Abstract
Background/Objectives:
The detection of malnutrition in the intensive care unit (ICU) is critical to appropriately address its contribution on outcomes. The primary objective of this investigation was to determine if nutritional status could be reliably classified using subjective global assessment (SGA) in mechanically ventilated (MV) patients.
Subjects/Methods:
Fifty-seven patients requiring MV >48 h in a university-affiliated medical ICU were evaluated in this cross-sectional study over a 3-month period. Nutritional status was categorized independently by two registered dietitians using SGA. Frequencies, means (+ s.d.), χ2 and t-tests were used to describe the population characteristics; agreement between raters was evaluated using the κ statistic.
Results:
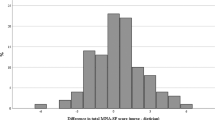
On admission, the average patient was 50.4 (±14.2) years of age, overweight (body mass index: 29.0±9.2kg/m2), had an acute physiology and chronic health evaluation II score of 24 (±10) and respiratory failure. Fifty percent (n=29) of patients were categorized as malnourished. Agreement between raters was 95% before consensus, reflecting near perfect agreement (κ=0.90) and excellent reliability. Patients categorized as malnourished were more often admitted to the hospital floor before the ICU (n=32; 56%), reported decreased dietary intake (69 vs 46%, P=0.02) and exhibited signs of muscle wasting (45 vs 7%, P<0.001, respectively) and fat loss (52 vs 7%, P<0.001, respectively) on physical exam when compared with normally nourished individuals.
Conclusions:
SGA can serve as a reliable nutrition assessment technique for detecting malnutrition in patients requiring MV. Its routine use should be incorporated into future studies and clinical practice.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Atalay BG, Yagmur C, Nursal TZ, Atalay H, Noyan T (2008). Use of subjective global assessment and clinical outcomes in critically ill geriatric patients receiving nutrition support. JPEN J Parenter Enteral Nutr 32, 454–459.
Baker JP, Detsky AS, Wesson DE, Wolman SL, Stewart S, Whitewell J et al. (1982). Nutritional assessment: a comparison of clinical judgement and objective measurements. N Engl J Med 306, 969–972.
Braunschweig C, Gomez S, Sheean PM (2000). Impact of declines in nutritional status on outcomes in adult patients hospitalized for more than 7 days. J Am Diet Assoc 100, 1316–1322.
Butterworth C (1974). The skeleton in the hospital closet. Nutr Today 9, 4–8.
Corish CA, Kennedy NP (2000). Protein-energy undernutrition in hospital in-patients. Br J Nutr 83, 575–591.
Correia MI, Waitzberg DL (2003). The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 22, 235–239.
de Jonghe B, Lacherade JC, Sharshar T, Outin H (2009). Intensive care unit-acquired weakness: risk factors and prevention. Crit Care Med 37, S309–S315.
Detsky AS, Baker JP, O'Rourke K, Johnston N, Whitwell J, Mendelson RA et al. (1987a). Predicting nutrition-associated complications for patients undergoing gastrointestinal surgery. JPEN J Parenter Enteral Nutr 11, 440–446.
Detsky AS, McLaughlin JR, Baker JP, Johnston N, Whittaker S, Mendelson RA et al. (1987b). What is subjective global assessment of nutritional status? JPEN J Parenter Enteral Nutr 11, 8–13.
Detsky AS, Smalley PS, Chang J (1994). The rational clinical examination. Is this patient malnourished? JAMA 271, 54–58.
Ferguson M, Capra S, Bauer J, Banks M (1999). Development of a valid and reliable malnutrition screening tool for adult acute hospital patients. Nutrition 15, 458–464.
Fuhrman MP, Charney P, Mueller CM (2004). Hepatic proteins and nutrition assessment. J Am Diet Assoc 104, 1258–1264.
Fung F, Sherrard DJ, Gillen DL, Wong C, Kestenbaum B, Seliger S et al. (2002). Increased risk for cardiovascular mortality among malnourished end-stage renal disease patients. Am J Kidney Dis 40, 307–314.
Gabay C, Kushner I (1999). Acute-phase proteins and other systemic responses to inflammation. N Engl J Med 340, 448–454.
Gamrin L, Andersson K, Hultman E, Nilsson E, Essen P, Wernerman J (1997). Longitudinal changes of biochemical parameters in muscle during critical illness. Metabolism 46, 756–762.
Giner M, Laviano A, Meguid MM, Gleason JR (1996). In 1995 a correlation between malnutrition and poor outcome in critically ill patients still exists. Nutrition 12, 23–29.
Gottschlich M ed. (2007). The A.S.P.E.N. Nutrition Support Core Curriculum. 3rd edn. American Society of Parenteral and Enteral Nutrition: Silver Spring, MD.
Griffiths RD (2003). Nutrition support in critically ill septic patients. Curr Opin Clin Nutr Metab Care 6, 203–210.
Hirsch S, de Obaldia N, Petermann M, Rojo P, Barrientos C, Iturriaga H et al. (1991). Subjective global assessment of nutritional status: further validation. Nutrition 7, 35–37.
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985). APACHE II: a severity of disease classification system. Crit Care Med 13, 818–829.
Kondrup J, Rasmussen HH, Hamberg O, Stanga Z (2003). Nutritional risk screening (NRS 2002): a new method based on an analysis of controlled clinical trials. Clin Nutr 22, 321–336.
Kyle UG, Pirlich M, Schuetz T, Luebke HJ, Lochs H, Pichard C (2003). Prevalence of malnutrition in 1760 patients at hospital admission: a controlled population study of body composition. Clin Nutr 22, 473–481.
Lacey K, Pritchett E (2003). Nutrition care process and model: ADA adopts road map to quality care and outcomes management. J Am Diet Assoc 103, 1061–1072.
Landis JR, Koch GG (1977). An application of hierarchical kappa-type statistics in the assessment of majority agreement among multiple observers. Biometrics 33, 363–374.
Lee R, Nieman DC (2007). Clinical Assessment of Nutritional Status IN: Nutritional Assessment. 4th edn. McGraw-Hill: New York. pp 354–371.
Martineau J, Bauer JD, Isenring E, Cohen S (2005). Malnutrition determined by the patient-generated subjective global assessment is associated with poor outcomes in acute stroke patients. Clin Nutr 24, 1073–1077.
McClave SA, Martindale RG, Vanek VW, McCarthy M, Roberts P, Taylor B et al. (2009). Guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). JPEN J Parenter Enteral Nutr 33, 277–316.
McWhirter JP, Pennington CR (1994). Incidence and recognition of malnutrition in hospital. Br Med J 308, 945–948.
Naber TH, Schermer T, de Bree A, Nusteling K, Eggink L, Kruimel JW (1997). Prevalence of malnutrition in nonsurgical hospitalized patients and its association with disease complications. Am J Clin Nutr 66, 1232–1239.
Plank LD, Connolly AB, Hill GL (1998). Sequential changes in the metabolic response in severely septic patients during the first 23 days after the onset of peritonitis. Ann Surg 228, 146–158.
Stephenson GR, Moretti EW, El-Moalem H, Clavien PA, Tuttle-Newhall JE (2001). Malnutrition in liver transplant patients: preoperative subjective global assessment is predictive of outcome after liver transplantation. Transplantation 72, 666–670.
Stratton RJ, Hackston A, Longmore D, Dixon R, Price S, Stroud M et al. (2004). Malnutrition in hospital outpatients and inpatients: prevalence, concurrent validity and ease of use of the ‘malnutrition universal screening tool’ (‘MUST’) for adults. Br J Nutr 92, 799–808.
Sungurtekin H, Sungurtekin U, Balci C, Zencir M, Erdem E (2004). The influence of nutritional status on complications after major intraabdominal surgery. J Am Coll Nutr 23, 227–232.
Sungurtekin H, Sungurtekin U, Oner O, Okke D (2008). Nutrition assessment in critically ill patients. Nutr Clin Pract 23, 635–641.
Ulander K, Grahn G, Jeppsson B (1993). Subjective assessment of nutritional status-validity and reliability of a modified Detsky index in a Swedish setting. Clin Nutr 12, 15–19.
Vincent JL, Norrenberg M (2009). Intensive care unit-acquired weakness: framing the topic. Crit Care Med 37, S296–S298.
Waitzberg DL, Caiaffa WT, Correia MI (2001). Hospital malnutrition: the Brazilian national survey (IBRANUTRI): a study of 4000 patients. Nutrition 17, 573–580.
Zimmerman JE, Kramer AA, McNair DS, Malila FM (2006). Acute physiology and chronic health evaluation (APACHE) IV: hospital mortality assessment for today's critically ill patients. Crit Care Med 34, 1297–1310.
Acknowledgements
The study was funded, in part, by a grant from the National Institutes of Health, National Heart Lung and Blood Institute no. R01 HL093142-02.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Sheean, P., Peterson, S., Gurka, D. et al. Nutrition assessment: the reproducibility of subjective global assessment in patients requiring mechanical ventilation. Eur J Clin Nutr 64, 1358–1364 (2010). https://doi.org/10.1038/ejcn.2010.154
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2010.154
Keywords
This article is cited by
-
Obesity and critical care nutrition: current practice gaps and directions for future research
Critical Care (2022)
-
Current clinical nutrition practices in critically ill patients in Latin America: a multinational observational study
Critical Care (2017)
-
Nutrition artificielle en réanimation
Réanimation (2014)
-
Monitoring der künstlichen Ernährung bei kritisch kranken Patienten
Intensivmedizin und Notfallmedizin (2011)