Abstract
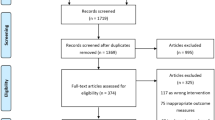
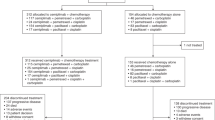
A total of 458 eligible patients, from 21 centres, with microscopically confirmed SCLC were allocated at random to three chemotherapy regimens, each given at 3-week intervals. In two regimens, etoposide, cyclophosphamide, methotrexate and vincristine were given for a total of either three courses (ECMV3) or six courses (ECMV6). In the third regimen, etoposide and ifosfamide were given for six courses (E16). Patients with limited disease also received radiotherapy to the primary site after the third course of chemotherapy in all three groups. As reported by clinicians, 59% of the ECMV3, 67% of the ECMV6 and 63% of the EI6 patients experienced moderate or severe adverse reactions to their chemotherapy. The major symptoms of disease, cough, haemoptysis, chest pain, anorexia, and dysphagia, were palliated in 63% or more of patients and the median duration of palliation was 63% or more of survival, the results being similar in the three groups. Among patients with poor overall condition, physical activity and breathlessness on admission, the proportions who improved were higher in the EI6 group but the differences were small. In all three groups, levels of anxiety fell substantially during treatment. Levels of depression were lower and showed little change. As assessed by patients using a daily diary card, the patterns of nausea, vomiting, activity and mood, associated with courses of chemotherapy were very similar in the three groups. In the EI6 group there was less dysphagia and better overall condition between courses, but these advantages need to be weighed against the inconvenience of the 24-h infusions required, compared with the 30-min infusions of the other two regimens. As reported in the companion paper (MRC Lung Cancer Working Party, 1993a) there was no statistically significant survival advantage to any of the three regimens, although the results do not exclude the possibility of a minor survival advantage with the two six-course regimens. In conclusion, there was no major clinical gain from continuing chemotherapy beyond three courses or from using the ifosfamide regimen.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Consortia
Rights and permissions
About this article
Cite this article
Bleehen, N., Girling, D., Machin, D. et al. A randomised trial of three or six courses of etoposide cyclophosphamide methotrexate and vincristine or six courses of etoposide and ifosfamide in small cell lung cancer (SCLC). II: Quality of life. Br J Cancer 68, 1157–1166 (1993). https://doi.org/10.1038/bjc.1993.497
Issue Date:
DOI: https://doi.org/10.1038/bjc.1993.497
This article is cited by
-
Defining and analysing symptom palliation in cancer clinical trials: a deceptively difficult exercise
British Journal of Cancer (1999)
-
Evaluation of quality of life for diverse patient populations
Breast Cancer Research and Treatment (1996)
-
MRC quality of life studies using a daily diary card—practical lessons learned from cancer trials
Quality of Life Research (1995)
-
Approaches to the analysis of quality of life data: experiences gained from a Medical Research Council Lung Cancer Working Party palliative chemotherapy trial
Quality of Life Research (1994)