ABSTRACT
Characterising the mechanisms of cell death following focal cerebral ischaemia has been hampered by a lack of an in vitro assay emulating both the apoptotic and necrotic features observed in vivo. The present study systematically characterised oxygen-glucose-deprivation (OGD) in primary rat cortical neurones to establish a reproducible model with components of both cell-death endpoints. OGD induced a time-dependent reduction in cell viability, with 80% cell death occurring 24 h after 3 h exposure to 0% O2 and 0.5 mM glucose. Indicative of a necrotic component to OGD-induced cell death, N-methyl-D-aspartate (NMDA) receptor inhibition with MK-801 attenuated neuronal loss by 60%. The lack of protection by the caspase inhibitors DEVD-CHO and z-VAD-fmk suggested that under these conditions neurones did not die by an apoptotic mechanism. Moderating the severity of the insult by decreasing OGD exposure to 60 min did not reduce the amount of necrosis, but did induce a small degree of apoptosis (a slight reduction in cell death was observed in the presence of 10 μM DEVD-CHO). In separate experiments purported to enhance the apoptotic component, cells were gradually deprived of O2, exposed to 4% O2 (as opposed to 0%) during the OGD period, or maintained in serum-containing media throughout. While NMDA receptor antagonism significantly reduced cortical cell death under all conditions, a caspase-inhibitor sensitive component of cell death was not uncovered. These studies suggest that OGD of cultured cortical cells models the excitotoxic, but not the apoptotic component of cell death observed in vivo.
Similar content being viewed by others
INTRODUCTION
The involvement of apoptotic cell death alongside necrosis within in vivo models of focal cerebral ischaemia has been observed in a number of reports over the last few years1,2,3,4,5,6,7,8 with only a few animal studies failing to find apoptotic indices9, 10. The potential for therapies targeted against it have driven the investigations to elucidate the cascade of events which characterises apoptosis associated with ischaemia11,12,13. Complementary studies examining similar phenomena in vitro would be hugely beneficial to progress in this area, as well as potentially providing means for the screening of compounds by the pharmaceutical industry. However, converting the in vivo ischaemia model with facets of apoptosis and necrosis, into a culture dish have proved less than straight forward. While some studies have suggested indications of apoptosis14,15,16 following combined oxygen-glucose-deprivation (OGD) in vitro, it has yet to be properly characterized.
The objective of the current study was to examine the cell death processes of OGD in rat cerebrocortical neurone cultures, exposing both necrotic and apoptotic components corresponding to that which is reported to occur in the salvageable (penumbral) regions of the ischaemic brain in vivo17. A systematic approach was employed, characterising OGD cell death before modifying aspects of the protocol and the severity of the insult. The study is comprehensive in its conclusion that OGD is a good model of the excitotoxic, but not the apoptotic constituent of cell death in cortical cultures.
MATERIALS AND METHODS
Primary culture
Primary cultures of rat cerebrocortical neurones were prepared using a method adapted from Pauwels et al18. Briefly, the cortices from embryonic day 17 Sprague-Dawley rats were dissociated for 12 min in Hank's Balanced Salt Solution (HBSS without Ca2+ and Mg2+) containing 0.09% trypsin and 500 IU/ml DNase, triturated in HBSS containing 500 IU/ml DNase and plated out at 1600 cells/mm2 in Neuronal Plating Medium (containing 5 % heat-inactivated horse serum, 5% heat-inactivated foetal bovine serum) onto poly-D-lysine-coated 15 mm wells. After 24 h, the medium was replaced with fresh, serum-free B27 medium. The neuronal cultures were further purified by treatment with cytosine arabinoside 5 μM at 5-7 d in vitro (DIV) to give cultures that were reliably 99% (B27-treated) or 98% (NCDM-treated) neuronal (as determined by GFAP positive and negative cell counts; data not shown). Thereafter the medium was partly refreshed twice weekly. Unless otherwise indicated, cultures were used for experimentation at 11-15 DIV. Care of all animals was in accordance with the UK Animals (Scientific Procedures) Act 1986.
Caspase activity
Cells were collected and pelleted in ice-cold phospho-buffered saline (PBS). Drained pellets were extracted in 25 μl extraction buffer (10 mM HEPES-KOH pH 7.4; 50 mM KCl, 2 mM MgCl2, 5 mM EGTA; 0.5% CHAPS; 1 mM phenylmethylsulphonyl fluoride (PMSF); 10 μg/ml pepstatin A, leupeptic, aprotinin; 1 mM dithiothreital (DTT)) on ice for 20-30 min followed by a freeze-thaw cycle. Nuclear and insoluble material was removed by centrifugation (30 min, 10,000 rpm at 4°C). Supernatants were diluted (1:8) with dilution buffer (25 mM HEPES-KOH pH 7.4; 50 mM NaCl; 5 mM EGTA; 0.1% CHAPS; 10 mM DTT; 10% sucrose) and protein concentration determined. Caspase activity was assayed using 20 μM fluorescent aminomethylcoumarin-peptide substrates (Peptide Institute Inc., Japan) for caspase-1-like (Ac-YVAD-AMC) and caspase-3-like (Ac-DEVD-AMC) enzymes. Inhibition of respective enzyme activities was assessed using 200 nM reversible aldehyde inhibitors Ac-YVAD-CHO or Ac-DEVD-CHO, for caspase-1-like and caspase-3-like enzymes respectively. Extracts were also made from cultures that had not had any treatment in order to determine whether there was any caspase activation in control cultures at various stages. Except where stated the protein concentration of the extracts were determined using a bicinchoninic acid (BCA) protein assay Kit (Pierce) and the concentration adjusted.
NMDA-induced neurotoxicity
Cultures were exposed to NMDA (10−4M, Tocris) in HEPES-buffered saline (mM: NaCl 51.3; KCl 5.4; glucose 25; HEPES 20; CaCl2 1.8; glycine 0.01; pH 7.3) for 30 min after which time the cells were returned to complete culture medium (containing B27) for a further 23 h. Drugs or appropriate vehicles were present throughout. At the end of the 24 h period, cell viability was assessed by determination of lactate dehydrogenase extrusion (LDH) using the Promega Cytotox 96® non-radioactive cytotoxicity assay (as per instructions). Colour change was detected with a Dynex Technologies MRX spectrophotometer plate reader.
Staurosporine-induced neurotoxicity
Staurosporine (STS) was made up in dimethylsulphoxide (DMSO) and then diluted into NCDM, so that the final concentration of DMSO was 0.1%. Cultures were exposed to STS (10−8-10−5M) for 24 h after which time cell survival was assessed by the reduction of 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrasolium bromide (MTT) to a coloured formazan product by viable cells. MTT (Sigma, UK) was added to the cell to give a final concentration of 0.3 mg/ml and incubated at 37°C for 2-4 h in a humidified 95%/5% O2/CO2 atmosphere. 100 μl isopropanolol/0.04 N HCl was added before measured on a Dynex Technologies MRX spectrophotometer plate reader (at 570 nm with a reference wavelength of 630 nm). Assessment of caspase activation (as an indicator of apoptotic cell death) was carried out using cell extracts from cultures exposed to STS or vehicle.
Oxygen-glucose deprivation
Cultures were exposed to a variety of ischaemic-like conditions (oxygen-, glucose- or combined oxygen-glucose-deprivation) for various time periods. All experiments were conducted in Neurobasal medium supplemented with 0.5 mM L-glutamine. For normog-lycaemic conditions the cells were maintained in media containing 25 mM glucose. For experiments requiring aglycaemic media, the glucose concentration was either 0.5 or 0 mM (as stated for each experiment). If required, appropriate solutions were made anoxic by placing them into an anaerobic workstation (don Whitley Scientific MACS VA set to run under anaerobic conditions with 5% CO2 at 37°C) and bubbling with 95% N2/5% CO2 for at least 30 min. Wells were washed with 0.5 ml of the appropriate medium and then incubated with 0.25 ml of the appropriate medium for the time periods indicated in either the anaerobic workstation (oxygen- and combined oxygen-glucose-deprived cells) or the normoxic incubator (control and glucose-deprived cells). At the end of the appropriate period, the cultures were removed from the respective incubator and media replaced with normoglycaemic media. The cells were placed in the normoxic incubator for the remainder of the recovery period. For MAP-2 immunostaining, cells were fixed in paraformaldehyde-lysine phosphate buffered (PLP) fixative for 20-30 min prior to 0.25% Triton permeabilisation. Cells were incubated in MAP-2 primary antibody (Santa-Cruz, USA) at 1:100 for 2 h. After washing in PBS FITC labelled secondary antibody (FITC-conjugated anti-mouse IgG; Santa-Cruz, USA) was added at 1:64 dilution. Fluorescence was read with a Labsystems Fluoroskan Ascent plate reader.
Gradual oxygen deprivation
In the experiments described above, exposure to oxygen-deprivation was carried out by exchanging the medium of experimental cultures with previously de-oxygenated medium so that deprivation was instantaneous. In this gradual deprivation experiment however, oxygen depletion was allowed to occur over time by placing the cells (in 25 mM glucose-containing Neurobasal medium plus appropriate drugs or vehicles) into the anaerobic incubator without any exchange of medium for 6 h. The plates were then removed to the normoxic incubator and allowed to recover for 48 h. Viability was assessed as before.
Drug treatment
Cultures were pre-treated for 30 or 90 min with drug or vehicle in normoxic Neurobasal medium containing 25 mM glucose. The cultures were then exposed to various oxygen and glucose conditions for periods of time after which they were returned to normoxic (20% O2)/normoglycaemic (25 mM glucose) medium for 24 h. Drugs or vehicles were present throughout the exposure and recovery periods.
(+)-5-methyl-10,11-dihydro-5H-dibenzo[a,d] cyclohepten-5, 10-imine maleate (MK-801) and D(−)-2-amino-5-phosphonopentanoate (D-AP5; Tocris) were dissolved in sterile purified water prior to dilution into Neurobasal medium.
6, 7-dichloroquinoxaline-2, 3-dione (CNQX; Tocris), DEVD-CHO (cell permeable form, Calbiochem) and z-VAD-fmk (Enzyme Systems Products) were dissolved in anhydrous DMSO. Final concentrations of DMSO in experimental solutions were 0.05, 0.5 and 1% respectively.
RESULTS
NMDA-induced neurotoxicity
30 min exposure of N-methyl-D-aspartate (NMDA; 10−4M) to rat cortical neurones induced excitotoxic cell death over the following 24 h. Pre-treatment with the NMDA receptor antagonist, MK801 (>3×10−8M) produced complete inhibition of NMDA-induced neurotoxicity (Fig 1).
Pharmacological modification of NMDA-induced neurotoxicity in cultured rat cortical neurones. Cultures of rat cerebrocortical neurones (7 DIV; maintained in B27 medium) were pre-treated for 30 min with the compounds indicated prior to a 30 min exposure to 10−4M NMDA. Following NMDA exposure, the cultures were returned to complete culture medium for a further 24 h. MK-801 was present throughout exposure and recovery periods. Cell death was assessed by measurement of LDH extrusion into the culture medium. *Value significantly different from control (one-way ANOVA on Rank's with post hoc Dunn's test, p<0.05).
Staurosporine-induced neurotoxicity
Staurosporine (STS) is a broad-based inhibitor of protein kinase C (PKC), which induces apoptosis in a wide variety of cell types including cerebrocortical neurones19. As can be seen in Fig 2, both STS (3×10−7 and 10−6M) and the vehicle (0.1% DMSO) induced caspase activation of the caspase-3-like (but not the caspase -1-like) family as evidenced by cleavage of Ac-DEVD-AMC substrate but not Ac-YVAD-AMC substrate. It should be noted that for these studies, although equivalent cell numbers were present at the start of the experimental period, it is possible that non-equivalent cell numbers were recovered and extracted at the end of the experimental period (i.e. STS treatment will have resulted in cell death, and according to the stage of cell death, fewer cells may have been recovered). In all further studies, enzyme activities was normalised to protein content of the extract, but as this required a protein assay able to withstand the constituents of the extraction buffer, this was not able to be performed for the present study.
Stimulation of capase activity in rat cerebrocortical neurones by staurosporine and DMSO. Rat cortical neurones (11 DIV) were exposed to either 0.1% DMSO or staurosporine (STS) for 24 h. Cells were then extracted and assayed for caspase activity of (A) caspase-1-like family (using Ac-YVAD-AMC) or (B) caspase-3-like family (using Ac-DEVD-AMC).
Effect of glucose concentration and exposure time on anoxia-induced cell death
Dose-response relationships between glucose concentration revealed that the cultures could withstand exposure to glucose levels down to 0.5 mM for up to 3 h without loss of viability (data not shown). Rat cortical cultures were subsequently exposed to either 0, 0.5 or 25 mM glucose-containing Neurobasal medium in either normoxic (20% oxygen) or anoxic (0% oxygen) conditions for various times (Fig 3A, B). Under these conditions of varying glucose and oxygen levels, it appeared that the cultures were more sensitive to the removal of glucose than they were to the removal of oxygen -- exposure to 0 mM glucose produced profound cell death following exposure times as short as 3 h regardless of whether oxygen had been removed or not (Fig 3A). In contrast, removal of oxygen under conditions of normoglycaemia (Fig 3C) produced cell death that differed very little from normoxic controls. From this data a 3 h exposure to 0.5 mM glucose and 0% oxygen was chosen for subsequent studies as this appeared to produce a loss of viability of approximately 50%.
Glucose concentration and anoxia-induced cell death in cultured rat cortical neurones. Rat cortical cultures were exposed to 0 (A), 0.5 (B) or 25 mM (C) glucose-containing Neurobasal Medium in either normoxic (20% oxygen) or anoxic (0% oxygen) conditions for the periods indicated. Following the exposure, cultures were returned to 25 mM glucose-containing, normoxic medium for a remainder of 24 h period, after which time viability was assessed by means of a MTT assay. Results shown are means ± SD of 3 independent experiments comprising 14 wells in total.
Caspase activity following 3 h OGD treatment
Rat cortical neurones were exposed to combined oxygen-glucose deprivation for 3 h (0% O2, 0.5 mM glucose). The cultures were then returned to normoxic, normog-lycaemic medium. Cells were harvested, extracted and assayed for group II caspase activity 0, 3, 8 and 24 h later (Fig 4).
DEVD-AMC cleavage activity in cultured rat cortical neurones after 3 h OGD. Rat cortical cultures were exposed to 0.5 mM glucose and 0% oxygen for 3 h and then returned to 25 mM glucose, 20% oxygen for a further 21 h. At the times indicated, cells were harvested and cytosolic extracts were made. The cell extracts were assayed for group-2 caspase activity by measuring the cleavage of the fluorogenic substrate Ac-DEVD-AMC. Results shown represent means ± SE of 3 separate experiments (comprising 9 data points in total). *Value significantly lower than the 0 h (control/untreated) group (One-way ANOVA with post-hoc Dunnett's test, p<0.05). A1.1 = extract from dexamethasone-treated A1.1 cells.
The activity of caspase-3-like caspases did not increase with 3 h OGD (compared to the untreated cells extracted at 0 h), producing instead a slight decrease at 24 h. However, this result should be interpreted with caution as the activity in all extracts was similar in magnitude to that observed in dexamethasone-treated A1.1 cell extracts (used as a positive control in this system and thus regarded as substantial activity). The reason for these high group II caspase activities in rat cerebrocortical cultures is not clear, but could be due to ongoing cell death occurring in this primary culture system. Previous experiments with these cultures have shown similarly high baseline levels of caspase activity even in cultures that had undergone no treatments (including sham washes; data not shown).
Effect of MK801, DEVD-CHO and z-VAD-fmk on 3 h OGD treatment
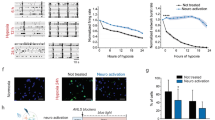
Exposure to 0.5 mM glucose, 0% oxygen for 3 h produced approximately 80% cell loss (assessed using microtubule-associated protein-2 (MAP-2) immunohistochemistry after 24 h; Fig 5). Addition of the NMDA receptor antagonist MK-801 (10−8-10−6M) 90 min prior to the onset of OGD significantly attenuated neuronal loss at the two higher concentrations (Fig 5). In contrast, neither the broad acting caspase inhibitor z-VAD-fmk (10−5-10−4M; Fig 8), nor the specific group II caspase inhibitor DEVD-CHO (10−7-10−5M; Fig 5) had any effect. Similar results for MK-801 and the caspase inhibitors were observed when the MTT assay replaced MAP-2 immunohistochemistry as an end-point (data not shown).
Pharmacological modification of 3 h OGD-induced cortical cell death. Rat cortical cultures were pre-treated for 90 min with drug or vehicle as indicated prior to a 3 h exposure to 0.5 mM glucose, 0% oxygen. Following the exposure period cells were returned to 25 mM glucose-containing, normoxic medium for 24 h. Drugs or vehicles were present throughout the exposure and recovery periods. At the end of the recovery period viability was assessed by fluorescence quantification of FITC-linked MAP-2 immunohistochemistry. Results shown represent means ± SE of 2 independent experiments comprising 5-9 wells in total. *Value significantly greater than OGD group (Kruskal-Wallis ANOVA on ranks with post-hoc Dunn's test, p<0.05).
Cortical neurone viability under 4% oxygen with or without glucose deprivation. (A) Rat cortical cultures were exposed to 0, 0.5, 1 or 25 mM glucose-containing Neurobasal medium in 4% O2 for the times indicated. They were then returned to normoxic, 25 mM glucose-containing Neurobasal for the remainder of a 24 h period after which viability was assessed as previously described. Results shown represent means ± SE of 3 experiments (16-18 wells). (B) Cultures were pre-treated with the drugs indicated (where DEVD=DEVD-CHO and zVAD = z-VAD-fmk) for 30 min prior to 3 h exposure to 4% O2 in glucose-free Neurobasal. Following the exposure period, cultures were returned to normoxic, normoglycaemic Neurobasal for 48 h prior to assessment of viability as previously described. Drugs were present throughout the exposure and recovery periods. Results show means ± SE of 6-23 wells. *Value significantly greater than OGD group (Kruskal Wallis ANOVA on ranks with post-hoc Dunn's test, p<0.05).
Effects of DEVD-CHO, z-VAD-fmk or D-AP5 on 60 min OGD treatment
Decreasing the duration of OGD (0% O2, 0.5 mM glucose) to 60 min consistently produced a 40-60% loss of neuronal viability (as measured by the fluorescence quantification of fluorescein isothiocyanate- (FITC-) linked MAP-2 immunohistochemistry after 24 h; Fig 6A-C). Similarly to the previous experiment, the addition of an NMDA receptor antagonist (D-AP5) significantly prevented cell loss (Fig 6A). The caspase inhibitor, z-VAD-fmk (10−5-10−4M) again had no effect, while the group II caspase inhibitor, DEVD-CHO (cell permeable form) produced a significant but small effect at the highest dose examined (10−5M; Fig 6B, C).
Pharmacological modification of 60 min OGD-induced cell death in cultured rat cortical neurones. Rat cortical cultures were pre-treated for 90 min with different concentrations of (A) D-AP5, (B) Z-VAD-fmk and (C) DEVD-CHO prior to a 60 min exposure to 0.5 mM glucose, 0% oxygen. Following the exposure, cells were returned to 25 mM glucose-containing, normoxic medium for 24 h. Drugs or vehicles were present throughout the exposure and recovery periods. At the end of the recovery period, viability was assessed by means of fluorescence quantification of FITC-linked MAP-2 immunohistochemistry. Results shown represent the means ± SE of 6 wells. *Value significantly greater than OGD group (A: Kruskal Wallis ANOVA on ranks with post-hoc Dunnett's test, p<0.05; B-C: One-way ANOVA with post-hoc Tukey test, p<0.05) **Value significantly lower than OGD group (One-way ANOVA with post-hoc Tukey test, p<0.05).
Gradual oxygen deprivation
Gradual exposure to oxygen (but not glucose) deprivation for 6 h produced a 75-80% loss of viability at 48 h (Fig 7). This loss of viability was prevented by those compounds acting at excitatory amino acid receptors (MK801: 10−8-10−6M, D-AP5: 10−5-10−4M and CNQX: 10−7-10−5M), but not by the caspase inhibitors (DEVD-CHO: 10−7-10−5M, z-VAD-fmk: 10−5-10−4M, Fig 7).
Pharmacological modification of cell viability after 6 h gradual oxygen deprivation in cultured rat cortical neurones. Cultures of rat cortical neurones were pre-treated for 30 min with the drugs indicated (where DEVD = DEVD-CHO and zVAD = z-VAD-fmk) prior to gradual exposure to 0% O2. No further medium exchanges or washes were carried out following this addition of drug-containing medium throughout the remainder of the experiment. Following 6 h exposure, the cultures were removed to a normoxic incubator and allowed to recover for 48 h. Viability was then assessed using MAP-2 immunohistochemistry. Results shown represent the means ± SE of 2-4 experiments comprising 12-24 wells. *Value significantly greater than OGD group (Kruskal Wallis ANOVA with post-hoc Dunn's test, p<0.05)
Effect of 4% oxygen on viability of cortical neurones
Cultures were exposed to 0, 0.5, 1 or 25 mM glucose-containing Neurobasal medium in hypoxic (4% oxygen) conditions for various times. Following the exposure period, cultures were returned to 25 mM glucose-containing, normoxic medium (20% O2) for the remainder of a 24 h period, after which time viability was assessed by means of fluorescence quantification of FITC-linked MAP-2 immunohistochemistry.
Exposure to 4% oxygen produced a loss of viability at 24 h only if carried out in glucose-free medium (Fig 8A). Under these conditions, viability was reduced to 40% of control cultures following a 3 h exposure (exposure to 0 mM glucose for 3 h did not produce a loss of viability in normoxic cultures) and total loss of viability was produced following a 6 h exposure. However, in cultures where glucose was present (even as low as 0.5 mM), no neuronal death occurred in response to exposure to 4% oxygen.
The effects of drugs (MK801: 10−8-10−6M, DEVD-CHO: 10−7-10−5M or z-VAD-fmk: 10−5-10−4M) against a 3 h exposure to 4% oxygen, 0 mM glucose were also studied (Fig 8B). Cultures were pre-treated for 30 min prior to OGD and were allowed to recover in normoxic, normoglycaemic Neurobasal medium for 48 h after exposure (drugs were present throughout). Exposure to 4% oxygen and 0 mM glucose did not uncover any apoptotic component to OGD-induced cell death as again only MK801 significantly attenuated cell death.
Effect of serum on viability of cortical neurones
The presence of serum during OGD period (4% O2, 0 mM glucose) prolonged neuronal viability (Fig 9A). With the addition of dialysed serum the 40% loss of viability observed with control cultures (without serum) after 3 h OGD was reduced to <10%. Nearly 6 h of OGD was required for serum-containing cultures to produce a comparable loss of viability.
The viability of cultured rat cortical neurones and serum deprivation. (A) Rat cortical neurone cultures were exposed to 0 mM glucose containing Neurobasal medium in either the presence or absence of serum in hypoxic (4% O2) conditions for the times indicated. They were returned to normoxic, 25 mM glucose-containing Neurobasal medium for the remainder of a 24 h period after which time viability was assessed by means of MAP-2 immunohis-tochemistry. Results shown are means±SE of 3 separate experiments comprising 12-24 wells in total. (B) Cultures were pre-treated with the drugs indicated (where DEVD = DEVD-CHO and zVAD = z-VAD-fmk) for 30 min prior to 6 h exposure to 4% O2 in glucose-free Neurobasal medium. Following the exposure period, cultures were returned to normoxic, normoglycaemic Neurobasal for 24 h prior to assessment of viability as previously described. Drugs were present throughout the exposure and recovery periods. Results show means ± SE of 6-24 wells. *Value significantly greater than OGD group (One-way ANOVA with post-hoc Dunnett's test, p<0.05).
The effect of NMDA receptor antagonists and caspase inhibitors against a 6 h exposure to 4% oxygen, 0 mM glucose in the presence of dialysed serum were also studied to observe whether this modification would affect a relative increase in apoptotic cell (Fig 9B). The addition 30 min prior to OGD of MK-801 (10−8-10−6M) significantly prevented the 50%. However, neither of the caspase inhibitors, DEVD-CHO (10−7-10−5M) or z-VAD. fmk (10−6 -10−4M), prevented the loss of cell viability. Similar results were observed if the exposure time was extended to 8 h, although extending the OGD exposure to 16 h resulted in the failure of even MK-801 to prevent the cell death (data not shown).
DISCUSSION
Recent studies have demonstrated that following an episode of stroke-like focal cerebral ischaemia in vivo, neurones die by both apoptotic and necrotic mechanisms17, 20, 21. In middle cerebral artery (MCA) occlusion (the most common occlusion in stroke patients), the epicentre of the insult is the striatum, an area in the core of the MCA blood supply territory. In animal models, neurones within this region predominantly necrose 24 to 48 h after the occlusion of the blood vessel22, 23. The cortical region at the fringes of the MCA territory, with limited ancillary microvascular perfusion of nutrients from surrounding tissue24,25,26, has been shown in some studies to provide an environment in which apoptosis can predominate3,4,5,6,7, 11, 12, 27. From a therapeutic viewpoint, these apoptotic cortical neurones provide the greatest opportunity for intervention and a number of studies have examined the efficacy of compounds targeted against the apoptotic cascade8, 28, 29. However, despite the versatility cortical cell culture offers in expanding the understanding of the ischaemic process or in screening for potential compounds, there is to date no consistent, chara-cterised model of focal cerebral ischaemia in vitro with both an apoptotic and necrotic component.
The aim of this work was to characterise an in vitro protocol using oxygen-, glucose- or combined oxygen-glucose-deprivation to mimic the mechanisms of neuronal cell death observed in focal stroke models. To ensure parity with in vivo focal models, the cultures were established from cerebrocortical tissue. With the inherent differences between cortical and hippocampal sensitivity to ischaemia30,31,32, utilising undifferentiated forebrain cultures containing both hippocampal and cortical neurones to elucidate focal cerebral ischaemic pathophysiology, would be unlikely to provide an accurate representation of the in vivo disorder. This is highlighted by Bossenmeyer-Pourie et al33, 34 who showed that 6 h of hypoxia (without any glucose reduction) was sufficient to induce apoptosis in 20-25% of the cells in forebrain culture after 96 h. During this time-period, necrosis only increased by 10-15%, a profile much more reminiscent of a global/hippocampal model of ischaemia33, 34.
Initial experiments were designed to establish controls for both neuronal necrosis (excitosis) and apoptosis (Fig 1). NMDA was added to cultures to produce a purely excitotoxic form of cell death. As expected35, 36 cell viability was maintained in these cultures with the addition of the NMDA receptor antagonist, MK-801. MK-801 as well as AP5 used in later experiments, have both been shown to be good markers of glutamate-mediated excitotoxic cell death37,38,39,40. Staurosporine was utilised to induce an insult likely to be apoptotic in nature19 in order to determine appropriate ways of assaying apoptosis in these cerebrocortical cells. Staurosporine-induced cell death corresponded with the activation of caspase-3-like caspases involved in the apoptotic cascade, but not those associated with the inflammatory response (caspase-1-like caspases, Fig 2).
Initial glucose-only deprivation showed that cortical cells could withstand low glucose concentrations for a sustained period (data not shown). However, with the combined absence of oxygen, 0.5 mM glucose produced a reproducible loss of 40-60% of the neurones after a 3 h exposure (Fig 3). This exposure time correlates well with in vivo studies which routinely use an occlusion period of 2-3 h to induce infarction28, 41,42,43. However, this insult did not directly increase the activity of group II caspases (Fig 4), although again a high background was observed in control A1.1 cell extracts. The caspase-specific inhibitors (the group II inhibitor DEVD-CHO and the broad spectrum caspase inhibitor z-VAD-fmk) also failed to uncover a caspase component (Fig 5). Caspase inhibitors were deliberately chosen as a less robust marker of apoptosis than for example morphology. Caspase inhibitors (such as z-VAD) have previously been shown to be able to discriminate between apoptosis and NMDA-mediated necrosis44 and caspase-3 activity has been tightly linked to both DNA fragmentation and cell shrinkage45. However, some caspase activity (amenable to caspase inhibition) has been observed in necrotic cells under certain conditions45. Morphological analysis of cellular appearance is therefore a crucial tool to confirm the presence of apoptosis. However, due to the lack of apoptosis observed during OGD in this study using less robust pharmacological tools, confirmation (of a non-occurring event) was not required.
Reducing the OGD exposure time to 60 min did provide conditions in which DEVD-CHO (but not z-VAD-fmk) displayed slight protection (Fig 6). The NMDA receptor antagonists used (either MK-801 or D-AP5) sustained neuronal viability under both conditions (Fig 5, 6). This suggests that both long and short exposure to OGD conditions produce an NMDA receptor-mediated excitotoxic insult with only a small apoptotic component at the shorter exposure time.
Neuronal death produced under the conditions above (0% oxygen, 0.5 mM glucose) was fairly rapid (within 24 h) and may therefore be representative of the cell death occurring within the core of an infarct rather than the more slowly evolving death one might expect to observe in the 'penumbral' region in vivo. In a subsequent study the objective was to modify the model to simulate the cell death that may occur in the salvageable regions of an ischaemic brain and exacerbate the apoptotic component of cell death. To this effect the severity of the insult was moderated using gradual oxygen deprivation (Fig 7) or 4% oxygen rather than 0% oxygen (Fig 8). As with previous experiments, the 80% loss of viability associated with a gradual loss of O2 over a 6 h exposure period was prevented by those compounds acting at excitatory amino acid receptors (MK801, D-AP5 and CNQX). However, no effect was apparent with caspase inhibitors. Similar results were obtained in cultures maintained at 4% O2 for the duration of OGD.
As use of in vitro models of hypoxic cell death has been criticised on the grounds that the culture medium used for these studies lacks the Ca2+ buffering capacity of the normal physiological milieu, exaggerating hypoxic damage46, approaches were taken to reduce the severity of the insult by maintaining serum in the medium throughout the OGD period (Fig 9). Again the NMDA receptor antagonist MK-801, but neither of the caspase inhibitors prevented the loss of viability.
In the above studies, systematic alterations of the OGD protocol did not reveal a large apoptotic component to oxygen-glucose-deprived cell death in cortical neurones. Modification of the severity insult designed to induce a protracted process of cell death also did not uncover an apoptotic component observed by other studies.
Of the literature observing OGD-induced apoptosis in cortical cells, most have used the characteristic fragmentation of DNA as the sole apoptotic indicator14, 16. However, similar OGD experiments on other CNS cell types have highlighted the unreliability of nuclear frag-mentation, without either morphological endorsement or caspase activity, as a measurement of apoptosis per se47, 48. Out with the confines of cell culture, other fields also have cautionary note on Terminal deoxynucleotidyl transferase-mediated biotin-dUTP nick-end labelling (TUNEL) specificity49,50,51,52, arguing against its role as the sole determinant of the presence of apoptosis.
A number of studies utilising ultrastructural or morphological indicies have failed to show apoptotic characteristics after 5555 or 6053, 54 min of OGD. Increasing OGD duration to 100 min in a similar mixed culture also did not give rise to any propidium-stained apoptotic cells56. Studies utilising caspase activation as an indication of apoptotic cell death, have also failed to demonstrate any increases in activity after either 6053 or 150 min57 exposure to OGD. Another study which analysed apoptotic cell death using TUNEL combined with morphological analysis after 30-90 min exposure to OGD, found only a tiny proportion of the cells (0.05 %) underwent apoptosis by 48 h58.
Gwag et al15 has observed an increase in OGD-induced apoptosis following blockade of glutamate receptors, with MK-801 combined with CNQX both protecting cells and 'unmasking' an apoptotic component to cell death. However, without suitable controls, this increase in cell loss may simply be due to the known apoptosis-inducing ability of MK-801 itself shown by both Hwang et al59 and Seo et al60. In the same study, Seo et al60 observed that protection of cortical cells after 120 min OGD with complestin (a blocker of the glutamate receptor-mediated ionic influx rather than the receptor itself), did not result in a secondary loss of viability at the later time-point.
The systematic in vitro approach employed by this study to characterise cell death following a period of OGD suggests that pure neuronal cortical cultures are liable to die exclusively by necrotic mechanisms. While this is in contrast to the in vivo situation of focal cerebral ischaemia, it is perhaps not surprising, due to the differences between the culture plate and the whole animal (such as the in vivo inflammatory response61, 62 not replicated in vitro). It may ultimately be these differences between culture plate and whole animal systems that provide the insight into the nascence of the apoptotic cascade in vivo.
References
Charriaut-Marlangue C, Remolleau S, Aggoun-Zouaoui D, Ben-Ari Y . Apoptosis and programmed cell death: a role in cerebral ischemia. Biomed Pharmacother 1989; 52:264–9.
Davoli MA, Fourtounis J, Tam J, et al. Immunohistochemical and biochemical assessment of caspase-3 activation and DNA fragmentation following transient focal ischemia in the rat. Neurosci 2002; 115:125–36.
Krupinski J, Lopez E, Marti E, Ferrer I . Expression of caspases and their substrates in the rat model of focal cerebral ischemia. Neurobiol Dis 2000; 7:332–42.
Le DA, Wu Y, Huang Z, et al. Caspase activation and neuro-protection in caspase-3- deficient mice after in vivo cerebral ischemia and in vitro oxygen glucose deprivation. Proc Natl Acad Sci USA 2002; 99:15188–93.
Li Y, Chopp M, Jiang N, Yao F, Zaloga C . Temporal profile of in situ DNA fragmentation after transient middle cerebral artery occlusion in the rat. J Cereb Blood Flow Metab 1995; 15:389–97.
Li Y, Chopp M, Jiang N, Zhang ZG, Zaloga C . Induction of DNA fragmentation after 10 to 120 min of focal cerebral ischemia in rats. Stroke 1995; 26:1252–8.
Linnik MD, Miller JA, Sprinkle-Cavallo J, et al. Apoptotic DNA fragmentation in the rat cerebral cortex induced by permanent middle cerebral artery occlusion. Mol Brain Res 1995; 32:116–24.
Wiessner C, Sauer D, Alaimo D, Allegrini PR . Protective effect of a caspase inhibitor in models for cerebral ischemia in vitro and in vivo. Cell Mol Biol 2000; 46:53–62.
DeGirolami U, Crowell RM, Marcoux FW . Selective necrosis and total necrosis in focal cerebral ischemia. Neuropathologic observations on experimental middle cerebral artery occlusion in the macaque monkey. J Neuropathol Exp Neurol 1984; 43:57–71.
van Lookeren Campagne M, Gill R . Ultrastructural morphological changes are not characteristic of apoptotic cell death following focal cerebral ischaemia in the rat. Neurosci Lett 1996; 213:111–4.
Asahi M, Hoshimaru M, Uemura Y et al. Expression of inter-leukin-1 beta converting enzyme gene family and bcl-2 gene family in the rat brain following permanent occlusion of the middle cerebral artery. J Cereb Blood Flow Metab 1997; 17:11–8.
Plesnila N, Zinkel S, Amin-Hanjani S, et al. Function of BID -a molecule of the bcl-2 family- in ischemic cell death in the brain. Eur Surg Res 2002; 34:37–41.
Velier JJ, Ellison JA, Kikly KK, et al. Caspase-8 and caspase-3 are expressed by different populations of cortical neurons undergoing delayed cell death after focal stroke in the rat. J Neurosci 1999; 19:5932–41.
Bruer U, Weih MK, Isaev NK, et al. Induction of tolerance in rat cortical neurons: Hypoxic preconditioning. FEBS Lett 1997; 414:117–21.
Gwag BJ, Lobner D, Koh JY, Wie MB, Choi DW . Blockade of glutamate receptors unmasks neuronal apoptosis after oxygen-glucose deprivation in vitro. Neurosci 1995; 68:615–9.
Ruscher K, Freyer D, Karsch M et al. Erythropoietin is a paracrine mediator of ischemic tolerance in the brain: evidence from an in vitro model. J Neurosci 2002; 22:10291–301.
Li Y, Powers C, Jiang N, Chopp M . Intact, injured, necrotic and apoptotic cells after focal cerebral ischemia in the rat. J Neurol Sci 1998; 156:119–32.
Pauwels PJ, van Assouw HP, Leysen JE, Janssen PA . Ca2+-mediated neuronal death in rat brain neuronal cultures by veratridine: protection by flunarizine. Mol Pharmacol 1989; 36:525–31.
Koh JY, Wie MB, Gwag BJ et al. Staurosporine-induced neuronal apoptosis. Exp Neurol 1995; 135:153–9.
Charriaut-Marlangue C, Margaill I, Represa A, et al. Apoptosis and necrosis after reversible focal ischemia: an in situ DNA fragmentation analysis. J Cereb Blood Flow Metab 1996; 16:186–94.
Chen J, Li Y, Wang L, Lu M, Chopp M . Caspase inbibition by Z-VAD increases the survival of grafted bone marrow cells and improves functional outcome after MCAo in rats. J Neurol Sci 2002; 199:17–24.
Aspey BS, Taylor FL, Terruli M, Harrison MJ . Temporary middle cerebral artery occlusion in the rat: consistent protocol for a model of stroke and reperfusion. Neuropathol Appl Neurobiol 2000; 26:232–42.
Belayev L, Alonso OF, Busto R, Zhao W, Ginsberg MD . Middle cerebral artery occlusion in the rat by intraluminal suture. Neurological and pathological evaluation of an improved model. Stroke 1996; 27:1616–23.
Dawson DA, Ruetzler CA, Hallenbeck JM . Temporal impairment of microcirculatory perfusion following focal cerebral ischemia in the spontaneously hypertensive rat. Brain Res 1997; 749:200–8.
Olsen TS, Larsen B, Herning M, Skriver EB, Lassen NA . Blood flow and vascular reactivity in collaterally perfused brain tissue. Evidence of an ischemic penumbra in patients with acute stroke. Stroke 1983; 14:332–41.
Roussel SA, van Bruggen N, King MD, Gadian DG . Identification of collaterally perfused areas following focal cerebral ischemia in the rat by comparison of gradient echo and diffusion-weighted MRI. J Cereb Blood Flow Metab 1995; 15:578–86.
Yuan Q, Li R, Yang H, Zhang G . Effects of reperfusion on neuronal changes and macrophagic response after transient focal ischemia—reperfusion of brain in rats. Hua Xi Yi Ke Da Xue Xue Bao 1999; 30:155–7.
Mouw G, Zechel JL, Zhou Y, et al. Caspase-9 inhibition after focal cerebral ischemia improves outcome following reversible focal ischemia. Metab Brain Dis 2002; 17:143–51.
Wang X, Wang H, Xu L, et al. Significant neuroprotection against ischemic brain injury by inhibition of the MEK1 protein kinase in mice: Exploration of potential mechanism associated with apoptosis. J Pharmacol Exp Ther 2003; 304:172–8.
Honkaniemi J, Massa SM, Breckinridge M, Sharp FR . Global ischemia induces apoptosis-associated genes in hippocampus. Mol Brain Res 1996; 42:79–88.
Nunn JA, LePeillet E, Netto CA, et al. Global ischaemia: Hippocampal pathology and spatial deficits in the water maze. Behav Brain Res 1994; 62:41–54.
Zhao G, Flavin MP . Differential sensitivity of rat hippocampal and cortical astrocytes to oxygen-glucose deprivation injury. Neurosci Lett 2000; 285:177–80.
Bossenmeyer-Pourie C, Koziel V, Daval JL . Effects of hypothermia on hypoxia-induced apoptosis in cultured neurons from developing rat forebrain: comparison with preconditioning. Pediatr Res 2000; 47:385–91.
Bossenmeyer-Pourie C, Lievre V, Grojean S, et al. Sequential expression patterns of apoptosis- and cell cycle-related proteins in neuronal response to severe or mild transient hypoxia. Neurosci 2002; 114:869–82.
Hartley DM, Choi DW . Delayed rescue of N-methyl-D-aspartate receptor-mediated neuronal injury in cortical culture. J Pharmacol Exp Ther 1989; 250:752–8.
Kirk CJ, Reddy NL, Fischer JB, et al. In vitro neuroprotection by substituted guani-dines with varying affinities for the N-methyl-D-aspartate receptor ionophore and for sigma sites. J Pharmacol Exp Ther 1994; 271:1080–5.
MacGregor DG, Avshalumov MV, Rice ME . Brain edema induced by in vitro ischemia: causal factors and neuroprotection. J Neurochem 2003; 85:1402–11.
Moldrich RX, Cheung NS, Pascoe CJ, et al. Excitotoxic profile of LY339434, a GluR5 agonist, in cultured murine cortical neurons. Brain Res 2000; 862:270–5.
Sei Y, Fossom L, Goping G, Skolnick P, Basile AS . Quinolinic acid protects rat cerebellar granule cells from glutamate-induced apoptosis. Neurosci Lett 1998; 241:180–4.
Sohn S, Kim EY, Gwag BJ . Glutamate neurotoxicity in mouse cortical neurons: atypical necrosis with DNA ladders and chromatin condensation. Neurosci Lett 1998; 240:147–50.
Curras-Collazo MC, Patel UB, Hussein MO . Reduced susceptibility of magnocellular neuroendocrine nuclei of the rat hypothalamus to transient focal ischaemia produced by middle cerebral artery occlusion. Exp Neurol 2002; 178:268–79.
Dijkhuizen RM, Singhal AB, Mandeville JB et al. Correlation between brain reorganization, ischemic damage, and neurologic status after transient focal cerebral ischemia in rats: a functional magnetic resonance imaging study. J Neurosci 2003; 23:510–7.
McCarter JF, McGregor AL, Jones PA, Sharkey J . FK506 protects brain tissue in animal models of stroke. Transplant 2001; 33:2390–2.
Ko HW, Han KS, Kim EY, et al. Synergetic activation of p38 mitogen-activated protein kinase and caspase-3-like proteases for execution of calyculin A-induced apoptosis but not N-methyl-d-aspartate-induced necrosis in mouse cortical neurons. J Neurochem 2000; 74:2455–61.
Hetz CA, Hunn M, Rojas P, et al. Caspase-dependent initiation of apoptosis and necrosis by the Fas receptor in lymphoid cells: Onset of necrosis is associated with delayed ceramide increase. J Cell Sci 2002; 115:4671–83.
Kristian T, Siesjo BK . Calcium in ischemic cell death. Stroke 1989; 29:705–18.
Kaasik A, Vassiljev V, Poldoja E, Kalda A, Zharkovsky A . Do nuclear condensation or fragmentation and DNA fragmentation reflect the mode of neuronal death? Neuroreport 1999; 10:1937–42.
Kalda A, Eriste E, Vassiljev V, Zharkovsky A . Medium transitory oxygen-glucose deprivation induced both apoptosis and necrosis in cerebellar granule cells. Neurosci Lett 1998; 240: 21–24.
Charriaut-Marlangue C, Ben-Ari Y . A cautionary note on the use of the TUNEL stain to determine apoptosis. Neuroreport 1995; 7:61–4.
de Torres C, Munell F, Ferrer I, Reventosand J, Macaya A . Identification of necrotic cell death by the TUNEL assay in the hypoxic-ischemic neonatal rat brain. Neurosci Lett 1997; 230:1–4.
Grasl-Kraupp B, Ruttkay-Nedecky B, Koudelka H, et al. In situ detection of fragmented DNA (TUNEL assay) fails to discriminate among apoptosis, necrosis, and autolytic cell death: a cautionary note. Hepatology 1995; 21:1465–8.
Pulkkanen KJ, Laukkanen MO, Naarala J, Yla-Herttuala S . False-positive apoptosis signal in mouse kidney and liver detected with TUNEL assay. Apoptosis 2000; 5:329–33.
Lobner D, Choi DW . Preincubation with protein synthesis inhibitors protects cortical neurons against oxygen-glucose deprivation-induced death. Neurosci 1996; 72:335–41.
Moroni F, Meli E, Peruginelli F, et al. Poly (ADP-ribose) polymerase inhibitors attenuate necrotic but not apoptotic neuronal death in experimental models of cerebral ischemia. Cell Death Differ 2001; 8:921–32.
Goldberg MP, Choi DW . Combined oxygen and glucose deprivation in cortical cell culture: calcium-dependent and calcium-independent mechanisms of neuronal injury. J Neurosci 1993; 13:3510–24.
Lobner D, Ali C . Mechanisms of βFGF and NT-4 potentiation of necrotic neuronal death. Brain Res 2002; 954:42–50.
Gendron TF, Mealing GA, Paris J, et al. Attenuation of neurotoxicity in cortical cultures and hippocampal slices from E2F1 knockout mice. J Neurochem 2001; 78:316–24.
Wise-Faberowski L, Raizada MK, Sumners C . Oxygen and glucose deprivation-induced neuronal apoptosis is attenuated by halothane and isoflurane. Anesth Analg 2001; 93:1281–7.
Hwang JY, Kim YH, Ahn YH, Wie MB, Koh JY . N-Methyl-D-aspartate receptor blockade induces neuronal apoptosis in cortical culture. Exp Neurol 1999; 159:124–30.
Seo SY, Yun BS, Ryoo IJ et al. Complestatin is a noncompetitive peptide antagonist of N-methyl-D-aspartate and alpha-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid/kainate receptors: Secure blockade of ischemic neuronal death. J Pharmacol Exp Ther 2001; 299:377–84.
Tanaka R, Komine-Kobayashi M, Mochizuki H et al. Migration of enhanced green fluorescent protein expressing bone marrow-derived microglia/macrophage into the mouse brain following permanent focal ischemia. Neurosci 2003; 117:531–9.
Tomita M, Fukuuchi Y . Leukocytes. Macrophages and secondary brain damage following cerebral ischemia. Acta Neurochir Suppl 1996; 66:32–9.
Acknowledgements
This work was supported by a research grant from Fujisawa Pharmaceuticals Co Ltd Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
JONES, P., MAY, G., MCLUCKIE, J. et al. Apoptosis is not an invariable component of in vitro models of cortical cerebral ischaemia. Cell Res 14, 241–250 (2004). https://doi.org/10.1038/sj.cr.7290225
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/sj.cr.7290225
Keywords
This article is cited by
-
AATF Competitively Interacts with Nuclear AIF and Inhibits Parthanatos of Neurons in dMCAO/R and OGD/R Models
Journal of Molecular Neuroscience (2022)
-
Protective Role of Kv7 Channels in Oxygen and Glucose Deprivation-Induced Damage in Rat Caudate Brain Slices
Journal of Cerebral Blood Flow & Metabolism (2015)
-
Increased concentrations of both NMDA receptor co-agonists d-serine and glycine in global ischemia: a potential novel treatment target for perinatal asphyxia
Amino Acids (2012)
-
VEGF-Induced BBB Permeability is Associated with an MMP-9 Activity Increase in Cerebral ischemia: Both Effects Decreased by ANG-1
Journal of Cerebral Blood Flow & Metabolism (2005)