Abstract
Aim:
Small GTPase Rac1 is a member of the Ras superfamily, which plays important roles in regulation of cytoskeleton reorganization, cell growth, proliferation, migration, etc. The aim of this study was to determine how a constitutively active Rac1b regulated cell proliferation and to investigate the effects of the Rac1b inhibitor sanguinarine.
Methods:
Three HEK293T cell lines stably overexpressing GFP, Rac1-GFP or Rac1b-GFP were constructed by lentiviral infection. The cells were treated with sanguinarine (1 μmol/L) or its analogue berberine (1 μmol/L) for 4 d. Cell proliferation was evaluated by counting cell numbers and with a BrdU incorporation assay. The levels of cleaved PARP-89 (an apoptosis marker) and cyclin-D1 (a proliferative index) were measured using Western blotting.
Results:
In 10% serum-containing media, overexpressing either Rac1 or Rac1b did not significantly change the cell proliferation. In the serum-starved media, however, the survival rate of Rac1b cells was significantly increased, whereas that of Rac1 cells was moderately increased. The level of cleaved PARP-89 was significantly increased in serum-starved Rac1 cells, but markedly reduced in serum-starved Rac1b cells. The level of cyclin-D1 was significantly increased in both serum-starved Rac1 and Rac1b cells. Treatment with sanguinarine, but not berberine, inhibited the proliferation of Rac1b cells, which was accompanied by significantly increased the level of PARP-89, and decreased both the level of cyclin-D1 and the percentage of BrdU positive cells.
Conclusion:
Rac1b enhances the cell proliferation under a growth-limiting condition via both anti-apoptotic and pro-proliferative mechanisms. Sanguinarine, as the specific inhibitor of Rac1b, is a potential therapeutic agent for malignant tumors with up-regulated Rac1b.
Similar content being viewed by others
Introduction
The small GTPase Rac1, a member of the Ras superfamily, plays a fundamental role in the regulation of cytoskeleton reorganization, cell growth, proliferation, migration, cytokinesis, and transformation1,2,3,4. Recent studies have implicated that up-regulated Rac1 expression or deregulated Rac1 activity is crucial for the pathogenesis of a series of diseases including tumorigenesis, tumor metastasis, neurodegenerative disorders, mental retardation syndromes, and liver cirrhosis5,6,7,8,9,10. However, there has been no evidence that any native, constitutively active Rac1 mutants have been detected in these diseases. Studies that characterized Rac1's function were performed using artificially mutated constitutively active forms of Rac1-V12 and Rac1-L61, both of which have been shown to inhibit intrinsic GTPase activity and decrease GTPase-activating protein-stimulated GTP hydrolysis11,12.
Rac1b, an alternatively spliced variant of Rac1 containing 19 additional amino acids after the switch II region, has been recently shown to be constitutively active13,14. Several reports have shown that Rac1b demonstrated impaired intrinsic GTPase activity, enhanced intrinsic guanine nucleotide exchange activity, and reduced association with Rho-GDI13,14,15. Concerning its role in the signaling pathways for cell growth, proliferation, and migration, unlike Rac1, Rac1b neither leads to lamellipodia formation nor activates PAK1 and c-Jun-NH2-kinase activities15.
Apart from its constitutive activity, significantly up-regulated Rac1b expression has been reported to be deeply involved in tumorigenesis and the metastasis of colorectal, breast, lung, and thyroid cancers6,16,17,18. Transient over-expression of Rac1b in cultured cells was able to promote cell proliferation19. However, the role of stably over-expressed Rac1b in cell proliferation, migration, and survival ability remains unknown. Because of the critical roles of Rac1b in tumorigenesis and metastasis, it is clinically urgent to identify potent Rac1b inhibitors. Sanguinarine, a benzophenanthridine alkaloid, has been recently reported to be a selective Rac1b inhibitor in in vitro nucleotide binding inhibition assays20.
In this study, we thus aimed to determine whether the stable over-expression of Rac1 or Rac1b in 293T cells via a lentiviral approach could impact cell proliferation and survival and to further examine the effect of sanguinarine in these cells. We found that cells overexpressing either Rac1 or Rac1b showed normal proliferation patterns when cultured in 10% serum. However, under serum-starved conditions, the Rac1b cells showed a significant increase in survival rate, whereas the cells overexpressing Rac1 only showed a moderate increase. Of the three cell lines examined, sanguinarine only exerted a significant inhibitory effect on cell proliferation in the Rac1b cells. Based on our studies, we found that Rac1b is involved in the following underlying mechanisms: 1) Rac1b inhibited cell apoptosis and promoted cell proliferation, and 2) sanguinarine promoted cell apoptosis and retarded cell proliferation by inducing an inhibitory effect in the cells overexpressing Rac1b. Thus, sanguinarine may be a promising therapeutic agent for cancers with up-regulated Rac1b expression.
Materials and methods
Cell culture
293T cells were cultured and passaged in Dulbecco's modified Eagle's medium (DMEM; Gibco-Life; Grand Island, NY, USA) supplemented with 4500 mg/L high glucose, 10% fetal bovine serum, 100 units/mL penicillin, and 100 μg/mL streptomycin at 37 °C and 5% CO2.
Antibodies and reagents
Rabbit anti-Rac1 antibodies, normal rabbit IgG, HRP-conjugated goat anti-mouse and goat anti-rabbit secondary antibodies were purchased from Proteintech (Chicago, IL, USA). Mouse anti-Rac1 antibody was purchased from Transduction Laboratories (Lexington, KY, USA), and the antisera against Rac1b were raised from rabbits using purified GST-Rac1b 76–94 as the antigen. The antisera were purified using protein-A chromatography and further purified by GST absorption. Rabbit anti-PARP-89 antibodies were purchased from Biovision (Milpitas, CA, USA). Rabbit anti-cyclin-D1 antibodies were purchased from Abcam (Cambridge, MA, USA). The HRP-conjugated polyclonal antibody against β-actin was from Sigma (St Louis, MI, USA). Berberine was purchased from Shenggong Biologics (Shanghai, China) and sanguinarine was kindly provided by Prof Luo at the Shanghai JiaoTong University School of Chemistry and Chemical Engineering. The reagents were initially dissolved in DMSO (50 mmol/L); the reagents were dissolved to the applicable concentrations with PBS (the final DMSO concentration was <0.1%).
Reverse transcription polymerase chain reaction (PCR)
One microgram of total RNA, isolated from 293T cells with the TRIzol reagent (Invitrogen; Grand Island, NY, USA), was reverse transcribed into cDNA using the 5×PrimeScript RT master mix which includes PrimeScript RTase, RNase inhibitor, random hexamers, oligo dT primer, dNTP mixture, and reaction buffer (Takara; Otsu, Shiga, Japan). The cDNA was then amplified by PCR using a 2×basic DNA polymerase mixture (BiovisuaLab, Shanghai, China) with the following primers: Rac1/Rac1b-forward (5′-TGCCAATGTTATGGTAGATGG-3′), Rac1/Rac1b-reverse (5′-TGGGAGTCAGCTTCTTCTCC-3′), GAPDH-forward (5′-TCTTCACCACCATGGAGAAG-3′), and GAPDH-reverse (5′-TGACCTTGCCCACAGCCTTG-3′). The reaction was initially heated to 94 °C for 1 min followed by 30 cycles of PCR (94 °C for 30 s, 57 °C for 30 s, and 72 °C for 30 s) using a GeneAmp PCR 2700 (ABI; CA, USA).
Cloning of lentiviral constructs, packaging, and viral infection
Human Rac1 and Rac1b cDNA were amplified by PCR from our human heart cDNA library using the following primers: forward (5′-GTCGCCCGGGGGGGATCTCATATGCAGGCCATCAAGTGTG-3′) and reverse (5′-AGTACCGGGATCCACTAGTACGCGTTTACAACAGCAGGCATTTTCTCTTC-3′). The PCR products were then subcloned into the pHR-GFP vector (Addgene; Cambridge, MA, USA) between the Nde I and Mlu I (Fermentas; Pittsburgh, PA, USA) restriction sites using the GBI Clonart seamless ligation kit (Genebank Bioscience; Suzhou, China). All obtained constructs were confirmed by sequencing. For lentivirus packaging, 293T cells were transfected with the pHR-GFP, pHR-Rac1-GFP or pHR-Rac1b-GFP constructs together with two other helper plasmids, PMD2G and PSPAX2. Three types of viral particles (Lenti-GFP, Lenti-Rac1-GFP, and Lenti-Rac1b-GFP) were collected 72–96 h after plasmid transfection and were concentrated by ultracentrifugation. The obtained virus titer was approximately 1×108. For infection, 293T cells were plated at 50%–70% confluency, and the viral doses were based on the multiplicity of infection (MOI) of the 293T cells. The infection efficiencies were checked by the GFP signal 72 h after infection.
6His-Rac1 and -Rac1b protein expression
The pQE-31-Rac1 and pQE-31-Rac1b were expressed in BL-21 E coli cells, induced with 1 mmol/L isopropyl-D-thiogalactopyranoside, and purified via Nickel-sepharose beads (Novagen; Hilden, NRW, Germany) as described previously21. The purified 6His-Rac1 and 6His-Rac1b were eluted from the beads with 250 mmol/L imidazole.
Western blotting
Cells were harvested in the sample buffer (62.5 mmol/L Tris-HCl pH 6.8, 12% glycerol, 2% SDS, 0.004% BPB, and 10% 2-mercaptoethanol)21. The samples were separated by 10%-12% SDS-PAGE, transferred onto PVDF membranes (Millipore; Billerica, MA, USA), and incubated in blocking solution [5% fat-free milk in PBS containing 0.05% Tween-20 (PBST)] for 30 min at room temperature. For the phosphor antibodies, we used 1% BSA in the blocking solution instead of 5% fat-free milk. Following an overnight incubation at 4 °C with the primary antibodies (anti-Rac1, anti-Rac1b, and anti-β-actin at 1:1000, 1:1000, and 1:5000 dilutions, respectively) in the blocking solution, the blots were washed 3 times with PBST and then incubated with the HRP-conjugated secondary antibodies (1:1000 dilution) for 1 h at room temperature before extensive washes. The blots were visualized using the ECL detection kit (Thermo-Pierce; Rockford, IL, USA) on a Chemi DocTM XRS+ (BIO-RAD, Heracles, CA, USA) and quantified using the Image Lab 2.0 software on a Criterion Stain Free System.
Immunofluorescence
The 293T cell lines grown on cover slips were fixed with 4% paraformaldehyde for 30 min, permeabilized in 0.3% Triton X-100, and then blocked in PBS containing 5% donkey serum (Jackson Laboratories) for 1 h at room temperature22. The samples were incubated with the primary antibodies (1:400 dilution for both Rac1 and Rac1b) for 1 h at room temperature, followed by incubation with the TRITC-labeled secondary antibodies (1:200 dilution; Jackson Laboratory; Bar Harbor, ME, USA) for 1 h. The cells were washed 3 times with PBS, stained for nuclei with 1 μg/mL DAPI (Dojindo; Kumamoto, Japan), and mounted with Antifade medium (Molecular Probes; OR, USA). Images were recorded on a Leica DMI3000B microscope and processed using the Image-J software.
Proliferation assay
Culture dishes were plotted with small circles at the bottom to make it easier to repeatedly count the cells grown inside the circles23. Three cell lines were initially seeded at 20% confluency in media with 10% FBS and at 35% confluency in media with 0% FBS. The media were changed every day to remove the dead cells and the viable cells within each circle were imaged and counted daily for 4–5 d. For a portion of the experiments, the cells were treated with berberine (0.1–10 μmol/L) or sanguinarine (0.1–3 μmol/L) 24 h after seeding. After the media were changed, berberine or sanguinarine was supplemented to maintain the same concentrations.
Migration assay
Tiny marks were drawn on the bottom of a culture dish to make it easier to re-localize the places where the cells were selected for follow-up. Three cell lines were seeded at 70%–80% confluency in the media with 10% FBS. Twenty-four hours later, the cell monolayer was scratched with a yellow pipette tip and was then mildly washed twice with PBS. Images were taken at 0 and 24 h after scratching, and the migration distance was measured using the Image-J software (NIH).
BrdU incorporation assay
Cell proliferation in S-phase was monitored by the incorporation of bromo-deoxy uridine (BrdU). Cells were seeded on 10-mm cover slips and cultured for 24 h in DMEM with and without 10% FBS in the presence and absence of 1 μmol/L sanguinarine. Following treatment with BrdU (0.1 mmol/L; Sigma), cells were cultured for 2 h. Then, the cells were washed three times with PBS, fixed with cold acetone-methanol (1:1, v/v), denatured with 4 mol/L HCl (Qiangsheng Biologics, Jiangsu, China), and incubated with anti-specific-BrdU antibody (Sigma; 1:1000 dilution) for 1 h. The cells were then prepared using the same protocol described above for the immunofluorescence experiments. The cells in S-phase that incorporated BrdU were counted from at least 10 randomly selected fields. For each group, at least 160 BrdU-(+) cells were accumulated.
Statistical analysis
Data are presented as the mean±SEM. Levene's test was used to determine the homogeneity of variance among the cell lines with the SPSS 19.0 statistical software. The ANOVA and repeated measurement data ANOVA tests were used for a portion of the analysis. Least significant difference (LSD) was used when an equal variance was assumed. The Games-Howell test was used when equal variance was not assumed. The Mann-Whitney test was used for two independent samples. Data were considered statistically significant when P<0.05.
Results
Establishment of stable cell lines overexpressing Rac1 and Rac1b
We initially checked the endogenous Rac1/Rac1b transcription and expression levels in normal 293T cells. RT-PCR results detected the Rac1 transcript, but not the Rac1b transcript, in the 293T cells (Figure 1A). Consistent with these results, Western blotting showed that Rac1 protein, but not Rac1b protein, was present in the cells (Figure 1B).
Rac1 or Rac1b expression in normal 293T cells and in Lenti-GFP, Lenti-Rac1-GFP, and Lenti-Rac1b-GFP cells lines. (A) The endogenous Rac1 and Rac1b transcripts in normal 293T cells were reverse transcribed into cDNA and amplified by PCR. The pCMV-Rac1 and pCMV-Rac1b plasmids were used as positive controls. (B) Normal 293T lysate was analyzed by Western blotting using anti-Rac1 (left panel) and anti-Rac1b (right panel) antibodies. The positive controls used are pure recombinant 6His-Rac1 and 6His-Rac1b. (C) GFP-fluorescence signals (upper row) and the corresponding light images (lower row) identified an almost 100% infection efficiency in all three cell lines 72 h after viral infection. (D) Quantification of the three independent blots indicates that Rac1 protein levels increased by 2.0 fold compared with the Lenti-GFP cells. (E) Similarly, three independent blots indicate that the Rac1b nascent protein levels increased by 17.3 fold compared with the Lenti-GFP cells. The bars represent 20 μm. Mean±SEM. cP<0.01.
Next, we made three stable 293T cell lines that were infected with Lenti-GFP, Lenti-Rac1-GFP, and Lenti-Rac1b-GFP. The infection efficiencies were confirmed to be 100% for all three cell lines (Figure 1C). The intensity of the GFP fluorescence was higher in the cells overexpressing GFP and much weaker in cells overexpressing either Rac1 or Rac1b. In the pHR constructs, the Rac1/Rac1b gene and the GFP gene were separated by an internal ribosome entry site (IRES) but shared the same promoter. Thus, a weaker GFP expression does not correlate to weaker Rac1/Rac1b expression. In the Rac1-overexpressing cells, Rac1 expression was increased by 2.0 fold at 96 h after infection (Figure 1D). In the Rac1b-overexpressing cells, nascent Rac1b expression was enhanced by 17.3 fold (Figure 1E). Over-expression was checked for at least 2 months during 20 passages (data not shown).
Effects of Rac1 and Rac1b on cell spreading and migration
First, we sought to identify the differences in cell spreading between the three cell lines by measuring the cell area after Rac1 or Rac1b immunofluorescence staining (Figure 2A). Compared with the control cells (34.2±4.2 μm2), the cells overexpressing Rac1b had the largest increase in size (67.9±5.6 μm2; P<0.01), while the cells overexpressing Rac1 showed a moderate increase in size (49.9±4.7 μm2; P<0.05) (Figure 2B).
Cell spreading of the three cell lines cultured in 10% serum. Three cell lines were sparsely seeded and fixed by paraformaldehyde for the staining of both Rac1 and Rac1b and for the measurement of the cell size 24 h after seeding. (A) Overexpressed Rac1 and Rac1b were detected mainly in nucleus with less in the cytoplasm. The bar represents 20 μm. (B) The cell sizes were determined and summarized using computerized morphometric cell area measurements from rhodamine-stained contours of the cells. cP<0.01 compared with the Lenti-GFP cell line. eP<0.05 compared with the Lenti-Rac1-GFP. n=70. Mean±SEM.
It is well known that Rac1 is deeply involved in cell spreading and migration2,3. The above results regarding the cell spreading of the Rac1 or Rac1b cells, measured as cell area, might promote cell migration. Thus, we next observed whether the stable over-expression of Rac1 or Rac1b would influence cell migration (Figure 3A and 3B). The cells overexpressing Rac1b (8.7±0.4 μm/h) showed no change in migration compared to the control cells (8.3±0.7; P>0.05). However, the cells overexpressing Rac1 (7.0±0.6) showed an attenuated migration pattern compared to the Rac1b cells (P<0.05).
Cell migration of the three cell lines cultured in 10% serum. The monolayer of cells was scratched and the wounds (arrow head) with the recognizable marker were photographed using a phased microscope. (A) Representative images of the three cell lines at 0 and 24 h after scratching. The bar represents 500 μm. (B) The migrating velocity calculated during the first 24 h after scratching. Rac1 cells were significantly slower at migrating than Rac1b cells (bP<0.05). The data were obtained from 6 independent experiments and for each experiment the velocities were measured from three marked locations. Mean±SEM.
Rac1b promotes cell proliferation in serum-starved 293T cells
Cell proliferation was monitored in two different media. In the medium containing 10% serum (Figure 4A), from the first to fourth day, the number of control cells increased from 36.0±4.0 to 240.5±21.7 per circle, the number of Rac1 cells increased from 43.3±2.8 to 434.4±26.0, and the number of Rac1b cells increased from 52.7±3.4 to 448.7±35.0. No differences were found between the three cell lines.
Changes in proliferation of the three cell lines cultured in 10% serum and 0% serum. The cells growing inside the drawn circles were photographed daily using a phased microscope and counted. (A) No differences in proliferation were observed between three cell lines when they were cultured in media with 10% serum (P>0.05). The data were obtained from three independent experiments and for each experiment the cells were counted from 10 circles. (B) Significant differences in cell survival were found among the three cell lines cultured in serum-starved (0% serum) media. cP<0.01 compared with the Lenti-GFP cell line. eP<0.05 compared with the Lenti-Rac1-GFP cell line. The data were obtained from three independent experiments, and for each experiment, the cells were counted from 5 circles. Mean±SEM. (C) Representative images of the control cells (upper), the Rac1 cells (middle), and the Rac1b cells (lower panel) growing inside the circles in serum-starved media during 1–4 d.
In the serum-starved medium (Figure 4B and 4C), from the d 1 to d 4, all three cell lines showed retarded proliferation to different extents. The number of control cells increased from 34.6±5.8 to 46.8±12.0, the number of Rac1 cells increased from 41.8±3.9 to 122.8±8.0, and the number of Rac1b cells increased from 52.8±5.5 to 207.4±26.9.
These results show that cell proliferation was almost completely suppressed in the control cells. In comparison, the suppression of cell proliferation was mild in the Rac1b cells (P<0.01 compared with control cells) and moderate in the Rac1 cells (P<0.01 compared with control cells). Compared with Rac1 cells, Rac1b cells demonstrated a significant increase in survival ability (P<0.05).
Sanguinarine inhibits Rac1b-rendered enhancement in cell survival
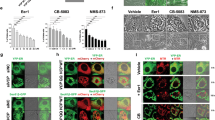
To test the selectivity of sanguinarine, a recently reported Rac1b inhibitor, towards Rac1 and Rac1b, we compared its effect on proliferation of the three cell lines. Berberine, a sanguinarine analogue was used as the control agent (Figure 5A). At the higher concentrations (3–10 μmol/L), sanguinarine was identified to be cytotoxic and the experiments were discontinued midway in all three cell lines. Treatment with 1 μmol/L sanguinarine (Figure 5B and 5C), from the first to the fifth day, increased the cell number 6.9±0.6 fold in the control cells, 4.9±0.8 fold in the Rac1 cells, and 1.8±0.7 fold in the Rac1b cells. In contrast, the cell number increased 7.1±2.5 fold in the control cells, 5.9±0.2 fold in the Rac1 cells, and 5.4±0.3 fold in the Rac1b cells when the cells were not treated with sanguinarine. These results suggested sanguinarine did not inhibit proliferation in the cells overexpressing GFP or Rac1 but significantly suppressed proliferation in the cells overexpressing Rac1b (P<0.01).
Changes in proliferation of the three cell lines after treatment with either berberine or sanguinarine. (A) The chemical structures of berberine (left) and sanguinarine (right). (B) Comparison of cell proliferation with and without treatment of either 1 μmol/L berberine (left) or 1 μmol/L sanguinarine (right) between the cell lines overexpressing GFP (upper panel), Rac1 (middle panel), and Rac1b (lower panel). cP<0.01 compared with sanguinarine. (C) Comparison of cell proliferation among the three cell lines with berberine (left) or sanguinarine (right) treatment. fP<0.01 compared with GFP. hP<0.05 compared with Rac1.
Treatment with 1 μmol/L berberine (Figure 5B and 5C), from the first to the fourth days, increased the cell number 8.2±1.3 fold in the control cells, 7.7±1.1 fold in the Rac1 cells, and 7.0±0.9 fold in the Rac1b cells. In contrast, the cell number increased 7.6±1.1 fold in the control cells, 7.8±1.4 fold in the Rac1 cells, and 6.9±0.7 fold in the Rac1b cells when cells were not treated with berberine. Thus, the sanguinarine analogue berberine was verified to have no anti-proliferative effects in all three cell lines at concentrations of 1 (Figure 5B) and 3 μmol/L (data not shown). However, at 10 μmol/L, berberine significantly inhibited cell proliferation in all three cell lines with similar potency, and no significant differences were found between any two cell lines (data not shown). These results suggest that berberine could exert its anti-proliferative activity by a different mechanism than through the inhibition of either Rac1 or Rac1b.
These results suggest that sanguinarine is a more selective inhibitor for Rac1b than Rac1. Sanguinarine inhibited cell proliferation in a dose-dependent manner (Figure 5D). At 0.1 μmol/L, it retarded proliferation in Rac1b cells by 5.3±0.4 fold (P>0.05). At 0.3 μmol/L, it attenuated proliferation in Rac1b cells to 3.9±0.4 fold (P>0.05). These results indicated that the effective concentration range of sanguinarine is very narrow.
(D) Dose-dependent inhibitory effects of sanguinarine on proliferation in Rac1b cells. cP<0.01 compared with cells without treatment (0 μmol/L). The data in (B, C, D) were collected from three independent experiments and for each experiment the cells were counted inside 10 marked circles for the berberine-treated cells and 5 marked circles for the sanguinarine-treated cells. (E) Comparison of cell proliferation among the three cell-lines cultured in serum-starved media with sanguinarine treatment. eP<0.05, Rac1 compared with GFP. iP<0.01, Rac1 compared with Rac1b. The data in (E) were obtained from three independent experiments and for each experiment cells were counted from 5 circles. Mean±SEM.
In the serum-starved media containing 1 μmol/L sanguinarine, cell proliferation increased in the control cells by 1.6±0.5 fold, in the Rac1 cells by 2.9±0.2 fold, and in the Rac1b cells by 1.4±0.4 fold (P<0.01 compared with Rac1 cells; P>0.05 compared with control cells) between the first and fifth days (Figure 5E). These results show that sanguinarine only inhibited cell survival in the cells overexpressing Rac1b. Compared with Figure 4B, sanguinarine almost completely inhibited Rac1b-rendered enhancement in cell survival.
Sanguinarine inhibited G1/S cell cycle progression in cells overexpressing Rac1b
To further verify the results from the proliferation assays, we performed BrdU incorporation assays. In the control cells growing in media with 10% serum, BrdU-(+) incorporation levels were 37.9%±1.4% and 38.8%±2.3% (P>0.05), respectively for the cells with and without sanguinarine (1 μmol/L) treatment. In the serum-starved media, the BrdU-(+) incorporation levels were 26.9%±1.1% and 27.8%±1.5% (P>0.05), respectively for the cells with or without sanguinarine treatment. In the cells overexpressing Rac1 with and without sanguinarine treatment, the BrdU-(+) incorporation levels were 40.4%±1.4% and 42.4%±1.0% (P>0.05), respectively when the cells were cultured in media containing 10% serum and were 27.4%±1.7% and 31.5%±2.7% (P>0.05), respectively when cultured in serum-starved media. These results indicate that sanguinarine did not inhibit G1/S cell cycle progression in the control or the Rac1 cells (Figure 6A and 6B).
Effect of sanguinarine on G1/S cell cycle progression. (A–C) Illustrations of the summarized percentage of BrdU-(+) cells in Lenti-GFP (A), Lenti-Rac1-GFP (B), and Lenti-Rac1b-GFP (C) cells cultured in either 10% or 0% serum and either with or without sanguinarine treatment. bP<0.05 compared with the 10% serum untreated control. fP<0.01 compared with the 0% serum untreated control. The data were obtained from three independent experiments. Mean±SEM. (D and E) Representative images of BrdU-(+) cells compared with the DAPI-stained Rac1b cells. Bars represent 50 μm.
For the cells overexpressing Rac1b cultured in the media containing 10% serum, the BrdU-(+) incorporation levels were 32.6%±1.3% and 41.5%±2.4% (P<0.05), respectively for the cells with and without sanguinarine treatment. In the serum-starved media, the BrdU-(+) incorporation levels were 26.4%±1.0% and 36.7%±1.4% (P<0.01), respectively for the cells with and without sanguinarine treatment. These results indicate that sanguinarine inhibited G1/S cell cycle progression and further supported the results from the proliferation assays (Figure 6C–6E).
Rac1b enhanced cell proliferation through anti-apoptotic and pro-proliferative mechanisms
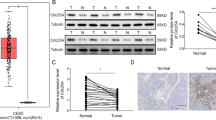
Anti-apoptosis and pro-proliferation are two potential mechanisms that Rac1b could use to promote the cell survival in serum-starved conditions. We first compared the intracellular levels of cleaved PARP-89 in the three cell lines following cell starvation for 4 d (Figure 7A and 7E). Compared with the control cells, PARP-89 levels significantly increased in the Rac1 cells (P<0.01) and decreased in the Rac1b cells (P<0.01). Compared with the Rac1 cells, PARP-89 levels significantly decreased in the Rac1b cells (P<0.01).
Changes in cleaved PARP-89 (A, C, E) and cyclin-D1 (B, D, F) in the three cell lines cultured in 0% serum in the presence (C, D) and absence (A, B) of sanguinarine. Figures A–D show Western blot results for PARP-89 and cyclin-D1. Figures E and F are quantified PARP-89 and cyclin-D1 results. n=3. bP<0.05, cP<0.01 both compared with Lenti-GFP. eP<0.05, fP<0.01 both compared with Lenti-Rac1-GFP. iP<0.01 compared with Rac1b cells without treatment. Mean±SEM.
Next, we checked the expression of cyclin-D1, a proliferation-related protein, in the three cell lines (Figure 7B and 7F). Compared with the control cells, cyclin-D1 also significantly increased in both the Rac1 cells (P<0.05) and the Rac1b cells (P<0.01).
Sanguinarine reversed the anti-apoptotic and pro-proliferative effects of Rac1b
We measured the levels of both PARP-89 and cyclin-D1 after sanguinarine treatment (1 μmol/L) for 4 d. Compared with the control cells, sanguinarine did not change PARP-89 levels in the Rac1 cells but remarkably increased PARP-89 levels in the Rac1b cells (P<0.05; Figure 7C and 7E).
As shown in Figures 7D and 7F, sanguinarine inhibited the cyclin-D1 levels in the Rac1b cells (P<0.01 compared with no treatment) but did not affect the cyclin-D1 levels in the Rac1 cells (P>0.05 compared with no treatment).
Discussion
In this study, our stable cell lines demonstrated a long-lasting but temperate upregulation of Rac1 or Rac1b and overcame all disadvantages of transient expression, such as low transfection efficiency, uncontrollable initial burst expression, and subsequent short-lasting duration. Thus, our cell lines are more suitable for the evaluation of cell proliferation, migration, and survival. We showed that all three cell lines demonstrated no significant changes in cell proliferation when cultured in the media containing 10% serum (Figure 4A). The variety of growth factors and cytokines in the serum could maximally stimulate both the endogenous Rac1 and the exogenously overexpressed Rac1/Rac1b to exert their effect on cell proliferation and could overcome any differences between the three cell lines.
In the case of serum-starvation, we found that cell proliferation increased in both the Rac1 and Rac1b cells compared with the control cells (Figure 4B and 4C). In addition, cells overexpressing Rac1b had a greater ability to survive compared with the cells overexpressing Rac1. These results indicate that Rac1b signaling contributed more than Rac1 signaling to cell survival in the growth-limiting condition. Our study also identified that both anti-apoptotic and pro-proliferative mechanisms were involved in promoting cell proliferation in these cell lines.
Serum-starvation in the culture medium could mimic nutrients shortage situations in vivo and could help us understand the mechanisms involved in tumorigenesis. In the tumor tissue, cancer cells usually encounter severe nutrient shortages due to vicious proliferation and the inappropriate formation of blood vessels. However, tumor cells with up-regulated Rac1b may partially survive this situation and thus greatly aggravate the process of the diseases. Our results support previous reports showing that up-regulated Rac1b can contribute to the tumor progression and metastasis6,16,17,18.
Our results vary slightly from the previous report by Matos et al19. They found that the transient over-expression of Rac1b, but not Rac1, was sufficient to promote 3T3 cell cycle progression and cell survival in very low serum (0.25% and 1%). However, in 0% serum, they found that both Rac1 and Rac1b cells could not survive. The inconsistencies may be due to the different cell types having different abilities to tolerate serum-starvation.
This study also found that sanguinarine possesses a selective inhibitory effect on proliferation in Rac1b cells, but not in Rac1 cells. Beausoleil et al recently demonstrated that the 19-amino acid insertion in Rac1b produces a large conformational change and generates a larger nucleotide-binding pocket, which is supposed to confer Rac1b selectivity20. This specific nucleotide binding inhibition towards Rac1b could block the anti-apoptotic downstream signaling. Previous studies showed that sanguinarine inhibits cell proliferation in various cancer cell lines by inhibiting cell cycling and by signaling apoptosis24,25,26. Our study further demonstrated that sanguinarine promoted apoptosis and inhibited cell proliferation by restricting G1/S cell cycle progression. However, it is still unknown why sanguinarine has such a narrow range of effective concentrations, even though the concentrations we used were similar to previous reports24,27.
Compared to sanguinarine, berberine has been shown to have a decreased ability to inhibit GTPase20. In accordance with nucleotide binding assays from a previous report20, berberine was ineffective at 1–3 μmol/L in our study. However, at 10 μmol/L berberine inhibited cell growth with similar potency in all three cell lines. Berberine may exert its anti-proliferative effect by pathways other than inhibition of Rac1 or Rac1b, such as by binding specifically to oligonucleotides to stabilize DNA triplexes or G-quadruplexes via telomerase or topoisomerase inhibition28,29.
Our results demonstrated that nascent Rac1b expression rendered cells a stronger ability to survive by utilizing anti-apoptotic and pro-proliferative pathways. Sanguinarine reversed both of these processes and is a drug discovery candidate for antineoplastics, particularly for malignant tumors with up-regulated Rac1b expression. Using several tumor cell lines with up-regulated expression of endogenous Rac1b we hope to confirm the Rac1b-dependent antineoplastic effect of sanguinarine.
Author contribution
Yue-peng WANG and Jun-li DUAN designed the research; Li YING, Gang LI, Si-si WEI, Hong WANG, Kai GUO, Qing ZHOU, Wei LI, Ying YU, Ji-min GAO, and Xian-jin LUO performed the experiments; Pei AN and Xun WANG analyzed the data; Li YING wrote the paper; Yue-peng WANG and Yi-gang LI revised the manuscript.
References
Jaffe AB, Hall A . Rho GTPases: Biochemistry and biology. Annu Rev Cell Dev Biol 2005; 21: 247–69.
Hall A . Rho family GTPases. Biochem Soc Trans 2012; 40: 1378–82.
Burridge K, Wennerberg K . Rho and Rac take center stage. Cell 2004; 116: 167–79.
Caron E, Hall A . Identification of two distinct mechanisms of phagocytosis controlled by different Rho GTPases. Science 1998; 282: 1717–21.
Schnelzer A, Prechtel D, Knaus U, Dehne K, Gerhard M, Graeff H, et al. Rac1 in human breast cancer: overexpression, mutation analysis, and characterization of a new isoform, Rac1b. Oncogene 2000; 19: 3013–20.
Jordan P, Brazao R, Boavida MG, Gespach C, Chastre E . Cloning of a novel human Rac1b splice variant with increased expression in colorectal tumors. Oncogene 1999; 18: 6835–9.
Karlsson R, Pedersen ED, Wang Z, Brakebusch C . Rho GTPase function in tumorigenesis. Biochim Biophys Acta 2009; 1796: 91–8.
Choi SS, Sicklick JK, Ma Q, Yang L, Huang J, Qi Y, et al. Sustained activation of rac1 in hepatic stellate cells promotes liver injury and fibrosis in mice. Hepatology 2006; 44: 1267–77.
Boettner B, Van Aelst L . The role of Rho GTPases in disease development. Gene 2002; 286: 155–74.
Schenck A, Bardoni B, Moro A, Bagni C, Mandel JL . A highly conserved protein family interacting with the fragile X mental retardation protein (FMRP) and displaying selective interactions with FMRP-related proteins FXR1P and FXR2P. Proc Natl Acad Sci U S A 2001; 98: 8844–9.
Keely PJ, Westwick JK, Whitehead IP, Der CJ, Parise LV . Cdc42 and Rac1 induce integrin-mediated cell motility and invasiveness through PI(3)K. Nature 1997; 390: 632–5.
Anand-Apte B, Zetter BR, Viswanathan A, Qiu RG, Chen J, Ruggieri R, et al. Platelet-derived growth factor and fibronectin-stimulated migration are differentially regulated by the Rac and extracellular signal-regulated kinase pathways. J Biol Chem 1997; 272: 30688–92.
Fiegen D, Haeusler LC, Blumenstein L, Herbrand U, Dvorsky R, Vetter IR, et al. Alternative splicing of Rac1 generates Rac1b, a self-activating GTPase. J Biol Chem 2004; 279: 4743–9.
Singh A, Karnoub AE, Palmby TR, Lengyel E, Sondek J, Der CJ . Rac1b, a tumor associated, constitutively active Rac1 splice variant, promotes cellular transformation. Oncogene 2004; 23: 9369–80.
Matos P, Collard JG, Jordan P . Tumor-related alternatively spliced Rac1b is not regulated by Rho-GDP dissociation inhibitors and exhibits selective downstream signaling. J Biol Chem 2003; 278: 50442–8.
Stallings-Mann M, Radisky D . Matrix metalloproteinase-induced malignancy in mammary epithelial cells. Cells Tissues Organs 2007; 185: 104–10.
Liu J, Lee W, Jiang Z, Chen Z, Jhunjhunwala S, Haverty PM, et al. Genome and transcriptome sequencing of lung cancers reveal diverse mutational and splicing events. Genome Res 2012; 22: 2315–27.
Silva AL, Carmo F, Bugalho MJ . RAC1b overexpression in papillary thyroid carcinoma: a role to unravel. Eur J Endocrinol 2013; 168: 795–804.
Matos P, Jordan P . Expression of Rac1b stimulates NF-κB-mediated cell survival and G1/S progression. Exp Cell Res 2005; 305: 292–9.
Beausoleil E, Chauvignac C, Taverne T, Lacombe S, Pognante L, Leblond B, et al. Structure–activity relationship of isoform selective inhibitors. Bioorg Med Chem Lett 2009; 19: 5594–8.
Wang YP, Zheng XR, Riddick N, Bryden M, Baur W, Zhang X, et al. ROCK isoform regulation of myosin phosphatase and contractility in vascular smooth muscle cells. Circ Res 2009; 104: 531–40.
Wang YP, Ei-Zaru MR EZ, Surks HK, Mendelsohn ME . Formin homology domain protein FHOD1 is a cyclic GMP-dependent protein kinase Ia binding protein and substrate in vascular smooth muscle cells. J Biol Chem 2004; 279: 24420–6.
Wang YP, Chen J, Wang Y, Taylor CW, Hirata Y, Hagiwara H, et al. Crucial role of type-1, but not type-3, inositol 1,4,5-trisphosphate (IP3) receptors in IP3-induced Ca2+ release, capacitative Ca2+ entry, and proliferation of A7r5 vascular smooth muscle cells. Cir Res 2001; 88: 202–9.
Adhami VM, Aziz MH, Mukhtar H, Ahmad N . Activation of prodeath Bcl-2 family proteins and mitochondrial apoptosis pathway by sanguinarine in immortalized human HaCaT keratinocytes. Clin Cancer Res 2003; 9: 3176–82.
Adhami VM, Aziz MH, Reagan-Shaw SR, Nihal M, Mukhtar H, Ahmad N . Sanguinarine causes cell cycle blockade and apoptosis of human prostate carcinoma cells via modulation of cyclin kinase inhibitor-cyclin-cyclin-dependent kinase machinery. Mol Cancer Ther 2004; 3: 933–40.
Malikova J, Zdarilova A, Hlobilkova A, Ulrichová J . The effect of chelerythrine on cell growth, apoptosis, and cell cycle in human normal and cancer cells in comparison with sanguinarine. Cell Biol Toxicol 2006; 22: 439–53.
Han MH, Kim GY, Yoo YH, Choi YH . Sanguinarine induces apoptosis in human colorectal cancer HCT-116 cells through ROS-mediated Egr-1 activation and mitochondrial dysfunction. Toxicol Lett 2013; 220: 157–66.
Maiti M, Kumar GS . Polymorphic nucleic acid binding of bioactive isoquinoline alkaloids and their role in cancer. J Nucleic Acids 2010; 2010: 1–23.
Bhadra K, Kumar GS . Therapeutic potential of nucleic acid-binding isoquinoline alkaloids: Binding aspects and implications for drug design. Med Res Rev 2010; 31: 821–62.
Acknowledgements
This study was supported by grants to Yue-peng WANG from the Welcome Trust for New Principal Investigators of Xinhua Hospital, the Natural Science Foundation of Zhejiang Province (Y2101019), the National Natural Science Foundation of China (NSFC; No 81170302 and 81370257), and the Pujiang Project for Extraordinary Scientists of the Science and Technology Commission of Shanghai Municipality (12PJ1406400); by grants to Jun-li DUAN from the NSFC (No 11374213); by grants to Yi-gang LI from the NSFC (No 81270258); and by grants to Li YING from the Innovation Fund for PhD Candidate at SJTU School of Medicine (BXJ201223).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Ying, L., Li, G., Wei, Ss. et al. Sanguinarine inhibits Rac1b-rendered cell survival enhancement by promoting apoptosis and blocking proliferation. Acta Pharmacol Sin 36, 229–240 (2015). https://doi.org/10.1038/aps.2014.115
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2014.115