- COMMENT
Which biological systems should be engineered?

Children receiving blood transfusions in Bangladesh, where maintaining the supply from donors can be more challenging than in wealthy countries. Credit: Noor Alam/ZUMA Wire
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 563, 177-179 (2018)
doi: https://doi.org/10.1038/d41586-018-07291-3
References
Morrow, J. F. et al. Proc. Natl Acad. Sci. USA 71, 1743–1747 (1974).
Chalfie, M. et al. Science 263, 802–805 (1994).
Wang, S. & Hazelrigg, T. Nature 369, 400–403 (1994).
Porter, D. L., Levine, B. L., Kalos, M., Bagg, A. & June, C. H. N. Engl. J. Med. 365, 725–733 (2011).
Majumder, S. & Liu, A. P. Phys. Biol. 15, 013001 (2017).
Richmond, D. L. et al. Proc. Natl Acad. Sci. USA 108, 9431–9436 (2011).
Weiss, M. et al. Nature Mater. 17, 89–96 (2018).
Dezi, M., Di Cicco, A., Bassereau, P. & Lévy, D. Proc. Natl Acad. Sci. USA 110, 7276–7281 (2013).
Sharma, P. & Allison, J. P. Science 348, 56–61 (2015).
June, C. H., O’Connor, R. S., Kawalekar, O. U., Ghassemi, S. & Milone, M. C. Science 359, 1361–1365 (2018).
Morsut, L. et al. Cell 164, 780–791 (2016).
Abu Shah, E. & Keren, K. eLife 3, e01433 (2014).
Weitz, M. et al. Nature Chem. 6, 295–302 (2014).
Kotterman, M. A., Chalberg, T. W. & Schaffer, D. V. Annu. Rev. Biomed. Eng. 17, 63–89 (2015).
Huang, B. et al. Sci. Transl. Med. 7, 291ra94 (2015).
Hutchison, C. A. et al. Science 351, aad6253 (2016).
Noireaux, V. & Libchaber, A. Proc. Natl Acad. Sci. USA 101, 17669–17674 (2004).
Cameron, D. E., Bashor, C. J. & Collins, J. J. Nature Rev. Microbiol. 12, 381–390 (2014).
Levskaya, A. et al. Nature 438, 441–442 (2005).
Denby, C. M. et al. Nature Commun. 9, 965 (2018).

 Nature special: Bottom-up biology
Nature special: Bottom-up biology
 Focus on the benefits of building life’s systems from scratch
Focus on the benefits of building life’s systems from scratch
 How biologists are creating life-like cells from scratch
How biologists are creating life-like cells from scratch
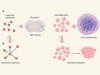 Cell parts to complex processes, from the bottom up
Cell parts to complex processes, from the bottom up
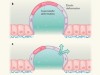 Cellular stretch reveals superelastic powers
Cellular stretch reveals superelastic powers
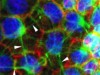 Active superelasticity in three-dimensional epithelia of controlled shape
Active superelasticity in three-dimensional epithelia of controlled shape
 Regulate ‘home-brew’ opiates
Regulate ‘home-brew’ opiates
 ‘Minimal’ cell raises stakes in race to harness synthetic life
‘Minimal’ cell raises stakes in race to harness synthetic life