- NEWS FEATURE
How COVID-19 can damage the brain
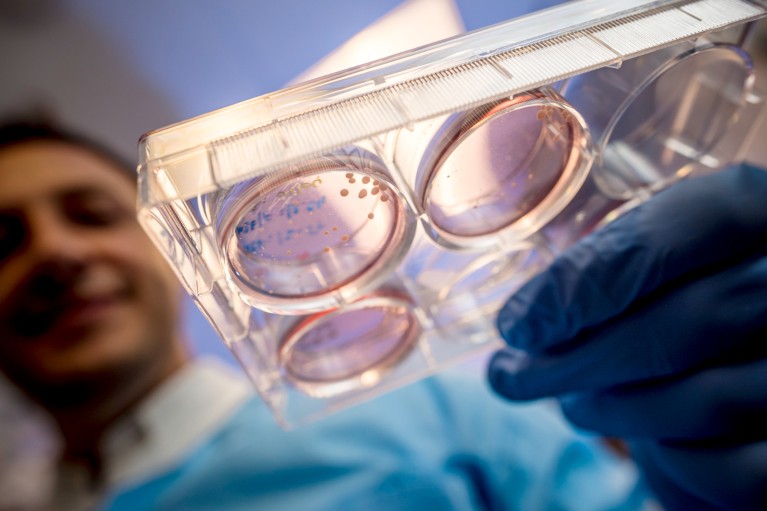
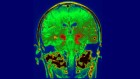
Some evidence that SARS-CoV-2 can infect the brain comes from ‘organoids’ — clumps of neurons created in a dish. Credit: Erik Jepsen/UC San Diego
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 585, 342-343 (2020)
doi: https://doi.org/10.1038/d41586-020-02599-5
References
Paterson, R. W. et al. Brain https://doi.org/10.1093/brain/awaa240 (2020).
Kotfis, K. et al. Crit. Care 24, 176 (2020).
Moriguchi, T. et al. Int. J. Infect. Dis. 94, 55–58 (2020).
Zanin, L. et al. Acta Neurochir. 162, 1491–1494 (2020).
Varatharaj, A. et al. Lancet Psychiatry https://doi.org/10.1016/S2215-0366(20)30287-X (2020).
Ellul, M. A. et al. Lancet Neurol. 19, 767–783 (2020).
Mesci, P. et al. Preprint at bioRxiv https://doi.org/10.1101/2020.05.30.125856 (2020).
Song, E. et al. Preprint at bioRxiv https://doi.org/10.1101/2020.06.25.169946 (2020).
Bryce, C. et al. Preprint at medRxiv https://doi.org/10.1101/2020.05.18.20099960 (2020).
Al Saiegh, F. et al. J. Neurol. Neurosurg. Psychiatry 91, 846–848 (2020).
Li, M.-Y., Li, L., Zhang, Y. & Wang, X.-S. Infect. Dis. Poverty 9, 45 (2020).

 How many people has the coronavirus killed?
How many people has the coronavirus killed?
 Autopsy slowdown hinders quest to determine how coronavirus kills
Autopsy slowdown hinders quest to determine how coronavirus kills
 Profile of a killer: the complex biology powering the coronavirus pandemic
Profile of a killer: the complex biology powering the coronavirus pandemic