Abstract
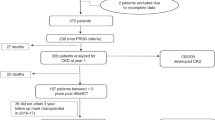
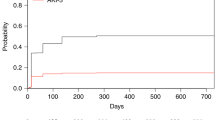
Acute kidney injury (AKI) following stem-cell transplantation (SCT) contributes to a poor prognosis, yet its impact may vary depending on the timing of AKI onset. A prospective cohort study was performed to understand the significance of the onset timing in 103 allogeneic SCT (allo-SCT) recipients. AKI prior to stem-cell engraftment was defined as early AKI and subsequently occurring AKI as late AKI. Propensity score (PS) for early AKI was calculated using a logistic regression model to reduce confounding effects related to differences in clinical background between the early and late AKI groups. The cumulative incidences of early and late AKI were 22.3% and 54.9%, respectively. Non-relapse mortality (NRM) was 39.1% and 7.0%, and overall survival (OS) was 56.5% and 90.9% in early and late AKI at 100 days after AKI, respectively (P<0.001). The cumulative incidence of chronic kidney disease (CKD) over 2 years after SCT was 41.5% and 19.1% in early and late AKI, respectively (P=0.048). Logistic regression analysis adjusted for the PS showed that early AKI was significantly associated with OS (odds ratio (95% confidence interval); 4.63 (1.15–21.4), P=0.031) but with neither NRM (1.25 (0.28–5.33), P=0.766) nor CKD (1.85 (0.41–8.60), P=0.422). In conclusion, early AKI may portend a poor survival for allo-SCT recipients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Parikh CR, Coca SG . Acute renal failure in hematopoietic cell transplantation. Kidney Int 2006; 69: 430–435.
Hingorani SR, Guthrie K, Batchelder A, Schoch G, Aboulhosn N, Manchion J et al. Acute renal failure after myeloablative hematopoietic cell transplant: incidence and risk factors. Kidney Int 2005; 67: 272–277.
Zager RA . Acute renal failure in the setting of bone marrow transplantation. Kidney Int 1994; 46: 1443–1458.
Kersting S, Koomans HA, Hene RJ, Verdonck LF . Acute renal failure after allogeneic myeloablative stem cell transplantation: retrospective analysis of incidence, risk factors and survival. Bone Marrow Transplant 2007; 39: 359–365.
Kersting S, Dorp SV, Theobald M, Verdonck LF . Acute renal failure after nonmyeloablative stem cell transplantation in adults. Biol Blood Marrow Transplant 2008; 14: 125–131.
Lopes JA, Goncalves S, Jorge S, Raimundo M, Resende L, Lourenco F et al. Contemporary analysis of the influence of acute kidney injury after reduced intensity conditioning haematopoietic cell transplantation on long-term survival. Bone Marrow Transplant 2008; 42: 619–626.
Schrier RW, Parikh CR . Comparison of renal injury in myeloablative autologous, myeloablative allogeneic and non-myeloablative allogeneic haematopoietic cell transplantation. Nephrol Dial Transplant 2005; 20: 678–683.
Morito T, Ando M, Kobayashi T, Kakihana K, Ohashi K, Akiyama H et al. New-onset microalbuminuria following allogeneic myeloablative SCT is a sign of near-term decrease in renal function. Bone Marrow Transplant 2013; 48: 972–976.
Sakellari I, Barbouti A, Bamichas G, Mallouri D, Kaloyannidis P, Fragidis S et al. GVHD-associated chronic kidney disease after allogeneic haematopoietic cell transplantation. Bone Marrow Transplant 2013; 48: 1329–1334.
Ellis MJ, Parikh CR, Inrig JK, Kanbay M, Patel UD . Chronic kidney disease after hematopoietic cell transplantation: a systematic review. Am J Transplant 2008; 8: 2378–2390.
Ando M, Ohashi K, Akiyama H, Sakamaki H, Morito T, Tsuchiya K et al. Chronic kidney disease in long-term survivors of myeloablative allogeneic haematopoietic cell transplantation: prevalence and risk factors. Nephrol Dial Transplant 2010; 25: 278–282.
Morito T, Ando M, Tsuchiya K, Nitta K . Early identification of acute kidney injury after hematopoietic stem cell transplantation by the measurement of urinary biomarkers. Nihon Jinzo Gakkai Shi 2011; 53: 1150–1158.
Imai H, Oyama Y, Miura AB, Endoh M, Sakai H . Hematopoietic cell transplantation-related nephropathy in Japan. Am J Kidney Dis 2000; 36: 474–480.
Igaki H, Karasawa K, Sakamaki H, Saito H, Nakagawa K, Ohtomo K et al. Renal dysfunction after total-body irradiation. Significance of selective renal shielding blocks. Strahlenther Onkol 2005; 181: 704–708.
Giralt S, Ballen K, Rizzo D, Bacigalupo A, Horowitz M, Pasquini M et al. Reduced intensity conditioning regimen workshop-Defining the dose spectrum. Biol Blood Marrow Transplant 2009; 15: 367–369.
Rogosheske JR, Fargen AD, DeFor TE, Warlick E, Arora M, Blazar BR et al. Higher therapeutic CsA levels early post transplantation reduce risk of acute GVHD and improves survival. Bone Marrow Transplant 2014; 49: 122–125.
Sorror ML, Maris MB, Storb R, Baron F, Sandmaier BM, Maloney DG et al. Hematopoietic cell transplantation (HCT)-specific comorbidity index: a new tool for risk assessment before allogeneic HCT. Blood 2005; 106: 2912–2919.
Kogon A, Hingorani S . Acute kidney injury in hematopoietic cell transplantation. Semin Nephrol 2010; 30: 615–626.
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG et al. Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 2007; 11: R31.
McGlave PB, Beatty P, Ash R, Hows JM . Therapy for chronic myelogenous leukemia with unrelated donor bone marrow transplantation: results in 102 cases. Blood 1990; 75: 1728–1732.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 2009; 53: 982–992.
Ruutu T, Barosi G, Benjamin RJ, Clark RE, George JN, Gratwohl A et al. Diagnostic criteria for hematopoietic stem cell transplant-associated microangiopathy: results of a consensus process by an International Working Group. Haematologica 2007; 92: 95–100.
Sato M, Nakasone H, Terasako-Saito K, Sakamoto K, Yamazaki R, Tanaka Y et al. Prediction of infectious complications by the combination of plasma procalcitonin level and localized infection before allogeneic hematopoietic cell transplantation. Bone Marrow Transplant 2014; 49: 553–560.
Kanda Y . Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant 2013; 48: 452–458.
Pulla B, Barri YM, Anaissie E . Acute renal failure following bone marrow transplantation. Ren Fail 1998; 20: 421–435.
Zager RA, O'Quigley J, Zager BK, Alpers CE, Shulman HM, Gamelin LM et al. Acute renal failure following bone marrow transplantation: a retrospective study of 272 patients. Am J Kidney Dis 1989; 13: 210–216.
Takatsuka H, Takemoto Y, Yamada S, Wada H, Tamura S, Fujimori Y et al. Complications after bone marrow transplantation are manifestations of systemic inflammatory response syndrome. Bone Marrow Transplant 2000; 26: 419–426.
Yap SC, Lee HT . Acute kidney injury and extrarenal organ dysfunction: new concepts and experimental evidence. Anesthesiology 2012; 116: 1139–1148.
Grams ME, Rabb H . The distant organ effects of acute kidney injury. Kidney Int 2012; 81: 942–948.
Shingai N, Morito T, Najima Y, Igarashi A, Kobayashi T, Doki N et al. Urinary liver-type fatty acid-binding protein linked with increased risk of acute kidney injury after allogeneic stem cell transplantation. Biol Blood Marrow Transplant 2014; 20: 2010–2014.
Shimoi T, Ando M, Munakata W, Kobayashi T, Kakihana K, Ohashi K et al. The significant impact of acute kidney injury on CKD in patients who survived over 10 years after myeloablative allogeneic SCT. Bone Marrow Transplant 2013; 48: 80–84.
Honda K, Ando M, Tsubokura M, Yamashita T, Akiyama H, Sakamaki H . An autopsy case that manifested no convincing histological changes of severe renal failure after hematopoietic stem cell transplantation. CEN Case Rep 2014; 3: 34–39.
Acknowledgements
We thank Makoto Saito, MSc, who helped with the statistical analysis.
Author contributions
MA designed the study and wrote the manuscript and was responsible for the study. NS and TM collected and analyzed the data and wrote the manuscript. YN, TK, ND, KK and KO contributed to the collection of raw data from SCT patients.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Shingai, N., Morito, T., Najima, Y. et al. Early-onset acute kidney injury is a poor prognostic sign for allogeneic SCT recipients. Bone Marrow Transplant 50, 1557–1562 (2015). https://doi.org/10.1038/bmt.2015.188
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2015.188
This article is cited by
-
Acute kidney injury within 100 days post allogeneic hematopoietic cell transplantation is associated with increased risk of post-transplant complications and poor transplant outcomes
Bone Marrow Transplantation (2022)
-
Acute kidney injury in cancer patients
Clinical and Experimental Nephrology (2022)
-
Risk factors for chronic kidney disease following acute kidney injury in pediatric allogeneic hematopoietic cell transplantation
Bone Marrow Transplantation (2021)
-
Mild renal dysfunction defined by creatinine clearance rate has limited impact on clinical outcomes after allogeneic hematopoietic stem cell transplantation
International Journal of Hematology (2018)
-
Acute kidney injury in HCT: an update
Bone Marrow Transplantation (2016)