- NEWS AND VIEWS
Human embryo implantation modelled in microfluidic channels
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 573, 350-351 (2019)
doi: https://doi.org/10.1038/d41586-019-02563-y
References
Wang, X. et al. Fertil. Steril. 79, 577–584 (2003).
Zheng, Y. et al. Nature 573, 421–425 (2019).
Shao, Y. et al. Nature Commun. 8, 208 (2017).
Christodoulou, N. et al. Nature Cell Biol. 20, 1278–1289 (2018).
Simunovic, M. et al. Nature Cell Biol. 21, 900–910 (2019).
Deglincerti, A. et al. Nature 533, 251–254 (2016).
Nakamura, T. et al. Nature 537, 57–62 (2016).
Itskovitz-Eldor, J. et al. Mol. Med. 6, 88–95 (2000).
Spence, J. R. et al. Nature 470, 105–109 (2011).
Irie, N. et al. Cell 160, 253–268 (2015).
Aach, J., Lunshof, J., Iyer, E. & Church, G. M. eLife 6, e20674 (2017).

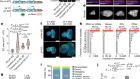
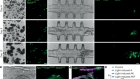
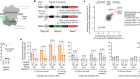
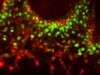 Read the paper: Controlled modelling of human epiblast and amnion development using stem cells
Read the paper: Controlled modelling of human epiblast and amnion development using stem cells
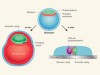 Implantation barrier overcome
Implantation barrier overcome
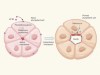 Early embryos kept in check
Early embryos kept in check