Abstract
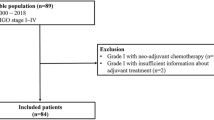
Survival and prognostic factors were analysed in 150 patients with histologically confirmed epithelial ovarian cancer stage IA-IIA. The relapse-free and overall survival rates were, respectively, 81% and 88% after 3 and 74% and 84% after 5 years. The analysis of various prognostic factors indicates as the main factor the grade differentiation of the tumour.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Villa, A., Parazzini, F., Acerboni, S. et al. Survival and prognostic factors of early ovarian cancer. Br J Cancer 77, 123–124 (1998). https://doi.org/10.1038/bjc.1998.19
Issue Date:
DOI: https://doi.org/10.1038/bjc.1998.19