- OUTLOOK
How cancer genomics is transforming diagnosis and treatment

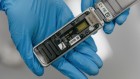
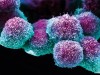
DNA sequencing allows oncologists to characterize tumours on the basis of genetic mutations. Credit: KTSDESIGN/SPL
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 579, S10-S11 (2020)
doi: https://doi.org/10.1038/d41586-020-00845-4
This article is part of Nature Outlook: Cancer diagnosis, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Schmitz, R. et al. N. Engl. J. Med. 378, 1396–1407 (2018).
van der Velden, D. L. et al. Nature 574, 127–131 (2019).
Berland, L. et al. J. Thorac. Dis. 11, S71–S80 (2019).

 The pros and cons of screening
The pros and cons of screening
 We need more evidence to answer questions about screening
We need more evidence to answer questions about screening
 Could liquid biopsies help deliver better treatment?
Could liquid biopsies help deliver better treatment?
 The future of liquid biopsy
The future of liquid biopsy
 Will a test to detect early pancreatic cancer ever be possible?
Will a test to detect early pancreatic cancer ever be possible?
 How AI is improving cancer diagnostics
How AI is improving cancer diagnostics
 Better cancer screening in resource-poor nations
Better cancer screening in resource-poor nations
 Research round-up: Cancer diagnosis
Research round-up: Cancer diagnosis