Abstract
Increasing evidence suggests a complex relationship between obesity, diabetes and cancer. Here we review the evidence for the association between obesity and diabetes and a wide range of cancer types. In many cases the evidence for a positive association is strong, but for other cancer types a more complex picture emerges with some site-specific cancers associated with obesity but not to diabetes, and some associated with type I but not type II diabetes. The evidence therefore suggests the existence of cumulative common and differential mechanisms influencing the relationship between these diseases. Importantly, we highlight the influence of antidiabetics on cancer and antineoplastic agents on diabetes and in particular that antineoplastic targeting of insulin/IGF-1 signalling induces hyperglycaemia that often evolves to overt diabetes. Overall, a coincidence of diabetes and cancer worsens outcome and increases mortality. Future epidemiology should consider dose and time of exposure to both disease and treatment, and should classify cancers by their molecular signatures. Well-controlled studies on the development of diabetes upon cancer treatment are necessary and should identify the underlying mechanisms responsible for these reciprocal interactions. Given the global epidemic of diabetes, preventing both cancer occurrence in diabetics and the onset of diabetes in cancer patients will translate into a substantial socioeconomic benefit.
Similar content being viewed by others
Main
Diabetes is a chronic disease affecting 9% of the adult population worldwide, with a prevalence predicted to double in 2030 by the World Health Organisation (WHO). Diabetes is strongly associated with death from cardiovascular disease and cancer and represents an enormous social and economic health burden. Type I diabetes (TID) arises from immune destruction of pancreatic β-cells leading to insufficient insulin production, whereas 90% of type II diabetes (TIID) develops following peripheral insulin resistance associated to obesity in ageing people. Both TID and TIID are characterised by altered metabolic, hormonal and immune balances represented by abnormalities in carbohydrate and lipid metabolism, in incretins, pancreatic hormones and adipokine action, and increased circulating pro-inflammatory cytokines such as TNFα. Obesity and diabetes are epidemiologically linked to cancer and both common and independent risk factors may contribute to cancer development (Garcia-Jimenez et al, 2014).
Cancers share with diabetes hormonal imbalances, such as increased insulin and IGF-1 or leptin/adiponectin secretion, immune abnormalities including elevated circulating pro-inflammatory cytokines and metabolic alterations. Cancer cells maximise the capture/use of glucose to sustain a high proliferation/apoptosis ratio and bypass senescence (Coller, 2014). Increased nutrient demand and altered metabolic by-products of cancer cells alter their environment, inducing metabolic and secretory adaptations in neighbouring noncancer cells such as fibroblasts, adipocytes and macrophages (Coller, 2014), affecting the whole organism. Ultimately, these changes compromise the function of adipose, liver and muscle tissues, leading to cachexia, a metabolic syndrome featuring typical diabetic features and responsible for 20% of cancer deaths (Argiles et al, 2014).
Substantial epidemiological evidence supports an association between diabetes and increased site-specific cancer risk (Shikata et al, 2013; Tsilidis et al, 2015). However, the burden of confounding factors that potentially bias interpretation blurs the strength of such associations. Metabolic, hormonal and immune links between diabetes and cancers represent potential cause–consequence relationships whose importance needs to be clarified separately with well-controlled in vitro and in vivo studies. Here we review the current epidemiological links with an emphasis on the influence of antidiabetic and antineoplastic therapies. We identify exposure time and dose and treatments among the most important factors to be considered in future studies.
Epidemiological links: hierarchy of site-specific cancers associated to diabetes and obesity
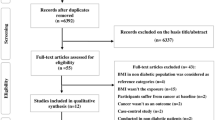
A meta-analysis (Supplementary Figure S1) was undertaken to examine the association between diabetes, obesity and cancer. The results indicate that the interplay between hyperglycaemia, increase in adipose mass and inflammation that appears with obesity is critical in both diabetes and cancer, suggesting that obesity may link diabetes and cancer. Epidemiological data positively associate obesity with many site-specific cancers (more strongly for endometrium and kidney and weaker for bladder, prostate and stomach cancers; Supplementary Table S1). Importantly, lung cancers that are highly prevalent are inversely associated with obesity.
Type II diabetes associates with most cancers linked to obesity (Supplementary Table S1) (Habib and Rojna, 2013; Shikata et al, 2013; Tsilidis et al, 2015). Note that TIID represents >90% of diagnosed diabetes, and consistently studies that do not distinguish TID from TIID (TI/IID) follow a pattern similar to TIID. Figure 1 summarises the epidemiological associations between obesity, TID, TIID or TI/IID and site-specific cancers using the rationale of a heat map. Importantly, most site-specific cancers positively associated to obesity present an even stronger association with TIID, suggesting that for those cancers TIID brings additional contributing factors. Interestingly, prostate cancer associates positively with obesity and inversely to TIID, whereas lung cancers inversely associate with obesity but not with TIID. Thus, it seems likely that factors associated with obesity and diabetes contribute differentially to site-specific cancers. Although body mass index (BMI) adjustments have been introduced in recent studies, in individual studies BMI correction does not alter the epidemiological association of diabetes with gastrointestinal cancer. However, BMI adjustment does decrease the association of diabetes with breast cancer (Shikata et al, 2013).
Association of cancers (classified by site) with obesity, diabetes and treatments. Raw data for this figure are presented in Supplementary Tables S1 and S2. Cancer relative risk was directly – red colours – or inversely (protection) – green colours – associated with obesity (Ob), TIID, TID or ADTs: insulin (Ins) and sulphonylurea (SU) that increase circulating insulin and metformin (Met) and TZDs that decrease blood glucose. Not statistically significant (NS) association (blue squares). Squares with very light red or green shadow represent trends to direct (red shadow) or inverse (green shadow) association, although statistically not significant mainly because of lack of sufficient studies.
Type I diabetes is also associated to site-specific cancers. Its association to endometrial and stomach cancer is stronger than TIID association (Supplementary Table S1). The association with TID or TIID was of a similar magnitude for cancers of the pancreas, thyroid, leukaemia and NHL. For most cancer sites, data for TID is scarce and populations smaller, resulting in big confidence intervals that make the significance dubious. Bearing this in mind we can still compare their tendencies by looking at the relative risks. In doing so, two subsets with opposite association to TID appear: gastrointestinal, some blood cancers, thyroid and bladder cancers appear positively associated, whereas melanoma, kidney, prostate and ovarian cancers are inversely associated (Figure 1). In addition, breast cancers do not associate with TID. Strikingly, there are more site-specific cancers inversely associated with TID than to TIID or obesity, highlighting the importance of protective factors associated with TID. What is different about melanomas, ovarian and kidney cancer from the other site-specific cancer types that reverses their association with TID and TIID is unknown.
Hyperglycaemia may also favour cancer development by diverse mechanisms, as reviewed elsewhere (Garcia-Jimenez et al, 2014), and we also explored its contribution through epidemiological data (not shown). Several prospective studies reported an elevated risk ratio for all-site cancer incidence in men – excluding prostate cancer – and women with each increase in 1 mmol l−1 of fasting plasma glucose levels (Stocks et al, 2009). Dietary hyperglycaemia, estimated by glycaemic index or load, positively associates with increased incidence of endometrial, gastric and colorectal cancers (CRC) and with colorectal cancer mortality (Hu et al, 2013). However, the time of exposure to hyperglycaemia might be critical for increased cancer risk, and therefore glycated haemoglobin (HbA1c) values that estimate the glycaemia for the past 2 months might be more informative than punctual glycaemic measurements. Remarkably, few diabetes–cancer studies collected HbA1c values and those that included them had confidence intervals too large to draw conclusions. Importantly, enhanced glucose uptake by cancer cells leads hepatic adaptation to increase circulating glucose, and consequently diabetes could be an early manifestation of a tumour. In contrast, in advanced cancers highly proliferative cells with enhanced glucose uptake may deplete blood glucose. In addition, cancer-associated anaemia and frequent blood transfusions will alter HbA1c values, possibly explaining the amplitude of the confidence intervals found in epidemiological studies. Understanding the changes in blood glucose and HbA1c during cancer evolution might help develop better treatments.
Thus, a generalised approach to study associations between global cancer risk and diabetes or obesity may be flawed as there are highly prevalent cancers not associated (lung), or inversely associated (prostate), with diabetes. Importantly, the coexistence of diabetes with cancer increases mortality even in cancers like prostate that are inversely associated (Habib and Rojna, 2013). Given that some antineoplastic treatments (i.e., glucocorticoids) may induce diabetes (see below), and that some antidiabetic treatments (ADTs) have been linked to cancer, the contribution of treatments should be explored in depth.
ADTs and cancer
The increasing incidence of diabetes has led to an ever-growing diversity of ADTs that are mainly directed to increase insulin levels or to reduce circulating glucose. Circulating insulin increases after administration of analogues (Lispro, Actrapid, glargine and so on), secretagogues (sulphonylureas, glinides) or incretin mimetics/enhancers. Alternatively, circulating glucose is reduced by insulin sensitisers (metformin, glitazones). Yet, other treatments slow down digestion of complex carbohydrates or reduce absorption like α-glucosidase inhibitors and bariatric surgery respectively.
Glucose metabolism and insulin signalling deregulation are shared by diabetes and cancers, and ADTs targeting them could influence cancer risk and mortality. For example, excess insulin induces cell proliferation in culture and tumour growth in animal models (Pollak and Russell-Jones, 2010), whereas epidemiological association of high insulin levels with increased cancer risk contrasts with metformin association to decreased cancer risk (Wu et al, 2015). These epidemiological associations prompted the hypothesis that ADTs that increase circulating insulin may increase diabetes-associated cancer risk, progression or mortality, whereas ADTs that improve insulin sensitivity (metformin and glitazones) may decrease cancer risk. Consistent with this hypothesis, treatment with insulin analogues like glargine were initially associated with increased frequency or mortality of various cancers. However, later studies either confirmed or not the association, opening a controversy that led to the introduction of an increasing number of correction factors (Singh et al, 2013; Lutz et al, 2014). Nevertheless, exposure to ADT (type, time and doses) should be among the most important factors included in studies on diabetes–cancer associations, and studies that aim to elucidate the mechanisms that may connect each ADT with cancers need strong support.
We next assessed (Supplementary Figure S2A) the relationship between ADTs and site-specific cancers in studies that compared insulin with non-insulin treatment, metformin with non-metformin, and so on.
Insulin excess and cancer risk
Hyperinsulinaemia may arise as a result of exogenous insulin administration in TID and endogenous insulin release at early stages of TIID to compensate for peripheral insulin resistance that develops after frequent exposure to high circulating levels of glucose and lipids in obesity. Insulin binding to its own tyrosine kinase receptor (IR) activates the PI3K/Akt/mTOR and MAPK/ERK pathways to induce metabolic, anti-apoptotic and proliferative changes. Insulin also binds (with lower affinity) the highly related receptor IGF-1R that signals towards proliferation through MAPK/ERK. Insulin signalling differs in healthy and diabetic patients (Groop et al, 2005; Noto et al, 2013), with insulin resistance being characterised by an altered metabolic branch that leaves mitogenic signalling unaffected (Pollak and Russell-Jones, 2010). Thus, excess insulin binding to IRs and IGF-1R in diabetes may lead to proliferative and anti-apoptotic effects mediated by PI3K-Akt/mTOR and Ras-MAPK signalling pathways that are frequently activated in human cancers (Ekstrand et al, 2010). Cancer cells also frequently overexpress IGF-1R and the uncommon form of insulin receptor IR-A that signal predominantly via MAPK to promote proliferation.
Consistently, increased pancreatic (Baur et al, 2011) and breast (Rendell et al, 2013) cancer risk in TIID patients treated with insulin was reported in retrospective epidemiological pooled studies. However, although the heterogeneity of these studies was criticised, the presence of some confounders is not proof of safety. Results from randomised clinical trials (RCTs) designed to analyse retinopathy, the DIGAMY study (Malmberg, 1997), confirmed the association, whereas the ORIGIN study (Origin Trial Investigators et al, 2008), designed for cardiovascular disease, did not confirm an association of insulin with global cancer risk. Important limitations of these studies are the lack of distinction by site-specific cancers, short follow-up time to evaluate cancer development (4–6 years) and missing confounding factors as the studies were designed to evaluate other outcomes.
Pooled data (Supplementary Table S2) comparing insulin and non-insulin treatments are summarised in Figure 1 and points to increased risk of gastrointestinal (pancreas, liver, colorectal and stomach), kidney and lung cancers. Importantly, insulin was inversely associated with prostate cancer risk (which is less frequent in diabetic patients, Supplementary Table S1), suggesting that insulin treatment may provide protection. However, insulin treatment is not protective in melanoma and kidney cancers that are also inversely associated to TID, suggesting that insulin effects are site specific. Whether insulin influences the capacity of prostate cells to adopt a tumourigenic phenotype while endangering others needs to be investigated.
Therapies directed towards enhancing insulin secretion, for example, targeting potassium channels with sulphonylureas (SUs), were associated with increased global cancer risk when compared with metformin (Ruiter et al, 2012) in cohorts; case–control studies are rare and only one shows increased global cancer risk within the limits of statistical significance (Chang et al, 2012). However, as mentioned above, analysis of global cancer risk is inappropriate given the differential effects on different cancer types. Multivariate analysis suggests an increased liver-specific cancer risk associated with SUs (Hassan et al, 2010), and subsequent studies confirmed the liver cancer association with first- and second-generation SUs but not with third generation SUs that are weaker enhancers of insulin secretion (Chang et al, 2012; Thakkar et al, 2013).
Treatment of SUs (Supplementary Table S2) is not associated with increased risk of any site-specific cancer in available studies but associates with decreased lung cancer risk, suggesting that SUs may provide protection. Exogenous insulin increased site-specific cancer risk (pancreas, liver, colorectal and lung), whereas endogenously produced insulin after SU treatment either did not increase or even reduced lung cancer risk. The data suggest that insulin excess may be associated to cancer (perhaps through unspecific effects) but more physiological doses, as reached by using secretagogues, are not. Alternatively, the subcutaneous delivery of exogenous insulin may explain differences.
Enhanced insulin secretion through incretin-based therapies (incretin analogues: exenatide or liraglutide, or inhibitors of dipeptidyl peptidase-4 such as sitagliptin, vidagliptin) has also been linked to certain cancers. Exenatide and sitagliptin have been directly associated with pancreatic cancer and sitagliptin with thyroid cancer (Nauck and Meier, 2013). Consistently, studies in rodents suggested an association of incretin-based therapies with thyroid (C cell) and pancreatic cancers (Lutz et al, 2014).
Insulin sensitisers: metformin and thiazoledinediones
Metformin, which at the cellular level targets AMPK and mitochondrial metabolism, reduces the levels of circulating glucose, improving insulin sensitivity and inducing weight loss. Treatment with metformin has been associated in meta-analysis of case–control and cohorts (Supplementary Table S2) with reduced breast, colon and pancreas cancer risk (Figure 1), although RCTs confirmed the inverse association or showed no impact of metformin (Thakkar et al, 2013). Metformin is the treatment of choice when diabetes is less severe and of shorter duration, factors that may condition cancer risk and may explain lack of metformin effects when corrected. In addition, it should be remembered that RCTs that find no association between metformin and cancer were designed to analyse other outcomes, did not include adequate confounding factors and follow-up was too short (maximum 4 years) (Lutz et al, 2014). Despite this evidence the latest meta-analysis shows that metformin decreased risk only for cancers of the liver, pancreas, CRC and stomach (Supplementary Table S2 and Figure 1).
Thiazolidinediones (TZDs), Rosiglitazone, Pioglitazone and Efatutazone, bind the nuclear receptor PPARγ to modify gene expression, reducing liver gluconeogenesis or fat accumulation and increasing insulin sensitivity and glucose uptake by the muscle. The action of TZDs might also be mediated by mechanisms independent of PPARs and affect differently each site-specific cancer. Rosiglitazone was forbidden in Europe and restricted in the United States because of its association with cardiovascular events, and results from epidemiological studies were conflicting. Pioglitazone was dose-dependently associated to increased bladder cancer and with diminished hepatic cancers in retrospective studies (Bosetti et al, 2013) and RCTs (the PROactive study, directed to evaluate cardiovascular outcomes). Meta-analysis of TZD treatment reveals an inverse association with liver and lung cancers (as for metformin), Supplementary Table S2. Any effect of rosiglitazone and efatutazone on the risk of site-specific cancers remains to be confirmed, and the mechanism involved elucidated to exclude that lack of association is because of premature death through cardiovascular events.
Other ADTs
Acarbose or miglitol, which interfere with glucose absorption, correlated with increased kidney and decreased lung, gastric and hepatic cancers in preliminary studies that included small numbers of patients and need confirmation including correction for confounding factors related to hyperglycaemia (HbA1c) (Lutz et al, 2014). Inhibitors of renal reabsorption have not been prescribed for long enough to have sufficient epidemiological data to evaluate their impact on diabetes-associated cancers. The mechanisms that link these treatments with cancers remain unexplored. Bariatric surgery that is successfully used to induce weight loss and diabetes remission may also affect cancer but it is not clear how. A Swedish retrospective study (Sjostrom et al, 2009) with 18 years of follow-up showed a reduction (by almost half) in CRC incidence in obese women (but not in men) after bariatric surgery. This result was confirmed by a US study (Adams et al, 2009). However, increases in mitosis and pro-tumourigenic markers were noticed in colorectal epithelium 3 years post bariatric surgery. Consistently, a later Swedish report showed increased colorectal cancer incidence (but not other neoplasias) associated with bariatric surgery, highlighting the weakness of epidemiological associations (Goh and Goh, 2013). Future studies must clarify this point.
Available studies indicate that prostate cancer is inversely associated with insulin treatment and shows a trend for inverse association (although not statistically significant) with diabetes, especially TID. In contrast, kidney cancer is directly associated to both diabetes and insulin treatment. This may suggest that the association of cancers with insulin and diabetes is linked. For example, protection from prostate cancers in diabetic populations could be attributed to insulin treatments. However, we found some cancer sites associated to diabetes but not to insulin (e.g., melanoma). In contrast, lung cancer risk was increased by insulin, although it is less frequent in obese people (most likely with hyperinsulinaemia) and was unrelated to diabetes. These results highlight the need to understand the mechanisms of insulin association with incidence of site-specific cancers. More studies on the association of TID to specific cancers are needed. Importantly, decreased lung cancer risk was associated to SUs, also suggesting that exogenous and endogenous insulin influences on lung cancer are not equivalent. Note that lung and prostate cancers exhibit opposite associations with obesity and insulin treatment and perhaps also differ in their association to diabetes and other treatments, although the underlying mechanisms remain unknown. Remarkably, gynaecological, bladder cancers and melanoma were not associated with ADTs, despite being strongly associated with obesity and/or diabetes.
Metformin – suggested to play a protective role – appears inversely associated only to gastrointestinal cancers, although more studies are needed for lung, kidney and thyroid cancers.
Comparing metformin and insulin association with cancer sites classifies them into three groups (Figure 1): (1) those not associated to any (e.g., gynaecological cancers), (2) those associated with insulin only (e.g., lung cancer) and (3) those associated with both, in which case they always associate directly with insulin and inversely with metformin (e.g., gastrointestinal cancers).
Antineoplastic therapies and diabetes
Cancer therapies (including radiation, biological agents and chemicals) target the immune system (i.e., glucocorticoids), endocrine signals that enhance cancer growth (androgens or oestrogens), or tumour cell biology including replicative immortality (e.g., pyrimidine analogues), apoptosis (e.g., cisplatin), signalling (antibodies against receptor tyrosine kinases) and metabolism (e.g., mTOR inhibitors). Some anticancer therapies may lead to acquired diabetes (transient or permanent) and the coexistence of diabetes and cancer increases mortality (Vigneri et al, 2009).
Most data on diabetes onset during cancer therapy come from studies intended to analyse the efficiency and side effects of therapies with a general lack of systematisation that hampers comparisons. First, glycaemia is estimated as: (1) blood glucose (mg dl−1 or mM), (2) HbA1c, (3) hyperglycaemia, grades 1–4, (4) expressed as high vs not high and/or (5) as relative risk of diabetes (or hyperglycaemia) among the treated population. Second, the drug to be compared is often in combination with other non-neutral drugs (e.g., mTOR inhibitors and glucocorticoids) and comparators vary from the same combination with placebo to alternative treatments. Third, the few studies that exist examine all cancers or diverse combinations of unrelated cancers (e.g., lymphoma and brain) or site-specific cancers (per se associated or not to diabetes). Fourth, during the course of cancer, deregulated haematopoiesis or frequent blood transfusions may alter haemoglobin synthesis and translate to misleading HbA1c values. In addition, tumours themselves dynamically modify their environment to increase circulating glucose that favours their growth, whereas in advanced stages tumours may deplete glucose from the blood. We have made an effort to normalise the available data (Supplementary Table S3) to assign hyperglycaemia grades that could be compared; the relative risk (RR) has been calculated from studies that included a control population.
Two major therapies targeting cancer growth or survival have been associated with development of hyperglycaemia grades 3–4 (>250 mg dl−1): mTOR inhibitors (Everolimus and Temsirolimus) and tyrosine kinase inhibitors (Nilotinib, Pazopanib). Hyperglycaemia induction by mTOR inhibitors has been recently reviewed (Verges and Cariou, 2015), reporting that Everolimus led to hyperglycaemia grades 3–4 in 12% of renal cell carcinoma patients, in 5% pancreatic or gastrointestinal cancers and 4% of breast cancer patients; similar percentages were obtained for Temsirolimus in renal cell carcinoma. For receptor tyrosine kinase inhibitors such as Nilotinib, hyperglycaemia grades 3–4 was reported in 5% of treated patients with chronic myeloid leukaemia; hyperglycaemia was not found in smaller treated populations with gastrointestinal or pancreatic cancers (Verges et al, 2014). Data suggest that Nilotinib-induced glycaemic changes are mild and transient (Ito et al, 2013). Inhibitors targeting PI3K/AKT signalling also induced hyperglycaemia. Up to 8.4% of patients treated with BKM120 developed grade 3–4 hyperglycaemia. Remarkably, targeting directly IR or IGF-1R resulted in higher percentage of patients developing hyperglycaemia. In a recent study by Geuna et al (2015), patients treated with PI3K/AKT/mTOR pathway (PAM) inhibitors (18 phase I clinical trials) were compared with control patients with non-PAM-directed treatments (10 phase I clinical trials). In both PAM- and not-PAM-treated groups, ∼80% of patients developed all-grade hyperglycaemia but grade 3–4 hyperglycaemia appeared only in the PAM-treated group (6.7% vs 0% of controls) (Geuna et al, 2015).
High-dose glucocorticoids, often used as adjuvants in cancer, are the most frequent pharmacological cause of hyperglycaemia and insulin resistance (Feng et al, 2013). The likelihood of developing hyperglycaemia has been dose-dependently correlated with dexamethasone treatment (Pilkey et al, 2012). In a cohort of 90 patients with lymphoma or brain tumours treated with prednisone (in a regime also containing doxorubicin–cyclophosphamide–vincristine±rituximab), 58.9% developed hyperglycaemia and 13.3% diabetes (Harris et al, 2013) (Supplementary Table S3). In another cohort of 80 lymphoma patients treated with high doses of prednisone (in a regime with cyclophosphamide–hydroxydaunorubicin–oncovin), 32.5% patients developed diabetes mellitus (Lee et al, 2014).
Androgen deprivation therapy is used against prostate cancer. However, testosterone deficiency correlates with central adiposity, increased circulating free fatty acids and subsequent insulin resistance (Saglam et al, 2012). However, only 12.5% of patients under androgen deprivation therapy developed insulin resistance and hyperglycaemia in two cohorts (Hara, 2012); the relative risk was 1.37 higher for men treated with androgen deprivation therapy vs other therapies (Verges et al, 2014). As the frequency of prostate cancer is smaller in diabetic men, development of hyperglycaemia upon androgen deprivation might be more significant than it appears.
Pyrimidine analogues, such as 5-Fluorouracil that inhibits RNA synthesis and induces DNA damage and apoptosis, are used to treat colorectal and pancreatic cancers (Ma et al, 2014). 5-Fluorouracil treatment induced hyperglycaemia in 26.1% of CRC patients and 13.2% developed diabetes (Feng et al, 2013).
Cisplatin, a heavy metal coordination compound that induces apoptosis of cancer cells, is widely used in a variety of cancers. Cisplatin treatment induced transient diabetes in 5% patients in two cohorts of head and neck cancer patients (Nan et al, 2003; Nguyen et al, 2009). Whether higher doses or extended treatment with cisplatin induces permanent diabetes and the role of co-administered glucocorticoids in this or other cancer sites remain to be elucidated.
Radiotherapy was associated with diabetes according to evidence from one study that found a 1.8-fold higher prevalence of diabetes mellitus in childhood cancer survivors treated with radiotherapy compared with their siblings (Meacham et al, 2009). However, the molecular mechanisms that support this outcome remain obscure.
Conclusion
Epidemiological data suggest that diabetes and specific ADTs increase the risk of some cancers and certain antineoplastics increase the risk of diabetes development. As the coexistence of diabetes and cancer always worsens the prognosis, glycaemic control during cancer treatment may considerably improve the outcome. The evolution of glycaemia should be evaluated and inaccuracies avoided using comparable units. The data available suggest the existence of multiple positive and negative links between obesity, diabetes and cancer, but the contribution of each individual mechanism or link may vary for each site-specific cancer.
Epidemiology establishes statistical correlations, but the lack of mechanistic studies that elucidate cause–consequence relationships may lead to inappropriate correction and inconsistent findings. Divergent epidemiological outcomes may be attributed to correction with different factors or different definitions for the same factor. Examples of non-equivalent definitions are: using dietary glycaemic index or glycaemic load, mmol l−1 glucose or HbA1c to define hyperglycaemia; using BMI >30 kg m−2, waist circumference or waist-to-hip ratio to define obesity. Antidiabetic treatments have been important sources of inconsistency because of: (1) non-random assignment of therapy, (2) usage of different comparators and (3) exposure (doses and time). First, therapy assignment depends on duration and severity of diabetes, with metformin representing first-line treatment whereas insulins are given to older and sicker patients. Thus, metformin–insulin comparisons should be adjusted for diabetes duration. Second, if the comparator is not neutral, interpretation must be biased; sulphonylureas compared with metformin or insulins will give different results. Doses and time of exposure to both disease and treatment should be considered in epidemiological studies and time bias is the most important confounder in TIID.
As hyperinsulinaemia and hyperglycaemia represent strong mechanistic links between obesity, diabetes and cancer, we compared the links between cancer and treatments that increase insulin or those reducing glycaemia: insulin and metformin. Data suggest the contribution of different combinations of mechanisms (from the disease and/or from treatments) for each site-specific cancer. More site-specific cancers were associated to insulin than to metformin; cancers directly associated to insulin were inversely associated to metformin or not related; importantly, inducers of insulin secretion (e.g., SUs) did not follow the insulin association pattern, suggesting different effects for exogenous or endogenous insulin. We noticed the scarcity of data on sulphonylureas and glitazones.
Molecular signatures of cancers help improve cancer treatment. Given the importance of treatments in the diabetes–cancer link, classification of cancers associated with diabetes by their molecular signatures instead of by site may shed more light.
Future research directions
-
Mechanistic studies that explore the molecular bases that support increased cancer risk for diabetic patients, induction of diabetes by specific antineoplastic treatments and the effects of antidiabetics on cancer cells are needed. Knowledge of mechanisms will help refine future epidemiological studies and selection of the most appropriate treatments.
-
The association of diabetes, obesity and hyperglycaemia to site-specific cancers, classified by their molecular signatures, still remains to be explored more conclusively. Studies for TID association to site-specific cancers are also needed.
-
The influence of antidiabetics on cancer should be explored in studies that are randomised and well controlled, with long-term follow-up, independent from pharmaceutical industry funding. We propose correction using values of glycaemia (registered as HbA1c) and obesity (BMI and waist circumference) that account for several metabolic, endocrine and inflammatory confounders and may simplify corrections. Correction with duration of diabetes, type and exposure to treatment should also be included. In addition, we remark that data are scarce for SUs and glitazones.
-
Studies that explore the induction of diabetes by specific antineoplastic treatments are also needed. Knowing the time and dose required, the transient or permanent nature of the associated diabetes and the specificity of the cancer site or hallmark may help improve the outcome of present therapies.
References
Adams TD, Stroup AM, Gress RE, Adams KF, Calle EE, Smith SC, Halverson RC, Simper SC, Hopkins PN, Hunt SC (2009) Cancer incidence and mortality after gastric bypass surgery. Obesity (Silver Spring) 17 (4): 796–802.
Argiles JM, Busquets S, Stemmler B, Lopez-Soriano FJ (2014) Cancer cachexia: understanding the molecular basis. Nat Rev Cancer 14 (11): 754–762.
Baur DM, Klotsche J, Hamnvik OP, Sievers C, Pieper L, Wittchen HU, Stalla GK, Schmid RM, Kales SN, Mantzoros CS (2011) Type 2 diabetes mellitus and medications for type 2 diabetes mellitus are associated with risk for and mortality from cancer in a German primary care cohort. Metabolism 60 (10): 1363–1371.
Bosetti C, Rosato V, Buniato D, Zambon A, La Vecchia C, Corrao G (2013) Cancer risk for patients using thiazolidinediones for type 2 diabetes: a meta-analysis. Oncologist 18 (2): 148–156.
Chang CH, Lin JW, Wu LC, Lai MS, Chuang LM (2012) Oral insulin secretagogues, insulin, and cancer risk in type 2 diabetes mellitus. J Clin Endocrinol Metab 97 (7): E1170–E1175.
Coller HA (2014) Is cancer a metabolic disease? Am J Pathol 184 (1): 4–17.
Ekstrand AI, Jonsson M, Lindblom A, Borg A, Nilbert M (2010) Frequent alterations of the PI3K/AKT/mTOR pathways in hereditary nonpolyposis colorectal cancer. Fam Cancer 9 (2): 125–129.
Feng JP, Yuan XL, Li M, Fang J, Xie T, Zhou Y, Zhu YM, Luo M, Lin M, Ye DW (2013) Secondary diabetes associated with 5-fluorouracil-based chemotherapy regimens in non-diabetic patients with colorectal cancer: results from a single-centre cohort study. Colorectal Dis 15 (1): 27–33.
Garcia-Jimenez C, Garcia-Martinez JM, Chocarro-Calvo A, De la Vieja A (2014) A new link between diabetes and cancer: enhanced WNT/beta-catenin signaling by high glucose. J Mol Endocrinol 52 (1): R51–R66.
Geuna E, Roda D, Rafii S, Jimenez B, Capelan M, Rihawi K, Montemurro F, Yap TA, Kaye SB, De Bono JS, Molife LR, Banerji U (2015) Complications of hyperglycaemia with PI3K-AKT-mTOR inhibitors in patients with advanced solid tumours on Phase I clinical trials. Br J Cancer 113 (11): 1541–1547.
Goh LY, Goh KL (2013) Obesity: an epidemiological perspective from Asia and its relationship to gastrointestinal and liver cancers. J Gastroenterol Hepatol 28 (Suppl 4): 54–58.
Groop PH, Forsblom C, Thomas MC (2005) Mechanisms of disease: pathway-selective insulin resistance and microvascular complications of diabetes. Nat Clin Pract Endocrinol Metab 1 (2): 100–110.
Habib SL, Rojna M (2013) Diabetes and risk of cancer. ISRN Oncol 2013: 583786.
Hara N (2012) Prostate carcinogenesis with diabetes and androgen-deprivation-therapy-related diabetes: an update. Exp Diabetes Res 2012: 801610.
Harris D, Barts A, Connors J, Dahl M, Elliott T, Kong J, Keane T, Thompson D, Stafford S, Ur E, Sirrs S (2013) Glucocorticoid-induced hyperglycemia is prevalent and unpredictable for patients undergoing cancer therapy: an observational cohort study. Curr Oncol 20 (6): e532–e538.
Hassan MM, Curley SA, Li D, Kaseb A, Davila M, Abdalla EK, Javle M, Moghazy DM, Lozano RD, Abbruzzese JL, Vauthey JN (2010) Association of diabetes duration and diabetes treatment with the risk of hepatocellular carcinoma. Cancer 116 (8): 1938–1946.
Hu J, La Vecchia C, Augustin LS, Negri E, de Groh M, Morrison H, Mery L Canadian Cancer Registries Epidemiology Research Group (2013) Glycemic index, glycemic load and cancer risk. Ann Oncol 24 (1): 245–251.
Ito Y, Miyamoto T, Chong Y, Maki T, Akashi K, Kamimura T (2013) Nilotinib exacerbates diabetes mellitus by decreasing secretion of endogenous insulin. Int J Hematol 97 (1): 135–138.
Lee SY, Kurita N, Yokoyama Y, Seki M, Hasegawa Y, Okoshi Y, Chiba S (2014) Glucocorticoid-induced diabetes mellitus in patients with lymphoma treated with CHOP chemotherapy. Support Care Cancer 22 (5): 1385–1390.
Lutz SZ, Staiger H, Fritsche A, Haring HU (2014) Antihyperglycaemic therapies and cancer risk. Diab Vasc Dis Res 11 (6): 371–389.
Ma YS, Yang IP, Tsai HL, Huang CW, Juo SH, Wang JY (2014) High glucose modulates antiproliferative effect and cytotoxicity of 5-fluorouracil in human colon cancer cells. DNA Cell Biol 33 (2): 64–72.
Malmberg K (1997) Prospective randomised study of intensive insulin treatment on long term survival after acute myocardial infarction in patients with diabetes mellitus. DIGAMI (Diabetes Mellitus, Insulin Glucose Infusion in Acute Myocardial Infarction) Study Group. BMJ 314 (7093): 1512–1515.
Meacham LR, Sklar CA, Li S, Liu Q, Gimpel N, Yasui Y, Whitton JA, Stovall M, Robison LL, Oeffinger KC (2009) Diabetes mellitus in long-term survivors of childhood cancer. Increased risk associated with radiation therapy: a report for the childhood cancer survivor study. Arch Intern Med 169 (15): 1381–1388.
Nan DN, Fernandez-Ayala M, Vega Villegas ME, Garcia-Castano A, Rivera F, Lopez-Brea M, Gonzalez-Macias J (2003) Diabetes mellitus following cisplatin treatment. Acta Oncol (Madr) 42 (1): 75–78.
Nauck MA, Meier JJ (2013) Author reply: To PMID 23208166. Ann Intern Med 158 (6): 501–502.
Nguyen NP, Vos P, Vinh-Hung V, Borok TL, Dutta S, Karlsson U, Lee H, Martinez T, Jo BH, Nguyen LM, Nguyen N, Sallah S (2009) Altered glucose metabolism during chemoradiation for head and neck cancer. Anticancer Res 29 (11): 4683–4687.
Noto H, Goto A, Tsujimoto T, Osame K, Noda M (2013) Latest insights into the risk of cancer in diabetes. J Diabetes Investig 4 (3): 225–232.
Origin Trial Investigators, Gerstein H, Yusuf S, Riddle MC, Ryden L, Bosch J (2008) Rationale, design, and baseline characteristics for a large international trial of cardiovascular disease prevention in people with dysglycemia: the ORIGIN Trial (Outcome Reduction with an Initial Glargine Intervention). Am Heart J 155 (1): 26–32, 32.e1-6.
Pilkey J, Streeter L, Beel A, Hiebert T, Li X (2012) Corticosteroid-induced diabetes in palliative care. J Palliat Med 15 (6): 681–689.
Pollak M, Russell-Jones D (2010) Insulin analogues and cancer risk: cause for concern or cause celebre? Int J Clin Pract 64 (5): 628–636.
Rendell M, Akturk HK, Tella SH (2013) Glargine safety, diabetes and cancer. Expert Opin Drug Saf 12 (2): 247–263.
Ruiter R, Visser LE, van Herk-Sukel MP, Coebergh JW, Haak HR, Geelhoed-Duijvestijn PH, Straus SM, Herings RM, Stricker BH (2012) Lower risk of cancer in patients on metformin in comparison with those on sulfonylurea derivatives: results from a large population-based follow-up study. Diabetes Care 35 (1): 119–124.
Saglam HS, Kose O, Kumsar S, Budak S, Adsan O (2012) Fasting blood glucose and lipid profile alterations following twelve-month androgen deprivation therapy in men with prostate cancer. ScientificWorldJournal 2012: 696329.
Shikata K, Ninomiya T, Kiyohara Y (2013) Diabetes mellitus and cancer risk: review of the epidemiological evidence. Cancer Sci 104 (1): 9–14.
Singh S, Singh PP, Singh AG, Murad MH, McWilliams RR, Chari ST (2013) Anti-diabetic medications and risk of pancreatic cancer in patients with diabetes mellitus: a systematic review and meta-analysis. Am J Gastroenterol 108 (4): 510–519, quiz 520.
Sjostrom L, Gummesson A, Sjostrom CD, Narbro K, Peltonen M, Wedel H, Bengtsson C, Bouchard C, Carlsson B, Dahlgren S, Jacobson P, Karason K, Karlsson J, Larsson B, Lindroos AK, Lonroth H, Naslund I, Olbers T, Stenlof K, Torgerson J, Carlsson LM Swedish Obese Subjects Study (2009) Effects of bariatric surgery on cancer incidence in obese patients in Sweden (Swedish Obese Subjects Study): a prospective, controlled intervention trial. Lancet Oncol 10 (7): 653–662.
Stocks T, Rapp K, Bjorge T, Manjer J, Ulmer H, Selmer R, Lukanova A, Johansen D, Concin H, Tretli S, Hallmans G, Jonsson H, Stattin P (2009) Blood glucose and risk of incident and fatal cancer in the metabolic syndrome and cancer project (me-can): analysis of six prospective cohorts. PLoS Med 6 (12): e1000201.
Thakkar B, Aronis KN, Vamvini MT, Shields K, Mantzoros CS (2013) Metformin and sulfonylureas in relation to cancer risk in type II diabetes patients: a meta-analysis using primary data of published studies. Metabolism 62 (7): 922–934.
Tsilidis KK, Kasimis JC, Lopez DS, Ntzani EE, Ioannidis JP (2015) Type 2 diabetes and cancer: umbrella review of meta-analyses of observational studies. BMJ 350: g7607.
Verges B, Cariou B (2015) mTOR inhibitors and diabetes. Diabetes Res Clin Pract 110 (2): 101–108.
Verges B, Walter T, Cariou B (2014) Endocrine side effects of anti-cancer drugs: effects of anti-cancer targeted therapies on lipid and glucose metabolism. Eur J Endocrinol 170 (2): R43–R55.
Vigneri P, Frasca F, Sciacca L, Pandini G, Vigneri R (2009) Diabetes and cancer. Endocr Relat Cancer 16 (4): 1103–1123.
Wu L, Zhu J, Prokop LJ, Murad MH (2015) Pharmacologic therapy of diabetes and overall cancer risk and mortality: a meta-analysis of 265 studies. Sci Rep 5: 10147.
Acknowledgements
This work was supported by Instituto de Salud Carlos III (FIS), Grant Numbers PI12/01201 to ADlV and PI13/01150 to CG-J, and Universidad Rey Juan Carlos-Banco de Santander (Excellence group QUINANOAP). ACC is a recipient of fellowships: Marie Curie FP7-PEOPLE-2013-IEF: PIEF-GA-2013-626098 and EMBO long-term ALTF 800–2013.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on British Journal of Cancer website
Supplementary information
PowerPoint slides
Rights and permissions
This work is licensed under the Creative Commons Attribution-Non-Commercial-Share Alike 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
García-Jiménez, C., Gutiérrez-Salmerón, M., Chocarro-Calvo, A. et al. From obesity to diabetes and cancer: epidemiological links and role of therapies. Br J Cancer 114, 716–722 (2016). https://doi.org/10.1038/bjc.2016.37
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2016.37