prandial and 24-h secretion patterns. J Endocrinol 138, 159–166.
Flint A, Raben A, Astrup A, Holst JJ (1998). Glucagon-like peptide 1 promotes satiety and suppresses energy intake in humans. J Clin Invest 101, 515–520.
Flint A, Raben A, Ersboll AK, Holst JJ, Astrup A (2001). The effect of physiological levels of glucagon-like peptide-1 on appetite, gastric emptying, energy and substrate metabolism in obesity. Int J Obes Relat Metab Disord 25, 781–792.
Gutzwiller JP, Drewe J, Goke B, Schmidt H, Rohrer B, Lareida J et al. (1999). Glucagon-like peptide-1 promotes satiety and reduces food intake in patients with diabetes mellitus type 2. Am J Physiol 276, R1541–R1544.
Hill AJ, Blundell JE (1986). The effects of a high-protein or high-carbohydrate meal on subjective motivation to eat and food preferences. Nutr Behav 3, 133–144.
Holst JJ (2007). The physiology of glucagon-like peptide 1. Physiol Rev 87, 1409–1439.
Hulshof T, De Graaf C, Weststrate JA (1993). The effects of preloads varying in physical state and fat content on satiety and energy intake. Appetite 21, 273–286.
Johnstone AM, Shannon E, Whybrow S, Reid CA, Stubbs RJ (2000). Altering the temporal distribution of energy intake with isoenergetically dense foods given as snacks does not affect total daily energy intake in normal-weight men. Br J Nutr 83, 7–14.
Korner J, Bessler M, Cirilo LJ, Conwell IM, Daud A, Restuccia NL et al. (2005). Effects of Roux-en-Y gastric bypass surgery on fasting and postprandial concentrations of plasma ghrelin, peptide YY, and insulin. J Clin Endocrinol Metab 90, 359–365.
Korner J, Inabnet W, Conwell IM, Taveras C, Daud A, Olivero-Rivera L et al. (2006). Differential effects of gastric bypass and banding on circulating gut hormone and leptin levels. Obesity (Silver Spring) 14, 1553–1561.
Korner J, Bessler M, Inabnet W, Taveras C, Holst JJ (2007). Exaggerated glucagon-like peptide-1 and blunted glucose-dependent insulinotropic peptide secretion are associated with Roux-en-Y gastric bypass but not adjustable gastric banding. Surg Obes Relat Dis 3, 597–601.
le Roux CW, Aylwin SJ, Batterham RL, Borg CM, Coyle F, Prasad V et al. (2006a). Gut hormone profiles following bariatric surgery favor an anorectic state, facilitate weight loss, and improve metabolic parameters. Ann Surg 243, 108–114.
le Roux CW, Batterham RL, Aylwin SJ, Patterson M, Borg CM, Wynne KJ et al. (2006b). Attenuated peptide YY release in obese subjects is associated with reduced satiety. Endocrinology 147, 3–8.
le Roux CW, Welbourn R, Werling M, Osborne A, Kokkinos A, Laurenius A et al. (2007). Gut hormones as mediators of appetite and weight loss after Roux-en-Y gastric bypass. Ann Surg 246, 780–785.
Morinigo R, Moize V, Musri M, Lacy AM, Navarro S, Marin JL et al. (2006). Glucagon-like peptide-1, peptide YY, hunger, and satiety after gastric bypass surgery in morbidly obese subjects. J Clin Endocrinol Metab 91, 1735–1740.
Naslund E, Barkeling B, King N, Gutniak M, Blundell JE, Holst JJ et al. (1999). Energy intake and appetite are suppressed by glucagon-like peptide-1 (GLP-1) in obese men. Int J Obes Relat Metab Disord 23, 304–311.
Naslund E, Gryback P, Hellstrom PM, Jacobsson H, Holst JJ, Theodorsson E et al. (1997a). Gastrointestinal hormones and gastric emptying 20 years after jejunoileal bypass for massive obesity. Int J Obes Relat Metab Disord 21, 387–392.
Naslund E, Hellstrom PM (1998). Glucagon-like peptide-1 in the pathogenesis of obesity. Drug News Perspect 11, 92–97.
Naslund E, Melin I, Gryback P, Hagg A, Hellstrom PM, Jacobsson H et al. (1997b). Reduced food intake after jejunoileal bypass: a possible association with prolonged gastric emptying and altered gut hormone patterns. Am J Clin Nutr 66, 26–32.
Onaga T, Zabielski R, Kato S (2002). Multiple regulation of peptide YY secretion in the digestive tract. Peptides 23, 279–290.
Orskov C, Wettergren A, Holst JJ (1996). Secretion of the incretin hormones glucagon-like peptide-1 and gastric inhibitory polypeptide correlates with insulin secretion in normal man throughout the day. Scand J Gastroenterol 31, 665–670.
Sloth B, Holst JJ, Flint A, Gregersen NT, Astrup A (2007). Effects of PYY1-36 and PYY3-36 on appetite, energy intake, energy expenditure, glucose and fat metabolism in obese and lean subjects. Am J Physiol Endocrinol Metab 292, E1062–E1068.
Toft-Nielsen MB, Madsbad S, Holst JJ (1999). Continuous subcutaneous infusion of glucagon-like peptide 1 lowers plasma glucose and reduces appetite in type 2 diabetic patients. Diabetes Care 22, 1137–1143.
Tournier A, Louis-Sylvestre J (1991). Effect of the physical state of a food on subsequent intake in human subjects. Appetite 16, 17–24.
Viskaal-van Dongen M, Kok FJ, de Graaf C (2009). Effects of snack consumption for 8 weeks on energy intake and body weight. Int J Obes (London) 34, 319–326.
Zijlstra N, Mars M, de Wijk RA, Westerterp-Plantenga MS, Holst JJ, de Graaf C (2009). Effect of viscosity on appetite and gastro-intestinal hormones. Physiol Behav 97, 68–75.
Acknowledgements
This study was supported by the Canadian Institutes of Health Research (Grant no. 79597). Éric Doucet is a recipient of a CIHR/Merck-Frosst New Investigator Award, CFI/OIT New Opportunities Award and of an Early Research Award.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Contributors: ED was involved in the conception of the study. SW collected the data. SW and ED analyzed and interpreted the data and wrote the article.
Supplementary Information accompanies the paper on European Journal of Clinical Nutrition website
Rights and permissions
About this article
Cite this article
Willbond, S., Doucet, É. Individually timing high-protein preloads has no effect on daily energy intake, peptide YY and glucagon-like peptide-1. Eur J Clin Nutr 65, 55–62 (2011). https://doi.org/10.1038/ejcn.2010.188
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2010.188