Abstract
Background:
Glioblastoma multiforme (GBM) cells are resistant to anticancer drugs. Cancer stem cells (CSCs) are a key mediator of chemoresistance. We have reported that disulfiram (DS), an aldehyde dehydrogenase (ALDH) inhibitor, targets breast CSC-like cells. In this study, the effect of DS and combination of DS and gemcitabine (dFdC) on GBM cells and GBM stem-like cells was investigated.
Methods:
1-(4,5-Dimethylthiazol-2-yl)-3,5-diphenylformazan (MTT), combination index (CI)-isobologram, western blot, luciferase reporter gene assay, electrophoretic mobility-shift assay and ALDH analysis were used in this study.
Results:
Disulfiram is cytotoxic in GBM cell lines in a copper (Cu)-dependent manner. Disulfiram/copper enhances the cytotoxicity of dFdC. Combination index-isobologram analysis indicates a synergistic effect between DS/Cu and dFdC. Disulfiram/copper induces reactive oxygen species (ROS), activates JNK and p38 pathways and inhibits nuclear factor-kappa B activity in GBM cell lines. Disulfiram/copper may trigger intrinsic apoptotic pathway via modulation of the Bcl2 family. Disulfiram/copper abolishes stem-like cell population in GBM cell lines.
Conclusion:
Our findings indicate that the cytotoxicity of DS/Cu and the enhancing effect of DS/Cu on the cytotoxicity of dFdC in GBM stem-like cells may be caused by induction of ROS and inhibition of both ALDH and the NFkB pathway. Both DS and dFdC can traverse the blood–brain barrier. Further study may lead them into GBM chemotherapy.
Similar content being viewed by others
Main
Glioblastoma multiforme (GBM) is the most common primary malignant brain tumour in adults with median survival time less than 1 year and 2 year survival rates of 3.3% (Reardon et al, 2006). To date, there are limited agents available for GBM chemotherapy. Because of the blood–brain barrier (BBB) blocking distribution to the target site and high level chemoresistance in this tumour type, current chemotherapy does not add much survival advantage over the classical approach of surgery followed by radiotherapy. Therefore, development of novel effective anti-GBM agents will be of significant clinical importance in GBM treatment.
Gemcitabine (2′,2′-difluorodeoxycytidine, dFdC) is a deoxyribonucleoside analogue with activity against a wide range of haematological and solid cancers either as a single agent or in combination with other anticancer agents (Bergman et al, 2002). Gemcitabine is one of the handful of classical anticancer drugs, which can pass the BBB, penetrate into the tumour mass and be efficiently converted into its active form in GBM tissues (Metro et al, 2010). Although dFdC is a good candidate, its use in GBM chemotherapy is limited by high resistance to this agent in GBM cells. Thus, it is currently primarily used in combination with radiotherapy as a radiosensitizer for GBM treatment (Metro et al, 2010). Identification of agents, which synergistically sensitise GBM cells to dFdC chemotherapy without increasing toxicity to normal brain tissues, may lead to new effective dFdC-based chemotherapy regimens for GBM treatment.
We have previously reported that disulfiram (DS) synergistically enhances dFdC cytotoxicity and reverses dFdC resistance in cancer cell lines (Guo et al, 2010). Disulfiram is a first line anti-alcoholism drug that has been used clinically for over 60 years (Johansson, 1992). Recent studies demonstrate that DS has strong anticancer activity in vitro and in cancer xenografts (Chen et al, 2006; Iljin et al, 2009; Conticello et al, 2012), highlighting it as a potential novel chemotherapeutic agent. Disulfiram potentiates the cytotoxicity of several classical anticancer drugs as well as radiation (Hacker et al, 1982; Bodenner et al, 1986; Cen et al, 2004; Chen et al, 2006; Yip et al, 2011).
The anticancer mechanisms of DS are still not fully elucidated. Our and others recent data indicate that the cytotoxicity of DS is copper (Cu) dependent (Cen et al, 2004; Chen et al, 2006; Yip et al, 2011). Copper has a crucial role in redox reactions and triggers generation of reactive oxygen species (ROS) in human cells (Barceloux, 1999). The concept of using Cu to tackle cancer was proposed many decades ago (Hieger, 1926) but it did not demonstrate clinical efficacy. The discord between theory and practice may be due to limited transport of Cu into cancer cells by the trans-membrane Cu transporter Ctr1. As a bivalent metal ion chelator, DS forms a complex with Cu and improves the transport of Cu into cancer cells. In comparison with Cu, the DS/Cu complex is a stronger ROS inducer (Burkitt et al, 1998). Reactive oxygen species are a group of reactive oxygen-containing chemical species normally generated from the mitochondrial respiratory chain reaction (Gupte and Mumper, 2009). High ROS activity can damage DNA, protein and lipids leading to apoptosis. In comparison with normal tissues, cancer cells possess higher ROS activity (Fruehauf and Meyskens, 2007). Because of their anti-apoptotic machinery, cancer cells can tolerate higher ROS levels. Reactive oxygen species even have a key role in signalling transduction in cancer cells. Considering the higher ROS-load in cancer cells, it has been proposed that a further ROS exposure induced by ROS-generating agents will exhaust their cellular antioxidant capacity and selectively lead cancer cells into apoptosis (Lopez-Lazaro, 2007). In comparison with normal tissues, many cancer types including GBM possess significantly higher levels of intracellular Cu (Margalioth et al, 1983; Yoshida et al, 1993). Disulfiram can penetrate and chelate Cu intracellularly. As the cytotoxicity of DS appears to be Cu dependent, high Cu concentration in cancer cells may enable DS to specifically target cancer and spare normal tissues (Hacker et al, 1982; Bodenner et al, 1986; Chen et al, 2006).
Furthermore, ROS-induced DNA damage can trigger the expression of anti-apoptotic proteins, which confer drug resistance upon cancer cells. Thus, targeting these proteins may result in improved chemotherapeutic outcomes following use of ROS-generating agents. Nuclear factor-kappa B (NFκB) is an important anti-apoptotic and chemoresistance-related factor. Many human cancer cells possess high constitutive NFκB activity, which can be further induced by chemotherapy. Activated NFκB triggers a series of molecular reactions including upregulation of genes encoding anti-apoptotic proteins (Rayet and Gelinas, 1999), inducing cancer chemoresistance. High NFκB activity has been identified in drug-resistant cancer cell lines. Ectopic overexpression of NFκB blocks apoptosis (Wang et al, 2003, 2004; Guo et al, 2010; Yip et al, 2011). Although NFκB is an attractive molecular target for therapeutic intervention, inhibition of NFκB alone only induces limited cell death. The disappointing clinical trials of NFκB inhibitors in the treatment of GBM patients (Robe et al, 2009) indicate that GBM chemotherapy cannot be efficiently improved by targeting NFκB pathway alone.
Owing to the cross-talk between NFκB and ROS, modulating either pathway is unlikely to be sufficient for GBM cell killing. Glioblastoma multiforme (GBM) chemotherapy may be improved by simultaneously inducing ROS generation and blocking ROS-activated anti-apoptotic pathways.
We have recently demonstrated that DS/Cu modulates both ROS-JNK and ROS-NFκB pathway and enhances paclitaxel-induced apoptosis in breast cancer cell lines (Yip et al, 2011). In this study, we examined the cytotoxic effect of DS/Cu alone and in combination with dFdC on three GBM cell lines. The molecular mechanisms of DS/Cu cytotoxicity against GBM were investigated. DS and dFdC can both efficiently penetrate the BBB (Gunasekaran et al, 1983; Metro et al, 2010) and thus may be potentially used in combination for GBM chemotherapy.
Material and methods
Reagents and cell lines
U251MG, U87MG and U373MG glioblastoma cell lines were purchased from ATCC (Teddington, UK). Gemcitabine, DS, copper (II) chloride (CuCl2), N-acetyl-cysteine (NAC), SP600125, SB203580 and poly-2-hydroxyethyl methacrylate (poly-HEMA) were purchased from Sigma (Dorset, UK). Annexin V kit was from Roche Applied Sciences (Burgess Hill, UK).
1-(4,5-Dimethylthiazol-2-yl)-3,5-diphenylformazan (MTT) cytotoxicity assay and CI-isobologram analysis
The GBM cell lines were cultured in DMEM medium (Lonza, Slough, UK) supplemented with 10% foetal calf serum (Lonza), 50 units ml–1 penicillin and 50 μg ml–1 streptomycin. For in vitro cytotoxicity assays, cells were seeded and cultured overnight (10 000 per well in 96-well flat-bottomed microtiter plates), exposed to drugs for 72 h and then subjected to a standard MTT assay as previously described (Yip et al, 2011). Combination index (CI)-isobologram was used to determine the relationship between dFdC and DS/Cu activity. Cells (10 000 per well) were exposed to various concentrations of dFdC, DS/Cu or a combination of dFdC and DS/Cu. Copper was used at 1 μ M. According to our pilot study, a constant ratio of dFdC:DS=1 : 10 was used for all cell lines. The combined cytotoxicity of dFdC with DS/Cu1 μ M was determined by CI-isobologram using CalcuSyn software (Biosoft) (Chou and Talalay, 1984). Mutually exclusive equations were used to determine the CI.
Western blotting analysis
Total protein (40 μg per lane) was electrophoresed through a 10% SDS–PAGE gel and transferred to a PVDF membrane (Millipore, UK) using an electrophoretic transfer chamber (Millipore, Walford, UK). The blots were stained with primary antibodies overnight at 4 °C and then with relevant HRP conjugated secondary antibodies (1 : 5000) for 1 h at room temperature. The primary antibodies (Cell Signaling, Herts, UK: JNK, phosphorylated JNK, c-Jun, phosphorylated c-Jun, ERK, phosphorylated ERK, phosphorylated p38, cleaved PARP, cleaved caspase 3; Santa Cruz, Santa Cruz, CA, USA: Bcl2 and Bax) were diluted at 1 : 1000 in 3% BSA-TBST (phosphorylated protein) or 5% fat-free milk-TBST (non-phosphorylated protein). Anti-α-tubulin (Sigma; 1 : 8000 diluted) was used as a loading control. The signal was detected using an ECL western blotting detection kit (GeneFlow, Staffordshire, UK).
Electrophoretic mobility-shift assays (EMSA)
Nuclear protein extraction was carried out as previously described (Yip et al, 2011). A double-stranded NFκB DNA probe (5′-AGT TGA GGG GAC TTT CCC AGG C-3′) was end labelled with biotin. Detection of NFκB-oligonucleotide complex was performed using a LightShift chemiluminescent EMSA kit (Pierce, Northumberland, UK). Briefly, nuclear protein (5 μg) was incubated with 20 fmol of biotin-labelled oligonucleotide for 20 min at room temperature in binding buffer consisting of 10 mM Tris at pH 7.5, 50 mM KCl, 1 mM DTT, 2.5% glycerol, 5 mM MgCl2, 50 ng of poly(dIdC) and 0.05% nonidet P-40. The specificity of the NFκB DNA binding was determined in competition reactions in which a 200-fold molar excess of unlabelled NFkB probe or mutant NFkB probe (5′-AGT TGA TAT TAC TTT TAT AGG C-3′) was added to the binding reaction. Products of binding reactions were resolved by electrophoresis on a 6% polyacrylamide gel. NFκB-oligonucleotide complex was electroblotted onto a nylon membrane (Amersham, Little Chalfont, UK). After incubation in blocking buffer for 1 h at room temperature, the membrane was incubated with streptavidin-HRP conjugate for 30 min at room temperature. The membrane was incubated with chemiluminescent substrate for 5 min and exposed to radiographic film.
Assessment of apoptosis
Apoptotic status was determined by FITC-conjugated Annexin-V/PI assay kit (Roche) using flow cytometry following the manufacturer’s instructions. Briefly, 5 × 105 cells were seeded in T25 flasks for 24 h and treated with drugs for a further 48 h. The cells were rinsed with calcium-containing HBSS and detached using EDTA-free trypsin. The detached cells were resuspended in 100 μl binding buffer containing FITC-conjugated Annexin-V (10 mg/ml)/PI (50 mg/ml) and incubated at RT for 15 min. The cells were diluted in 400 μl of PBS and analysed by a FACScan flow cytometry (Becton Dickinson, Franklin Lakes, NJ, USA). Apoptosis and necrosis were evaluated using FL2 (PI) vs FL1 (Annexin V) plots. The cells stained with Annexin V only were classified as early apoptosis and the Annexin V and PI double-stained cells were classified as late apoptosis or necrosis.
Measurement of ROS activity
The intracellular ROS levels were determined using a Total ROS Detection Kit (Enzo, Exeter, UK) following the supplier’s instruction. Briefly, the cancer cells (2 × 105 cells per well) were cultured in six-well plate until 70% confluence. The cells were exposed to DS (U87MG: 250 nM; U251MG and U373MG: 500 nM) in combination with Cu (1 μ M). The ROS inducer (pyocyanin 200 μ M) and H2O2 (200 μ M) were used as positive control. Cells exposed to NAC (2 mM) were used as a negative control. After 1 h exposure, the drug containing medium was discarded and the cells were collected by trypsinization. The cell pellets were resuspended and incubated in 500 μl of ROS detection solution at 37 °C for 30 min in the dark. The ROS-positive population was detected using a FACSCalibur flow cytometer (BD Biosciences, San Jose, CA, USA) with 488-nm blue laser and standard FITC 530/30 nm bandpass filter.
Luciferase reporter gene assay
The effect of different treatments on the transcriptional activity of NFκB was determined by luciferase reporter gene assays. Transfections were performed using Lipofectamine transfection reagent according to the manufacturer’s instructions (Invitrogen, Paisley, UK). Cells (1 × 104 per well) were cultured in 96-well plates overnight. The luciferase reporter vectors (0.8 μg per well) (pNFκB-Tal-Luc (BD Biosciences) and pGL3-Basic (Promega, Southampton, UK)) were co-transfected with 0.008 μg per well pSV40-Renilla (Promega) DNA, an internal control for normalisation of the transcriptional activity of the reporter vectors. Forty-eight hours after transfection, the cells were lysed and luciferase activity was determined using Dual Luciferase Assay reagents (Promega) according to the manufacturer’s instructions. The luciferase activity in each well was normalised to pSV40-Renilla using Ln=L/R (Ln: normalised luciferase activity; L: luciferase activity reading; R: Renilla activity reading). The Ln was further standardized to the transcriptional activity of the pGL3-Basic using relative luciferase unit (RLU)=Ln/pGL3-basic. All transfections were performed in triplicate with at least duplicate independent experiments.
In vitro neurosphere culture
The GBM cell lines were cultured in poly-HEMA coated ultra-low adherence flasks or plates. The flasks or plates were incubated with poly-HEMA (10 mg ml−1 in ethanol) at 50 °C until dry and rinsed with PBS twice. The GBM cells were cultured in stem cell medium (SCM, serum-free DMEM-F12 supplemented with B27 and N2 serum replacement (Invitrogen), 0.3% glucose (Sigma), 10 ng ml−1 epidermal growth factor (Sigma), 10 ng ml−1 basic fibroblasts growth factor (R&D System, Abingdon, UK), 20 μg ml−1 insulin (Sigma), 2 μg ml−1 heparin (Sigma)) at a density of 10 000 cells ml−1. To determine the effect of different treatments on neurosphere-forming ability, 7–10 day cultured neurospheres were trypsinized and exposed to drugs. The drug-treated CSCs were subcultured in 30 wells of the ultra-low adherence 96-well plates (20 cells per well). After 14 days culture, colonies were counted in each well and micro-photographed.
Flow cytometric analysis of aldehyde dehydrogenase (ALDH) activity
The adherent or neurosphere cells (2.5 × 105) were stained for 30 min at 37 °C using ALDEFLUOR kit (Stem Cell Tech., Durham, NC, USA) following the manufacturer’s instructions. Diethylaminobenzaldehyde (DEAB), a specific ALDH inhibitor, treated cells were used as a negative control. The ALDH-positive population was detected using a FACSCalibur flow cytometer with 488-nm blue laser and standard FITC 530/30 nm bandpass filter.
Statistical analysis
Student’s t-test and one-way analysis of variance was used for data analysis in this study. P-values<0.05 were considered significant. All analyses were performed in SPSS V11.1 (SPSS, IBM, Armonk, NY, USA).
Results
Cytotoxicity of DS/Cu and its synergism with dFdC in GBM cell lines
Disulfiram cytotoxicity in GBM cell lines was copper-dependent. No cytotoxicity was observed when the GBM cell lines were treated either with DS or Cu alone up to concentration of 10 μ M. When used in combination with 1 μ M of copper, DS was highly cytotoxic in all GMB lines evaluated, with an IC50–72 h of 119.7 nM to 464.9 nM (Table 1). We have previously reported that DS/Cu enhances dFdC cytotoxicity and reverses dFdC chemoresistance in colon cancer cell lines (Guo et al, 2010). As shown in Table 1, the cytotoxicity of dFdC was significantly enhanced by DS/Cu (2.6 – >24-fold) in all three GBM cell lines. In combination with dFdC, the cytotoxicity of DS/Cu was enhanced although only U87MG reached statistical significance (Table 1). Combination index-isobologram analysis demonstrated a synergistic effect between DS/Cu and dFdC over a wide range of dFdC concentrations (IC50 – IC90, Table 1).
Disulfiram/copper-induced apoptosis in GBM cell lines
The apoptotic status of drug-treated GBM cell lines was examined. The cell lines were treated with DS0.5 μ M, Cu1 μ M, dFdC1 μ M, DS0.5 μ M+Cu1 μ M (DS/Cu) or DS0.5 μ M+Cu1 μ M+dFdC1 μ M (DS/Cu/dFdC) for 48 h. The apoptotic population was detected by Annexin V/PI staining and flow cytometric analysis. In comparison with the control or single agent (dFdC, DS or Cu) treated groups, a large population of apoptotic cells were detected in DS/Cu and DS/Cu/dFdC-treated cells (P<0.01, Figures 1A and B). In contrast there was no significant difference between the control and single-agent treated groups.
Disulfiram/copper-induced apoptosis in GBM cell lines. (A) Annexin V assay. The GBM cells were exposed to 0.5 μ M of disulfiram (DS), 1 μ M of CuCl2 (Cu), 1 μ M of gemcitabine (dFdC) or disulfiram plus CuCl2 (DS/Cu) and disulfiram plus CuCl2 plus gemcitabine (DS/Cu/dFdC) in combination for 48 h. The drug-treated and control cells (2 × 105) were stained with PI and Annexin V and analysed by flow cytometry. (B) The percentage of different cell populations identified by PI/Annexin V assay. **P<0.01 (Mean+s.d.; n=3); (C) The expression levels of cleaved PARP, Bax and Bcl2 protein. The expression of cleaved PARP, Bax and Bcl2 proteins were analysed by western blot in GBM cell lines exposed to 0.5 μ M of DS, 1 μ M of Cu or 0.5 μ M of DS plus 1 μ M of Cu for 48 h. Tub: α-tubulin used as a loading control. (D) The ratio of Bax/Bcl2. The band density in C was analysed by ImageJ programme. Abbreviations: Nec=necrosis; Apo=apoptosis.
PARP protein cleavage, an indicator of caspase activation, was detected in DS/Cu-treated cells (Figure 1C). Disulfiram/copper inhibited Bcl2 and induced Bax protein expression in all GBM cell lines (Figure 1C). The Bax/Bcl2 ratio was significantly increased in cells treated with DS/Cu for 48 h (Figure 1D).
Reactive oxygen species has a crucial role in DS/Cu-induced cytotoxicity
The cytotoxicity of DS is Cu dependent. As a redox metal ion, Cu triggers ROS generation (Gupte and Mumper, 2009). Therefore, ROS may be a mediator of DS/Cu-induced apoptosis. Disulfiram/copper induced ROS activity in GBM cell lines (Figures 2A and B). Both DS/Cu and H2O2 induce ROS activity, which was reversed by addition of the ROS scavenger, NAC. We examined the effect of DS/Cu-induced ROS on cytotoxicity in GBM cell lines. In line with the ROS activity change, NAC significantly reversed DS/Cu and H2O2-induced cytotoxicity. Disulfiram/copper-induced cytotoxicity was only very slightly reversed by singly blocking JNK (SP600125) and p38 (SB203580) pathway (Figure 2C).
Reactive oxygen species (ROS) activity is related to DS/Cu-induced cytotoxicity. (A, B) Disulfiram/copper induces ROS generation. The cancer cells (2 × 105 cells per well) were exposed to DS (250 nM), Cu (1 μ M), DS (250 nM) plus Cu (0.5–1 μ M) for 5–30 min. Hydrogen peroxide (100 μ M) and pyocyanin (200 μ M) were used as positive control. (A) The dot lines represent the untreated cells and the solid lines represent DS-, Cu-, DS/Cu- and pyocyanin-treated cells, respectively. In NAC-treated group, the dot and solid lines represent DS/Cu-treated cells with or without NAC reversion, respectively. (B) The ROS activity in DS/Cu and H2O2-treated cells was reversed by co-exposure to NAC (2 mM). Non-treated cells are denoted by –VE. (C) The effect of ROS and MAPK pathway inhibitors on DS/Cu-induced cytotoxicity. The cancer cells were exposed to DS (500 nM)/Cu (500 nM), DS/Cu plus NAC (2 mM), SP600125 (10 μ M) or SB203580 (10 μ M) for 72 h. The viability of drug-treated cells was determined by MTT assay. Hydrogen peroxide (100 μ M)-treated group was used as a control.
Disulfiram/copper persistently activated JNK and p38 but not the ERK pathway in GBM cell lines
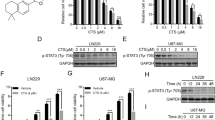
JNK and p38 pathways have key roles in ROS-induced apoptosis in some cancer cell lines (McCubrey et al, 2006). The JNK pathway was persistently activated for at least 24 h by DS/Cu and DS/Cu/dFdC in all three GBM cell lines (Figures 3A–C). Total JNK protein expression was not influenced by the drug exposure. Phosphorylation of JNK and c-Jun, which is downstream of JNK signalling, was persistently induced (up to 24 h) by DS/Cu and DS/Cu/dFdC exposure. The expression of total c-Jun protein was also induced by DS/Cu and DS/Cu/dFdC. p38 protein was also phosphorylated in GBM cell lines in response to DS/Cu and DS/Cu/dFdC (Figure 3D). In contrast to JNK, c-Jun and p38, ERK phosphorylation was detected after DS/Cu and DS/Cu/dFdC exposure (Figure 3E). Disulfiram activated JNK pathway in a copper-dependent manner. The phosphorylation of c-Jun protein was not induced by either DS or Cu alone in two GBM cell lines although moderate induction was observed in U373MG cells (Figure 3E).
Disulfiram/copper activated MAPK pathway and inhibited NFκB activity. (A–C) The GBM cells were exposed to dFdC1 μ M, DS1 μ M/Cu1 μ M or dFdC1 μ M/DS1 μ M/Cu1 μ M for 3, 6 and 24 h. The expression levels and phosphorylation status of proteins in JNK pathway were examined by western blot. (D) Disulfiram/copper activates p38 pathway. The GBM cell lines were exposed to different treatments for 24 h. The phosphorylation status of p38 was examined by western blot. (E) The effect of DS, Cu alone or DS and Cu in combination (DS/Cu) on phosphorylation status of c-Jun and ERK. To rule out the influence of trace amount of copper contained in the serum, the GBM cell lines were cultured in serum-free medium containing DS1 μ M or Cu1 μ M alone or DS1 μ M/Cu1 μ M for 24 h. The phosphorylation of c-Jun and ERK was detected by western blot. Alpha-tubulin (TUB) was used as a loading control. (F) N-acetyl-cysteine inhibited DS/Cu-induced c-Jun and p38 phosphorylation. The GBM cell lines were exposed to DS1 μ M/Cu1 μ M with or without NAC (2 mM) for 24 h. The phosphorylation status of c-Jun and p38 was examined by western blot. (G) Electrophoretic mobility-shift assay analysis of NFκB DNA binding activity. Nu: western blot of nucleolin was used as a protein loading control. (H) Examination of NFκB transcriptional activity by luciferase reporter gene assay. The GBM cell lines were exposed to dFdC1 μ M, DS1 μ M/Cu1 μ M or dFdC1 μ M/DS1 μ M/Cu1 μ M for 24 h before subjected to EMSA and luciferase reporter gene assay.
To investigate ROS-dependent activation of JNK and p38 pathways, the GBM cell lines were exposed to DS/Cu with or without addition of NAC. Disulfiram/copper-induced c-Jun and p38 phosphorylation was blocked by inhibition of ROS (Figure 3F) demonstrating that activation of JNK and p38 pathways by DS/Cu is ROS dependent.
Disulfiram/copper and DS/Cu/dFdC inhibits NFκB activity in GBM cell lines
In addition to MAPK pathways, ROS is also a very strong activator of the NFκB pathway, which, in most circumstances, possesses anti-apoptotic activity and neutralises ROS-induced apoptotic effects (Nakano et al, 2006). Therefore, we examined NFκB activity in drug-treated GBM cell lines. NFκB DNA binding (Figure 3G) and transcriptional (Figure 3H) activity was induced by dFdC treatment. Both dFdC-induced and constitutive NFκB DNA binding and transcriptional activities were significantly inhibited by DS/Cu.
Disulfiram/copper inhibits ALDH activity in neurosphere population and blocks neurosphere formation
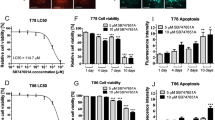
Our previous studies demonstrated that DS/Cu reverses chemoresistance to agents with different resistant mechanisms (Wang et al, 2003, 2004; Guo et al, 2010; Yip et al, 2011). It is widely accepted that CSCs are resistant to a wide range of classical cytotoxic anticancer drugs. Disulfiram is a specific inhibitor of ALDH, a functional marker of CSCs. In this study we examined the effect of DS/Cu on GBM stem-like cells in U251MG and U87MG cell lines. Both cell lines formed neurospheres when cultured in CSC medium (Figure 4A). After only 3 h exposure to DS0.5 μ M/Cu1 μ M or DS0.5 μ M/Cu1 μ M/dFdC1 μ M, the neurosphere-forming ability of GBM cell lines was completely abolished. In contrast the neurosphere-forming ability in both cell lines was not affected by exposure to DS or Cu alone. The neurosphere number in dFdC-treated cells was slightly lower than that of the control group but the difference was not statistically significant (Table 2).
The effect of DS/Cu on stem-like status in GBM cell lines. (A) Disulfiram/copper and DS/Cu/dFdC blocked neurosphere-forming ability in GBM cell lines. The GBM cells formed neurospheres after 7 days culture in SCM. The neurosphere cells were separated by tripsinization and exposed to DS0.5 μ M, Cu1 μ M, dFdC1 μ M alone or DS0.5 μ M/Cu1 μ M and DS0.5 μ M/Cu1 μ M/dFdC1 μ M for 3 h. The drug-treated cells were cultured at a cell density of 20 cells per well in 30 wells of ultra-low attachment 96-well plates containing drug-free SCM for 14 days. The neurospheres were photographed at × 40 magnificaiton. (B) Disulfiram/copper and DS/Cu/dFdC abolished ALDH-positive population in neurospheres. The neurosphere cells were treated as those in (A). The ALDH-positive cells were determined by ALDEFLUOR staining and flow cytometer analysis. (C) Aldehyde dehydrogenase activity in neurosphere cells were not directly inhibited by DS/Cu. Diethylaminobenzaldehyde (DEAB, 30 μ M), DS (0.5 μ M) and DS (0.5 μ M) plus Cu (1 μ M) were added into the ALDH staining tubes and incubated at 37 °C for 30 min. The ALDH activity in the cells was detected by flow cytometer. The inserted numbers represent percentage of the positive cells (mean (s.d.), n=3). **P<0.01 (in comparison with NS−VE), ¶P<0.01 (in comparison with other groups). Abbreviation: NS=neurosphere.
The effect of different treatments on the ALDH-positive population in neurospheres was examined. Figure 4B shows that in comparison with attached cells, a significantly higher percentage of ALDH-positive cells were detected in neurospheres. After 3 h DS/Cu or DS/Cu/dFdC exposure followed by 16 h culture in drug-free medium the ALDH-positive population was abolished in both cell lines. Inhibition of ALDH by DS was Cu dependent. Disulfiram or Cu alone did not demonstrate any inhibitory effect on ALDH-positive neurosphere cells. Gemcitabine had no effect on ALDH-positive neurosphere cells. Furthermore, we examined if DS or DS/Cu directly inhibits ALDH activity in GBM cells when added into the ALDEFLUOR reaction. The ALDH activity in the non-treated U251MG neurosphere cells was measured by ALDEFUOR assay with indicated additives in the reaction tubes. As shown in Figure 4C, ALDH activity in U251MG neurosphere cells was inhibited by diethylaminobenzaldehyde (DEAB), a specific ALDH inhibitor, but not by DS or DS/Cu.
Discussion
The diffuse infiltration of GBM in the brain makes complete removal of GBM by surgery impossible. Chemotherapy remains the main option for elimination of residual GBM cells. Because of de novo chemoresistance of GBM cells and problems with drug bioavailability, the outcomes of GBM chemotherapy are still very poor (Reardon et al, 2006). Therefore, identification of drugs that efficiently pass through the BBB and synergistically enhance the cytotoxicity of conventional anti-GBM drugs is needed to improve the therapeutic outcomes of GBM. Development of novel agents is a time- and cash-consuming procedure (DiMasi et al, 2003). Any newly identified application for an existing drug would facilitate rapid evaluation in phase II clinical trials because of extensive existing data on the pharmacokinetics and safety profiles of these agents in humans (Chong and Sullivan, 2007). This study is aiming to investigate the anti-GBM activity of DS, a clinically used anti-alcoholism drug with extensive pre-clinical and clinical data (Eneanya et al, 1981; Johansson, 1992). Previous studies demonstrate that DS is highly cytotoxic to a wide range of cancer cell lines in vitro and in vivo (Wang et al, 2003; Cen et al, 2004; Wang et al, 2004; Chen et al, 2006; Iljin et al, 2009; Guo et al, 2010; Yip et al, 2011). Disulfiram can penetrate the BBB with very low systemic toxicity. Therefore, investigation of its anti-GBM effect may lead to its relatively rapid translation into GBM therapeutics.
This study indicates that Cu is essential for DS-induced cytotoxicity in GBM cell lines. The potential explanation of Cu-induced cellular toxicity is that Cu ions participate in the formation of ROS. Copper induces ROS generation and cytotoxicity in breast cancer and melanoma cell lines (Cen et al, 2002; Yip et al, 2011). Copper exits in the cell as cupric [Cu(I)] and cuprous [Cu(II)]. Both forms of Cu can participate in oxidation and reduction reactions. Copper induces the generation of hydroxyl radicals (OH) from hydrogen peroxide (H2O2). The hydroxyl radical is the most powerful oxidising radical as it is theoretically capable of reacting with every biological molecule and thus initiates oxidative damage. Our results indicate that the cytotoxicity of DS/Cu in GBM cells is ROS-related. Disulfiram/copper-induced ROS activity and cytotoxicity was reversed by ROS inhibition. Copper alone was not cytotoxic to GBM cells. The transport of Cu into cells is regulated by the copper transporter, Ctr1. In order to maintain redox homoeostasis, intracellular Cu levels are strictly controlled (Kim et al, 2008). As a strong bivalent metal ion chelator, DS and its derivative, N,N-diethyldithiocarbamate (deDTC), can form a complex [Cu(deDTC)2] with copper. This DS/Cu complex can transport Cu into cancer cells in a Ctr1-independent manner, (Cen et al, 2004) thus overcoming the transporter controlled regulation of intracellular Cu homoeostasis. Selectivity of anticancer drug is vital for GBM chemotherapy as brain is a highly vulnerable organ. Most cancer tissues contain higher levels of Cu, which leads to higher ROS activity in cancer cells than normal tissues (Margalioth et al, 1983). Glioblastoma multiforme tissue also possesses a significantly higher Cu load (>4-fold) than the surrounding brain tissues (Yoshida et al, 1993). Therefore, intracellular transport of Cu may push the ROS generation in the GBM cells over their tolerable levels but spare normal cells.
Gemcitabine has been successfully used in the treatment of a wide range of malignancies. Its success in GBM chemotherapy has been markedly limited by de novo chemoresistance of GBM cells (Gertler et al, 2000). We have previously demonstrated that DS/Cu sensitises cancer cells to dFdC and reverses dFdC resistance in other types of cancer (Guo et al, 2010). In this study the sensitising effect of DS/Cu on dFdC in GBM cell lines was examined. Our results demonstrate that DS/Cu enhances the cytotoxicity of dFdC in GBM cell lines. Combination index-isobologram indicates a synergistic effect between DS/Cu and dFdC. Both dFdC and DS can traverse the BBB and get into GBM tissue. The synergistic effect between DS/Cu and dFdC may help to overcome de novo dFdC resistance in GBM cells and be beneficial for dFdC-based chemotherapy in GBM patients.
Our data demonstrate that ROS may have a key role in DS/Cu-induced cytotoxicity and apoptosis in GBM cells. There has been a long history of using ROS inducers to tackle cancer with little success. One of the principal reasons is that apart from activation of pro-apoptotic pathways, ROS also trigger the expression of anti-apoptotic proteins, which neutralise the pro-apoptotic effects of ROS (Gloire et al, 2006). Our results demonstrate that DS/Cu complex but not DS or Cu alone persistently activated JNK and p38 MAPK pathways that promote ROS-induced apoptosis (Junttila et al, 2008) in GBM cell lines. Inhibition of ROS inhibited DS/Cu-induced JNK and p38 MAPK pathway activation and reversed DS/Cu-induced cytotoxicity in GBM cell lines. In contrast, DS/Cu did not activate the ERK pathway, which has essential roles in cell growth, proliferation and survival downstream of ROS (Junttila et al, 2008). Pro-apoptotic Bax was induced and anti-apoptotic Bcl2 was inhibited by DS/Cu leading to an increased Bax/Bcl2 ratio and thus a pro-apoptotic phenotype in response to ROS. These results indicate that DS/Cu may trigger intrinsic apoptosis via persistent activation of JNK and p38 pathways that is ROS dependent.
Nuclear factor-kappa B is one of the most important ROS-induced transcription factors (Gloire et al, 2006). Nuclear factor-kappa B inhibits JNK and p38 activation by suppressing ROS accumulation in cancer cells (Gloire et al, 2006; Nakano et al, 2006). Cancer cell fate is highly dependent on the cross-talk between JNK/p38 and NFκB pathways. High constitutive and dFdC-induced NFκB activity was detected in the GBM cell lines. The NFκB activity in GBM cell lines was significantly inhibited by DS/Cu. Simultaneous activation of ROS-JNK/p38 and inhibition of NFκB pathways may contribute to DS/Cu-induced cytotoxicity in the GBM cell lines.
It has been suggested that GBM contain a small population of CSCs (Vescovi et al, 2006), which are highly radio- and chemo-resistant and have been proposed to be responsible for cancer recurrence. Targeting CSCs may improve patient outcomes after chemotherapy. In recent years ALDH has been recognised as a CSC marker in a number of solid tumours. The function of ALDH in CSCs is still largely unknown. Abundant ALDH in mammalian cornea cells protects these cells from oxidative stress-induced damage (Estey et al, 2007). High ALDH activity promotes survival of human muscle stem-like cells (Jean et al, 2011). Overexpression of ALDH induces resistance to different kinds of anticancer drugs with various resistant mechanisms (Pappa et al, 2005; Moreb et al, 2008; Landen et al, 2010). In comparison with their normal counterparts, the CSCs possess significantly lower levels of ROS activity (Diehn et al, 2009; Ye et al, 2011). Aldehyde dehydrogenase is involved in detoxification of a wide range of aliphatic/aromatic aldehyde and other reactive radicals. High ALDH activity may be at least partially responsible for maintaining the lower intracellular ROS activity in CSCs and protect CSCs from ROS-induced DNA, lipid and protein damage.
In recent years accumulating evidence indicates that ALDH may not only be a surrogate marker but also a functional target for anti-CSC chemotherapy. Knocking down ALDH genes inhibits the growth of ovarian, breast, lung cancer and leukaemia cell lines and sensitises CSCs to conventional anticancer drugs (Moreb et al, 2008, 2011; Landen et al, 2010; Croker and Allan, 2011). Aldehyde dehydrogenase is a superfamily containing 19 functional isoenzymes. Because of the overlap of the substrates of different ALDH isoenzymes currently available detecting methods are not specific for any individual isoenzyme. ALDH1A1 was the first indicated stem cell marker. Recent studies manifested that high expression of other ALDH isoenzymes (1A2, 1A3, 1A7, 2*2, 3A1, 4A1, 5A1, 6A1 and 9A1) was also detected in stem cells (Muzio et al, 2012). The subtype of ALDH isoenzymes expressed in CSCs may be cancer type-dependent. Several ALDH isoenzymes may also be co-expressed in the same cancer and have redundant functions (Moreb et al, 2011). Therefore, targeting individual ALDH isoenzyme may not be an efficient approach to eliminate the CSC population within a cancer mass. As a pan-ALDH inhibitor, we propose that DS/Cu may induce intracellular ROS activity in CSC, which typically have lower ROS levels than their normal counterparts, and intensify ROS triggered CSC apoptotic cell death by simultaneous inhibition of various ALDH isoenzymes and subsequent loss of ALDH-mediated protection against oxidative stress. Neurosphere-forming ability, a the major characteristic of GBM CSC (Singh et al, 2004), was completely abolished after only 3 h exposure to DS/Cu.
Although DS is widely reported as an ALDH inhibitor, in our study DS alone did not show any inhibitory effect on ALDH activity in cell culture or in the ALDEFLUOR assay. These discrepant findings may be due to the different DS concentrations used. The IC50 concentration of DS for ALDH activity is over 36 μ M (Lipsky et al, 2001). A significantly lower concentration (500 nM) of DS was used in this study for our evaluation of GBM cytotoxity. Disulfiram/copper strongly inhibited ALDH activity in cultured GBM neurospheres. Although DS/Cu inhibited ALDH activity in cell culture, no ALDH inhibition was observed when DS/Cu was added directly into the ALDEFLUOR reaction. It has been reported that methylated DS derivatives are the functional inhibitors of ALDH (Veverka et al, 1997). Therefore, DS may inhibit ALDH activity in GBM CSC indirectly downstream of intracellular metabolism.
Our study indicates that DS/Cu alone or in combination with dFdC may be a successful therapeutic for chemoresistant GBM by successfully targeting chemoresistant CSC via ROS generation and attenuation of ALDH-mediated protection from oxidative damage.
Change history
11 October 2012
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Barceloux DG (1999) Copper. J Toxicol Clin Toxicol 37: 217–230
Bergman AM, Pinedo HM, Peters GJ (2002) Determinants of resistance to 2',2'-difluorodeoxycytidine (gemcitabine). Drug Resist Updat 5: 19–33
Bodenner DL, Dedon PC, Keng PC, Katz JC, Borch RF (1986) Selective protection against cis-diamminedichloroplatinum(II)-induced toxicity in kidney, gut, and bone marrow by diethyldithiocarbamate. Cancer Res 46: 2751–2755
Burkitt MJ, Bishop HS, Milne L, Tsang SY, Provan GJ, Nobel CS, Orrenius S, Slater AF (1998) Dithiocarbamate toxicity toward thymocytes involves their copper-catalyzed conversion to thiuram disulfides, which oxidize glutathione in a redox cycle without the release of reactive oxygen species. Arch Biochem Biophys 353: 73–84
Cen D, Brayton D, Shahandeh B, Meyskens FL, Farmer PJ (2004) Disulfiram facilitates intracellular Cu uptake and induces apoptosis in human melanoma cells. J Med Chem 47: 6914–6920
Cen D, Gonzalez RI, Buckmeier JA, Kahlon RS, Tohidian NB, Meyskens FL (2002) Disulfiram induces apoptosis in human melanoma cells: a redox-related process. Mol Cancer Ther 1: 197–204
Chen D, Cui QC, Yang H, Dou QP (2006) Disulfiram, a clinically used anti-alcoholism drug and copper-binding agent, induces apoptotic cell death in breast cancer cultures and xenografts via inhibition of the proteasome activity. Cancer Res 66: 10425–10433
Chong CR, Sullivan DJ (2007) New uses for old drugs. Nature 448: 645–646
Chou TC, Talalay P (1984) Quantitative analysis of dose-effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv Enzyme Regul 22: 27–55
Conticello C, Martinetti D, Adamo L, Buccheri S, Giuffrida R, Parrinello N, Lombardo L, Anastasi G, Amato G, Cavalli M, Chiarenza A, De Maria R, Giustolisi R, Gulisano M, Di Raimondo F (2012) Disulfiram, an old drug with new potential therapeutic uses for human haematological malignancies. Int J Cancer 131: 2197–2203
Croker AK, Allan AL (2011) Inhibition of aldehyde dehydrogenase (ALDH) activity reduces chemotherapy and radiation resistance of stem-like ALDH(hi)CD44 (+) human breast cancer cells. Breast Cancer Res Treat 133: 75–87
Diehn M, Cho RW, Lobo NA, Kalisky T, Dorie MJ, Kulp AN, Qian D, Lam JS, Ailles LE, Wong M, Joshua B, Kaplan MJ, Wapnir I, Dirbas FM, Somlo G, Garberoglio C, Paz B, Shen J, Lau SK, Quake SR, Brown JM, Weissman IL, Clarke MF (2009) Association of reactive oxygen species levels and radioresistance in cancer stem cells. Nature 458: 780–783
DiMasi JA, Hansen RW, Grabowski HG (2003) The price of innovation: new estimates of drug development costs. J Health Econ 22: 151–185
Eneanya DI, Bianchine JR, Duran DO, Andresen BD (1981) The actions of metabolic fate of disulfiram. Annu Rev Pharmacol Toxicol 21: 575–596
Estey T, Piatigorsky J, Lassen N, Vasiliou V (2007) ALDH3A1: a corneal crystallin with diverse functions. Exp Eye Res 84: 3–12
Fruehauf JP, Meyskens FL (2007) Reactive oxygen species: a breath of life or death? Clin Cancer Res 13: 789–794
Gertler SZ, MacDonald D, Goodyear M, Forsyth P, Stewart DJ, Belanger K, Perry J, Fulton D, Steward W, Wainman N, Seymour L (2000) NCIC-CTG phase II study of gemcitabine in patients with malignant glioma (IND.94). Ann Oncol 11: 315–318
Gloire G, Legrand-Poels S, Piette J (2006) NF-kappaB activation by reactive oxygen species: fifteen years later. Biochem Pharmacol 72: 1493–1505
Gunasekaran S, Weinstein P, Anderson G, Parker D, Misiorowski RL, Chvapil M (1983) Distribution of disulfiram in brain after carotid ligation in gerbils. Neuropharmacology 22: 1159–1163
Guo X, Xu B, Pandey S, Goessl E, Brown J, Armesilla AL, Darling JL, Wang W (2010) Disulfiram/copper complex inhibiting NFkappaB activity and potentiating cytotoxic effect of gemcitabine on colon and breast cancer cell lines. Cancer Lett 291: 104–113
Gupte A, Mumper RJ (2009) Elevated copper and oxidative stress in cancer cells as a target for cancer treatment. Cancer Treat Rev 35: 32–46
Hacker MP, Ershler WB, Newman RA, Gamelli RL (1982) Effect of disulfiram (tetraethylthiuram disulfide) amd diethyldithiocarbamate on the bladder toxicity and antitumor activity of cyclophosphamide in mice. Cancer Res 42: 4490–4494
Hieger I (1926) The effect of copper compounds upon the growth of carcinoma in the rat. Biochem J 20: 232–236
Iljin K, Ketola K, Vainio P, Halonen P, Kohonen P, Fey V, Grafstrom RC, Perala M, Kallioniemi O (2009) High-throughput cell-based screening of 4910 known drugs and drug-like small molecules identifies disulfiram as an inhibitor of prostate cancer cell growth. Clin Cancer Res 15: 6070–6078
Jean E, Laoudj-Chenivesse D, Notarnicola C, Rouger K, Serratrice N, Bonnieu A, Gay S, Bacou F, Duret C, Carnac G (2011) Aldehyde dehydrogenase activity promotes survival of human muscle precursor cells. J Cell Mol Med 15: 119–133
Johansson B (1992) A review of the pharmacokinetics and pharmacodynamics of disulfiram and its metabolites. Acta Psychiatr Scand Suppl 369: 15–26
Junttila MR, Li SP, Westermarck J (2008) Phosphatase-mediated crosstalk between MAPK signaling pathways in the regulation of cell survival. FASEB J 22: 954–965
Kim BE, Nevitt T, Thiele DJ (2008) Mechanisms for copper acquisition, distribution and regulation. Nat Chem Biol 4: 176–185
Landen CN, Goodman B, Katre AA, Steg AD, Nick AM, Stone RL, Miller LD, Mejia PV, Jennings NB, Gershenson DM, Bast RC, Coleman RL, Lopez-Berestein G, Sood AK (2010) Targeting aldehyde dehydrogenase cancer stem cells in ovarian cancer. Mol Cancer Ther 9: 3186–3199
Lipsky JJ, Shen ML, Naylor S (2001) Overview – in vitro inhibition of aldehyde dehydrogenase by disulfiram and metabolites. Chem Biol Interact 130-132: 81–91
Lopez-Lazaro M (2007) Dual role of hydrogen peroxide in cancer: possible relevance to cancer chemoprevention and therapy. Cancer Lett 252: 1–8
Margalioth EJ, Schenker JG, Chevion M (1983) Copper and zinc levels in normal and malignant tissues. Cancer 52: 868–872
McCubrey JA, Lahair MM, Franklin RA (2006) Reactive oxygen species-induced activation of the MAP kinase signaling pathways. Antioxid Redox Signal 8: 1775–1789
Metro G, Fabi A, Mirri MA, Vidiri A, Pace A, Carosi M, Russillo M, Maschio M, Giannarelli D, Pellegrini D, Pompili A, Cognetti F, Carapella CM (2010) Phase II study of fixed dose rate gemcitabine as radiosensitizer for newly diagnosed glioblastoma multiforme. Cancer Chemother Pharmacol 65: 391–397
Moreb JS, Baker HV, Chang LJ, Amaya M, Lopez MC, Ostmark B, Chou W (2008) ALDH isozymes downregulation affects cell growth, cell motility and gene expression in lung cancer cells. Mol Cancer 7: 87
Moreb JS, Ucar D, Han S, Amory JK, Goldstein AS, Ostmark B, Chang LJ (2011) The enzymatic activity of human aldehyde dehydrogenases 1A2 and 2 (ALDH1A2 and ALDH2) is detected by Aldefluor, inhibited by diethylaminobenzaldehyde and has significant effects on cell proliferation and drug resistance. Chem Biol Interact 195: 52–60
Muzio G, Maggiora M, Paiuzzi E, Oraldi M, Canuto RA (2012) Aldehyde dehydrogenases and cell proliferation. Free Radic Biol Med 52: 735–746
Nakano H, Nakajima A, Sakon-Komazawa S, Piao JH, Xue X, Okumura K (2006) Reactive oxygen species mediate crosstalk between NF-kappaB and JNK. Cell Death Differ 13: 730–737
Pappa A, Brown D, Koutalos Y, DeGregori J, White C, Vasiliou V (2005) Human aldehyde dehydrogenase 3A1 inhibits proliferation and promotes survival of human corneal epithelial cells. J Biol Chem 280: 27998–28006
Rayet B, Gelinas C (1999) Aberrant rel/nfkb genes and activity in human cancer. Oncogene 18: 6938–6947
Reardon DA, Rich JN, Friedman HS, Bigner DD (2006) Recent advances in the treatment of malignant astrocytoma. J Clin Oncol 24: 1253–1265
Robe PA, Martin DH, Nguyen-Khac MT, Artesi M, Deprez M, Albert A, Vanbelle S, Califice S, Bredel M, Bours V (2009) Early termination of ISRCTN45828668, a phase 1/2 prospective, randomized study of sulfasalazine for the treatment of progressing malignant gliomas in adults. BMC Cancer 9: 372
Singh SK, Hawkins C, Clarke ID, Squire JA, Bayani J, Hide T, Henkelman RM, Cusimano MD, Dirks PB (2004) Identification of human brain tumour initiating cells. Nature 432: 396–401
Vescovi AL, Galli R, Reynolds BA (2006) Brain tumour stem cells. Nat Rev Cancer 6: 425–436
Veverka KA, Johnson KL, Mays DC, Lipsky JJ, Naylor S (1997) Inhibition of aldehyde dehydrogenase by disulfiram and its metabolite methyl diethylthiocarbamoyl-sulfoxide. Biochem Pharmacol 53: 511–518
Wang W, Cassidy J, O’Brien V, Ryan KM, Collie-Duguid E (2004) Mechanistic and predictive profiling of 5-Fluorouracil resistance in human cancer cells. Cancer Res 64: 8167–8176
Wang W, McLeod HL, Cassidy J (2003) Disulfiram-mediated inhibition of NF-kappaB activity enhances cytotoxicity of 5-fluorouracil in human colorectal cancer cell lines. Int J Cancer 104: 504–511
Ye XQ, Li Q, Wang GH, Sun FF, Huang GJ, Bian XW, Yu SC, Qian GS (2011) Mitochondrial and energy metabolism-related properties as novel indicators of lung cancer stem cells. Int J Cancer 129: 820–831
Yip NC, Fombon IS, Liu P, Brown S, Kannappan V, Armesilla AL, Xu B, Cassidy J, Darling JL, Wang W (2011) Disulfiram modulated ROS-MAPK and NFkB pathways and targeted breast cancer cells with cancer stem cell like properties. Br J Cancer 104: 1564–1574
Yoshida D, Ikeda Y, Nakazawa S (1993) Quantitative analysis of copper, zinc and copper/zinc ratio in selected human brain tumours. J Neurooncol 16: 109–115
Acknowledgements
We thank Dr E Collie-Duguid for her very helpful discussions and critical reading of this manuscript. This work is funded by Brain Tumour Charity (6025835), UK.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Liu, P., Brown, S., Goktug, T. et al. Cytotoxic effect of disulfiram/copper on human glioblastoma cell lines and ALDH-positive cancer-stem-like cells. Br J Cancer 107, 1488–1497 (2012). https://doi.org/10.1038/bjc.2012.442
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2012.442
Keywords
This article is cited by
-
NPLOC4 is a potential target and a poor prognostic signature in lung squamous cell carcinoma
Scientific Reports (2023)
-
The immunomodulatory function and antitumor effect of disulfiram: paving the way for novel cancer therapeutics
Discover Oncology (2023)
-
DSF/Cu induces antitumor effect against diffuse large B-cell lymphoma through suppressing NF-κB/BCL6 pathways
Cancer Cell International (2022)
-
Disulfiram inhibits liver fibrosis in rats by suppressing hepatic stellate cell activation and viability
BMC Pharmacology and Toxicology (2022)
-
Copper homeostasis and cuproptosis in health and disease
Signal Transduction and Targeted Therapy (2022)