- WORLD VIEW
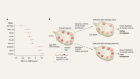
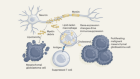
Cancer research needs better databases
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 610, 607 (2022)
doi: https://doi.org/10.1038/d41586-022-03390-4
Competing Interests
T. S. K. E.-M. is an external scientific consultant at Datavant, which sells data-linkage software.


 Cancer ‘moonshot’ has lofty new goal: halve deaths in 25 years
Cancer ‘moonshot’ has lofty new goal: halve deaths in 25 years
 Clarifying the burden of ovarian cancer
Clarifying the burden of ovarian cancer
 Untangling the complex roots of cancer in Brazil
Untangling the complex roots of cancer in Brazil
 How engineers and drug developers are working to change childhood cancer’s deadly calculus
How engineers and drug developers are working to change childhood cancer’s deadly calculus