- NEWS AND VIEWS
Unexpected cell population gives fat a brake
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 559, 41-42 (2018)
doi: https://doi.org/10.1038/d41586-018-05120-1
References
Schwalie, P. C. et al. Nature 559, 103–108 (2018).
Sanchez-Gurmaches, J., Hung, C.-M. & Guertin, D. A. Trends Cell Biol. 26, 313–326 (2016).
Lynes, M. D. & Tseng, Y.-H. Ann. NY Acad. Sci. 1411, 5–20 (2018).
Schoettl, T., Fischer, I. P. & Ussar, S. J. Exp. Biol. 221, jeb162958 (2018).
Rosen, E. D. & Spiegelman, B. M. Cell 156, 20–44 (2014).
Hepler, C., Vishvanath, L. & Gupta, R. K. Genes Dev. 31, 127–140 (2017).
Berry, R., Jeffery, E. & Rodeheffer, M. S. Cell Metab. 19, 8–20 (2014).
Tang, W. et al. Science 322, 583–586 (2008).
Orkin, S. H. & Zon, L. I. Cell 132, 631–644 (2008).
Kusuma, G. D., Carthew, J., Lim, R. & Frith, J. E. Stem Cells Dev. 26, 617–631 (2017).

 Read the paper: A stromal cell population that inhibits adipogenesis in mammalian fat depots
Read the paper: A stromal cell population that inhibits adipogenesis in mammalian fat depots
 Dietary fat promotes intestinal dysregulation
Dietary fat promotes intestinal dysregulation
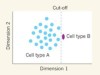 How to catch rare cell types
How to catch rare cell types