Abstract
Background:
Breast cancer susceptibility gene 1 (BRCA1) expression differentially affects outcome to platinum- and taxane-based chemotherapy. Mediator of DNA damage checkpoint protein 1 (MDC1), p53-binding protein 1 (53BP1), multiple myeloma SET domain (MMSET) and ubiquitin-conjugating enzyme 9 (UBC9) are involved in DNA repair and could modify the BRCA1 predictive model.
Methods:
Mediator of DNA damage checkpoint protein 1, 53BP1, MMSET and UBC9 mRNA were assessed in gastric tumours from patients in whom BRCA1 levels had previously been determined.
Results:
In vitro chemosensitivity assay, MMSET levels were higher in docetaxel-sensitive samples. In a separate cohort, survival was longer in those with low MMSET (12.3 vs 8.8 months; P=0.04) or UBC9 (12.4 vs 8.8 months; P=0.01) in patients receiving only folinic acid, fluorouracil (5-FU) and oxaliplatin (FOLFOX). Conversely, among patients receiving second-line docetaxel, longer survival was associated with high MMSET (19.1 vs 13.9 months; P=0.003). Patients with high MMSET and BRCA1 attained a median survival of 36.6 months, compared with 13.9 months for those with high BRCA1 and low MMSET (P=0.003). In the multivariate analyses, low MMSET (hazard ratio (HR), 0.59; P=0.04) and low UBC9 (HR, 0.52; P=0.01) levels were markers of longer survival to first-line FOLFOX, whereas palliative surgery (HR, 2.47; P=0.005), low BRCA1 (HR, 3.17; P=0.001) and low MMSET (HR, 2.52; P=0.004) levels were markers of shorter survival to second-line docetaxel.
Conclusions:
Breast cancer susceptibility gene 1, MMSET and UBC9 can be useful for customising chemotherapy in gastric cancer patients.
Similar content being viewed by others
Main
Gastric cancer represents 8% of total cancer cases and 10% of total deaths worldwide, with an annual estimate of 989 600 new cases and 738 000 deaths (Jemal et al, 2011). China accounts for 40% of all gastric cancer patients, most of whom are diagnosed with advanced disease (Jemal et al, 2011). The outcome for locally advanced and metastatic gastric cancer is still dismal, with a median survival of <1 year (Wagner et al, 2006). In our previous experience, however, median survival was 15.8 months in gastric cancer patients with low mRNA expression of excision repair cross-complementing 1 (ERCC1) treated with the combination of folinic acid, fluorouracil (5-FU) and oxaliplatin (FOLFOX) (Wei et al, 2008). We also found that among patients receiving second-line docetaxel, median overall survival was 25.8 months for patients with high mRNA expression of breast cancer susceptibility gene 1 (BRCA1; Wei et al, 2011).
Chemotherapy induces widespread DNA damage. Although ERCC1 and BRCA1 can affect survival to chemotherapy because of their pivotal roles in DNA damage response pathways, recent studies have revealed a more complex network involved in the response to DNA damage. Preclinical evidence showed that receptor-associated protein 80 (RAP80) is essential for the BRCA1 repair function (Sobhian et al, 2007; Morris et al, 2009). In addition, BRCA1 is also modified by small ubiquitin-related modifier (SUMO) in response to genotoxic damage. Protein inhibitor of activated STAT (PIAS) SUMO ligases are required for proficient double-strand break repair (Galanty et al, 2009), which has been investigated in our previous study (Wei et al, 2011). In DNA damage repair, mediator of DNA damage checkpoint protein 1 (MDC1) serves as a upstream molecular, which promotes H2AX phosphorylation and then helps to amplify ataxia telangiectasia mutated signalling by a time-dependent, sequential assembly of repair proteins, including BRCA1 and p53-binding protein 1 (53BP1), thus controlling damage-induced cell cycle arrest checkpoints (Stewart et al, 2003; Stucki et al, 2005). The function of 53BP1 in DNA repair is abrogated when BRCA1 is depleted (Rauch et al, 2005; Bunting et al, 2010). Impaired 53BP1 accumulation to DNA damage sites was also observed along with depletion of PIAS4 and ubiquitin-conjugating enzyme 9 (UBC9), the E3 and E2 ubiquitin ligases in the SUMO conjugation system (Galanty et al, 2009). Ubiquitin-conjugating enzyme 9 transports BRCA1 proteins to the nucleus, and knockdown of UBC9 resulted in cytoplasmic localisation of BRCA1 proteins, which were impaired in their capacity to inhibit growth of ovarian cancer cells (Qin et al, 2012). The methyltransferase multiple myeloma SET domain (MMSET) has a central role in the recruitment of 53BP1 to DNA damage sites (Pei et al, 2011), and depletion of MMSET confers hypersensitivity to ionising radiation (Pei et al, 2011). Multiple myeloma SET domain is highly expressed in several tumour types compared with normal tissues (Kassambara et al, 2009; Hudlebusch et al, 2011a), and high MMSET expression contributes to cell viability and growth and thus to poor prognosis (Hudlebusch et al, 2011b). In addition, MMSET knockdown decreased transcript levels of several cell cycle genes, including BRCA1 (Brito et al, 2009; Figure 1).
The MDC–MMSET–UBC9–53BP1–BRCA1 pathway. In response to DNA double-stand breaks, MDC1 directly binds to histone H2A variant H2AX, regulating cellular responses to DNA repair by BRCA1 and 53BP1. Breast cancer susceptibility gene 1 needs to be SUMOylated through the activity of UBC9-PIAS1/4 at sites of DNA damage to increase its ubiquitin ligase activity. Multiple myeloma SET domain is required for the recruitment of 53BP1 to DNA damage sites.
In order to examine the impact of MDC1, 53BP1, MMSET and UBC9 on the predictive model based on BRCA1 mRNA expression, we have analysed the mRNA expression of these genes in tumour samples from two separate cohorts of advanced gastric cancer patients. In 99 patients, we correlated expression levels with in vitro cytotoxicity of cisplatin and docetaxel, and in the second cohort of 132 advanced gastric cancer patients in whom BRCA1 mRNA expression had previously been determined (Wei et al, 2011), we correlated expression levels with survival to first-line FOLFOX and to second-line docetaxel-based chemotherapy.
Materials and methods
Patients
Freshly removed gastric tumour tissues were obtained from 99 patients undergoing gastrectomy between 2010 and 2011 at the General Surgery Department of Drum Tower Hospital, Nanjing, China. Gene expression levels of MDC1, 53BP1, MMSET and UBC9 were determined and correlated with in vitro tumour chemosensitivity. In a second independent cohort of 132 patients (Wei et al, 2011) with histologically proven locally advanced or metastatic gastric cancer and Eastern Cooperative Oncology Group (ECOG) performance status (PS) ⩽2, we examined the expression of the four genes in tumour samples obtained at the time of surgical resection and correlated gene expression levels with overall survival. All patients received a modified FOLFOX regimen as first-line chemotherapy, and 58 patients were also treated with second-line docetaxel-based chemotherapy. Thirty-five patients received single-agent docetaxel and the remaining 23 patients were treated with docetaxel-based doublets, based on their response to first-line chemotherapy, PS and patient consent.
Survival was calculated from the starting date of first-line treatment to the date of last follow-up or death from any cause. All patients gave their signed informed consent, and the study was approved by the institutional ethics review board of Drum Tower Hospital.
In vitro chemosensitivity
Sensitivity to docetaxel and cisplatin was examined in vitro by histoculture drug response assay (Furukawa et al, 1995). Briefly, fresh tumour specimens were cut into small pieces of approximately 10 mg and then placed on prepared collagen surfaces in 24-well microplates. After treatment with docetaxel and cisplatin at the concentration of 100 μg ml–1 (Hayashi et al, 2009) and 20 μg ml–1 (Fujita et al, 2009), respectively, 3-(4,5-dimethyl-2-thiazotyl)-2,5-diphenyl-2H-tetrazoliumbromide assay was used to examine cytotoxicity. The inhibition rate was calculated as previously reported (Shen et al, 2012).
Gene expression analysis
Breast cancer susceptibility gene 1 expression had previously been determined in all patients (Wei et al, 2011). We analysed the mRNA expression of MDC1, 53BP1, MMSET and UBC9 by quantitative PCR. RNA was isolated from the macrodissected tumour tissue specimens in accordance with a proprietary procedure (European patent number EP1945764-B1). Briefly, paraffin was removed by xylene. Macrodissected tumour samples were lysed in a proteinase K-containing buffer. RNA was then purified with phenol–chloroform–isoamyl alcohol, followed by precipitation with isopropanol in the presence of glycogen and sodium acetate. RNA was re-suspended in water and treated with DNAse I to avoid DNA contamination. cDNA was generated using M-MLV retrotranscriptase enzyme. Template cDNA was amplified with specific primers and probes for each gene and Taqman Universal Master Mix (Applied Biosystems, Foster City, CA, USA). Quantification of gene expression was performed using the ABI Prism 7900HT Sequence Detection System (Applied Biosystems). In all quantitative experiments, only triplicates with an s.d. of the Ct values <0.30 were accepted. Relative gene expression quantifications were calculated according to the comparative Ct method using β-actin as an endogenous control and commercial human lung and liver RNA (Stratagene, La Jolla, CA, USA) as calibrators. Final results were determined by the formula 2−ΔΔCt and were performed according to Technical Bulletin #2 (Applied Biosystems).
Statistical analysis
Median values and ranges were calculated for quantitative variables and gene mRNA expression. Qualitative variables were summarised by absolute frequencies and percentages. The normality of quantitative variables was analysed by the Kolmogorov–Smirnov test and compared with the Mann–Whitney U and Kruskal–Wallis tests. In order to correlate gene expression levels with clinical characteristics, the χ2 test or Fisher’s exact test was used for qualitative variables. The Spearman rho method was used to correlate the expression levels of the four genes. The Mann-Whitney U-test was used to compare gene expression levels in chemosensitive and chemoresistant groups. The distributions of survival were obtained by the Kaplan–Meier method and compared with the log-rank test. A univariate analysis was performed to evaluate the survival differences according to gender, ECOG PS, histology, site, stage or expression levels of MDC1, 53BP1, MMSET and UBC9. A multivariate analysis was performed and the hazard ratio (HR) and 95% confidence intervals (CIs) were estimated with the use of the forward and backward Cox proportional hazards model.
All statistical calculations were performed with the Statistical Package for the Social Sciences for Windows version 17 (SPSS Inc., Chicago, IL, USA) and S-Plus 6.1 (Insightful Corporation, Seattle, WA, USA). Two-sided P-values <0.05 was considered statistically significant.
Results
Patient characteristics
The in vitro study included 99 gastric cancer patients. All patients had adenocarcinoma, and 73.3% were males. The clinical study included a separate cohort of 132 gastric cancer patients in whom BRCA1 expression had previously been analysed (Wei et al, 2011). Median age was 60.5 years (range, 22–84); 102 patients were males; 90.9% had PS 0–1; 98.4% had adenocarcinoma. Curative gastrectomy was performed in 65.9% of the patients, while the rest received palliative surgery. Forty patients (30.3%) had stage IIIA, 41 (31.1%) stage IIIB and 51 (38.6%) stage IV disease at the time of diagnosis (Table 1). The median number of cycles of FOLFOX was three (range, 1–8). All patients progressed to first-line chemotherapy, and 58 patients were treated with second-line docetaxel chemotherapy. The median number of cycles of second-line chemotherapy was three (range, 1–7). The median age of patients receiving second-line docetaxel-based therapy was younger than those treated only with first-line chemotherapy (58 vs 64 years, P=0.05). No other differences were observed between patients receiving and those not receiving second-line therapy (Table 1).
Gene expression levels and in vitro chemosensitivity
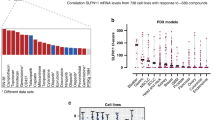
The expression levels of MDC1, 53BP1 and MMSET were successfully assessed in 94 of the 99 samples, whereas UBC9 expression was assessed in 90 samples. In the in vitro study, the median gene expression relative to the housekeeping β-actin gene was 1.1 for MDC1 (range, 0.05–18.8), 3.6 for 53BP1 (range, 0.2–23.4), 3.3 for MMSET (range, 0.1–35.8) and 2.5 for UBC9 (range, 0.04–13.1). When the gastric cancer samples were divided into chemosensitive and chemoresistant subgroups by the median value of inhibition to docetaxel or cisplatin, MMSET mRNA levels were higher in the docetaxel-sensitive than in the docetaxel-resistant group (7.17 vs 3.63; P=0.013; Figure 2). No other differences in gene expression were observed between the chemosensitive and chemoresistant groups.
Gene expression levels and overall survival
BRCA1 expression levels had previously been determined in all 132 patients (Wei et al, 2011). The expression levels of MDC1, 53BP1, MMSET and UBC9 were successfully assessed in all samples. The median gene expression relative to the housekeeping β-actin gene was 3.3 for MDC1 (range, 0.5–43.7), 5.7 for 53BP1 (range, 1.2–66), 6.5 for MMSET (range, 0.8–73.6) and 1.9 for UBC9 (range, 0.3–13.2). Patients were classified as having high or low gene expression using the median as cutoff. No differences in clinical characteristics were observed according to the mRNA expression levels of any of the four genes.
With a median follow-up of 13.7 months (range, 1.3–68.1 months), median survival was 11.6 months (95% CI, 9.8–13.4 months) for all 132 patients. There was no difference in overall survival time according to the expression levels of any of the genes. Median survival time for the 58 patients receiving second-line therapy was 14.9 months (95% CI, 11.6–18.3 months), compared with 9.9 months (95% CI, 8.2–11.7 months) for those receiving only first-line chemotherapy (P=0.03).
Among patients receiving only first-line therapy, median survival was 12.3 months (95% CI, 7.9–16.6 months) for those with low levels of MMSET, compared with 8.8 months (95% CI, 5.9–11.7 months) for those with high levels (P=0.04; Figure 3A). Median survival was 12.4 months (95% CI, 10.2–14.5 months) for those with low levels of UBC9 and 8.8 months (95% CI, 5.8–11.8 months) for those with high levels (P=0.01; Figure 3B). Longer survival was also observed in patients with low levels of MDC1 (P=0.49) and 53BP1 (P=0.09), although the difference was not significant. As previously reported in this patient cohort, longer trend of survival was also observed in patients with low BRCA1 expression (P=0.20; Wei et al, 2011). Among patients with low MMSET expression, median survival was 19.9 months (95% CI, 0.7–39.1 months) for those with low 53BP1 levels and 5.9 months (95% CI, 1.6–10.3 months) for those with high 53BP1 levels (P=0.02; Figure 4). A nonsignificant trend towards longer survival was observed in those with low UBC9 levels (P=0.36), those with low BRCA1 levels (P=0.36) and those with low MDC1 levels (P=0.67).
Among the 58 patients receiving second-line chemotherapy, those with high MMSET levels had longer survival (19.1 months; 95% CI, 5.2–33.1 months) than those with low levels (13.9 months; 95% CI, 7.1–20.7 months; P=0.003; Figure 5A). As previously reported, longer survival was also attained by patients with high levels of BRCA1 (28.6 months; 95% CI, 20.2–36.9 months) compared with those with low levels (9.8 months; 95% CI, 7.2–12.5 months; P<0.0001; Wei et al, 2011). A nonsignificant trend toward longer survival was also observed in patients with high expression of MDC1 (P=0.07), 53BP1 (P=0.36) and UBC9 (P=0.17). In the subgroup of 25 patients with high BRCA1 levels receiving second-line chemotherapy, overall survival was 36.6 months (95% CI, 23.6–49.6 months) in patients with high MMSET levels and 13.9 months (95% CI, 3.2–24.6 months) in those with low levels (P=0.003; Figure 5B). Two-year survival was 70.6% (95% CI, 48.8–92.3%) in patients with high BRCA1 and high MMSET levels, compared with 25% (95% CI, 0.1–54.9%) in those with high BRCA1 but low MMSET levels. Five-year survival rates were 33% (95% CI, 7.7–58.3%) for patients with high BRCA1 and MMSET levels and 0% for those with high BRCA1 and low MMSET levels (test for trend: P=0.002).
Multivariable analyses were performed separately in patients receiving only first-line treatment and in those receiving second-line treatment. In patients receiving only first-line chemotherapy, a lower risk of mortality was observed in patients with low MMSET levels (HR, 0.59; 95% CI, 0.35–0.98; P=0.04) and in patients with low UBC9 levels (HR, 0.52; 95% CI, 0.31–0.88; P=0.01; Table 2). In patients receiving second-line chemotherapy, a higher risk of mortality was observed in patients undergoing palliative surgery (HR, 2.47; 95% CI, 1.31–4.66; P=0.005), in patients with low BRCA1 levels (HR, 3.17; 95% CI, 1.61–6.22; P=0.001) and in patients with low MMSET levels (HR, 2.52; 95% CI, 1.34–4.70; P=0.004; Table 2).
Discussion
Most gastric cancer patients present with advanced disease and their prognosis is dismal (Leung et al, 2008). Although there was no remarkable progress in chemotherapy for advanced gastric cancer in the 1990s, in the early 2000s new agents and optional treatments emerged. The ToGA trial (Bang et al, 2010) showed that trastuzumab confers a survival benefit for patients with HER2-positive gastric cancer, which comprises 10–20% of patients. Many targeted agents are currently being investigated and the progress in the treatment of advanced gastric cancer, including individualised therapy, can be expected in the near future. We have previously observed that gastric cancer patients with low ERCC1 mRNA levels could benefit from FOLFOX chemotherapy (Wei et al, 2008) and that patients with high BRCA1 levels had longer survival when treated with docetaxel-based second-line chemotherapy (Wei et al, 2011).
In this study, patients with low levels of MMSET had longer survival than those with high levels (12.3 vs 8.8 months) when treated with only platinum-based first-line chemotherapy. Multiple myeloma SET domain is involved in the t(4 : 14) translocation, which is present in approximately 15–25% of multiple myelomas (Asangani et al, 2013). High MMSET protein levels are associated with high malignant potential in several solid tumours (Glinsky et al, 2004; Yang et al, 2005; Wurmbach et al, 2007; Xiao et al, 2012; Zhou et al, 2012). Overexpression of MMSET was associated with increased c-MYC expression, related to the ability of MMSET to repress the expression of miR-126*, a microRNA targeting c-MYC (Min et al, 2012), which also has an oncogenic function in gastric cancer through suppression of SOX2 (Otsubo et al, 2011). Multiple myeloma SET domain interacts with MDC1 in a DNA damage-inducible manner and downregulation of MMSET significantly decreases histone methylation and the subsequent accumulation of 53BP1 (Pei et al, 2011). A similar effect of MMSET was also observed in class switch recombination (Pei et al, 2013). Downregulation of MMSET confers hypersensitivity to DNA damage (Pei et al, 2011).
In contrast to the survival benefit conferred by low MMSET expression in patients receiving platinum-based treatment, MMSET expression was higher in docetaxel-sensitive than in docetaxel-resistant samples in vitro, and moreover, low levels of MMSET were associated with shorter survival (13.9 vs 19.1 months) in patients receiving docetaxel-based treatment. High MMSET levels could potentially enhance BRCA1 function, and a similar differential effect has been reported for BRCA1 expression, which induces a 10- to 1000-fold increase in resistance to cisplatin but an 800- to >1000-fold increase in sensitivity to docetaxel (Quinn et al, 2003, 2007). In our previous study in tumour cells isolated from malignant effusions of gastric cancer patients, we observed a similar effect of BRCA1 expression (Wang et al, 2008).
Nevertheless, the most intriguing finding in this study was the combined effect of MMSET and BRCA1 in patients receiving second-line docetaxel-based treatment, wherein those with high levels of both genes attained an unprecedented median survival of 36.6 months compared with 13.9 months in those with high levels of BRCA1 and low levels of MMSET (P=0.003). The 2-year and 5-year survival rates were also higher in patients with high levels of both BRCA1 and MMSET (70.6% vs 25% and 33% vs 0%, respectively). Moreover, in the multivariate analysis, together with type of surgery, BRCA1 and MMSET levels emerged as significant markers of survival. This combined effect of MMSET and BRCA1 expression on outcome to docetaxel in advanced gastric cancer could be explained by the experimental data in myeloma, where MMSET deregulation affected cell cycle progression and adhesion regulations, including BRCA1 (Brito et al, 2009). However, MMSET serves as chromatin modifiers in cancer development. It functions as a master regulator of transcriptional repression, activation and oncogenesis (Asangani et al, 2013). The global impact of MMEST levels in patients beyond DNA damage response should be further investigated.
In this study, we have also observed striking differences in survival according to UBC9 expression in patients receiving only first-line FOLFOX. Patients with low levels of UBC9 attained a median survival of 12.4 months, in contrast with 8.8 months for those with high levels (P=0.01). Similar, although nonsignificant, trends were also observed in patients with low levels of BRCA1, MDC1 or 53BP1, and a subgroup of patients with low levels of both MMSET and 53BP1 attained the longest overall survival (19.9 months). In the multivariate analysis, only MMSET and UBC9 levels significantly influenced survival to first-line FOLFOX. In response to DNA damage, inhibition of MDC1 results in defective BRCA1 and 53BP1 foci formation after ionising radiation (Goldberg et al, 2003). Before being transported to DNA damage sites, BRCA1 needs to be SUMOylated through the activity of UBC9-PIAS1/4 at sites of DNA damage to increase its ubiquitin ligase activity (Morris et al, 2009). Ubiquitin-conjugating enzyme 9 is the sole E2-conjugating enzyme identified for SUMOylation. Ubiquitin-conjugating enzyme 9 depletion impairs 53BP1 accumulation (Galanty et al, 2009). Dysregulation of UBC9, MMSET, MDC1, 53BP1 and BRCA1 results in aberrant responses to DNA damage, which may have led to the poorer outcome observed in this subgroup of patients treated with platinum-based chemotherapy.
To date, there is no gold standard for first-line chemotherapy for gastric cancer patients, despite a great deal of information on the heterogeneous biological background of the disease. Moreover, at the time of failure to first-line chemotherapy, nearly half the patients could be candidates for further treatment (Ji et al, 2009). This study provides a tool for selecting patients who will likely benefit from FOLFOX – based on MMSET and UBC9 – and those who will benefit from docetaxel – based on BRCA1 (Wei et al, 2011) and MMSET. Prospective studies are needed to further validate the potential roles of MMSET and UBC9 on BRCA1 expression-based personalised therapeutic strategy in gastric cancer patients.
Change history
27 May 2014
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Asangani IA, Ateeq B, Cao Q, Dodson L, Pandhi M, Kunju LP, Mehra R, Lonigro RJ, Siddiqui J, Palanisamy N, Wu YM, Cao X, Kim JH, Zhao M, Qin ZS, Iyer MK, Maher CA, Kumar-Sinha C, Varambally S, Chinnaiyan AM (2013) Characterization of the EZH2-MMSET histone methyltransferase regulatory axis in cancer. Mol Cell 49 (1): 80–93.
Bang YJ, Van Cutsem E, Feyereislova A, Chung HC, Shen L, Sawaki A, Lordick F, Ohtsu A, Omuro Y, Satoh T, Aprile G, Kulikov E, Hill J, Lehle M, Ruschoff J, Kang YK (2010) Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet 376 (9742): 687–697.
Brito JL, Walker B, Jenner M, Dickens NJ, Brown NJ, Ross FM, Avramidou A, Irving JA, Gonzalez D, Davies FE, Morgan GJ (2009) MMSET deregulation affects cell cycle progression and adhesion regulons in t(4;14) myeloma plasma cells. Haematologica 94 (1): 78–86.
Bunting SF, Callen E, Wong N, Chen HT, Polato F, Gunn A, Bothmer A, Feldhahn N, Fernandez-Capetillo O, Cao L, Xu X, Deng CX, Finkel T, Nussenzweig M, Stark JM, Nussenzweig A (2010) 53BP1 inhibits homologous recombination in Brca1-deficient cells by blocking resection of DNA breaks. Cell 141 (2): 243–254.
Fujita Y, Hiramatsu M, Kawai M, Nishimura H, Miyamoto A, Tanigawa N (2009) Histoculture drug response assay predicts the postoperative prognosis of patients with esophageal cancer. Oncol Rep 21 (2): 499–505.
Furukawa T, Kubota T, Hoffman RM (1995) Clinical applications of the histoculture drug response assay. Clin Cancer Res 1 (3): 305–311.
Galanty Y, Belotserkovskaya R, Coates J, Polo S, Miller KM, Jackson SP (2009) Mammalian SUMO E3-ligases PIAS1 and PIAS4 promote responses to DNA double-strand breaks. Nature 462 (7275): 935–939.
Glinsky GV, Glinskii AB, Stephenson AJ, Hoffman RM, Gerald WL (2004) Gene expression profiling predicts clinical outcome of prostate cancer. J Clin Invest 113 (6): 913–923.
Goldberg M, Stucki M, Falck J, D'Amours D, Rahman D, Pappin D, Bartek J, Jackson SP (2003) MDC1 is required for the intra-S-phase DNA damage checkpoint. Nature 421 (6926): 952–956.
Hayashi Y, Kuriyama H, Umezu H, Tanaka J, Yoshimasu T, Furukawa T, Tanaka H, Kagamu H, Gejyo F, Yoshizawa H (2009) Class III beta-tubulin expression in tumor cells is correlated with resistance to docetaxel in patients with completely resected non-small-cell lung cancer. Intern Med 48 (4): 203–208.
Hudlebusch HR, Santoni-Rugiu E, Simon R, Ralfkiaer E, Rossing HH, Johansen JV, Jorgensen M, Sauter G, Helin K (2011a) The histone methyltransferase and putative oncoprotein MMSET is overexpressed in a large variety of human tumors. Clin Cancer Res 17 (9): 2919–2933.
Hudlebusch HR, Skotte J, Santoni-Rugiu E, Zimling ZG, Lees MJ, Simon R, Sauter G, Rota R, De Ioris MA, Quarto M, Johansen JV, Jorgensen M, Rechnitzer C, Maroun LL, Schroder H, Petersen BL, Helin K (2011b) MMSET is highly expressed and associated with aggressiveness in neuroblastoma. Cancer Res 71 (12): 4226–4235.
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61 (2): 69–90.
Ji SH, Lim do H, Yi SY, Kim HS, Jun HJ, Kim KH, Chang MH, Park MJ, Uhm JE, Lee J, Park SH, Park JO, Park YS, Lim HY, Kang WK (2009) A retrospective analysis of second-line chemotherapy in patients with advanced gastric cancer. BMC Cancer 9: 110.
Kassambara A, Klein B, Moreaux J (2009) MMSET is overexpressed in cancers: link with tumor aggressiveness. Biochem Biophys Res Commun 379 (4): 840–845.
Leung WK, Wu MS, Kakugawa Y, Kim JJ, Yeoh KG, Goh KL, Wu KC, Wu DC, Sollano J, Kachintorn U, Gotoda T, Lin JT, You WC, Ng EK, Sung JJ (2008) Screening for gastric cancer in Asia: current evidence and practice. Lancet Oncol 9 (3): 279–287.
Min DJ, Ezponda T, Kim MK, Will CM, Martinez-Garcia E, Popovic R, Basrur V, Elenitoba-Johnson KS, Licht JD (2012) MMSET stimulates myeloma cell growth through microRNA-mediated modulation of c-MYC. Leukemia 27 (3): 686–694.
Morris JR, Boutell C, Keppler M, Densham R, Weekes D, Alamshah A, Butler L, Galanty Y, Pangon L, Kiuchi T, Ng T, Solomon E (2009) The SUMO modification pathway is involved in the BRCA1 response to genotoxic stress. Nature 462 (7275): 886–890.
Otsubo T, Akiyama Y, Hashimoto Y, Shimada S, Goto K, Yuasa Y (2011) MicroRNA-126 inhibits SOX2 expression and contributes to gastric carcinogenesis. PLoS One 6 (1): e16617.
Pei H, Wu X, Liu T, Yu K, Jelinek DF, Lou Z (2013) The histone methyltransferase MMSET regulates class switch recombination. J Immunol 190 (2): 756–763.
Pei H, Zhang L, Luo K, Qin Y, Chesi M, Fei F, Bergsagel PL, Wang L, You Z, Lou Z (2011) MMSET regulates histone H4K20 methylation and 53BP1 accumulation at DNA damage sites. Nature 470 (7332): 124–128.
Qin Y, Xu J, Aysola K, Oprea G, Reddy A, Matthews R, Okoli J, Cantor A, Grizzle WE, Partridge EE, Reddy ES, Landen C, Rao VN (2012) BRCA1 proteins regulate growth of ovarian cancer cells by tethering Ubc9. Am J Cancer Res 2 (5): 540–548.
Quinn JE, James CR, Stewart GE, Mulligan JM, White P, Chang GK, Mullan PB, Johnston PG, Wilson RH, Harkin DP (2007) BRCA1 mRNA expression levels predict for overall survival in ovarian cancer after chemotherapy. Clin Cancer Res 13 (24): 7413–7420.
Quinn JE, Kennedy RD, Mullan PB, Gilmore PM, Carty M, Johnston PG, Harkin DP (2003) BRCA1 functions as a differential modulator of chemotherapy-induced apoptosis. Cancer Res 63 (19): 6221–6228.
Rauch T, Zhong X, Pfeifer GP, Xu X (2005) 53BP1 is a positive regulator of the BRCA1 promoter. Cell Cycle 4 (8): 1078–1083.
Shen J, Wang H, Wei J, Yu L, Xie L, Qian X, Zou Z, Liu B, Guan W (2012) Thymidylate synthase mRNA levels in plasma and tumor as potential predictive biomarkers for raltitrexed sensitivity in gastric cancer. Int J Cancer 131 (6): E938–E945.
Sobhian B, Shao G, Lilli DR, Culhane AC, Moreau LA, Xia B, Livingston DM, Greenberg RA (2007) RAP80 targets BRCA1 to specific ubiquitin structures at DNA damage sites. Science 316 (5828): 1198–1202.
Stewart GS, Wang B, Bignell CR, Taylor AM, Elledge SJ (2003) MDC1 is a mediator of the mammalian DNA damage checkpoint. Nature 421 (6926): 961–966.
Stucki M, Clapperton JA, Mohammad D, Yaffe MB, Smerdon SJ, Jackson SP (2005) MDC1 directly binds phosphorylated histone H2AX to regulate cellular responses to DNA double-strand breaks. Cell 123 (7): 1213–1226.
Wagner AD, Grothe W, Haerting J, Kleber G, Grothey A, Fleig WE (2006) Chemotherapy in advanced gastric cancer: a systematic review and meta-analysis based on aggregate data. J Clin Oncol 24 (18): 2903–2909.
Wang L, Wei J, Qian X, Yin H, Zhao Y, Yu L, Wang T, Liu B (2008) ERCC1 and BRCA1 mRNA expression levels in metastatic malignant effusions is associated with chemosensitivity to cisplatin and/or docetaxel. BMC Cancer 8: 97.
Wei J, Costa C, Ding Y, Zou Z, Yu L, Sanchez JJ, Qian X, Chen H, Gimenez-Capitan A, Meng F, Moran T, Benlloch S, Taron M, Rosell R, Liu B (2011) mRNA expression of BRCA1, PIAS1, and PIAS4 and survival after second-line docetaxel in advanced gastric cancer. J Natl Cancer Inst 103 (20): 1552–1556.
Wei J, Zou Z, Qian X, Ding Y, Xie L, Sanchez JJ, Zhao Y, Feng J, Ling Y, Liu Y, Yu L, Rosell R, Liu B (2008) ERCC1 mRNA levels and survival of advanced gastric cancer patients treated with a modified FOLFOX regimen. Br J Cancer 98 (8): 1398–1402.
Wurmbach E, Chen YB, Khitrov G, Zhang W, Roayaie S, Schwartz M, Fiel I, Thung S, Mazzaferro V, Bruix J, Bottinger E, Friedman S, Waxman S, Llovet JM (2007) Genome-wide molecular profiles of HCV-induced dysplasia and hepatocellular carcinoma. Hepatology 45 (4): 938–947.
Xiao M, Yang S, Chen J, Ning X, Guo L, Huang K, Sui L (2012) Overexpression of MMSET in endometrial cancer: a clinicopathologic study. J Surg Oncol 107 (4): 428–432.
Yang XJ, Tan MH, Kim HL, Ditlev JA, Betten MW, Png CE, Kort EJ, Futami K, Furge KA, Takahashi M, Kanayama HO, Tan PH, Teh BS, Luan C, Wang K, Pins M, Tretiakova M, Anema J, Kahnoski R, Nicol T, Stadler W, Vogelzang NG, Amato R, Seligson D, Figlin R, Belldegrun A, Rogers CG, Teh BT (2005) A molecular classification of papillary renal cell carcinoma. Cancer Res 65 (13): 5628–5637.
Zhou P, Wu LL, Wu KM, Jiang W, Li JD, Zhou LD, Li XY, Chang S, Huang Y, Tan H, Zhang GW, He F, Wang ZM (2012) Overexpression of MMSET is correlation with poor prognosis in hepatocellular carcinoma. Pathol Oncol Res 19 (2): 303–309.
Acknowledgements
This work was funded by grants from the National Natural Science Foundation of China (grant no. 81000980, 81220108023, 81370064), Jiangsu Provincial Program of Medical Science (BL2012001) and the distinguished young investigator project of Nanjing (JQX12002). Work in Dr Rafael Rosell's laboratory was partially supported by a grant from La Caixa Foundation. The funding sources had no role in the study design, data collection, data analysis, data interpretation or writing of the report.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Wei, J., Costa, C., Shen, J. et al. Differential effect of MMSET mRNA levels on survival to first-line FOLFOX and second-line docetaxel in gastric cancer. Br J Cancer 110, 2662–2668 (2014). https://doi.org/10.1038/bjc.2014.231
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2014.231
Keywords
This article is cited by
-
The role of NSD1, NSD2, and NSD3 histone methyltransferases in solid tumors
Cellular and Molecular Life Sciences (2022)
-
Plasma mRNA expression levels of BRCA1 and TS as potential predictive biomarkers for chemotherapy in gastric cancer
Journal of Translational Medicine (2014)