- NEWS AND VIEWS
Survival skills ensure that cancer spreads
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 573, 353-354 (2019)
doi: https://doi.org/10.1038/d41586-019-02570-z
References
Kennecke, H. et al. J. Clin. Oncol. 28, 3271–3277 (2010).
Bogenrieder, T. & Herlyn, M. Oncogene 22, 6524–6536 (2003).
Padmanaban, V. et al. Nature 573, 439–444 (2019).
Yang, J. & Weinberg, R. A. Dev. Cell 14, 818–829 (2008).
Nakaya, Y. & Sheng, G. Dev. Growth Differ. 50, 755–766 (2008).
Haensel, D. & Dai, X. Dev. Dyn. 247, 473–480 (2018).
Aiello, N. M. & Kang, Y. J. Exp. Med. 216, 1016–1026 (2019).
Onder, T. T. et al. Cancer Res. 68, 3645–3654 (2008).
Frixen, U. H. et al. J. Cell Biol. 113, 173–185 (1991).
Derksen, P. W. B. et al. Cancer Cell 10, 437–449 (2006).
Ciriello, G. et al. Cell 163, 506–519 (2015).
Onder, T. T. et al. Cancer Res. 68, 3645–3654 (2008).
Chaffer, C. L. et al. Cancer Res. 66, 11271–11287 (2006).
Acs, G., Lawton, T. J., Rebbeck, T. R., LiVolsi, V. A. & Zhang, P. J. Am. J. Clin. Pathol. 115, 85–98 (2001).
Kowalski, P. J., Rubin, M. A. & Kleer, C. G. Breast Cancer Res. 5, R217–R222 (2003).
Pastushenko, I. & Blanpain, C. Trends Cell Biol. 29, 212–226 (2019).
Zhang, Z. et al. Cell Death Dis. 9, 83 (2018).
Pastushenko, I. et al. Nature 556, 463–468 (2018).
Aceto, N. et al. Cell 158, 1110–1122 (2014).

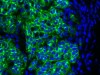 Read the paper: E-cadherin is required for metastasis in multiple models of breast cancer
Read the paper: E-cadherin is required for metastasis in multiple models of breast cancer
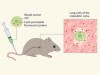 Cells tagged near an early spread of cancer
Cells tagged near an early spread of cancer
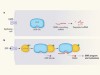 Metabolic signal curbs cancer-cell migration
Metabolic signal curbs cancer-cell migration