- NEWS AND VIEWS
Weighing in on weight loss in pancreatic cancer
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 558, 526-528 (2018)
doi: https://doi.org/10.1038/d41586-018-05424-2
References
DiMagno, E. P. Ann. Oncol. 10 (Suppl. 4), S140–S142 (1999).
Danai, L. V. et al. Nature 558, 600–604 (2018).
Tisdale, M. J. Nature Rev. Cancer 2, 862–871 (2002).
Fearon, K., Arends, J. & Baracos, V. Nature Rev. Clin. Oncol. 10, 90–99 (2013).
Milton, K. J. Nutr. 133, 3886S–3892S (2003).
Vujasinovic, M., Valente, R., Del Chiaro, M., Permert, J. & Löhr, J. M. Nutrients 9, 183 (2017).
Murphy, R. A. et al. Lipids 47, 363–369 (2012).
Dev, R. et al. Oncologist 16, 1637–1641 (2011).
Abe, K. et al. Anticancer Res. 38, 2369–2375 (2018).
Mayers, J. R. et al. Nature Med. 20, 1193–1198 (2014).
Michaelis, K. A. et al. J. Cachexia Sarcopenia Muscle 8, 824–838 (2017).
Hingorani, S. R. et al. Cancer Cell 4, 437–450 (2003).
Di Sebastiano, K. M. et al. Br. J. Nutr. 109, 302–312 (2013).
Gupta, S. et al. Clin. Gastroenterol. Hepatol. 4, 1366–1372 (2006).
Kalyani, R. R., Corriere, M. & Ferrucci, L. Lancet Diabetes Endocrinol. 2, 819–829 (2014).
Hardt, P. D. et al. Pancreatology 3, 395–402 (2003).
Wagner, E. F. & Petruzzelli, M. Nature 521, 430–431 (2015).
Greco, S. H. et al. PLoS ONE 10, e0132786 (2015).
Löhr, J. M., Panic, N., Vujasinovic, M. & Verbeke, C. S. J. Intern. Med. 283, 446–460 (2018).
Competing Interests
J.M.L does consulting for Abbott/Mylan. The author also declares non-financial competing interests: he is a steering group member of pancreaticcancereurope.org

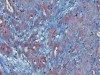 Read the paper: Altered exocrine function can drive adipose wasting in early pancreatic cancer
Read the paper: Altered exocrine function can drive adipose wasting in early pancreatic cancer
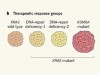 Pancreatic cancer foiled by a switch of tumour subtype
Pancreatic cancer foiled by a switch of tumour subtype
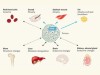 A waste of insulin interference
A waste of insulin interference