- NEWS AND VIEWS
Sabotage by the brain’s supporting cells helps fuel neurodegeneration
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 557, 499-500 (2018)
doi: https://doi.org/10.1038/d41586-018-04988-3
References
Peng, C. et al. Nature 557, 558–563 (2018).
Jucker, M. & Walker, L. C. Nature 501, 45–51 (2013).
Krismer, F. & Wenning, G. K. Nature Rev. Neurol. 13, 232–243 (2017).
Nussbaum, R. L. Cold Spring Harb. Perspect. Med. 7, a024109 (2017).
Hernandez, D. G., Reed, X. & Singleton, A. B. J. Neurochem. 139 (Suppl. 1), 59–74 (2016).
Peelaerts, W. et al. Nature 522, 340–344 (2015).
Walker, L. C. Annu. Rev. Genet. 50, 329–346 (2016).
Prusiner, S. B. et al. Proc. Natl Acad. Sci. USA 112, E5308–E5317 (2015).
Koga, S. & Dickson, D. W. J. Neurol. Neurosurg. Psychiatry 89, 175–184 (2018).
Woerman, A. L. et al. Cold Spring Harb. Perspect. Med. 7, a024588 (2017).
Brück, D., Wenning, G. K., Stefanova, N. & Fellner, L. Neurobiol. Dis. 85, 262–274 (2016).
Bengoa-Vergniory, N., Roberts, R. F., Wade-Martins, R. & Alegre-Abarrategui, J. Acta Neuropathol. 134, 819–838 (2017).

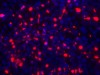 Read the paper: Cellular milieu imparts distinct pathological α-synuclein strains in α-synucleinopathies
Read the paper: Cellular milieu imparts distinct pathological α-synuclein strains in α-synucleinopathies
 Aggregates feel the strain
Aggregates feel the strain
 Disorder in the court
Disorder in the court