Abstract
The BCR/ABL tyrosine kinase promotes leukemogenesis through activation of several targets that include the phosphoinositide 3-kinase (PI3K). Tyrosine kinase inhibitors (TKIs), which target BCR/ABL, induce striking clinical responses. However, therapy with TKIs is associated with limitations such as drug intolerance, inability to universally eradicate the disease and emergence of BCR/ABL drug-resistant mutants. To overcome these limitations, we tested whether inhibition of the PI3K/target of rapamycin (mTOR) signaling pathway has antileukemic effect in primary hematopoietic stem cells and BA/F3 cells expressing the BCR/ABL oncoprotein. We determined that dual inhibition of PI3K/mTOR causes growth arrest and apoptosis leading to profound antileukemic effects both in vitro and in vivo. We also established that pharmacologic inhibition of the mTORC1/mTORC2 complexes is sufficient to cause these antileukemic effects. Our results support the development of inhibitors of the mTORC1/2 complexes for the therapy of leukemias that either express BCR/ABL or display deregulation of the PI3K/mTOR signaling pathway.
Similar content being viewed by others
Introduction
BCR/ABL is a constitutively active tyrosine kinase that promotes leukemogenesis. Imatinib and other tyrosine-kinase inhibitors (TKI) induce complete remissions in the vast majority of patients with chronic myelogenous leukemia (CML) and exert significant antileukemic effects in patients with acute lymphoblastic leukemia (ALL) expressing the BCR/ABL oncoprotein. However, even though TKI therapy achieves long-term control of CML in the majority of patients, it is believed that TKI therapy is not sufficient to eradicate leukemia. Moreover, therapy with TKIs is associated with limitations such as drug intolerance and the emergence of BCR/ABL drug-resistant mutants. In this regard, a common cause of TKI resistance is due to point mutations in the BCR/ABL kinase domain that preclude or hamper TKI binding. Second generation TKI can overcome certain TKI-resistant mutations except for the pan-resistant T315I.1, 2 These shortcomings provide the rationale to develop improved therapies for CML and ALL.
BCR/ABL promotes leukemogenesis through activation of several oncogenic signaling pathways that include the phosphoinositide 3-kinase (PI3K)/AKT/mammalian target of rapamycin (mTOR) signaling pathway.1, 3 The mTOR kinase is found in two distinct complexes: mTORC1 and mTORC2. The S6 kinase and the eukaryotic-initiation-factor 4E-binding protein-1 are substrates of mTORC1, whereas AKT is a substrate of mTORC2.4 The PI3K/AKT/mTOR signaling axis is a pivotal regulator of leukemogenesis and of solid tumorigenesis.5, 6, 7 As a result, the PI3K/AKT/mTOR signaling pathway is a prime target for drug development.8, 9
Rapamycin and its derivatives (rapalogs) are allosteric inhibitors of mTORC1. These drugs are potent immunosuppressors, but they have demonstrated limited anticancer activity in patients.10, 11 This is most likely due to the fact that rapamycin and RAD001 inhibit only one of the several downstream targets of PI3K leaving AKT unaffected. Moreover, they also disrupt a feedback mechanism that dampens PI3K activity leading to a compensatory upregulation of AKT activity, causing counterproductive prosurvival effects.11, 12 On the contrary, ATP-competitive dual PI3K/mTORC1/2 and mTORC1/2 inhibitors display potent anticancer properties both in vitro and in vivo in a wide range of malignant cells including leukemia. Several of these compounds are being tested in preclinical models.8, 9, 13, 14, 15, 16 Thus, we tested the antileukemic effects of PI3K signaling pathway inhibitors in primary murine CML samples and in BA/F3 cells, a murine pro-B cell line that recapitulates the effects of wild-type and TKI-resistant BCR/ABL in leukemic disease.
Materials and methods
Cell studies
BA/F3 cells expressing empty vector (control), BCR/ABL wild-type or imatinib-resistant mutations (BCR/ABL E255K and T315I) were a kind gift of Dr Brian Druker (Oregon Health Science University, Portland, OR, USA) and maintained as described.17 Growth curves were performed in triplicate and the cell number was determined after 72 h. Primary bone marrow cells were isolated from healthy or CML leukemic adult C57/B6 mice. To generate CML mice, we isolated E15.5 fetal liver Lin− cells by AutoMACS (Auburn, CA, USA) and performed spin inoculation with MSCV-BCR/ABL-IRES-GFP retroviral supernatant in a medium containing 10% fetal bovine serum, 20 ng/ml stem cell factor, 20 ng/ml interleukin-3 and 10 ng/ml interleukin-6 with 5 μg/ml polybrene. Infected cells were then transplanted into lethally irradiated (1000 rad) C57BL/6 mice by retro-orbital injection. Primary murine bone marrow colonies were grown in MethoCult GM (Stem cell Technologies, Vancouver, BC, Canada) supplemented with the indicated drug dosage in duplicate and counted after 7 days in culture.
Inhibitors
BEZ235, KU-0063794 and GDC0941 were from Chemdea (Ridgewood, NJ, USA);18, 19, 20 rapamycin was from Invitrogen (Carlsbad, CA, USA). AZD8055 and ARRY142886 were from Chemitek (Indianapolis, IN, USA).21, 22 Inhibitors were added to mid-log-phase cell cultures at the indicated concentrations. The concentration for rapamycin was 100 nM. Control cells were incubated with a medium containing a solvent (dimethyl sulfoxide) at a concentration corresponding to the highest dose used in inhibitor-treated cells. For western blot analysis, cells were incubated with the inhibitor for 48 h. In vivo, BEZ235 was administered by gavage daily in N-methyl-2-pyrrolidone (NMP)/PEG300 (10:90, v/v), control mice received PEG300 containing 10% NMP.18
Determination of apoptosis
Cell cycle analysis and determination of apoptosis by propidium iodide staining were done following a standard procedure with a FC500 Beckman Coulter flow cytometer (Brea, CA, USA) using the WinMDI V2.8. software (Purdue University Cytometry Laboratories, West Lafayette, IN, USA).23, 24 We assessed apoptosis also by determining caspase activity (Promega Caspase-Glo 3/7 assay, Madison, WI, USA). Following the manufacturer's protocol, we measured relative luminescence as a ratio between treated and untreated cells. The ratio was calculated as follows: luminescence was measured and subtracted from a background control. Values were normalized to the number of cells in each well. The ratio was calculated between treated and untreated sample. We used, staurosporine, a well-known inducer of apoptosis, as a positive control at the indicated concentrations and time points.
For determination of apoptosis in vivo, we used the Tunel assay ApopTag Plus Peroxidase in situ Apoptosis Detection Kit (Millipore, Billerica, MA, USA). Bright field images of spleen sections were taken with a Leica Inverted Microscope DMI6000 at a magnification of × 200.
Immunoblotting and immunohistochemistry
Western blotting and immunohistochemical studies were done as described previously.24 The following antibodies were obtained from Cell Signaling Technologies (Danvers, MA, USA): AKT, Ser473 phospho-AKT, Ser235/236 phospho-S6, S6, phospho-ERK, ERK, 4-EBP1 and phospho-4EBP1. Tubulin and HSP-90 were from Sigma-Aldrich (St Louis, MO, USA).
Mouse studies
BA/F3 (1 × 106) cells expressing mutant BCR/ABL T315I were delivered by tail vein injection in NOD-SCID-IL2gKO. We assessed tumor burden by counting blasts in blood smears and spleen sections. These studies were performed according to the guidelines of the UT Southwestern Institutional Animal Care and Use Committee.
Statistical analyses
All data presented are representatives of experiments repeated at least twice or more with equivalent results. Significance was determined using t-test analysis or one-way analysis of variance (Holm–Sidak method) utilizing the SigmaPlot software (Systat Software Inc., San Jose, CA, USA).
Kern's method was used to evaluate synergistic effects in vitro.25 In brief, the expected cell number for dual treatment was defined as product of the percentages of remaining cells treated with drug A or B divided by 100. A ratio was calculated by dividing the expected cell number by the observed cell number. A ratio of 1 was termed additive, whereas a ratio larger than 1 or smaller than 1 was termed synergistic or antagonistic, respectively.
Results
Dual PI3K/mTORC1/2 blockade with BEZ235 leads to a striking antiproliferative effect in primary murine CML samples
To begin testing the antileukemic effects of inhibitors of the PI3K signaling pathway we performed methylcellulose colony assays with primary murine CML cells obtained from mice that underwent bone marrow reconstitution with hematopoietic cells transduced with a retroviral vector-expressing BCR/ABL. For these studies we used BEZ235, a dual PI3K/mTORC1/2 inhibitor, GDC0941, a pan-PI3K inhibitor and KU-0063794, a dual mTORC1/2 inhibitor.18, 19, 20 We found that all three compounds fully suppressed colony formation of primary murine CML samples to an equivalent degree (Figure 1a). Notably, wild-type hematopoietic cells were less sensitive to the antiproliferative effects exerted by BEZ235, GDC0941 and KU-0063794 (Figure 1a).
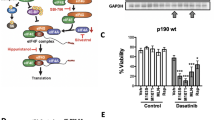
Dual PI3K/mTORC1/2 blockade inhibits proliferation of primary CML cultures and of BA/F3 cells expressing BCR–ABL. (a) Histogram of primary murine hematopoietic stem cell cultures obtained from wild-type (BM wt) and primary CML murine bone marrow (BM BCR–ABL) treated as indicated. Relative colony formation was calculated as percentage between treated and untreated cells and shown on the y axis. (b) Proliferation assay of BA/F3 cells expressing vector control (control), wild-type BCR–ABL (wt) or BCR–ABL mutants (T315I) treated with BEZ235 (BEZ). Note that BEZ235 causes inhibition of proliferation in a dose-dependent manner in BCR/ABL-expressing cells. (c) Growth curve of the indicated BA/F3 cells treated with increasing doses of the mTORC1 inhibitor rapamycin for 72 h. (d) Representative growth curve of the indicated BA/F3 cells treated with imatinib (Imat.) for 72 h. (e) BA/F3 control, wt and T315I cells treated with BEZ235 at the indicated concentrations for 24 h. We detected total and phosphorylated (p-) proteins by western blot. BEZ235 decreases phosphorylation of S6 and 4EBP1 and upregulates p-ERK. (f, g) BA/F3 cells expressing control (g) or wild-type BCR/ABL (f) were treated with 1 μM Imat inib (Imat.), 10 μM GDC0941 (GDC), 1.5 μM KU-0067394 (KU), 100 nM AZD8055 (AZD), 100 nM BEZ235, 5 μM ARRY142886 (ARRY) or 100 nM insulin. TORC2 activity was determined by western blot of phospho-AKT S473. The drugs inhibited their intended targets within 1 h of treatment.
Inhibition of the PI3K signaling pathway leads to a striking antiproliferative effect in BA/F3 cells expressing wild-type and imatinib-resistant BCR/ABL mutants
We used BA/F3 cells to better characterize the antileukemic effects we observed in primary CML cells. We determined that BEZ235 strikingly inhibits proliferation of cells expressing BCR/ABL and imatinib-resistant mutants (Figure 1b), whereas rapamycin not only had a modest effect on cell proliferation, but also showed little selectivity toward BCR/ABL-expressing cells (Figure 1c). Notably, parental BA/F3 cells were significantly less sensitive to BEZ235 treatment than cells expressing BCR/ABL (Figure 1b). As expected, imatinib did not affect proliferation of BA/F3 cells expressing mutant BCR/ABL (Figure 1d). These antiproliferative effects correlate with the ability of BEZ235 to inhibit mTORC1/2 signaling in these cells as determined by phospho-4EBP1 (T37/46), phospho-S6 (Figure 1e), which are downstream targets of mTORC1, and phospho-AKT (T473), a target of mTORC2 (Figures 1f and g). We also determined that phospho-ERK was upregulated by BEZ235 in BA/F3 cells expressing BCR–ABL, most likely due to a compensatory feedback mechanism (Figure 1e).11, 26 Furthermore, we confirmed that inhibition of PI3K with GDC0941, and mTOR with KU-0063794 and AZD8055, but not of MEK1 with ARRY142886, appropriately suppressed phosphorylation of AKT S473 (Figures 1f and g), independently of BCR–ABL expression.
Dual PI3K/mTORC1/2 blockade induces cell death in BA/F3 cells
To better characterize the antiproliferative effect of dual PI3K/mTOR blockade we analyzed BA/F3 cells treated with BEZ235 by flow cytometry. For these experiments, we used BEZ235 at a concentration of 150 nM, which significantly inhibits the growth of BA/F3 cells expressing BCR/ABL. We determined that BEZ235 induced a striking increase of the percentage of cells present in the sub-G0 phase of the cell cycle, which represents cells undergoing apoptosis (Figures 2a and b). The percentage increase in the sub-G0 cell population was significantly more evident in BA/F3 cells expressing wild-type and BCR/ABL mutants resistant to TKI (Figure 2b). To confirm with an unrelated assay that BEZ235-treated cells undergo apoptosis, we measured cleaved caspase 3, a well-known marker of apoptosis. Indeed, we found that BEZ235 promoted a twofold increase of caspase 3 activation in a time- and dose-dependent manner (Figures 2c and d). Taken together these experiments indicate that dual PI3K/mTOR blockade leads to apoptosis of BA/F3 cells expressing wild-type and TKI-resistant BCR/ABL.
Dual PI3K/mTORC1/2 inhibition with BEZ235 induces apoptosis in BA/F3 cells expressing BCR–ABL. (a) Cell cycle analysis of BA/F3 control, wild-type (wt) BCR/ABL and T315I untreated (UT) and treated with BEZ235 at 150 nM for 48 h. Note that treatment with BEZ235 causes a significant increase in the Sub-G0 fraction of the cell cycle in cells expressing BCR/ABL indicating apoptotic response. (b) Fold change analysis histograms of BA/F3 control, wt BCR–ABL and mutant T315I treated with BEZ235 of three individual flow cytometry experiments. In brief, percentages of each cell cycle faction were averaged. Fold change was calculated by normalizing to the percentage of untreated cells. Standard deviations were calculated and are shown as error bars. Cells were treated with 150 nM of BEZ235 for 48 h. (c, d) Graphs show activation of caspase 3 and 7 upon BEZ235 treatment in BA/F3 cells expressing wild-type BCR/ABL in a dose- (c) and time- (d) dependent manner. Cells were treated as indicated and apoptosis was measured by luminescence with the Caspase-Glo 3/7 assay kit. Luminescence was normalized to cells present in each sample and presented as relative value. Staurosporine was used as positive control to detect caspase activation upon apoptotic stimuli. Vertical lines indicate standard deviations in all graphs presented.
Pharmacologic inhibition of mTORC1/2 recapitulates the effects of dual PI3K/mTORC1/2 blockade in BCR/ABL-expressing cells
We sought to determine whether the antileukemic effect exerted in vitro by BEZ235 is due to inhibition of the PI3K, mTORC1 or mTORC2 protein kinases. For these experiments, we used KU-0063794 and its derivative AZD8055, small molecules that target specifically the mTORC1 and mTORC2 protein complexes and GDC0941, a specific pan-PI3K inhibitor.19, 20, 21 We determined that mTORC1/2 inhibition with KU-0063794 or AZD8055 strikingly reduces cell proliferation in BA/F3 cells expressing BCR/ABL independently of mutation status. Moreover, we found that parental BA/F3 cells were significantly less sensitive to the effects of both of these inhibitors than cells expressing BCR/ABL (Figures 3a and b, respectively). We also determined that the GDC0941 effectively decreases cell proliferation, however, this drug did not show a selective effect based on BCR/ABL expression in BA/F3 cells (Figure 3c).
Inhibition of the mTORC1/2 complex recapitulates the effects of BEZ235 treatment in BA/F3 cells. (a) Growth curve of BA/F3 control, wild type (wt), E255K and T315I cells treated with increasing doses of mTOR inhibitor KU-0067394 (KU) for 72 h. Note that KU-0063794 causes inhibition of cell proliferation preferentially in BCR–ABL-expressing cells. (b) Growth curve of BA/F3 control, wt and T315I cells treated with increasing doses of mTOR inhibitor AZD8055 (AZD) for 72 h. Note that AZD8055 also causes inhibition of cell proliferation preferentially in BCR–ABL-expressing cells. (c) Growth curve of BA/F3 control, wt, E255K and T315I cells treated with increasing doses of PI3K inhibitor GDC0941 (GDC) for 72 h. (d, e) Western blot analysis of BA/F3 cells treated with KU-0063794 or GDC0941, respectively. Detected proteins are indicated on the left. Note that both drugs decreased phosphorylation of S6 ribosomal protein, a downstream target of TORC1. Densitometry analysis was performed using ImageJ software, Research Services Branch, NIH (rsbweb.nih.gov). Level of phosphorylation of S6 protein was calculated as a ratio to total S6 protein. The resulting ratios were normalized to the level of untreated cells of each cell line. (f) Western blot of BA/F3 BCR/ABL wt cells untreated (UT) and treated with 1 μM imatinib (Imat.), 10 μM GDC0941, 1.5 μM KU-0067394 and 100 nM AZD8055 (AZD). Note that both, KU and AZD, upregulated p-ERK and downregulated the activity of the TORC1 target 4-EBP1. Vertical lines indicate standard deviations in all graphs presented.
We confirmed by western blot analysis that KU-0063794 and GDC0941 inhibit targets downstream of the mTORC1 complex such as p-S6 (Figures 3d and e, respectively) in both parental BA/F3 and cells expressing BCR–ABL. These findings suggest that GDC0941 may lack therapeutic index in leukemic cells. Thus, we conclude that dual inhibition of the mTORC1/2 complexes is a more desirable therapeutic strategy to affect oncogenic signaling downstream of BCR/ABL.
Dual PI3K/mTORC1/2 inhibition with BEZ235 in a mouse model of CML
Others and we have used BEZ235 in mouse models of cancer due to its excellent bioavailability and have demonstrated significant antitumor effects.18, 24 Moreover, this drug has been already tested in phase I clinical trials and is presently tested in phase II clinical trials for other human cancer types.9 Thus, our in vitro data prompted us to test the antileukemic properties of BEZ235 in vivo. For this purpose, we injected NOD-SCID-IL2gKO mice intravenously with BA/F3 cells expressing the pan-TKI-resistant BCR/ABL T315I mutant. In this mouse model, mice invariably succumb to a CML-like disease in about 3 weeks.27 Two cohorts of five leukemic mice each, received treatment with BEZ235 or vehicle 14 days after injection. We killed mice of both cohorts after 4 days of treatment and measured spleen weight as readout of its degree of infiltration with leukemic cells, to quantify response to treatment. We determined that BEZ235 caused a significant reduction in leukemic burden (Figure 4a). All leukemic animals showed extramedullary hematopoiesis in their spleens (Figure 4b panel B1) as compared with control animals (Figure 4b panel A1). On the contrary, spleens of untreated animals were packed with leukemic cells with abundant mitotic figures (Figure 4b, panel B1). Spleens of mice treated with BEZ235 showed nuclear fragmentation suggesting the presence of apoptotic cells (Figure 4b panel E1). In addition, the spleens of two treated animals contained neutrophil clusters, a sign of an inflammatory response, and one spleen showed extensive necrosis (Figure 4b panels C1 and D1, respectively). Terminal transferase dUTP nick-end labeling staining confirmed an increase in DNA fragmentation of leukemic cells consistent with an apoptotic response in treated animals (Figure 4b, panel H1). These data show that dual PI3K/mTOR blockade with BEZ235 induces a striking antileukemic effect both in vitro and in vivo.
Dual PI3K/mTOR inhibition with BEZ235 induces antileukemic effects in vivo. (a) Histogram demonstrating the weights of spleens obtained from mice injected with BA/F3 BCR/ABL T315I cells. Mice received BEZ235 or its diluent by gavage. Animals were killed after 4 days of treatment. Compared with untreated leukemic mice, spleens from treated mice displayed dramatic weight reduction. Vertical lines indicate standard deviations. (b; A1–H1) Hematoxylin and eosin staining of representative spleen sections ( × 200 magnifications). Spleens were obtained from (A1) leukemia-free, (B1) untreated leukemic and (C1–H1) leukemic mice treated with BEZ235. Histologic changes in spleens from treated mice included (C1) neutrophil clusters, (D1) necrosis and (E1) condensed apoptotic nuclei (indicated by asterisk and inlay). Terminal transferase dUTP nick-end labeling staining (F1–H1) was performed using the Apo Tag peroxidase in situ apoptosis detection kit (Millipore, Billerica, MA, USA). (F1) Negative control section, (G1) untreated leukemic spleen, (H1) leukemic spleen after therapy. Cells positive for DNA fragmentation appear brown as indicated by asterisk and inlay.
Discussion
The treatment modalities of CML have been revolutionized by the availability of TKIs that specifically target the BCR/ABL oncogene. Such therapies lead a 10-year survival that approaches 90% in newly diagnosed patients. Nevertheless this form of therapy is hampered by several limitations. For example, patients with advanced CML are less sensitive to TKI therapy and responses are short lived. Moreover, drug resistance due to the emergence of TKI-resistant mutants is significant in advanced phase CML patients. Second generation TKIs can over-ride some, but not all imatinib-resistant mutants.1 Finally, it is believed that TKI therapy should be continued indefinitely in responding patients due to the inability of these drugs to eradicate CML. Thus, innovative treatment modalities are needed to improve the outcome of CML even further, for example, by over-riding TKI-resistant mutants, or to promote eradication of BCR/ABL-harboring cells in patients that respond to TKI therapy. BA/F3 used in this study grow independently of interleukin-3 when expressing the BCR/ABL oncoprotein and have been previously demonstrated to recapitulate not only the events leading to BCR/ABL-induced leukemogenesis but also the therapeutic effects of TKIs.17
The BCR/ABL oncogene has a pivotal role in leukemogenesis by activating several oncogenic signaling pathways. Among these, the PI3K/mTORC1/2 network has been under intense investigation for the pivotal role that it has in regulating cell proliferation, survival and metabolism.4, 5 As a result PI3K, mTORC1/2 or dual PI3K/mTORC1/2 inhibitors have been developed with the expectation that these drugs would elicit potent antitumor effects.
Our study supports the clinical development of mTORC1/2 inhibitors for the treatment of leukemias expressing BCR/ABL as well as TKI-resistant BCR/ABL mutants including the pan-resistant T315I mutant. We observed that KU-0063794 exerts antiproliferative effects at a dosage comparable to previous studies conducted in cells exposed to cytokines and growth factors.19 Moreover, our observation that its derivative AZD8055 elicits comparable antileukemic effects in vitro suggests that the mTORC1/2 complexes are critical therapeutic targets in BCR/ABL-induced disease, which was previously placed downstream of PI3K in CML cells.28 These observations provide a rationale to explain the failure of rapamycin, which targets only mTORC1, to produce profound antileukemic effects in vivo. We found surprising that GDC0941 affected the parental BA/F3 with similar efficacy as compared with BA/F3 cells expressing BCR/ABL. This could be caused by off target or mTORC1/2-independent drug effects such as the ability of BCR/ABL to induce ROS activity through PI3K.29 The mechanistic underpinnings of this divergent effect should be investigated in future studies. Based on these considerations, we propose that mTORC1/2 inhibitors are promising drugs for the treatment of BCR/ABL-expressing leukemias.
These data confirm and extend several in vivo studies with pan-PI3K/mTORC1/2 or mTORC1/2 inhibitors. So far, this class of drugs has been tested mostly in cellular and preclinical models of solid malignancies.8, 9 In this setting, PI3K/mTOR inhibition leads to antiproliferative or proapoptotic effects depending on cellular context.24, 30, 31 More recently, these drugs have demonstrated activity in lymphoma, acute leukemias and myeloma cells.16, 32, 33, 34 In hematopoietic malignancies inhibition of the PI3K/mTOR signaling pathway has been mostly associated with pro-apoptotic effects. This observation suggests that PI3K/mTORC1/2 inhibitors will be valuable anticancer drugs in a wide spectrum of neoplastic diseases.
Notably, we have not noticed overt toxicities or effects on blood counts during BEZ235 administration in vivo (data not shown). These results are in agreement with the experience of others and us with murine mouse models.24, 31, 34 Future studies should determine whether mTORC1/2 inhibitors provide advantages over pan-PI3K/mTORC1/2 inhibitors. In this regards, it was recently shown that pan-PI3K/mTORC inhibitors cause greater immunosuppression than TORC1/2 inhibitors in mouse models.34 We observed an increase in phosphorylation of ERK, when treating cells with BEZ235 suggesting a feedback mechanism to overcome PI3K and mTORC1/2 blockade. As the activation of other survival signaling pathways could be detrimental in the treatment of CML, we analyzed the combination therapy of BEZ235 with ARRY142886, a MEK1/2 inhibitor (Supplementary Figure 1a). However, dual treatment with BEZ235 did not increase the antitumorigenic effects observed with either drug alone. It will be of interest to determine whether combination therapy with inhibitors of mTORC1/2 and other targets of BCR/ABL such as SRC and JNK will be beneficial.1
Others and we have reported that dual PI3K/mTORC1/2 blockade and DNA damage synergize to induce apoptosis.18, 24 Thus, we tested cytarabine, an antimetabolite commonly used in the treatment of acute leukemias. Unexpectedly, we found, that the combination of cytarabine with BEZ235 led to an antagonistic effect on the growth of leukemic BA/F3 cells (Supplementary Figures 1c and d); whereas it had a neutral effect on the parental BA/F3 cells (Supplementary Figure 1e). These data suggest that combination regimens of PI3K/mTOR inhibitors with antimetabolites or DNA-damaging agents may lead to unintended consequences in leukemias.
Taken together, our findings provide the rationale for the development of selective mTOR inhibitors for the treatment of leukemias expressing BCR/ABL and other malignancies that depend on the mTORC1/2 complex.
References
Kantarjian HM, Talpaz M, Giles F, O’Brien S, Cortes J . New insights into the pathophysiology of chronic myeloid leukemia and imatinib resistance. Ann Intern Med 2006; 145: 913–923.
Jabbour E, Kantarjian H, Cortes J . Chronic myeloid leukemia and second-generation tyrosine kinase inhibitors: when, how, and which one? Semin Hematol 2010; 47: 344–353.
Steelman LS, Pohnert SC, Shelton JG, Franklin RA, Bertrand FE, McCubrey JA . JAK/STAT, Raf/MEK/ERK, PI3K/Akt and BCR-ABL in cell cycle progression and leukemogenesis. Leukemia 2004; 18: 189–218.
Sengupta S, Peterson TR, Sabatini DM . Regulation of the mTOR complex 1 pathway by nutrients, growth factors, and stress. Mol Cell 2010; 40: 310–322.
Guertin DA, Sabatini DM . Defining the role of mTOR in cancer. Cancer Cell 2007; 12: 9–22.
Kubota Y, Ohnishi H, Kitanaka A, Ishida T, Tanaka T . Constitutive activation of PI3K is involved in the spontaneous proliferation of primary acute myeloid leukemia cells: direct evidence of PI3K activation. Leukemia 2004; 18: 1438–1440.
Martelli AM, Nyakern M, Tabellini G, Bortul R, Tazzari PL, Evangelisti C et al. Phosphoinositide 3-kinase/Akt signaling pathway and its therapeutical implications for human acute myeloid leukemia. Leukemia 2006; 20: 911–928.
Yap TA, Garrett MD, Walton MI, Raynaud F, de Bono JS, Workman P . Targeting the PI3K-AKT-mTOR pathway: progress, pitfalls, and promises. Curr Opin Pharmacol 2008; 8: 393–412.
Maira SM, Finan P, Garcia-Echeverria C . From the bench to the bed side: PI3K pathway inhibitors in clinical development. Curr Top Microbiol Immunol 2011; 347: 209–239.
Thomson AW, Turnquist HR, Raimondi G . Immunoregulatory functions of mTOR inhibition. Nat Rev Immunol 2009; 9: 324–337.
Guertin DA, Sabatini DM . The pharmacology of mTOR inhibition. Sci Signal 2009; 2: pe24.
Carracedo A, Pandolfi PP . The PTEN-PI3K pathway: of feedbacks and cross-talks. Oncogene 2008; 27: 5527–5541.
Chiarini F, Fala F, Tazzari PL, Ricci F, Astolfi A, Pession A et al. Dual inhibition of class IA phosphatidylinositol 3-kinase and mammalian target of rapamycin as a new therapeutic option for T-cell acute lymphoblastic leukemia. Cancer Res 2009; 69: 3520–3528.
Kharas MG, Janes MR, Scarfone VM, Lilly MB, Knight ZA, Shokat KM et al. Ablation of PI3K blocks BCR-ABL leukemogenesis in mice, and a dual PI3K/mTOR inhibitor prevents expansion of human BCR-ABL+ leukemia cells. J Clin Invest 2008; 118: 3038–3050.
Park S, Chapuis N, Bardet V, Tamburini J, Gallay N, Willems L et al. PI-103, a dual inhibitor of class IA phosphatidylinositide 3-kinase and mTOR, has antileukemic activity in AML. Leukemia 2008; 22: 1698–1706.
Weisberg E, Banerji L, Wright RD, Barrett R, Ray A, Moreno D et al. Potentiation of antileukemic therapies by the dual PI3K/PDK-1 inhibitor, BAG956: effects on BCR-ABL- and mutant FLT3-expressing cells. Blood 2008; 111: 3723–3734.
La Rosee P, Corbin AS, Stoffregen EP, Deininger MW, Druker BJ . Activity of the Bcr-Abl kinase inhibitor PD180970 against clinically relevant Bcr-Abl isoforms that cause resistance to imatinib mesylate (Gleevec, STI571). Cancer Res 2002; 62: 7149–7153.
Maira SM, Stauffer F, Brueggen J, Furet P, Schnell C, Fritsch C et al. Identification and characterization of NVP-BEZ235, a new orally available dual phosphatidylinositol 3-kinase/mammalian target of rapamycin inhibitor with potent in vivo antitumor activity. Mol Cancer Ther 2008; 7: 1851–1863.
Garcia-Martinez JM, Moran J, Clarke RG, Gray A, Cosulich SC, Chresta CM et al. Ku-0063794 is a specific inhibitor of the mammalian target of rapamycin (mTOR). Biochem J 2009; 421: 29–42.
Folkes AJ, Ahmadi K, Alderton WK, Alix S, Baker SJ, Box G et al. The identification of 2-(1H-indazol-4-yl)-6-(4-methanesulfonyl-piperazin-1-ylmethyl)-4-morpholin -4-yl-thieno[3,2-d]pyrimidine (GDC-0941) as a potent, selective, orally bioavailable inhibitor of class I PI3 kinase for the treatment of cancer. J Med Chem 2008; 51: 5522–5532.
Chresta CM, Davies BR, Hickson I, Harding T, Cosulich S, Critchlow SE et al. AZD8055 is a potent, selective, and orally bioavailable ATP-competitive mammalian target of rapamycin kinase inhibitor with in vitro and in vivo antitumor activity. Cancer Res 2010; 70: 288–298.
Huynh H, Soo KC, Chow PK, Tran E . Targeted inhibition of the extracellular signal-regulated kinase kinase pathway with AZD6244 (ARRY-142886) in the treatment of hepatocellular carcinoma. Mol Cancer Ther 2007; 6: 138–146.
Nicoletti I, Migliorati G, Pagliacci MC, Grignani F, Riccardi C . A rapid and simple method for measuring thymocyte apoptosis by propidium iodide staining and flow cytometry. J Immunol Methods 1991; 139: 271–279.
Konstantinidou G, Bey EA, Rabellino A, Schuster K, Maira MS, Gazdar AF et al. Dual phosphoinositide 3-kinase/mammalian target of rapamycin blockade is an effective radiosensitizing strategy for the treatment of non-small cell lung cancer harboring K-RAS mutations. Cancer Res 2009; 69: 7644–7652.
Kern DH, Morgan CR, Hildebrand-Zanki SU . In vitro pharmacodynamics of 1-beta-D-arabinofuranosylcytosine: synergy of antitumor activity with cis-diamminedichloroplatinum(II). Cancer Res 1988; 48: 117–121.
Brachmann SM, Hofmann I, Schnell C, Fritsch C, Wee S, Lane H et al. Specific apoptosis induction by the dual PI3K/mTor inhibitor NVP-BEZ235 in HER2 amplified and PIK3CA mutant breast cancer cells. Proc Natl Acad Sci USA 2009; 106: 22299–22304.
McLaughlin J, Cheng D, Singer O, Lukacs RU, Radu CG, Verma IM et al. Sustained suppression of Bcr-Abl-driven lymphoid leukemia by microRNA mimics. Proc Natl Acad Sci USA 2007; 104: 20501–20506.
Ly C, Arechiga AF, Melo JV, Walsh CM, Ong ST . Bcr-Abl kinase modulates the translation regulators ribosomal protein S6 and 4E-BP1 in chronic myelogenous leukemia cells via the mammalian target of rapamycin. Cancer Res 2003; 63: 5716–5722.
Kim JH, Chu SC, Gramlich JL, Pride YB, Babendreier E, Chauhan D et al. Activation of the PI3K/mTOR pathway by BCR-ABL contributes to increased production of reactive oxygen species. Blood 2005; 105: 1717–1723.
Faber AC, Li D, Song Y, Liang MC, Yeap BY, Bronson RT et al. Differential induction of apoptosis in HER2 and EGFR addicted cancers following PI3K inhibition. Proc Natl Acad Sci USA 2009; 106: 19503–19508.
Engelman JA, Chen L, Tan X, Crosby K, Guimaraes AR, Upadhyay R et al. Effective use of PI3K and MEK inhibitors to treat mutant Kras G12D and PIK3CA H1047R murine lung cancers. Nat Med 2008; 14: 1351–1356.
Chapuis N, Tamburini J, Green AS, Vignon C, Bardet V, Neyret A et al. Dual Inhibition of PI3K and mTORC1/2 Signaling by NVP-BEZ235 as a New Therapeutic Strategy for Acute Myeloid Leukemia. Clin Cancer Res 2010; 16: 5424–5435.
Chiarini F, Grimaldi C, Ricci F, Tazzari PL, Evangelisti C, Ognibene A et al. Activity of the novel dual phosphatidylinositol 3-kinase/mammalian target of rapamycin inhibitor NVP-BEZ235 against T-cell acute lymphoblastic leukemia. Cancer Res 2010; 70: 8097–8107.
Janes MR, Limon JJ, So L, Chen J, Lim RJ, Chavez MA et al. Effective and selective targeting of leukemia cells using a TORC1/2 kinase inhibitor. Nat Med 2010; 16: 205–213.
Acknowledgements
We thank Dr Brian Druker (Oregon Health Science University) for providing BA/F3 cells expressing BCR/ABL and TKI-resistant mutants. KS was supported by NRSA Award F32CA154237 from the National Cancer Institute. PPS was supported by NIH K08 grant CA112325, R01CA137195, American Cancer Society Institutional Research Grant #02-196, the Concern Foundation, the Gibson Foundation and Leukemia Texas Inc. CCZ was supported by Cancer Prevention and Research Institute of Texas RP100402.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Blood Cancer Journal website
Supplementary information
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Schuster, K., Zheng, J., Arbini, A. et al. Selective targeting of the mTORC1/2 protein kinase complexes leads to antileukemic effects in vitro and in vivo. Blood Cancer Journal 1, e34 (2011). https://doi.org/10.1038/bcj.2011.30
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bcj.2011.30
Keywords
This article is cited by
-
Chronic myeloid leukemia stem cells: targeting therapeutic implications
Stem Cell Research & Therapy (2021)