Credit: Eva Marie Uzcategui/Bloomberg/Getty
As clinical trials get under way for COVID-19 vaccines, a worryingly high number of people around the world are saying they don’t plan to get inoculated — an act that could put them in harm’s way and delay the end of the pandemic.
Concerns about approvals being rushed, suspicion of the pharmaceutical industry and a pandemic of vaccine misinformation are combining to erode the public’s trust in the process by which vaccines are approved for use.
And fears of political interference are not helping. In the United States, President Donald Trump has repeatedly contradicted public-health experts by saying that a vaccine could be available by the November presidential election — prompting concerns that his administration could put pressure on regulators to approve a vaccine before data show that it is effective and safe. Similar concerns have dogged the rapid approval of vaccines for clinical use in China and Russia.
COVID-vaccine results are on the way — and scientists’ concerns are growing
The pharmaceutical industry in particular must do more to build and maintain vaccine confidence. As we report this week in a News story, companies are in talks on this very question. They, and their academic partners, must agree to a higher standard of transparency in their communication of the process and reporting of clinical trials.
In early September, a multi-country clinical trial of a leading vaccine candidate that is being developed by AstraZeneca and the University of Oxford, UK, was paused while researchers evaluated a possible safety risk affecting one of its participants. Pauses are not uncommon in such trials; it’s a sign that investigators are following safety protocols strictly. That’s reassuring, considering the pressure scientists are under to test this vaccine rapidly.
But the fact that the trial’s leaders chose not to engage with questions from researchers, reporters and members of the public is adding to safety concerns. Although the trial has been restarted in Brazil, South Africa and the United Kingdom, it remains on hold in the United States.
Who gets a COVID vaccine first? Access plans are taking shape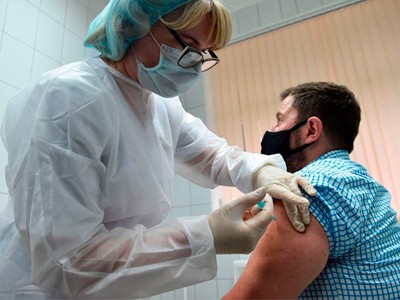
Confidentiality is important in a trial. Participants’ privacy needs to be respected, and prematurely releasing some information could bias investigators while a trial is ongoing.
But there are fewer good reasons to keep other information secret. For example, pharmaceutical companies tend not to publish the details — known as protocols — of how a trial is to be conducted and assessed. And in some cases, they do not release actual clinical trial results.
Making protocols and results public allows researchers independent of the trial to assess the data, and verify reported results and claims. It also enables researchers to use the data in new ways, which could prompt further studies. This maximizes the benefits of a clinical trial for society, not only resulting in a more transparent evaluation of the therapy being tested, but potentially leading to better vaccines in the long run.
Companies counter that such details can reveal crucial information to their competitors. But they must find a way to balance this with their responsibility to study participants, without whom there would be no trials. Participants might hope to benefit from a trial themselves, but they also put their health at risk to help further research that can benefit society at large. The best way to maximize the chances of achieving this objective is to open the trial protocol and results to scrutiny.
The unequal scramble for coronavirus vaccines — by the numbers
In response to these arguments and pressure from researchers, the drug companies seem to be listening. First Moderna, Pfizer and AstraZeneca, and then, last week, Johnson & Johnson and its partners, have made public clinical-trial protocols for vaccine candidates that are in phase III clinical trials — each involving tens of thousands of participants. The details in these protocols show how the effectiveness of these vaccines will be evaluated; the possible timing of results; and what criteria could be used to halt a trial early, if a vaccine clearly works.
Such openness is likely to continue for COVID-19 vaccines during the pandemic. But it cannot end with this virus. Future trials need transparency, too.
Those running vaccine trials and studies of potential COVID-19 treatments must consider how to change. It should be possible for clinical-trial sponsors to be more transparent, not only with protocols, but also with data gleaned from trials. The question is how to do this.
History has shown that once public trust in vaccines has been compromised it is difficult to win back — and that distrust in one vaccine can fuel concerns about others. People wary of a COVID-19 vaccine might be less likely to get vaccinated against other ailments, fuelling the vaccine-hesitancy movement that has already led to dangerous resurgences of diseases such as measles that were once largely contained. The causes of vaccine hesitancy are complex. But delays and reluctance in communicating results, or outright secrecy, do not help. Researchers, publishers, regulators, policymakers — and especially pharmaceutical companies — need to accept this if we are to succeed in quickly disrupting the path of the pandemic.

 COVID-vaccine results are on the way — and scientists’ concerns are growing
COVID-vaccine results are on the way — and scientists’ concerns are growing
 Who gets a COVID vaccine first? Access plans are taking shape
Who gets a COVID vaccine first? Access plans are taking shape
 Scientists relieved as coronavirus vaccine trial restarts — but question lack of transparency
Scientists relieved as coronavirus vaccine trial restarts — but question lack of transparency
 The unequal scramble for coronavirus vaccines — by the numbers
The unequal scramble for coronavirus vaccines — by the numbers