- COMMENT
Genomics: data sharing needs an international code of conduct
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 578, 31-33 (2020)
doi: https://doi.org/10.1038/d41586-020-00082-9
References
Rozenblatt-Rosen, O. et al. Nature 550, 451–453 (2017).
Nature 523, 136–137 (2015).
Stein, L. D., Knoppers, B. M., Campbell, P., Getz, G. & Korbel, J. O. Nature 523, 149–151 (2015).
Mochama, V. ‘DNA testing to aid deportations leaves plenty of room for misinterpretation and mistreatment’ (The Star, 29 July 2018).
Ohm, P. UCLA Law Rev. 57, 1701–1777 (2010).
El Emam, K. & Arbuckle, L. Anonymizing Health Data (O’Reilly, 2013).
Phillips, M. & Knoppers, B .M. Nature Biotechnol. 34, 1102–1103 (2016).
Phillips, M., Dove, E. S. & Knoppers, B. M. J. Bioeth. Inq. 14, 527–539 (2017).
Rocher, L., Hendrickx, J. M. & de Montjoye, Y.-A. Nature Commun. 10, 3069 (2019).
Shringapure, S. S. & Bustamante, C. D. Am. J. Hum. Genet. 97, 631–646 (2015).
Contreras, J. L. & Knoppers, B. M. Annu. Rev. Genom. Hum. Genet. 19, 429–453 (2018).
Thorogood, A. et al. Hum. Genomics 12, 7 (2018).
Thorogood, A., Dalpé, G. & Knoppers. B. M. Eur. J. Hum. Genet. 27, 535–546 (2019).
Wolf, L. E. et al. J. Law Med. Ethics 43, 594–609 (2015).
Knoppers, B. Nature 558, 189 (2018).
Birney, E., Vamathevan, J. & Goodhand. P. Preprint at bioRxiv https://doi.org/10.1101/203554 (2017).

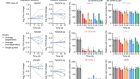
 Global genomics project unravels cancer’s complexity at unprecedented scale
Global genomics project unravels cancer’s complexity at unprecedented scale
 Read the paper: Pan-cancer analysis of whole genomes
Read the paper: Pan-cancer analysis of whole genomes
 Create a cloud commons
Create a cloud commons
 Crack down on genomic surveillance
Crack down on genomic surveillance
 Science needs clarity on Europe’s data-protection law
Science needs clarity on Europe’s data-protection law